 |
 |
 |
| |
HEPATITIS ABSTRACTS PRESENTED AT 41ST ANNUAL INTERSCIENCE CONFERENCE ON ANTIMICROBIAL AGENTS AND CHEMOTHERAPEUTICS
Written by Andrew Talal, MD, Cornell-NY Hospital, NYC
|
| |
| |
Note to readers: The 41st annual ICCAC was originally scheduled to be held September 22-25, 2001 but it was cancelled after the World Trade Center disaster. As a result, many authors did not present their posters and slide presentations, particularly those from outside of the United States. In this review, I have taken the information from the abstract and I have indicated where the poster or slide presentation was missing.
In this review, I have organized the presentations according to topic areas as indicated below:
I. Treatment of HCV/HIV Coinfection
A. HCV treatment in IFN-naive, coinfected patients treated with IFN/RBV combination
B. Treatment of coinfected individuals who relapsed or did not respond to a previous course of therapy:high-dose infergen with induction dose
C. Treatment of HCV monoinfected individuals: an evaluation of 2 doses of Pegasys; Histamine
II. HCV Pathogenesis and natural history
III. Immunology
IV. Hepatotoxicity and other complications of ARV therapy.
V. Hepatic transplantation
A. Infectious complications of hepatic transplantation (Herpes & CMV)
B. Hepatic Transplantation in HIV/HCV coinfected individuals
VI. Hepatitis B
Editorial note from Jules Levin: I was struck by the poor study design of coinfection studies at ICAAC. As you read through these studies you can see that often potential cofactors were not considered in the outcomes. It is difficult to draw conclusions out of such studies. For example, if you are comparing the development of hepatotoxicity depending on which NNRTI or PI a patient is taking, unless you know the duration of HCV infection broken down by the particular drug the results are uninterpretable.
I. Treatment of Coinfection
A. HCV treatment in IFN-naive, coinfected patients with IFN/RBV combination
Abstract: H-745: Effectiveness of Use of INF Alfa plus Ribavirin in Patients with Chronic Hepatitis C Comparing the HIV-Positive Population to those HIV-Negative.
J. GOMEZ, J.J. BLANCH, F. MATEOS, V. MARTI, I. TERRANCLE, J.M. CALBO, E. MARTINEZ, J. SOLERA
(Poster not presented, information taken from Program Guide)
A total of 41 patients (29 HIV-/HCV+, 12 HIV+/HICV+) were treated with interferon alfa 3 million units three times per week and ribavirin 1000-1200 mg per day. At week 12 of treatment, 10/12 HIV/HCV coinfected patients remained on therapy with no virologic responses compared to 10/29 (34%) HCV monoinfected patients with undetectable viral load. The poster was not presented and the abstract does not clarify the genotype of the HIV-infected patients except to state that they were not genotype 3. At Week 24, in the HIV-infected group, all patients still have detectable HCV RNA. In the HIV negative group, 6/13 who have reached Week 24 are undetectable. The authors note the small sample size of the study and state that HIV infection is associated with genotypes with worse prognosis and HIV+ patients had worsehistology.
Abstract: H-748: Fast Relapse and High Drop Out Rate after Interferon (ifn) Treatment among HIV-HCV Coinfected Patients.
R. BRUNO, P. ACCHI, V. IAPPINA, C. OCCHETTI, E. RUNETTI, C. ILICE, G. ILICE
(Poster not presented, information taken from Program Guide)
This study evaluated fifty coinfected patients who were all treated with HAART (2NRTI and 1PI) who all received interferon alfa 2a 3 million units each day. 26 of the patients were infected with HCV genotype 1b and 24 patients were infected with genotypes 2 or 3. 34 patients had a high inflammatory (HAI) score (>10) and 18 patients had severe hepatic disease with high fibrosis stage.
At 48 weeks, 10 patients (20%) achieved biochemical and virological response. A virological response as defined at HCV-RNA <100 copies/ml and 16 patients (32%) did not respond to treatment. 24 patients (48%) withdrew from the study mainly because of side effects related to overlapping toxicity of interferon and antiretroviral therapy. All of the patients who responded to the treatment relapsed within the first month after treatment discontinuation.
Commentary: H-745 included a small number of participants and only included very early response data. Liver disease was significantly more advanced and prevalence of genotype 3 significantly reduced in coinfected compared to that in the monoinfected. H-748, a study that only included coinfected patients, also had a high percentage of patients with advanced liver disease. These studies suggest (as have others) that response rate in coinfected may be decreased compared to monoinfected. Had the posters been presented, they most likely would have included data from patients who were treated for a longer period of time.
B. Treatment of coinfected individuals who relapsed or did not responder to a previous course of therapy
Abstract: H-459: Infergen(R) Treatment of HCV in Patients Co-Infected with HIV Who Failed a Previous Course of Interferon.
M. RODRIGUEZ1, J.F. RODRIGUEZ2
There are no effective treatments for interferon nonresponders and there are few no prior studies have evaluated effective treatment of HIV/HCV coinfected individuals who failed to respond to interferon. The objective of this study is to evaluate the effectiveness of high dose consensus interferon with or without a 4 week daily induction in HIV/HCV coinfected individuals who failed to respond to standard interferon. The important point of this study is that it evaluated treatment in coinfected patients who did not respond to a prior course of interferon.
Patients were divided into two groups. Group 1, which contained a total of 10 patients, received Infergen 15 mcg three times per week for 48 weeks and Group 2, which contained a total of 87 patients, received Infergen 15 mcg each day for 4 weeks followed by Infergen 15 mcg three times per week for a total of 44 weeks.
|
|
| |
 |
|
| |
Conclusions: Overall, there is a 9.3% response rate in nonresponders and relapsers to IFN who are treated with an induction dose of daily consensus IFN followed by three times per week treatment for 48 weeks. Daily, high-dose interferon is difficult to tolerate in coinfected individuals as indicated by the fact that 43% did not complete week 4 of therapy. There is a high rate of relapse in these subjects since 25% of the subjects were undetectable at week 24 but more than half relapsed by week 48. Higher levels of circulating IFN, as is seen with pegylated IFN and RBV, may decrease the high rate of relapse.
