 |
 |
 |
| |
Impact of Pegylated Interferon alfa-2b (Peg-Intron) and Ribavirin on Progression of Liver Fibrosis in patients with Chronic Hepatitis C
Reported by Jules Levin
|
| |
| |
Based on 2 biopsies 20 months apart, this study reported:
- Sustained responders improved activity grade, were less likely to have worsened activity, and less likely to see worsened fibrosis
- On average non-responders with fibrosis (F2, F3, and F4) could stop fibrosis progression
- On average sustained responders with fibrosis (f2, F3, and F4) show regression of fibrosis
- 49% with cirrhosis showed some degree of reversal of cirrhosis from F4 stage to either F3, F2 or F1; achieving a sustained response was a significant factor
Thierry Poynard first commented on aims of therapy: (1) to achieve a sustained virologic response which permits fibrosis regression, disappearance of extrahepatic manifestations, disappearance of contamination risks; (2) to block fibrosis progression in patients without a sustained virologic response (perhaps also using a suppressive maintenance therapy).
Editorial note from Jules Levin: Blocking fibrosis progression in nonresponders remains controversial. A number of studies have found fibrosis can be slowed or stopped in transient responders and nonresponders. Some studies have found nonresponders are not able to block fibrosis progression. And it also depends how you define a nonresponder. Mitch Shiffman reported in his study in Gastroenterology (1999; 117: 1164-1172) that patients with some early viral load reduction (1.4 log) and some early fibrosis improvement during therapy are able to sustain viral load reduction and improved histology (liver condition) with ongoing maintenance interferon therapy for the two years of this study. What about patients who are unable to reduce viral load at all and who don't show early fibrosis improvement? I think this remains a question. Two large multiple-year studies HALT-C by the NIH & Roche and CO-PILOT from Schering are exploring this question now. The findings Poynard presented here and earlier at EASL in the Spring of 2001 have been controversial. The question of whether nonresponders can reverse, slow or stop fibrosis progression is perhaps the most controvesial question currently. Poynard first presented this data at EASL but the presentation here at AASLD had several additional new pieces of information. Several observers and researchers I spoke with at AASLD do not buy his findings (the controversy). One doctor told me he does not see these kinds of benefits in his practice. I think other researchers do feel these data have merit.
Poynard pooled data on 3,010 HCV treatment naive, HIV negative patients with paired biopsies from 4,493 patients in 4 trials receiving 10 different regimens (Poynard et al, McHutchison et al, Lindsay et al, and Mannes et al.)
The ten regimens included IFN 24 weeks, IFN 48 weeks, PegIntron 0.5 ug/kg, PegIntron 1.0 ug/kg, PegIntron 1.5 ug/kg, IFN/RBV 24 weeks, IFN/RBV 48 weeks, PegIntron 0.5 ug/kg+RBV, PegIntron 1.5 ug/kg/RBV.
Some characteristics of the 3,010 patients: 66% male, 43 years age, 80 kg weight, 53% IVDUs, genotype 1 70%, genotype 2 28%, genotype 4,5,6 3%, viral load 4 million.
Duration of HCV infection for patients was 18 years. Duration between the 2 biopsies was 20 months. The size of the biopsy in mm was 16.
25% had fibrosis (F2 13%, F3 7%, F4 5%-cirrhosis), and 73% had F1 (minimal fibrosis) and 2% had F0 (no fibrosis). About about 1/3 of patients had each of severe, moderate or mild activity (A1, A2, or A3).
The histological impact of each regimen was estimated by the percentage of patients with at least one grade improvement in the necrosis and inflammation (METAVIR score), the percentage of patients with at least one stage worsening in fibrosis METAVIR score and by the fibrosis progression rate per year.
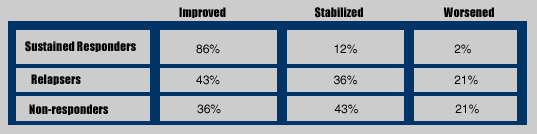
Activity Grade Improvement (at least one grade improvement Metavir score)
|
|
| |
 |
|
| |
This was new information presented for the first time at AASLD and not earlier at EASL. Being able to achieve a sustained virologic response is an important factor in being able to achieve a significant improvement in activity. Obviously, choosing the most effective regimen (its potency and tolerability) is important in being able to achieve a sustained response significantly and in turn improved activity and fibrosis. So, you want to use the most potent (antiviral activity) and tolerable regimen. Tolerabiliy is important because with more side effects and adverse events adherence may be more challenging.
Poynard reported an analysis of the change in activity grade by each of the ten regimens including PegIntron 1.5 ug/kg+RBV using the optimized weight based dose of RBV.
