| |
Patients Can Remain Undetectable for 20 years on HIV Therapy
|
| |
| |
"Viral rebound after suppression with HAART: experience from 237 people with viral load < 50 cps/ ml followed for up to 4.4 years"
In this study, researchers looked to see if treatment-naive patients achieved <50 copies/ml and sustained good adherence how long could they maintain undetectable viral load -- would regimens have intrinsic ability to sustain viral load. They therefore studied the rate of viral rebound (break- through) in people who had not interrupted therapy. In studying patients in this study for a maximum of 4.4 years, they found viral rebound rate was about 3.7% per year. Of 237 patients in the study 13 had viral rebound; the total percent of patients experiencing failure was only 5.4%. Some patients may not have been adherent or may have taken an interruption without telling the study, and its possible the viral failure rate could have been lower. The viral failure rate decreases over time, but if it were to remain the same over time the researchers estimate that the median time before viral break- through would be approximately 20 years.
Fiona Lampe, Margaret A Johnson, Clive Loveday, Mike Youle, Darren Ransom, Caroline A Sabin, Mervyn Tyrer, Andrew N Phillips. Royal Free Centre for HIV Medicine, UCL, London, UK.
Introduction
It is known that current HAART regimens initially reduce viral load to < 50 copies/ mL in the majority of drug- naive people within 24- 32 weeks. Less is known about the long- term durability of this suppression, particularly in those that have achieved viral load < 50 copies/ mL. Few existing clinical trials
are sufficiently long- lasting to provide this information. A recent report from the Frankfurt Clinic Cohort found extremely low rates of viral break- through (ie viral rebound despite the patient continuing to take therapy) for up to 3.3 years in those who had achieved viral load < 50 copies/ mL (1). We sought to
confirm this result and extend the length of follow- up time under study.
Methods
The lower limit of quantification of viral load (using the Roche RT- PCR based approach) used for people at the Royal Free clinic was 400 copies/ mL from 1996 to 1998 and then has been 50 copies/ mL from 1998 onwards. We followed all 237 people from the Royal Free Hospital Clinic who were naive to
antiretrovirals when they started a HAART regimen (3 nucleosides including abacavir, 2 nucleosides + 1 non- nucleoside reverse transcriptase inhibitor (NNRTI) or 2 nucleosides + a protease inhibitor (PI - including ritonavir
boosted), reached a viral load < 400 copies/ mL (within 32 weeks) and also reached a viral load < 50 cps/ ml without having previously experienced viral rebound. The reason for not insisting on viral load < 50 copies/ mL by 24
weeks was that the more sensitive assay had not always been used by this time, due to its more recent introduction. Viral rebound was defined as two consecutive values >400 cps/ ml. When viral rebound was associated with stopping of all drugs, follow- up time was right censored at this point.
Results
Twenty one percent of subjects were female; main HIV exposures were homosexual (60%) and heterosexual (34%) sex. The median age at start of HAART was 35 years. HAART was started on a median date of Dec 98 (IQR Sep 96 - Nov 00). Baseline median (IQR) viral load was 5.3 (4. 8 - 5. 7) log
copies/ mL and CD4 count 193 (75 - 302) /mm 3 . Nucleoside drugs in the initial regimen were zidovudine/ 3TC 126 (53%), stavudine/ 3TC 76 (32%) and other 35 (15%). Other drugs were nevirapine 58 (25%), efavirenz 44 (19%), indinavir 56
(24%), ritonavir 21 (9%), nelfinavir 50 (21%) and ritonavir boosted PI 29 (12%).
Median time from start of HAART to first measured value 50 cps/ ml was 180 days. 1342 viral load measures were made over a total 347 person- years of follow- up after the first viral load < 50 cps/ ml - a median of one measure per 13.5 weeks (median over all patients of 3.8 per year). Maximum follow- up
was 4.4 years. Overall 13 people (5. 4%) experienced viral rebound (break- through) on therapy (rate 0.037 per person- year) representing one person with viral rebound per 26.7 person- years of follow- up (Table 1). There was a (non- significant) trend towards lower rebound rate with increasing time from start of HAART.
Comment
In this analysis we sought to assess what would be the rate of viral break- through in people naive to therapy before starting HAART in whom a viral load < 50 copies/ ml had been achieved. It is known that drug toxicity and inconvenience of pill- taking schedules mean that it will be difficult for patients to remain continuously on therapy indefinitely. A key question,
however, is whether regimens would have sufficient sustained intrinsic efficacy, even if it were possible to maintain good adherence indefinitely.
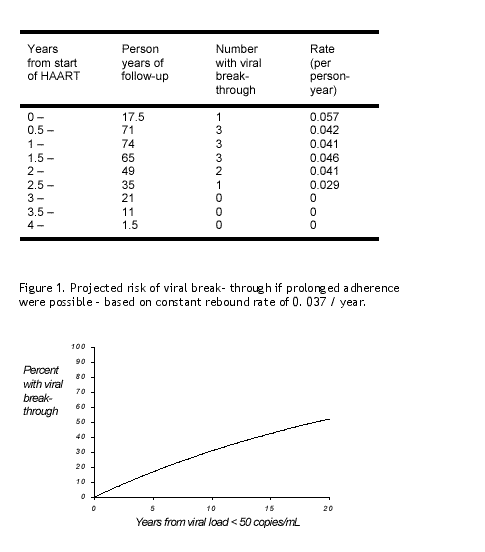
We therefore studied the rate of viral rebound (break- through) in people who had not interrupted therapy. As confirmation of findings from a similar analysis of a different clinic cohort, in Frankfurt (1), we observed a low rate (~ 3. 7% per year) of viral breakthough up to 4.4 years from start of therapy in people who had achieved viral load < 50 copies/ mL. Some viral rebound that we observed may have been due to periods of non- adherence that were not recorded, rather than actual break- through, so the true intrinsic breakthrough rate may be even lower. The break- through rate appears to decrease over time, consistent with the previous study (1). If the rate we observed of 0.037 per year were to continue indefinitely, the median time before viral break- through would be approximately 20 years (Figure 1). Considering currently
available drugs there must be severe doubts as to whether people will be able to consistently adhere to their antiretroviral regimen for such long periods, but the hope is that future regimens will be sufficiently less toxic and more convenient to make this possible.
Conclusion
Viral suppression on HAART for people who were naive to therapy and in whom a viral load < 50 copies/ mL is achieved is proving extremely durable in those that can tolerate these regimens over long periods.
Acknowledgement
This work has been undertaken within an MRC Co- operative Group "HIV infection: new insights in the therapeutic era" based at Royal Free and University College Medical School. We thank Clinton Chaloner for invaluable assistance with extracting clinical data from case notes.
Reference 1. Phillips AN, Miller V, Sabin C, Cozzi Lepri A, Klauke S, Bickel M, Doerr HW, Hill A, Staszewski S. Durabilty of HIV- 1 Viral Suppression Over 3.3
Years with Multi- DrugTherapy in Previously Drug- Naive People. AIDS 2001; 15: 2379.
Table 1.
Numbers of person- years of follow- up, numbers of people with
viral break- through and rate of viral breakthrough by years from
start of HAART in people achieving viral load < 50 copies/ mL
without previous viral failure/ rebound.
| |
| |
 |
| |
|
|
|