Commentary: This study demonstrates a 9.3% SVR to IFN monotherapy who received an induction dose in previous nonresponders. Zylberberg et al (see citation below) treated patients with IFN/RBV combination therapy and reported an SVR of 14.3% in HIV/HCV coinfected individuals who were nonresponders or relapsers after treatment with standard interferon. Pegylated interferon, which may have a similar effect as daily interferon, in combination with ribavirin should further increase the response. Studies evaluating the efficacy of pegylated-IFN and RBV in coinfected individuals who relapse or do not respond to conventional therapies are currently in progress.
1. Zylberberg H, Benhamou Y, Lagneaux JL, et al: Safety and efficacy of interferon-ribavirin combination therapy in HCV-HIV coinfected subjects: an early report. Gut 2000;47:694-697.
C. Treatment of HCV in monoinfected individuals
Abstract: H-457: Evaluation of Two Doses of Peginterferon Alfa-2a for the Treatment of Chronic Hepatitis C (CHC).
P.J. POCKROS1, R. CARITHERS2, P. DESMOND3, D. DHUMEAUX4, M.W. FRIED5, P. MARCELLIN6, M.L. SHIFFMAN7, G. MINUK8, K.R. REDDY9, R.W. REINDOLLAR10, A. LIN11, M. BRUNDA11, FOR THE PEGASYS STUDY GROUP
Covalent attachment of IFN to polyethylene glycol (pegylated interferon) results in more durable IFN levels and an increased SVR. The goal of this study was to evaluate the effectiveness of Peg-IFN-a-2a administered at 135 mcg/wk as a step-down dose compared to the standard dose of Peg-IFN 180mcg/wk and conventional IFN.
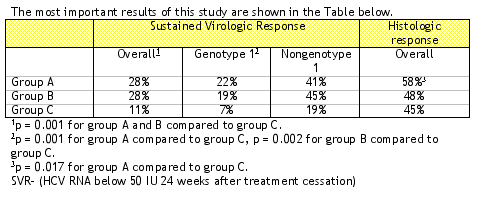
Subjects were randomized to one of three groups 210 subjects received Peg-IFN-a 2a 180 mcg/wk, 215 subjects received Peg-IFN-a-2a 135 mcg/wk, and 214 received standard IFN 3 million units SC three times per week. The primary endpoints of the study were to achieve a sustained virologic response (SVR) (defined as HCV RNA < 100 copies/ml at week 72 (<50 IU by Roche Amplicore), and histologic improvement with at least a 2 point improvement from baseline on post-treatment liver biopsy. All analyses were intention-to-treat. Genotype 1 distribution was not significantly different between the three arms: 65% in 135 arm, 71% in 180 arm, and 65% in IFN 3 MIU arm.
|
|
| |
 |
|
| |
As indicated in the Table above, the virologic response to each of the two doses of pegylated interferon were significantly better than standard interferon. However, the histologic response was significantly better only at the highest dose. The histologic response in the patients who received 135 mcg/wk was not significantly improved to those who received standard interferon. Ten percent of the individuals in each group had to withdraw because they were not able to tolerate the medication intolerance. Depression was observed in 17-20% of patients.
In terms of SVR, 180 mcg/wk and 135 mcg/wk are equally effective doses. In terms of histologic response, 180 mcg/wk appears to be superior to 135 mcg/wk. All patients should be treated initially with 180 mcg/wk in order to achieve early viral clearance, although the dose can be decreased to 135 mcg/wk if adverse effects necessitate. Given the absence of significant histologic improvement between 135 mcg and standard interferon, maintenance therapy to prevent fibrosis progression should probably be given at 180 mcg/wk.
Abstract: H-458: Early Response to Combination Therapy with Low-Dose Pegylated Interferon-Alpha (Peg-IFN) 2b and Ribavirin for Chronic Hepatitis C in HIV-Infected Patients.
L. MORENO, C. QUEREDA, A. MORENO, J.L. CASADO, F. DRONDA, M.J. PEREZ-ELIAS, M.L. MATEOS, S. MORENO
The objectives of this study were to evaluate the safety and efficacy of low-dose Peg-IFN and RBV in HIV/HCV coinfected patients. In this study, 35 HIV/HCV coinfected individuals with persistently elevated ALT and portal or bridging fibrosis on liver biopsy were treated with Peg-IFN a-2b (50 mcg/wk) and RBV 800 mg BID for 12 months. All subjects had CD4 > 300 cells/mm3 and HIV RNA < 10,000 copies/ml. The primary endpoint of the study was the SVR with HCV RNA below assay detection. 86% of the subjects were IVDUs, the average weight 60 kg, and 69% of the individuals in the study were men. The average duration of HCV infection was 16 years, the median HCV-RNA 1 million copies, 54% genotype 1, fibrosis score 1.8, Knodell (inflammation) 6. 32, patients were on ART and 2 were on no therapy. HIV-RNA median 1.7 log, 60% <1.7 log (<50 copies/ml). Median CD4 544, 63% >500 CD4s.
|
|
| |
 |
|
| |
In an analysis that combined multiple factors together, a virologic response at wk 48 was predicted by being infected with nontype genotype 1 (p = 0.012), and HCV RNA below assay detection at week 4 (p = 0.04). These results are consistent with other studies that have shown that those individuals who are infected with genotypes other than 1 respond better and that those individuals who respond early are likely to maintain the response.
Adverse effects that were suffered by the individuals in this trial are as follows: 88% of the individuals had flu-like symptoms, 82% had fatigue, 28% had local inflammatory reactions, 20% had severe headaches, 14% had depression, and 17% had cytopenias. Overall 5 patients (14%) withdrew because of side effects. Lab abnormalities: 23% (n=8) dose reduced and 6% (n=2) discontinued due to hemoglobin <10 g/dL. 14% dose reduced due to neutropenia, none discontinued. 1 patient discontinued due to hyperlactemia.
This study demonstrates that low dose pegylated interferon is safe but the poor virologic response indicates the need for additional studies of higher dose pegylated interferon in coinfected patients. Several of these studies are currently in progress and the results are anxiously awaited. The ET response with the low dose of 50 mcg per week was similar to that seen with standard IFN 3 MIU+RBV (1000-1200 mg/day).
Abstract: H-751: Histamine Dihydrochloride and Interferon Alpha-2b as a Potential New Combination Therapy in Patients with Chronic Hepatitis C (HCV).