- IFN alone 24 weeks: 39% of patients improved, 39% stabilized, 24% worsened
- IFN alone 48 weeks: 41% improved, 40% stabilized,19% worsened
- Peg-Intron 0.5 ug/kg: 48% improved, 35% stabilized, 20% worsened
- Peg-Intron 1.0 ug/kg: 49% improved, 33% stabilized, 18% worsened
- Peg-Intron 1.5 ug/kg: 49% improved, 33% stabilized, 18% worsened
- IFN+RBV 24 weeks: 51% improved, 34% stabilized, 15% worsened
- IFN+RBV 48 weeks: 64% improved, 24% stabilized, 12% worsened
- Peg 0.5+RBV: 70% improved, 24% stabilized, 6% worsened
- Peg 1.5+RBV: 65% improved, 23% stabilized, 12% worsened
- Peg 1.5+RBV*: 73% improved, 21% stabilized, 6% worsened
*RBV optimized weight based dosing
I think its important to note that no data was presented by Poynard on the statistical significance of the differences between the regimens, either on the slides or verbally in his talk. So, you don't know if for example there is a real difference between the 41% of patients receiving IFN for 48 weeks who showed improvement and the 49% who showed improvement using PegInron 1.5 ug/kg. Or for that matter, you don't know for sure if there is a significant difference between standard IFN+RBV taken for 48 weeks (64% improved), PegIntron 0.5 ug/kg+RBV (70%), PegIntron 1.5 ug/kg+RBV (65% improved), and PegIntron 1.5 ug/kg+ optimzed dose of RBV based on weight (73%). In fact, Poynard's data shows little difference if any between the 70% of patients who saw improvement using the low dose of Pegintron 0.5+RBV compared to the patients receiving PegIntron 1.5 ug/kg+ optimized weight based dose of RBV who Poynard reported 73% of these patients experienced improved activity grade. There may not be any significant difference between 70% and 73%.
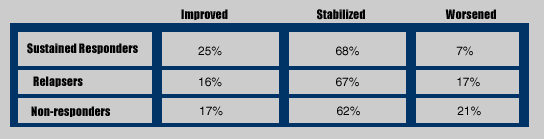
Fibrosis Stage Variation
(the percentage of patients with at least one stage change in fibrosis METAVIR score). The biopsies were performed 20 months apart so Poynard suggested that given more time fibrosis ought to continue to improve further for some patients. In particular, you might expect if any will continue to improve it would be sustained responders and perhaps some patients continuing on maintenance therapy.
|
|
| |
 |
|
| |
Again, Poynard did not present data on the statistical significance between any of the differences between the groups. But, he did comment orally in his presentation that the differences in the worsening category (7% vs 17% vs 21%) were statistically significant. I think its fair to conclude that a sustained responder has a better chance for improved fibrosis than a relapser and moreso than a non-responder. The difference in the worsening category between sustained responders and non-responders and relapsers (21% vs 7% and 17%) strikes my attention.
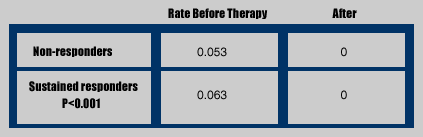
Fibrosis Progression Rate Per Year
Poynard reported the fibrosis progression rate per year in 1900 patients with F0-F1 (no or minimal fibrosis) with paired biopsies and known duration of infection.
|
|
| |
 |
|
| |
Poynard is reporting here that in patients with HCV alone and little or no fibrosis their fibrosis progression rate per year stopped whether they were a non-responder or sustained responder. Since the biopsies were performed 20 months apart, you don't know what might occur regarding the fibrosis progression rate in 2-3 years or longer for non-responders. Non-responders may start progressing after being off therapy for a while. How long off therapy does it take for progression to get going or to get back to baseline? I don't know of any data on this. But some doctors tell me they think the benefit can last for a little while. Follow-up biopsies should be helpful in evaluating this.
Poynard reported on an analysis of fibrosis progression rate per year in 679 patients with extensive fibrosis (F2, F3, F4) with paired biopsies and known duration of therapy. Poynard commented that the progression rates in this group were very high before therapy.
|
|
| |
 |
|
| |
Poynard said the sustained responders experienced a dramatic decrease or regression in fibrosis rate.
Fibrosis Stage Variation By Regimen
The percentage of patients with at least one stage change in fibrosis METAVIR score. Again, the biopsies were 20 months apart.
