 |
 |
 |
| |
Does HIV Accelerate HCV Progression?
Reported by Jules Levin
|
| |
| |
Most knowledgeable researchers and doctors feel HIV accelerates HCV. There have been a number of clinical studies in patients finding accelerated progression, and there have been just a couple of studies finding HIV did not accelerate HCV progression. Laboratory or viral kinetics studies such as the one presented by Andrew Talal at this AASLD conference find coinfected patients have impaired responses to HCV therapy, and it¹s probably due to HIV impairing the immune system. At the Intl AIDS Conference in Barcelona this past Summer French researchers found HIV accelerated HCV progression by 1.5 fold. In the studies finding HIV accelerates HCV progression the increased progression rate ranges from 2-5 fold but the studies at the higher end of the range looked at patients with hemophilia who may have a greater risk of progression than HIV-infected without hemophilia. It appears we can¹t the question with certainty as there are so many variables including duration of HCV, the affect of HAART, when HAART was started, alcohol consumption, general health and lifestyle of the patient, age, and immunocompetence. The timing of HIV exposure relative to HCV exposure may play a role. Clearly, better natural history studies of HCV/HIV coinfection need to be conducted. Most knowledgeable researchers and doctors I know feel HIV accelerates HCV, and their feeling about the range of increased risk is from 2-fold to 3-4 fold; and the risk is probably related to the risk factors listed above. In an analysis of a number of studies, which was published in CID by Dr Graham she estimated HIV accelerates HCV by 3-4 fold. Some of the studies included looked at hemophiliacs.
At this AASLD conference Maurizio Bonacini presented a study at yesterday¹s oral session on HCV/HIV coinfection. In this session many of the studies were not well done, they were too small, and not well analyzed. There also appear to be some questions about Bonacini¹s conclusions. The aim of this study was to assess liver mortality in patients with HIV with or without viral hepatitis coinfection. In other words, does HIV accelerate death due to liver disease associated with HCV or HBV in these patients in this study. So, this study does not look at does HIV accelerate progression to cirrhosis, liver disease associated complications, or liver cancer.
474 patients with HIV were followed for a total of 8,300 patient months at the USC Clinic. The followup is only 2 years which may not be long enough to detect differences in outcomes. In was unclear whether the patients included in this study were all the clinic patients or a subgroup of patients referred to the hepatitis clinic. There could be a bias by looking at patients who are referred.
Mortality data were obtained from the Los Angeles County Epidemiology Unit. The use of death certificates, if that¹s what he used have flaws because certificate may not mention end stage liver disease as the cause of death. The post mortem exam may not look for this cause. Of the 473 patients with HIV 233 also had HCV, 73 were HbsAg positive, 154 had HIV alone (HbsAg and HCV RNA negative), and 14 patients had multiple hepatitis viruses.
Patients with HIV infection and no viral hepatitis had higher all-causemortality rates, compared to HCV/HIV or HBV/HIV coinfected patients by Kaplan-Meier curves. However, when these data were adjusted for CD4 counts, liver mortality was not significantly different in those coinfected with either HBV or HCV vs HIV alone. Furthermore, both all-cause and liver mortality curves for HCv/HIV and HBV/HIV groups were superimposable.
In the group of 320 patients with hepatitis C or B, initial CD4 count <200 and an average lifetime alcohol use >50 grams/day was associated with asignificantly higher liver mortality vs those with CD4 count >200 and alcohol use <50 g/day.
Liver mortality was also significantly higher in the subgroup of patients first evaluated in clinic prior to HAART (1996) vs those seen in 1996 or later. The significance of this finding is unclear and was not addressed in much detail. This finding raises another question. If you look only at the patients evaluated after 1996 would you find a different affect of HIV on hepatitis progression? Would the use of ART or HAART, or specific types of HIV drugs have an affect? This was not discussed by Bonacini.
The presence of all 3 factors (CD4 <200, alcolhol >50 g/day, evaluation prior to 1996) was associated with a 12-fold higher mortality risk compared to those with none of these factors. Age, gender, ethnicity, or risk factor for HIV were not associated with liver mortality. Bonacini concluded that in this study patients with HIV/HCV coinfection had survival similar to patients infected with HIV. Patients with HBV/HIV have the same liver mortality as patients with HCV/HIV coinfection. The 3 rask factors mentiioned above are independent risk factors for liver mortality. HIV patients without viral hepatitis have substantial liver mortality.
So, why did Bonacini find HIV did not accelerate HCV? 50% of the clinic population had HCV as reported above and that¹s a relatively high rate. If the USC clinic has a high percentage of patients who were infected by IVDU, perhaps I can speculate that they may not have benefited as much from HAART for a variety of reasons. If that is true the rate of death due to HIV might be higher. If the rate of death due to HIV is higher than would be expected which I think is reflected in the table below that might obscure the rate of death to hepatitisassociated liver disease. The rate of liver mortality might be higher in coinfected patients if the rate of death due to HIV were lower.
|
|
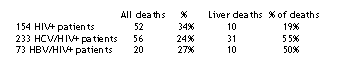 |
| |
|
 |
 |
|
|