Y. LURIE1, K. GEHLSEN2
Interferon appears to have an effect on both the hepatitis C virus and an effect on the immune system. Interferon can increase the production of cytokines (chemicals) by lymphocytes that can be effective in controlling hepatitis C infection. Unfortunately, monocytes and macrophages (MO) in the liver can inhibit this effect of IFN. Histamine may protect lymphocytes from the effect of monocytes and may restore their responsiveness. The objective of this study was to evaluate the feasibility, and safety of four different doses of histamine dihydrochloride in combination with interferon a2b in therapy-naive HCV infected individuals.
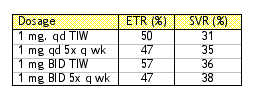
This study (Phase 2) was conducted at multiple centers throughout the world and randomized, patients to receive one of four different doses of histamine dihydrochloride (1 mg. qd TIW, 1 mg qd. 5x qwk, 1 mg BID TIW, 1 mg BID 5x q wk).
End of treatment responses (ETR) and sustained virologic responses (SVR) (as evaluated by intention to treat analysis) are shown in the Table below:
|
|
| |
 |
|
| |
Based on these data, the authors concluded that combination therapy containing histamine and IFN-a-2b appears more effective than IFN-a-2b monotherapy as reported historically (since they did not have a control group), the data suggest that combination therapy containing histamine has an acceptable safety profile and that additional clinical trials with histamine in HCV are warranted and planned.
Comments: This same group recently reported similar results at the AASLD meeting in Dallas, November, 2001 (abs #986 and #713). The results of these studies have been reported in the AASLD meeting summary written for NATAP. In a Phase II study (abs. #713) in which histamine dihydrochloride was given with IFN-a-2b monotherapy, the authors reported an SVR of 44% for the highest histamine dihydrochloride dose. While these preliminary data appear interesting, the authors have failed to demonstrate a statistically significant improvement with the higher doses and they have not demonstrated that the SVR with histamine is significantly better than with standard therapy alone. Hopefully, future trials will compare histamine combined with pegylated interferon and ribavirin to pegylated interferon and ribavirin alone.
Editorial note: histamine is administered by multiple subcutaneous injections per week and side effects are associated with taking the injections (flushing), and this makes administration more cumbersome.
II. HCV pathogenesis and natural history
Abstract: H-456: Pathogenesis of Hepatitis C Virus (HCV) in HIV Positive Patients.
K.A. STELLRECHT, A. MCELHONE, K. PROVIDENCE
Several studies have documented that hepatic fibrosis is accelerated in HIV/HCV coninfected patients, but why coinfected patients have increased fibrosis progression has not been evaluated, although changes in various cytokines (chemicals) that are secreted in the liver may partially account for these observations.
This study evaluated the amount of an important chemical (serum levels of tumor necrosis factor alfa (TNF-a) that is secreted by lymphocytes and which may cause cell damage. It also measured the amount of its receptor (soluble tumor necrosis factor alfa receptor II [TNF-aRII]) and another chemical (transforming growth factor beta [TGF-b]) that is important for telling the cells in the liver to produce fibrous tissue. There were a total of 24 HCV monoinfected and 28 HIV/HCV coinfected individuals who were naive to anti-HCV therapy who took part in this study. HCV RNA was determined by "in-house" RT-PCR assay. Liver biopsies were scored using the Knodell system and apoptosis staining (to detect dead cells) was performed using the Apoptag system. In this cohort of subjects, hepatic inflammation and fibrosis were increased in HIV/HCV coinfected individuals compared to that in HCV monoinfected individuals.
This study showed that the levels of TNF-a (a cytokine that has been shown to be associated with injury in other organs) are significantly increased in coinfected individuals compared HCV monoinfected individuals (6.6 vs 3.9 pg/ml, p = 0.04). In an additional analysis, these authors found a correlation between the levels of the TNF-a receptor and hepatic histology suggesting that the increase in the amount of TNF-a binding may be associated with worse liver histology.
Since increased TNF-a levels are also associated with HIV infection, it is difficult to discern if there is a direct effect on hepatic fibrosis or if they may simply be elevated as a consequence of HIV infection. While these preliminary results are certainly interesting, additional investigation will be required to discern how and why liver fibrosis is increased in coinfected patients.
III. Immunology
Abstract: I-204: Impact of Highly Active Antiretroviral Therapy (HAART) in the Natural History of Decompensated Liver Cirrhosis in HIV-Infected Patients.
C. QUEREDA, L. MORENO, M.E. MORENO, M. RIVERO, S. DIZ, E. BERMUDEZ, M. URIARTE, E. NAVAS, S. MORENO
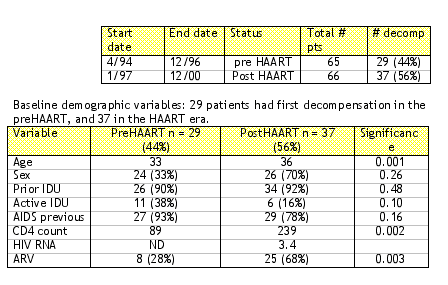
The objectives of this study were to evaluate the effect of HAART on patients with advanced liver disease who start therapy after their first episode of hepatic decompensation. Decompensated liver disease was clinically defined as the presence of one of these conditions: ascites, hepatic encepholopathy, bleeding esphageal varices, hepatocellular carcinoma, bacterial peritonitis.
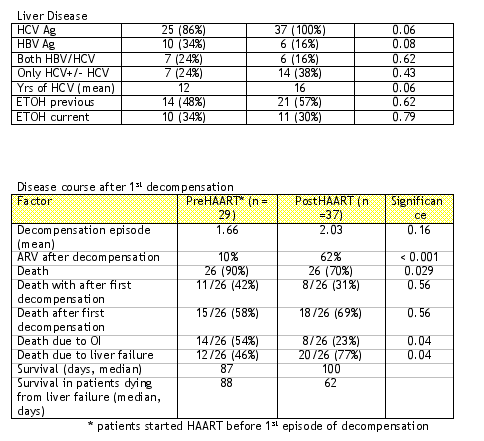
The outcome of patients in two study periods were compared, preHAART and postHAART, as shown in the Table below.
|
|
| |
 |
|
| |
 |
|
| |
The bottom line is that all coinfected patients should be treated aggressively before decompensation and consider liver transplantation after decompensation occurs since HAART does not improve survival of HCV-infected cirrhotic patients.
Commentary: Several studies, including the present one, have documented that liver disease, which may be associated with HCV, is becoming a very important cause of death in HIV infected individuals. Unlike the pre-HAART era, HIV-infection is usually not as advanced in HIV-infected individuals who die in the post-HAART era, as indicated by increased CD4 lymphocytes and HIV RNA below assay detection.
