 |
 |
 |
| |
Opportunistic Conditions in the HAART Era
David Alain Wohl, MD
University of North Carolina AIDS treatment and Research Center
|
| |
| |
The most immediate and obvious benefit of potent HIV therapies has been the precipitous decline seen in opportunistic infections. In regions where HAART is available, conditions such as Pneumocystis pneumonia (PCP), cryptococcal meningitis and toxoplasmosis have faded to a background inhabited mostly by those who, for the usual reasons, are not benefiting from HAART or are unaware of their HIV infection. However, with the decline of opportunistic infections, other conditions have emerged as threats to the lives and quality of life of persons living with HIV infection. Most prominent among these are liver and kidney diseases but other conditions such as cardiovascular disease and cancers not typically associated with HIV have also been described (See Dr. Judy Aberg's report on risk of cardiovascular disease among HIV-infected persons). Several presentations at the 9th CROI examined the current causes of morbidity and mortality among HIV-infected patients.
Reisler and colleagues (Abstr 36) from the U.S. based Terry Beirn Community Programs for Clinical Research on AIDS (CPCRA) group retrospectively analyzed 5 large HIV treatment clinical trials involving over 3200 participants for the incidence (new cases) of serious clinical events and death. In these trials serious clinical events such as drug toxicity, HIV-related illnesses, and events not known to be due to HIV or treatment are recorded and graded. Grade IV events are those which are considered to be life threatening.
The subjects studied were enrolled in the trials from late 1996 to the end of 2001. Average age was 40 years, mean CD4 cell count was 241 (43-327), 84% were male, 42% African-American, 37% had a prior diagnosis of AIDS and a third of subjects were hepatitis C virus co-infected. The 30-month cumulative incidence rates were 10% for death, 13.5% for progression to AIDS and 27% of grade IV events. These 663 grade IV events were liver-related (6.1%), neutropenia (3.9%), pancreatitis (2.2%), anemia (2.1%), psychiatric (2.1%), cardiac-related (1.6%), cardiovascular (1.6%), kidney-related (1.5%), thrombocytopenia (1.2%) and hemorrhage (0.9%). Having such an event was associated with death to the same extent as progression to AIDS (about 6-fold greater risk). Certain grade IV event categories stood out as the most deadly. These were cardiovascular events, which carried a more than 9-fold greater risk of death, kidney disease with a 6-fold increase risk and liver disease associated with a 4-fold greater risk. Regarding the latter, persons who were co-infected with hepatitis B or C had 4 times the risk of liver problems compared to those who not co-infected.
Predictors of grade IV events were older age, treatment experience and low CD4 cell count. African-American subjects had an increased risk of anemia, neutropenia and kidney disease. This study suggests that the vacuum left by the decline in opportunistic infections has been filled by serious clinical events and that these may be related to adverse effects of treatment, concomitant diseases that may or may not be influenced by HIV and HIV treatment, and co-infection with viral hepatitis.
As described in the CPCRA study, kidney disease can be a major cause of morbidity among HIV-infected persons (L. Gardner. Abst 722-T). African-Americans, disproportionately affected by the HIV epidemic, also have high rates of hypertension and kidney disease. HIV infection and injection drug use have also been associated with renal failure. In a study of over 800 women participating in the HIV Epidemiology Research Study (HERS) study, the association of renal disease and hospitalization was examined. Renal lab abnormalities were defined as a single urinary protein analysis of 2+ or greater or a serum creatinine of 1.4 mg/dL. Hospitalization rates were found to be about 2 times higher for women with renal disease. Hypertension alone also carried a similar hospitalization risk. Even when hospitalization rates were restricted to events without evidence of renal disease in the hospital medical record, adjusted rate ratios remained significantly elevated for renal abnormalities and for hypertension.