- IFN 24 weeks: 12% of patients receiving this regimen experienced improved fibrosis, 65% stabilized, and 23% worsened
- IFN 48 weeks: 16% of patients improved fibrosis, 66% stabilized, and 18% worsened
- Peg 0.5 ug/kg: 22% improved, 62% stabilized, 17% worsened
- Peg 1.0 ug/kg: 21% improved, 62% stabilized, 16% worsened
- Peg 1.5 ug/kg: 17% improved, 65% stabilized, 18% worsened
- IFN/R 24 wks: 20% improved, 66% stabilized, 14% worsened
- IFN/R 48 wks: 20% improved, 66% stabilized, 14% worsened
- Peg 0.5/RBV: 23% improved, 67% stabilized, 10% worsened
- Peg 1.5/RBV: 23% improved, 57% stabilized, 20% worsened
- Peg 1.5/R*: 24% improved, 68% stabilized, 8% worsened
*With Optimized weight based dosing
So far there does not appear to be any difference between the percent of patients showing improved or stabilized fibrosis stage between most of the regimens. In particular, there is no difference between Peg 1.5 with optimized weight based RBV dosing, Peg 1.5 with RBV but without weight based RBV dosing, and standard IFN + RBV for 48 weeks.
Again, Poynard did not present any data on the statistical significance of differences between groups in his slides. But he pointed out orally that there was a significant difference between the 8% worsening in the Peg 1.5+ optimized RBV arm compared to the 14% experienced by IFN/RBV 48 weeks arm. But, he did not comment on the point that the Peg 0.5/RBV arm was 10% compared to 8% with optimized RBV dose & higher PegIntron dose. Although, the biopsies were only 20 months apart and so some patients, as Poynard points out, may continue to improve further.
Factors Associated With Absence of Extensive Fibrosis at 24 Months
n=2861, (20 months between biopsies), multivariate analysis
- The baseline fibrosis stage (F0, F1) had the most impact. Patients with little or minimal fibrosis (stage F0, F1) had an 88% reduced risk for having extensive fibrosis in the second biopsy 20 months after the first biopsy and after therapy (Odds Ratio 0.12, p<0.001)
- Achieving a sustained virologic response had the second most impact reducing risk for extensive fibrosis on the 2nd biopsy by 64% (OR 0.36, p<0.001)
- Age lower than 49 had the third most impact reducing risk by 49% (OR 0.51, p<0.001)
- Interestingly, Body Mass Index (<27) had the fourth most impact by reducing risk by 35% (OR 0.65, p<0.001)
- Baseline activity (A0, A1: patients with little or no activity) had the fifth most impact by reducing risk by 30% (OR 0.70, p<0.02)
- Viral Load <3.5 million reduced risk by 21% (OR 0.79, p=0.03)
I think the most interesting from the above data is that body mass index had an effect on outcome, Having more body mass increased risk. Expectedly, low viral load and achieving a sustained response were significant factors in reducing risk for having significant fibrosis in the 2nd biopsy.
Predictability of SVR After 12 week PCR Response
Poynard reported data similar to found with Pegasys+RBV on the predictability of sustained response based on the viral load response at 12 weeks. The analysis included 174 patients from the database who received PegIntron 1.5+RBV. 90% (n=120) who were PCR negative at week 12 achieved a sustained response. 26% who had a 2 log or greater reduction in PCR (n=23) achieved a sustained response. And 0 patients with <2 log reduction in viral load (n=31) at week 12 achieved a sustained response. The Pegasys analysis on using 12-week PCR response to predict outcome was more extensive and can be read in the NATAP AASLS report on this topic.
Can Cirrhosis Be Reversed?
153 patients with cirrhosis were included in this analysis. Poynard called these results surprising-- 49% (n=75) reversed cirrhosis. In the first biopsy 153 patients had F4 stage fibrosis (cirrhosis). In the second biopsy 23 patients had regressed to stage 3 (f3), 26 patients regressed to stage 2 (F2), 23 patients regressed to stage 1 (F1). And 78 patients still had stage 4. Poynard did comment on the sample size of liver taken in biopsy alluding to the limitations this presents.
Using a univariate analysis Poynard found the following significant factors in reversing cirrhosis:
using a reinforced regimen which I think he defined as IFN for greater then 24 weeks which I assume means or includes 48 weeks IFN/RBV and PegIntron/RBV regimens translates into a greater likelihood of reversing cirrhosis
achieving a sustained response (33% vs 15%) increases chance of reversing cirrhosis
reduction of activity grade in the second biopsy after therapy was a factor. 45% of patients with activity grade of A0/A1 in second biopsy reversed cirrhosis compared to 23% who did not have activity grade of A0/A1
Another study using Pegasys monotherapy presented by Jenny Heathcote showed patients with cirrhosis could improve their histology (a histologic response in this study was defined as a decrease of at least 2 points on the 22-point Histological Activity Index). 30% using Pegasys montherapy achieved a sustained response vs 8% using standard interferon.
www.natap.org/2001/sep/can_cirrhotics090401.htm
|
|
| |
|
 |
 |
|
|