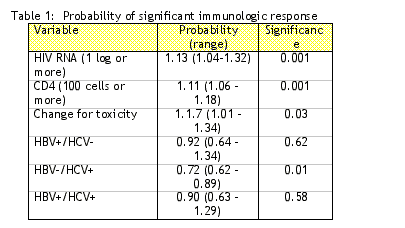
Abstract: I-205: The Influence of HBV-HCV Serostatus on Immunologic and Virologic Responses to HAART in HIV-Infected Naive Individuals.
A. DE LUCA1, R. BUGARINI2, E. GIRARDI3, A. POGGIO4, C. IZZO5, E. PIZZIGALLO6, B. GRISORIO7, A. COZZI-LEPRI8, A. DARMINIO- MONFORTE9
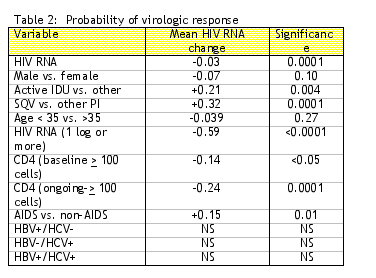
The Swiss HIV cohort study demonstrated that HCV infection impairs CD4 recovery but that there is no difference in virologic efficacy in HIV/HCV coinfected individuals compared to HIV monoinfected individuals. The risk of clinical progression is increased in HIV/HCV coinfected, intravenous drug using (IDU) individuals. The thought is that HCV may inhibit T cell proliferation, which is an important way that lymphocytes are regenerated in people on HAART. These investigators wanted to evaluate the response to ARV medications in HCV treatment-naive subjects, what is the relationship between a therapeutic response and adherence or medication toxicity, and can the findings be extended to HBVHIV coinfected subjects, as well? The goal of this study was to identify whether HCV or HBV serostatus is associated with virologic and immunologic response in therapy-naive subjects initiating HAART.
|
|
| |
 |
|
| |
 |
|
| |
 |
|
| |
Conclusions: An immunologic response to ARV was impaired in HIV infected individuals who were also HCV-infected, while a virologic response was impaired in IDU individuals (may be due to nonadherence; change of therapy due to toxicity associated with better immunologic & virologic responses), but was not associated with HCV infection. The probability of an immunologic response was decreased by 34% in HCV infected individuals and probability of virologic response decreased by 23% in active IDUs. HCV infected individuals are at risk of clinical progression.
This study demonstrates that HCV may delay and prevent full immunologic reconstitution in HIV/HCV coinfected patients. As suggested by other studies, HCV may impair lymphocyte proliferation, which is an important way for lymphocytes to repopulate the immune system.
IV. Hepatotoxicity and other complications of ARV
Abstract: I-206: The Use of Nelfinavir (NFV) and Two Nucleosides Concomitantly with Methadone (MTH) Is Effective and Well-Tolerated in HepC Co-Infected Patients.
L.S. BROWN1, M. CHU1, C. AUG2, S. DABO1 (ARTC, Agouron)
NFV and MTH are both metabolized via the same pathway in the liver (cytochrome p450) and may require dose adjustment in patients with liver dysfunction. The goal of this study was to see if coinfected patients could tolerate both NFV and MTH. This study was conducted by a retrospective chart review a large, multi-clinic methadone maintenance treatment agency in New York City. Subjects had to take NFV and had to be on a stable methadone dose one month prior to NFV initiation.
A total of 32 subjects were identified but only 29 were eligible for the study. Mean length of NFV treatment 20 months. Of the 29 patients, only 12 had pre and post baseline HIV RNA and CD4 measurements, which showed that HIV RNA decrease (median-0.98 log) and CD4 lymphocyte increase (median-32 cells/mm3) (NS). Only 2/32 (6%) patients complained of diarrhea.
The authors concluded that the combination of NFV and MTH is well tolerated in HIV/HCV coinfected individuals. However, the efficacy of the combination in this subgroup of patients will require further investigation.
Abstract: I-207: Hepatotoxicity Associated with Antiretroviral Therapy in HIV-Infected Adults: Seriousness and Predictive Factors.
M.E. MORENO, A. MORENO, M. RIVERO, M. URIARTE, S. DIZ, F. DRONDA, M.J. PEREZ-ELIAS, L. MORENO, C. QUEREDA, S. MORENO
Many antiretroviral medications are associated with liver toxicity. The goal of this study was to investigate the incidence of liver toxicity after HAART initiation and to identify the factors that predispose to liver toxicity.
This study prospectively evaluated 221 individuals who began HAART after January, 1997 and who had at least 12 months of follow-up. Liver function tests were obtained before therapy and every 3 months thereafter. Liver toxicity was defined by the study authors as grade 3/4 elevations and liver toxicity considered related to HAART if there were no other likely explanations. 58% were IVDUs. CD4 count 186. HIV-RNA 100,000 copies/ml. 62% in study had HCV, but this was not broken down by the prevalence of HCV for each PI patients were taking. 37% had alcoholism but again the incidence was not broken down by which PI patient was taking. 68% of patients had normal ALT & AST, 3% had grade 3, 0.5% had grade 4.
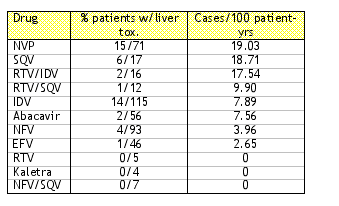
Results: Thirty (15.4%) subjects developed severe hepatotoxicity (grade 3 or 4), (incidence was 6.9 per 100 patient-years) which resulted in discontinuation of therapy in 9 (4.2%) individuals 6/9 during the first six months of therapy. 3 discontinuations occurred by the 3rd month, 3 by the 6th month, and 1 each by the 18th, 23rd, and 32nd months. There were no associated deaths. Liver abnormalities were reversible in all patients. Author's poster said there was no impact on virologic or CD4 response. Patients with or without liver toxicity had the same CD4 increases. But a graph showed viral load at month 36 was 3.95 log for patients with liver toxicity vs. 2.33 log for patients without liver toxicity. Viral load was equally suppressed in both arms until month 36 when it increased in the group with liver toxicity but remained suppressed in other group.