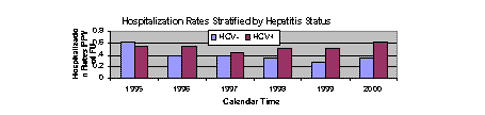
Liver disease has led to an increase in hospitalization of HIV-infected individuals at Johns Hopkins in Baltimore (K. Gebo, et al. Abst 660-M). Looking at hospital admissions from 1995 through 2000, each admit was classified as IDU related if one of the discharge diagnoses was cellulitis, osteomyelitis, abscess, bacteremia, or endocarditis and liver-related if one of the discharge diagnoses was GI bleed, hepatic encephalopathy, hepatitis, chronic liver disease, or necrosis of the liver. Over 3300 patients were included in the analysis; two thirds were male and three quarters African-American. From 1998 on, hospitalization rates for hepatitis C infected (HCV+) patients rose significantly.
|
|
 |
| |
Over 30% of hospitalizations in HCV+ patients were for liver-related and 27.4% were for IDU complications, whereas comparable rates of HCV- patients were 10.5% and 15.3%, respectively. Rates for hepatic complications increased significantly from 11.4% to 57.3% in this time period for HCV+ patients, whereas rates for IDU related complications remained relatively constant between 24-29%.
Can You Stop Prohylaxis For Toxoplasmosis, MAC, Cryptococosis
Can You Stop Prohylaxis For Toxoplasmosis, MAC, Cryptococosis
Lastly, how to manage the classic opportunistic infections of yore continues to be relevant in the era of HAART. For one thing, the much-needed attention to new causes of morbidity and mortality aside HIV-infected persons still do suffer from opportunistic infections (in a report from France, over half of the 535 deaths occurring during the first half of 2000 were due to opportunistic infections [C. Lewden, et al. Abstr 735-W]. Ten percent were due to hepatitis C and 7% were secondary to cardiovascular conditions). In addition, it has become clear that those subjects responding to HIV therapies can forego prophylaxis for opportunists such as PCP. Small studies have also suggested that discontinuation of prophylactic measures for other infections can also be accomplished, even among patients who already have experienced the infection. In a joint analysis the fate of patients in Europe discontinuing maintenance therapy for cryptococcal disease, mycobacterium avium complex (MAC), toxoplasmosis and cytomegalovirus (CMV) were described (O. Kirk, et al. Abstr 37). A total of 358 patients interrupted at least 1 type of maintenance therapy (162 for CMV, 103 for MAC, 75 for toxoplasmosis, and 39 for cryptococcosis). At discontinuation of prophylaxis/treatment, the CD4 counts were 231 (150-386) for CMV, 190 (129-290) for MAC, 320 (233-474) for toxoplasmosis, and 297 (180-392) for cryptococosis. Following a median follow-up of 29 months, 5 relapses were diagnosed: 2 relapses (CMV and MAC) were diagnosed after treatment was interrupted at a CD4 count below or only shortly above 100 cells/mm3; 2 relapses (CMV and MAC) were diagnosed after therapy was interrupted following CD4 counts above 100 cells/mm3 for 10 and 8 months, respectively, and 1 relapse (toxoplasmosis) was diagnosed after interruption at a CD4 count which had been above 200 cells/mm3 for 15 months. Those subjects with a CD4 cell count above 200 when discontinuing maintenance therapy had a much reduced risk of relapse compared to those quitting therapy at 100-200 cells.
In a related study from the Swiss Cohort Study Group, 17 subjects with a history of cerebral toxoplasmosis, ART-induced increase of absolute CD4 cell count to at least 200 and CD4 percentage of 14% sustained for more than 12 weeks, toxoplasmosis treatment for at least 6 months and gadolinium-enhanced cerebral MRI without signs of focal inflammation (S. Bertschy, et al. Abstr 633-W). Median absolute CD4 cell count at entry was 418 (260-580) and median CD4 percentage was 22% (15-30%). A HIV viral load below 50 copies was recorded in 14 subjects. One subject experienced a relapse of toxoplasmosis encephalitis. This patient had a nadir CD4 count that was 80, CD4 count at study entry was 307 (16%) and at the time of relapse 350 (14%). Plasma HIV RNA was below 20 copies/mL at study entry and at the time of relapse and prior toxoplasmosis treatment was in place for 4 years. This study indicates that discontinuation of toxoplasmosis therapy is largely successful following HAART-induced recovery of CD4 cells but that there is a small but important risk of relapse despite lack of inflammation on MRI at the time of therapy discontinuation.
|
|
| |
|
 |
 |
|
|