 |
 |
 |
| |
HIV Healhcare Costs Driven by CD4 Count
Reported by Jules Levin
|
| |
| |
This study set out to identify the actual costs of care for HIV-infected patients with <50 Cd4s and 50-199 Cd4s compared to patients with higher Cd4 counts. Chen said healthcare costs for HIV-infected adults have been estimated by models but actal costs have not been reported.
In this study patients were from the University of Alabama HIV clinic. All direct costs within the UAB hospital system from 3/1/2000 to 3/1/2001 were included. These did not include physician professional fees. Medication costs based on 2001 averagw wholesaleprice. Physician/clinic costs based on 2001 Medicare CPT reimbursement rates, included inpatient and outpatient physician fees, and included all clinic-related costs (staff, building, etc). Other costs included lab costs, radiology, outpatient procedures including surgeries, home health, and outpatient infusion and injection fees.
Of the 635 patients included the average age was 35 yrs, 77% male, 59% caucasion, 62% MSM, 10% IVDUs, average CD4 count 364, average viral load 2.4 log (251 copies/ml), 27% with history of OI, and 80% on HAART.
The total annual average cost for patients:
|
|
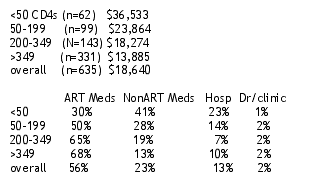 |
| |
The average annual costs are much higher for patients with <50 CD4s and 2.5 times as high as for patients with >349 CD4s. Medication costs are 75% of total costs. Medication costs increase as CD4s decline. Increase in CD4s are associated with decreased overall costs due to decreased cost in all cost components (p<0.0005). Hospitalization and nonART costs appear to increase the most as Cd4s decline and decrease the most as Cd4s increase. The authors conclude that physician/clinic costs do not increase but remain the same regardless of CD4 count and contribute 2% or less of costs.
|
|
| |
|
 |
 |
|
|