The study results could have been strengthened if the authors had reported the incidence of hepatoxicity according to the PI and NNRTI drugs the patient was taking. Other factors that would have strengthened the study include stratification by cofactors such as alcohol use and duration of HCV.
|
|
| |
 |
|
| |
By multivariate analysis, preHAART increased transaminases (RR, 0.98; 95% CI 0.98 - 0.99) was the only variable significantly predictive of hepatotoxicity. NVP use (RR 2.25, p value 0.074) and saquinavir use (RR 3.16, p-value 0.081) appeared to perhaps have some association with liver toxicity but there was no significance and again potential cofactors were not reported-including which accompanying NRTIs patients were taking, how many patients on a particular regimen had elevated ALT, etc.
Conclusions: A significant proportion of patients are at risk of developing hepatotoxicity after HAART, but the clinical consequences do not seem to be severe. PreHAART transaminase elevation and drug use are risk factors for development of hepatotoxicity.
Abstract: I-208: Risk and Determinants of Developing Severe Hepatic Cytolysis During Therapy with Non-Nucleoside Analogue Reverse Transcriptase Inhibitor Combinations in HIV-Infected Patients.
J. ENA, C. AMADOR, F. PASQUAU, C. BENITO, V. FENOLL, V. MARTINEZ LOPEZ
This is a retospective cohort study that was conducted from January 1997 to December 2000. To evaluate the safety of non-nucleoside analogue reverse transcriptase inhibitors in individuals with HBV and HCV infection taking efavirenz or nevirapine combinations. Grade 3/4 elevations in AST, or ALT, or bilirubin were the outcomes looked for in this study.
Again in this study, the authors did not report the incidence of cofactors according to which ART drug the patient was taking. HCV duration, alcohol use, etc. could have been higher in patients receiving a particular NNRTI.
A total of 136 patients treated with follow-up every three months. Nevirapine was combined with two nucleoside analogue reverse transcriptase inhibitors (NRTIs) in 50 (47%) and with two NRTIs plus protease inhibitor (PIs) in 20 (18%) of the treated individuals. Efavirenz was combined with two NRTIs in 34 (31%) and with NRTI plus Pis in 4 (4%) of treated individuals. Fifty-two/136 (48%) of the HIV-infected individuals also were HCV antibody positive. Median HIV-RNA was 2000 copies/ml. 6% were HbsAg+. 12% of patients were ART-naive. Median CD4 was 364. 43% were IVDUs. 68% were men.
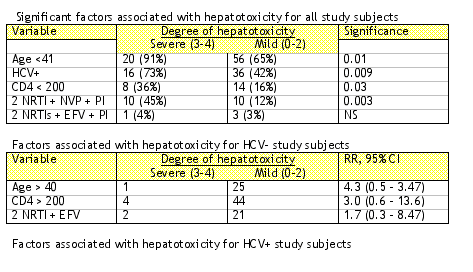
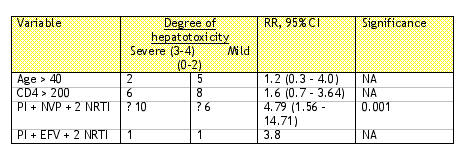
The results of this study are shown in the table below. Six out of 56 (11%) HCV- and 16/52 (31%) HCV+ individuals developed severe hepatotoxicity (RR: 2.87, 95% CI: 1.22 - 6.78, p = 0.009).
Significant factors associated with hepatotoxicity for all study subjects
Variable Degree of hepatotoxicity
|
|
| |
 |
|
| |
 |
|
| |
Conclusions: No risk of developing severe hepatotoxicity was observed between when a NVP or EFV containing regimen was combined with 2 NRTIs. However, the addition of a PI (70% NVF) to a regimen containing NVP + 2 NRTIs increased the risk of developing severe hepatotoxicity. HCV+ antibody patients had about 3-fold risk of developing severe liver cytolosis compared with HCV- antibody patients (31% vs 11%). HIV infected patients with HCV coinfection should be monitored closely during ART for liver function tests.
Abstract: I-209: Nevirapine Induced Acute Hepatitis.
M.L. FERNANDEZ-GUERRERO, J. BECARES, M. GORGOLAS, R. GARCIA-DELGADO
(Poster not presented)
BKG/Objectives: To evaluate the incidence and significance of hepatitis due to NVP.
Methods: Retrospective review (1/98-1/01) of 394 NVP treated individuals for > 1 wk.
Results: 110 /394 (28%) of treated individuals had minor elevations of hepatic enzymes and 5 (1.5%) patients developed acute icteric hepatitis within 3-5 wks. of NVP initiation. 1/5 HBV had "chronic hepatitis B" and all patients had mild eosinophilia. Median TB = 4.7 mg/dL, AST = 901 U/L, GGT = 710 U/L. Liver biopsy performed in one individual showed periportal hepatitis with eosinophilic infiltration of the portal areas and colostasis. Clinical and biochemical abnormalities resolved in all individuals within 8 weeks of NVP discontinuation.
Conclusions:Although the risk of developing acute icteric hepatitis following NVP administration is low, it needs to be considered in any patient who presents with compatible symptoms and signs.
Abstract: H-739: Pancreatitis: an Emerging Complication of HCV Treatment in HIV Co-Infected Patients Treated with Didanosine/Stavudine Containing Regimens.
J. HESTER1, P. KEISER2, R. BERGGREN2
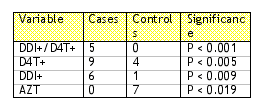
This study evaluated the incidence of pancreatitis in HIV infected individuals on DDI, D4T or a combination of DDI and D4T who were treated with RBV. 10/25 individuals developed chemical pancreatitis (defined as two-fold increase in lipase), 5/10 developed clinical pancreatitis and one patient required hospitalization. Pancreatitis developed between 86-102 days after initiation of DDI or D4T, respectively. Based on this study, it would seem advisable to measure pancreatic enzymes (amylase and lipase) in any patient on D4T and/or DDI who initiates RBV therapy for the first six months.
|
|
| |
 |
|
| |
Abstract: H-738: Effect of Protease Inhibitors on the Severity of Liver Disease in HCV Patients Co-Infected with HIV.
