 |
 |
 |
| |
Atazanavir Maintained Patient Utility and Improved Quality of Life, Comparing Favorably to LPV/RTV: 24-Week Data from BMS 043
|
| |
| |
Poster at 9th EACS in Warsaw, Poland
Jayanti Mukherjee, PhD; Ying Wu, PhD; Linda Odeshoo, MA; Thomas Kelleher, PhD; Uche Iloeje, MD; Anne Cross, PhD; Michael Giordano, MD. Pharmaceutical Research Institute, Bristol-Myers Squibb Company, Wallingford, CT, USA
BACKGROUND
- Highly Active Anti-Retroviral Therapy (HAART) has significantly reduced HIV-related morbidity and mortality in recent years.1 As patients live longer, maintaining patient quality of life while on HAART has become an important issue.
- Atazanavir is a new, safe, and potent protease inhibitor (PI) recently approved by the US FDA. It is currently under review by the EMEA.
- Antiretroviral efficacy has been demonstrated for non-boosted atazanavir in naïve patients (034 study) and boosted atazanavir in experienced patients (045 study).
OBJECTIVE
To evaluate effect of atazanavir therapy on patient quality of life (QOL) and utility compared to LPV/RTV in study 043.
STUDY POPULATION AND DESIGN
- BMS 043 is a randomized, multinational, open-label, controlled two arm study. Patients who failed one prior PI-HAART regimen with CD4 >50 cells/mm 3 and HIV RNA >1,000 c/mL were randomized to ATV 400 mg or LPV/RTV combined with two NRTIs.
- A total of 300 subjects were randomized and 290 were treated.
- Patient utility was measured by the EQ-5D questionnaire and quality of life by MOS-HIV. Both questionnaires were validated and have been widely used in HIV studies.
- Questionnaires were administered at baseline, Week 24, and end of study. This analysis presents data at baseline and Week 24.
METHODS
MOS-HIV
Patient quality of life was measured by MOS-HIV questionnaire. Developed from the SF-20, there is extensive evidence to support the reliability, validity, and responsiveness of the MOS-HIV.3
The MOS-HIV questionnaire, which consists of 35 questions, measures several dimensions of health.
- Domains include General health perception, Pain, Physical functioning, Role functioning, Social functioning, Mental health, Energy/fatigue, Health distress, Cognitive function, and Quality of life.
- Furthermore, two summary scores physical health summary and mental health summary can be derived.
- The MOS-HIV scores are transformed on a 0-100 scale where higher scores indicate better health using a standard algorithm.
EQ-5D
Patient utility was measured by EQ-5D. EQ-5D is a preference-based measure that yields a single number, or health index score to represent respondent’s subjective health status.
- The index is based on responses on five questions on mobility, self-care, usual activities, pain/discomfort, and anxiety/depression. The score is anchored from 0 to 1, representing death and full health.
- The index score is derived by using a standard algorithm. It also yields an overall general health index via a Visual Analog Scale (VAS), where higher scores indicate better health.
Methods
Mean change from baseline score was evaluated for both utility and QOL. Mean change of ≥2 points in MOS-HIV summary scores was considered clinically meaningful. We used criteria of ≥2 points to determine clinical significance for MOS-HIV domain scores. We also used criteria of ≥5 points as used in some analyses.
RESULTS
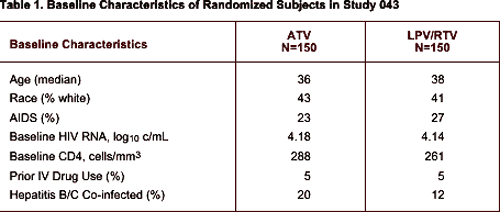
Patient population characteristics at baseline are summarized in Table 1.
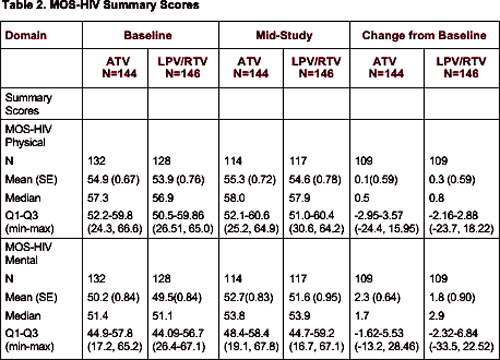
Baseline scores were comparable in both treatment arms. After 24 weeks, using the criteria of 2 points or more to determine clinically meaningful changes in MOS summary scores, atazanavir therapy was associated with clinically relevant improvement in mental health sub-scale (2.3 increase) vs. none in LPV/RTV arm (Table 2).
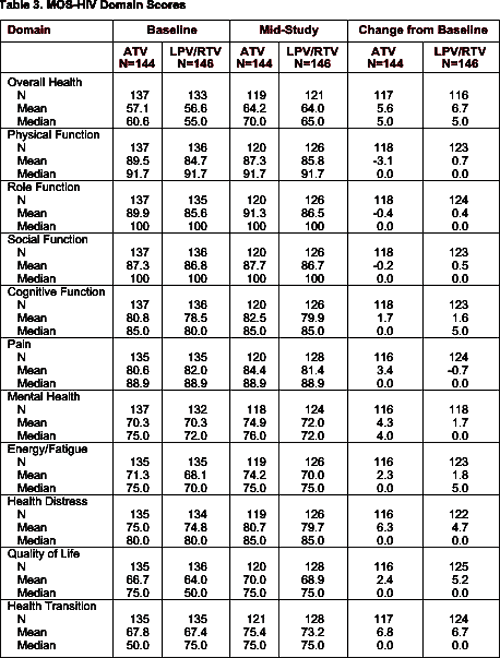
Using the criteria of 2 points or more to determine clinically meaningful changes in MOS domain scores, at week 24, atazanavir therapy was associated with clinically relevant improvement in 6 domains (general health, pain, mental health, energy/fatigue, health distress, and quality of life) and worsening in physical function. LPV/RTV improved 3 domains (general health, health distress and quality of life) (Table 3).
If a 5-point criteria was used for domain scores, atazanavir therapy improved patients’ general health, and health distress, while LPV/RTV improved general health and quality of life.
The mean health utility score was 0.85 for atazanavir arm, and 0.86 for LPV/RTV arm at baseline. After 24 weeks, ATV patient utility increased to 0.89, while LPV/RTV patient utility dropped to 0.84.
VAS data indicated similar trends. Baseline VAS scores were 82.54, 83.09, respectively. At week 24, ATV patients increased to 87.05 (mean increase of 3.31), while LPV/RTV patients increased to 85.88 (mean increase of 2.3).
AUTHOR’S CONCLUSIONS
In this study, while non-boosted ATV demonstrated less antiviral efficacy than the boosted LPV/RTV regimen, from the quality of life perspective, quality of life data suggest that atazanavir therapy was associated with clinically relevant quality of life improvements in certain areas.
While anchored around death/perfect health, an increase of about 0.05 in utility score observed in atazanavir-treated arm is important. A recent meta-analysis estimates utility scores associated with various stages of HIV infection range from 0.70 for AIDS, 0.82 for symptomatic HIV infection, to 0.94 for asymptomatic infection.6 The utility difference between AIDS and symtomatic HIV is only 0.12.
Several strengths associated with atazanavir, such as ease of administration related to low pill burden, QD, and a better safety profile, may have played a part in the quality of life advantages we observed. More data are needed to further confirm these trends.
|
|
| |
| |
 |
|
| |
| |
 |
|
| |
| |
 |
|
| |
|
 |
 |
|
|