| |
Carotid Intima-Media Thickness in Heavily Pretreated HIV-Infected Patients
|
| |
| |
In the current issue of the journal JAIDS (Journal of Acquired Immune Deficiency Syndromes 2003; 32(5):490-4930), a French research group (Gilles Chironi and colleagues) reports on measuring carotid intima-media thickness in HAART treated HIV-infected individuals. IMT is a measure of the intima thickness of the carotid artery. It is measured by a non-invasive ultrasound technique and has been found to be predictive of clinical cardiovascular events in symptomatic and asymptomatic individuals. In HIV+ persons, studies looking at IMT have had conflicting results but it could be because studies have not followed individuals long enough or because studies have had too many confounding factors. Two studies were presented at the February 2003 Retrovirus Conference. One study found increased IMT in HIV+ persons but a second with short-term followup of patients did not find increased IMT. You can see these study results in the NATAP Report: http://www.natap.org/2003/Retro/day56.htm
The current study discussed in this report finds an increased IMT in HIV-infected and therefore a potential increased risk for heart disease when lipids are higher in HIV than in HIV negative individuals. However, when lipids in HIV- persons are similar they do not find increased IMT. Patients' time on therapy, however, is limited and the study investigators do not tell us how long lipids have been elevated. Read the author's discussion at the end of this paper for their interpretation.
Ultrasound measurement of carotid intima-media thickness (IMT) is of special interest in this population because it reflects early atherosclerosis. Therefore, these researchers measured IMT in a sample of heavily pretreated HIV-infected patients prone to atherosclerosis (cases) and in two non-HIV-infected groups (controls) without or with metabolic disturbances similar to those of the patients.
Cases (n = 36) were consecutively selected from heavily pretreated HIV-infected patients with at least one cardiovascular risk factor: hypoHDLemia, current smoking, hypercholesterolemia, hypertension, diabetes, and/or
previous cardiovascular disease. The cases had HIV-infection for an average 11 years. Current average Cd4 count was 352, but during the past 3 years the lowest average Cd4 count was 98. Cases had a cumulative time on ART of 73 months; 34 patients had PI therapy for a cumulative total of 31 months on PI therapy; cases had been on NRTI therapy for average cumulative total of 35 months; and 11 cases had been on NNRTI therapy for average cumulative total of 11 months.
Two groups of non-HIV-infected controls (matched to cases according to average values for age, sex ratio, and smoking status) without (control group 1) or with (control group 2) blood lipid and glucose disturbances similar to those of cases were randomly chosen from two large pools of subjects . Control group 1 included 36 healthy subjects chosen from the AXA Study cohort. Control group 2 included 36 subjects chosen from patients referred for cardiovascular risk assessment.
|
|
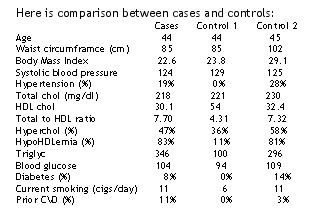 |
| |
The average IMT was measured in a plaque-free far wall segment of the right common carotid artery with a B-mode ultrasound imager (ATL Ultramark 9, HDI). The IMT image, on >1 cm of the longitudinal carotid length, was
frozen in telediastole (ECG triggering) and analyzed with an automated edge detection program (Itec System, Idata). IMT was measured once in each subject and calculated as the average of at least 100 measurements along the
length of vessel explored. Lucite phantom precision of this technique was 2.4%, and the intraobserver reproducibility was on average 4.3%.
RESULTS
Carotid IMT was greater in cases than in control group 1 (p < .05). After excluding the three highest IMT values for the cases, this IMT difference was reduced to marginal nonsignificance (p = .09). None of the
cases with the highest IMT values had a prior cardiovascular event. The IMT difference between cases and control group 1 remained significant after adjustment for age (p < .01), sex (p < .05), body mass index (p < .01), waist
circumference (p < .01), systolic blood pressure (p < .01), current smoking (p < .01), and prior cardiovascular disease (p < .05) and after excluding cases with prior cardiovascular disease (0.54 vs. 0.48 mm, respectively; p < .05). The IMT difference between cases and control group 1 was not significant after adjustment for blood glucose level, triglyceride levels, or total-to-HDL cholesterol ratio. IMT was not different between cases and control group 2
before and after adjustment for the aforementioned factors.
A positive association of IMT with age existed for the cases and control group 1 before and after adjustment for all risk factors (p < .01 and p < .05, respectively) but not for control group 2. A positive association of IMT with waist circumference existed for the cases before (p < .001) and after adjustment for age (p < .05) and after adjustment for all risk factors (p < .05) but not for both control groups. A positive association of IMT with the
total-to-HDL cholesterol ratio existed for the cases after adjustment for age and for all risk factors (p < .05) but not for both control groups. No association existed between IMT and factors of HIV infection or type and duration of antiretroviral therapy for the cases.
DISCUSSION By Authors
Using a highly precise and well-validated technique of IMT measurement, we found that IMT was greater in HIV-infected patients than in non-HIV-infected subjects without metabolic disturbances. Such increased IMT does reflect early alteration of the large artery wall in HIV-infected patients, but it is not synonymous with atherosclerosis, because we measured IMT in the common carotid artery free from plaque and not at multiple sites including bifurcation and the internal carotid artery that would incorporate atherosclerotic lesions. However, even IMT measured in the common carotid segment can be considered as an indicator of the global atherosclerotic burden in one individual. Moreover, on the basis of our previous work, one can assume that the small increase (0.07 mm) in IMT in patients compared with non-HIV-infected subjects without metabolic disturbances represents about a twofold
increase in the Framingham coronary risk. However, such an IMT difference disappeared when comparison of the above groups was adjusted for blood lipid and glucose levels. Likewise, IMT did not differ between HIV-infected
patients and non-HIV-infected subjects with similar metabolic disturbances. Therefore, increased IMT in HIV-infected patients can be reasonably attributed to lipid and glucose disturbances. In contrast, we did not find direct associations of highly active antiretroviral therapy and HIV infection parameters with IMT, but the meaning of this negative result is questionable. Indeed, our study was not designed for testing such associations, because our patients had all experienced antiretroviral treatment.
Another interesting result was that positive associations of IMT with the total-to-HDL cholesterol ratio and waist circumference existed independent of other risk factors for HIV-infected patients. The influence of the total-to-HDL
cholesterol ratio on atherosclerosis has been previously described, probably due to the HDL cholesterol transfer in the vessel wall. For our patients, elevation of the ratio was mainly the consequence of hypoHDLemia.
HypoHDLemia may be a result of the hypolipidemia of long-standing (mean, 11 years) HIV infection or result from hypertriglyceridemia, which is also seen in long-standing HIV disease. Elevated triglyceride levels can also arise as an adverse effect of protease inhibitor treatment.
Our study is limited by its cross-sectional nature, its small sample size, and the lack of measurement of key factors such as plasma insulin levels or flow-mediated vasodilation. Therefore, larger longitudinal studies are required to
confirm our findings and better interpret their mechanisms.
|
|
| |
| |
|
|
|