M. RODRIGUEZ
This poster was initially reported at AASLD in November 2001. The study evaluated the association between hepatic inflammation and individuals who were treated with one of three protease inhibitors (saquinavir, nelfinavir, indinavir). Maribel Rodriguez reported in a poster on 100 of her HCV/HIV coinfected patients referred to her clinic for HCV treatment from the metropolitan area of San Juan, PR from 1998-2000. She concludes that despite overall good control of HIV a high percentage of her Hispanic patients have end stage liver disease. 55% had either bridging fibrosis (33%) or cirrhosis(22%). Only 22% had no indication of fibrosis and the rest (33%) had mid fibrosis. Alcohol use was frequent (65%). Average cd4 was 437. And 45% had undetectable HIV viral load (<400). One of the important cofactors that was omitted was the duration of HCV, which could have an impact on the interpretation of the results. Other potential cofactors were not considered.
Abstract: H-740: Factors Associated with Hyperglycemia Complicating HAART in the HIV/HCV Coinfected Population.
M.L. HOFFMAN-TERRY, E. ODONNELL, A. WASYLIK, T. WASSER, M.N. SAQIB
Hyperglycemia and type II diabetes mellitus are common in HCV infection and in HIV-infected patients treated with ARV. The goal of this study was to evaluate the incidence and risk factors associated with the development of hyperglycemia and type II diabetes mellitus in HIV/HCV coinfected patients treated with ARV. This study was a retrospective, case-control study in which 53 HIV/HCV coinfected patients (group 1) were matched by age, sex and body mass index (BMI) with 53 HIV+/HCV- patients (group 2). Preexisting DM was an exclusion factor.
This study showed that baseline fasting blood sugars, while being similar at baseline, were significantly higher in the HIV/HCV coinfected individuals (group 1) at 3, 6, and 9 months of follow-up. Hyperglycemia developed in 6/53 HIV/HCV coinfected individuals compared to 0/53 HCV monoinfected (p = 0.012), and 5/6 met ADA criteria of diabetes mellitus. All of the individuals in the hyperglycemic group were overweight with BMI > 25 and 5/6 were on protease inhibitor containing regimens. 4/6 of the hyperglycemic patients had liver biopsies with mean Scheuer biopsy grade 3.3.
The implications of this study are that careful attention to the possibility of diabetes mellitus should be considered in HIV/HCV coinfected individuals who manifest risk factors for the disease such as increased BMI and a regimen containing medications (PI) that are associated with diabetes.
Abstract: H-742: Self-Reported Quality of Life in a Population-Based Cohort of HIV and Viral Hepatitis C Co-Infection.
V.C. MONTESSORI, K. CHAN, J.S.G. MONTANER, M.V. OSHAUGHNESSY, R. HOGG
(Poster not presented)
All ARV medications in British Columbia are distributed by the Provincial Health Authority. 339 patients completed a questionnaire to ascertain quality of life and self-assessment of health status. HCV/HIV coinfected patients were more likely to have impaired quality of life and poor health assessment compared to HIV monoinfected subjects.
Abstract: H-741: HIV Infected Inpatients in The HAART Era; Impact of Hepatitis C Virus.
O. FALUSI1,2, J. PULVIRENTI1,2, J. SARAZINE1, P. SHASTRI1, C. GAIL1, R. GLOWACKI1
The goal of this study was to compare the demographic and clinical characteristics of HIV+/HCV+ patients to HIV+/HCV- patients in the inpatient setting. The study consisted of a retrospective review of all HIV+ patients admitted to Cook County Hospital HIV ward from Oct 1999-Sept 2000.
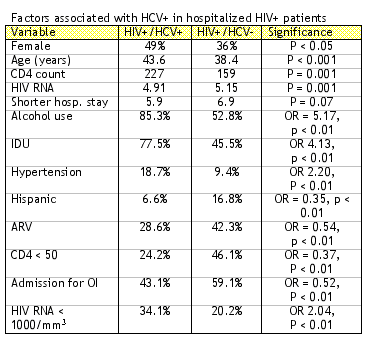
During the study, 644 HIV+ individuals accounted for 1050 hospital admissions. Of these, 510 had documented HCV serology with 203 (40%) being HCV+.
|
|
| |
 |
|
| |
Regarding causes for hospitalization, HCV+ patients were more likely to be hospitalized with hepatitis (12.3% vs. 6.5% Or 2.01, p = 0.02), internal medicine problems (diabetes, endocarditis, pancreatitis, cardiac, renal disease) (91.9% vs. 87.4% OR 1.62, p = 0.04), and complications of liver disease (GI bleed, encephalopathy, ascites, coagulopathy) (67.9% vs. 32.1% p < 0.001).
Conclusions/Commentary: This study demonstrates, as have several others, that HIV/HCV coinfected individuals have more severe liver disease and more frequent hospitalizations for complications of liver disease compared to HIV-infected individuals without hepatitis C. It is not clear why more of the HCV- patients were on ARV therapy, even though the percentage of individuals with HIV RNA < 1000/mm3 was lower in the coinfected patients and CD4 cell count was higher. While the course of HIV disease may not have been as advanced in these patients, their ability to spontaneously control HIV replication is interesting.
Abstract: H-743: Significance of HCV Coinfection with Persistent Normal Alanine Aminotransferase (ALT) Levels in HIV-Infected Patients.
L. FONQUERNIE, L. SERFATY, A. CHARROIS, D. WENDUM, B. LEFEBVRE, P. TANGRE, J. MEYNARD
The issue of whether HCV monoinfected individuals with normal ALT levels have progressive liver disease and should be treated has been controversial. Current opinion is that these patients do have progressive liver disease and that they should be considered to receive treatment. The goal of this study was to assess prevalence, clinical, biological, histological, and predictive factors of chronic hepatitis C with persistent normal ALT levels in HIV-infected patients.
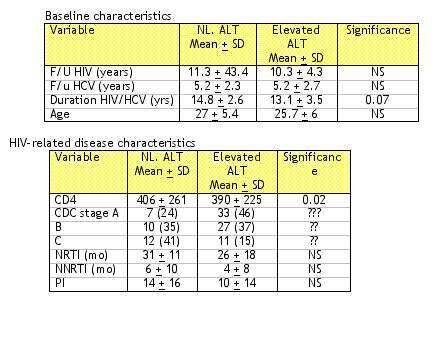
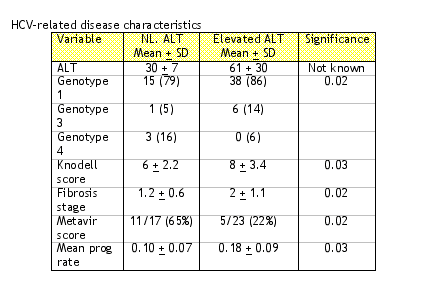
This study was a retrospective comparison of HIV/HCV coinfected individuals with normal ALT (<48 IU/mL) to those with increased ALT. The results of this study demonstrate that 182/800 individuals were coinfected and a total of 112 were eligible for this study. 101 had HCV RNA detectable and 29 with normal ALT and 72 with elevated ALT. Characteristics that were different between the two groups are demonstrated in the table below:
|
|
| |
 |
|
| |
 |
|
| |
Abstract: H-744: Alcohol Consumption Effects in HIV Infected Persons with Hepatitis C.
