Elmar Jaeckel, M.D., Markus Cornberg, M.D., Heiner Wedemeyer, M.D., Teresa Santantonio, M.D., Julika Mayer, M.D., Myrga Zankel, D.V.M., Giuseppe Pastore, M.D., Manfred Dietrich, M.D., Christian Trautwein, M.D., Michael P. Manns, M.D., and the German Acute Hepatitis C Therapy Group
ABSTRACT
(Notice: Because of its potential clinical implications, this article is being published early [on October 1, 2001]. It will appear in the November 15 issue of the Journal. Click on "PDF of this article" for the full text.)
Background - In people who are infected with the hepatitis C virus (HCV) chronic infection often develops and is difficult to eradicate. We sought to determine whether treatment during the acute phase could prevent the development of chronic infection.
Methods - Between 1998 and 2001, we identified 44 patients throughout Germany who had acute hepatitis C. Patients received 5 million U of interferon alfa-2b subcutaneously daily for 4 weeks and then three times per week for another 20 weeks. Serum HCV RNA levels were measured before and during therapy and 24 weeks after the end of therapy.
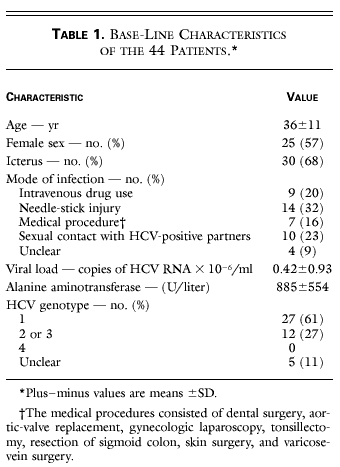
Results - The mean age of the 44 patients was 36 years; 25 were women. Nine became infected with HCV through intravenous drug use, 14 through a needle-stick injury, 7 through medical procedures, and 10 through sexual contact; the mode of infection could not be determined in 4. The average time from infection to the first signs or symptoms of hepatitis was 54 days, and the average time
from infection until the start of therapy was 89 days. At the end of both therapy and follow-up, 42 of the 43 patients who have completed follow-up (98 percent) had undetectable levels of HCV RNA in serum and normal serum alanine aminotransferase levels. Levels of HCV RNA became undetectable after an average of 3.2 weeks of treatment. Therapy was well tolerated in all but one
patient, who stopped therapy after 12 weeks because of side effects.
Conclusions - Treatment of acute hepatitis C with interferon alfa-2b prevents chronic infection.
The average time from infection to the first signs or symptoms of disease was
54 days (range, 15 to 105), and the average time from infection until the
start of therapy was 89 days (range, 30 to 112).
Current therapies for chronic infection eliminates the virus in only 54 to 56 percent of cases of chronic infection. An alternative approach is to treat the acute infection early with the goal of preventing progression.
Two pieces of evidence suggest that early treatment can prevent the progression of chronic infection. First,in patients with acute human immunodeficiency virus (HIV) infection, antiretroviral therapy sufficiently decreased the viral load to allow the patientsą immune systems subsequently to control viral replication (the authors ate referring to the Rosenberg data which merely suggests that HIV can be controlled by treatment during acute infection; the long-term effects are unclear). Second, early control of viral load in a murine model of lymphocytic choriomeningitis virus infection enabled the host ąs immune system to clear the virus and thus prevent the development of chronic infection. In contrast, if viral replication is not controlled early, virus-specific CD4 T cells and CD8 T cells are deleted from the T-cell repertoire by apoptosis or are rendered anergic. The strong responses of CD4 T cells 19,20 a d CD8 T cells to acute HCV infection in humans are similar to those in the the murine model of lymphocytic choriomeningitis virus infection. These strong immune responses during acute infection are weakened if viral replication is not controlled.
Safety
Therapy was well tolerated in all patients except the one who discontinued treatment. The spectrum of side effects was similar to that reported in previous trials of monotherapy with interferon alfa-2b. There were o serious adverse effects during therapy. The incidence of adverse effects was not higher during the initial 4 weeks of daily dosing than during the subsequent 20 weeks. None of the 43 patients who completed treatment required a dose modification. In all patients, Thrombocytopenia (mean platelet count at week 4, 161,000 ±43,000 per cubic millimeter, as compared with 250,000 ±66,000 per cubic millimeter before therapy; P<0.001) and leukopenia (mean leukocyte count at week 4,3900 ±1100 per cubic millimeter, as compared with 6600 ±1500 per cubic millimeter before therapy; P<0.01) developed during therapy and resolved after the end of therapy.
DISCUSSION
We found that early treatment of acute hepatitis C with i terferon alfa-2b alone prevented the development of chronic HCV infection in almost all patients.The response to i terferon alfa-2b was not influenced by the viral genotype,the patients ąsex, or the mode of transmission. The use of interferon alone rather than in combination with ribavirin ‹the standard therapy for chronic HCV infection ‹results in fewer side effects and lower costs. Furthermore, a 24-
week course of treatment was sufficient to preve t chronic infection. The suggested course of treatment is 48 weeks in patients with chronic infections with HCV genotype 1a or 1b.27,28 Even shorter periods of treatment might be sufficient in patients in whom serum levels of HCV RNA quickly become undetectable. There is o standard therapy for acute HCV infection. Several studies have evaluated the efficacy of interferon therapy for acute HCV infection, and all but one 8 reported a be eficial effect of treatment. However, these studies had substantial limitations. Some included primarily patients with trans-
fusion-associated HCV infection, some were very small, and others used interferon beta or treated patients for only a short period. Not all studies measured outcome on the basis of serum levels of HCV RNA 31,36-38 A larger prospective trial with a more representative group of patients was therefore needed.
We enrolled a large number of patients in a short period by conducting a nationwide study that included a suggested protocol for screening after suspected exposure to HCV.Although it is possible that our findings apply only to a subgroup of seriously ill patients,we believe that our methods of enrollment minimized the likelihood of a referral bias. We did ot include a placebo group. However, when our results are compared with those among patients who did ot receive therapy after acute HCV infection,the beneficial effect of early treatment is clear.
Although rates of conversion to chronic HCV infection of 50 to 55 percent have been found in some groups of children and young women, most studies have reported rates of 70 to 84 percent, even after the exclusion of patients with transfusion-associated HCV.
It is likely that about 30 percent of our patients would have had self-limited disease,regardless of whether they received interferon alfa-2b.So far, there are o means to ide tify such patients at presentation. Since the current treatment for chronic HCV infection eliminates the virus in only about half of cases, we suggest that all patients with acute hepatitis C should be treated.The value of other treatments, such as peginterferon alfa, should also be studied. Since all our patients had hepatitis, as defined by an elevated serum alanine aminotransferase level, our findings may ot apply to patients with HCV RNA in serum and ormal serum liver-enzyme levels after acute infection.However,we did not identify any such patients during our national study.