A.J. GORDON1, J. CONIGLIARO1, A.C. JUSTICE1, K. MCGINNIS1, A.M. KILBOURNE1, L. RABENECK2, S. BROWN3, FOR THE VACS PROJECT TEAM
The goal of this study was to evaluate the influence of alcohol binge drinking behavior on viral load and liver toxicity for HIV-infected individuals with and without hepatitis C. The data for this study were collected from the Veterans Aging Cohort Study-3 VACS 3), a multi-site, longitudinal, cohort of 881 HIV-infected veterans
The results of this study are that overall, 43% of the cohort was HCV coinfected and 40% drank alcohol. Among those who drank alcohol, 66% are binge drinkers. HCV coinfected individuals are more likely to binge drink compared to those without HCV. Among individuals who did not binge drink, HCV-infected individuals had significantly higher AST levels (p < 0.001) than those who where not HCV-infected. HIV RNA were significantly higher in HIV positive individuals who binge drink. After stratifying on HCV serostatus, binge drinkers had lower median CD4 counts and higher HIV RNA levels compared to non-binge drinkers.
This study shows that HCV infected individuals are more likely to drink hazardous amounts of alcohol and may be synergistic with HCV in causing hepatic injury. This is an important study that adds to the data that substance abuse is more common in HIV/HCV coinfected. Physicians who treat these patients need to assess the effect of alcohol in each individual patient and counsel those who abuse it regarding its toxic effects.
Abstract: H-747: The Impact of Demographic Background, ALT, CD4 and HIV Viral Load on HCV Viral Load in HIV/HCV-Coinfected Patients.
C. HSIAO, P. GADA, M. SHELTON, Y. WU
BKG/objectives: To evaluate factors among HIV infected individuals that might affect HCV viral load and to develop a mathematical model to predict a patient's HCV RNA level in coinfected patients. This study was a retrospective evaluation of HIV-infected individuals admitted to Erie County Medical Center, Buffalo NY 12/98-8/01.
A total of 157/538 individuals were HCV RNA+. Patients race, ALT, HDL, CD4 count, and HIV RNA all significantly correlated with HCV RNA level. Race also was associated with HCV RNA, white individuals tend to have HCV RNA < 5,000 copies while African Americans have HCV RNA > 5,000. Patients with high HIV RNA also tend to have high HCV RNA (VL > 850,000).
Regarding the mathematical modeling-- considering three factors (a) ALT > 50, (b) HDL < 30, and (c) HIV RNA > 75,000, the estimated chance of HCV RNA > 850,000 copies/ml is 90% if all three factors are present, 70-80% if two factors are present, 50-60% if one factor is present and 30% if none of the above factors is present. The same formula can be used to predict the likelihood that an individual will have HCV RNA < 5,000: three factors (a) ALT > 50, (b) HDL < 30, and (c) AA race, the estimated chance of HCV RNA <5,000 copies/ml is 0.6% if all three factors are present, 2-10% if two factors are present, 10-30% if one factor is present, and 60% if none of the above factors are present.
V. Hepatic transplantation
A. Infectious complications of hepatic transplantation
Abstract: H-461: Impact of Human Herpesvirus-6 (HHV-6) Viremia on the Frequency and Severity of Recurrent Hepatitis C Virus (HCV) Hepatitis in Liver Transplant Recipients.
N. SINGH1, S. HUSAIN2, D. CARRIGAN3, K. WECK2, M. WAGENER2, T. GAYOWSKI2
This study evaluated the same cytokines that were evaluated in the study described earlier H-456. This study evaluated the amount of an important chemical (serum levels of tumor necrosis factor alfa (TNF-a) that is secreted by inflammatory cells, which may cause cell damage, and which is increased in viral hepatitis, including human herpes virus (HHV)-6. After hepatic transplantation, increased TNF-a is associated with disease recurrence. High levels also predict a poor response to IFN.
This study was designed to evaluate the impact of HHV-6 on the outcome and progression of recurrent HCV-associated hepatitis in liver transplant recipients. HCV recurrence was monitored in 51 consecutive liver transplant recipients were prospectively monitored for HHV-6 and cytomegalovirus (CMV) viremia. HCV recurrence was detected by histopathological evaluation and HCV disease was assessed by the HAI and Knodell scores (two measures that are used to grade inflammation and fibrosis in the liver). Other variables that were monitored were HCV genotype, degree of alcohol intake and whether the immunosuppressive regimen contained OKT-3.
The frequency of recurrent hepatitis did not differ between those with and without HHV-6 viremia (p = 0.9). However, HCV relapsed more quickly (median 3.7 vs. 9.9 mos, p = 0.17) and more severely (mean fibrosis score 1.5 vs. 0.03, p = 0.01) in HHV-6 viremic subjects compared to those who were not HHV-6 viremic. Several other variables including CMV viremia and CMV and HHV-6 viremia did not have an effect of HCV recurrence. Several established variables that are known to effect recurrence including HCV genotype, biopsy proven rejection, augmented immunosuppression, and pretransplant alcohol use did not increase the likelihood of HHV-6 viremia.
The implications of this study are that among HCV-infected individuals undergoing hepatic transplantation, HHV-6 viremia was associated with early and more severe HCV recurrence in the transplanted liver. Monitoring of HHV-6 levels among patients undergoing hepatic transplantation may be important in the management of these patients.
Abstract: H-462: Interactions Between Cytomegalovirus (CMV), Human Herpesvirus-6 (HHV6), and the Recurrence of Hepatitis C (HCV) after Liver Transplantation.
A. HUMAR1, D. KUMAR2, A. CALIENDO3, L. LILLY1, G. MOUSSA4, G. LEVY1, T. MAZZULLI4
The goal of this study is very similar to the one that was just reported above. The authors also wanted to test the hypothesis that CMV and HHV6 may be associated with HCV recurrence after hepatic transplantation.
67 HCV-infected liver transplant recipients with serial serum measurements for CMV and HHV6. Among patients with more severe HCV recurrence (hepatic fibrosis or inflammation score > 2 on liver biopsy), HHV6 positivity was significantly increased (p = 0.009).
Commentary: These studies both demonstrate that HHV6 viremia post hepatic transplantation in HCV-infected individuals is associated with earlier and more severe hepatitis recurrence.
B. Hepatic Transplantation in HIV/HCV coinfected individuals
Abstract: I-203: Solid Organ Transplantation in Patients with Human Immunodeficiency Syndrome: a Successful Case Series.
G.T. NEFF, D. JAYAWEERA, O. HUNG, D. LEVI, D. WEPPLER, J. NERRY, T. KATO, L. DOWDY, C. OBRIAN, K. REDDY, L. KRAVETZ, E. SCHIFF, A. TZAKIS
With the improvement in HIV-associated morbidity and mortality, solid organ transplantation in HIV-infected individuals has recently become a consideration. Several large studies are currently evaluating the efficacy and feasibility of liver transplantation in HIV-infected individuals. This study reported on the experience at the University of Miami.
Seven HIV-infected individuals with decompensated cirrhosis secondary to HBV (3/7), HCV (3/7), or HBV/HCV (1/6) were approved for orthotopic hepatic transplantation. One patient died of sepsis while awaiting transplantation. Antiretroviral therapy was initiated prior to OLT in 6/7. All but 1 patient had HIV viral load <50 c/ml and CD4 <100. One patient presented with fulminant hepatitis and they were unable to start HAART prior to OLT. All patients were reviewed and treated by the University of Miami HIV team. Patients are followed by a medical team consisting of transplant surgeons, transplant hepatologists, and clinical immunologists.
Six patients successfully received OLT. One patient succumbed to sepsis while waiting for the OLT. The six patients that received OLT have to date survival period of 2, 8, 10, 12, 16, 30 months (mean 13.0). Side effects included acute rejection (n = 2), wound infection (n = 1), tacrolimus toxicity (n = 2) due to drug interaction with their prospective PI. All 6 patients are currently on HAART, have >100 CD4+ lymphocytes and HIV RNA < 50 copies/ml. None of the patients suffered an opportunistic infection during the post-transplantation period.
The implications of this study are that orthotopic liver transplantation can be performed successfully in HIV-infected individuals with decompensated cirrhosis secondary to viral hepatitis. Given the large number of HIV-infected individuals who are also infected with hepatitis B and/or C viruses is common in HIV-infected individuals, many of these individuals are currently being treated with interferon-based regimens. Approximately fifty percent of these individuals will respond to therapy, which means that the other fifty percent may eventually be candidates for hepatic transplantation. The data from large clinical trials of solid organ transplantation in HIV-infected individuals will help to clarify the survival and management of these patients. In speaking with Neff he told me that 2 HCV/HIV transplants were doing well at 1.5 years and the third patient was not doing well.
VI. Hepatitis B Virus (HBV)
Abstract: H-464: Dose Optimization for LdT and Other Hepatitis B Antivirals: Importance of Second-Phase Clearance and Viral Dynamics Modeling.
X. ZHOU1, C. LAI2, N. BROWN1, M. MYERS1, D. POW1, S. LIM3
BKG: Current HBV treatment regimens (IFN, lamivudine [3TC]) are unsatisfactory secondary to poor response rates, large number of individuals affected by adverse effects (particularly those treated with IFN,) and viral resistance(particularly those treated with 3TC). This problems are magnified in patient subgroups that are poor responders to treatment such as individuals with precore mutations (HbeAg-), cirrhotics, immunocompromised, and HIV/HBV coinfected subjects. In the early years of the HIV epidemic, the same factors complicated HIV treatment. However, the development of more potent antiretroviral agents and their use in combination have had a dramatic effect on HIV-associated morbidity and mortality. Several clinical trials are currently in progress to find additional and more effective therapeutic agents for the treatment of HBV. Within the next few years, HBV-infected individuals will be treated simultaneously with several agents, as is currently the practice in the treatment of HIV.
LdT is an L-nucleoside, which is a potent inhibitor of HBV DNA polymerase. Previous studies have demonstrated that doses ranging from 25-200 mg/d resulted in HBV DNA decline of 2-3 log10 within 2-4 weeks. Previous investigation has demonstrated that HBV, like HIV and HCV, decays according to a two-compartment model. The first phase corresponds to HBV clearance from peripheral blood and the second phase corresponds to loss of virally infected cells. By analyzing the slope of HBV DNA decline during the second phase, the efficacy of different therapeutic regimens and different doses of the same regimen can be evaluated. (i.e. the more potent the medication, the higher the slope). The goal of this study was to optimize the LdT dosage by modeling viral decay during the second phase.
Methods: LdT was administered to subjects at doses of 25, 50, 75, 100 and 200 mg/d) for 4 weeks. Subjects were also followed for an additional 12 weeks. Matching 6:1 drug recipients:placebo was performed.
Results: The association between HBV DNA reductions and LdT dose were evaluated by (a) direct analysis of HBV DNA reductions during week 1 (first-phase clearance) compared with weeks 2-4 (second phase clearance) and (2) viral dynamic modeling to determine the clearance-rate constant of infected cells. The model demonstrated that HBV DNA clearance during the second phase was accelerated and the half-life of infected cells diminished with higher doses of LdT. Modeling predicted that higher doses (600-800 mg/d) or longer treatment may result in greater (e.g. >6-7 log10) HBV DNA reductions.
Conclusions: Analysis of the second phase clearance (a) eliminates confounding by rapid HBV clearance during the first phase and (b) demonstrates that the clearance of infected cells is dependent on the dose of medication used.
Commentary: This study demonstrates that LdT induces HBV clearance according to a two-compartment model. The first phase corresponds to HBV clearance from peripheral blood and the second phase corresponds to the clearance of productively infected cells. The most efficacious drug should provide the most rapid clearance during the second phase. This study demonstrates that applying mathematical models to the results obtained at lower doses of a medication (that may be tested first because they may cause less side effects) can be used to predict and to justify the evaluation of higher doses. Based upon the results obtained with the lower dose, the protocol was amended to test the higher dose.
|
|
| |
|
 |
 |
|
|