| |
Diabetes in HIV & HCV/HIV; prevalence, immunology
|
| |
| |
Written by Judith Aberg, MD, Washington University, St Louis, Missouri and ACTG
This meeting had little to offer in the way of enhancing our current knowledge of HIV and its association with diabetes. There were 2 oral abstract presented during the metabolic complications of HIV session.
Abstract: H-1715. Understanding the Association between DM and HIV and HCV Infections in the Era of HAART.
A.A. BUTT1,2,3, S.L. FULTZ1,2,3, M. SKANDERSON2,3, D. KELLEY1, A.C. JUSTICE1,2,3
1 Univ. Pittsburgh, Pittsburgh, PA, 2 VA Pittsburgh, Pittsburgh, PA, 3 Veterans Aging Cohort Study, Pittsburgh, PA.
It remains unclear if HIV and its therapy are associated with the increase risk of diabetes mellitus (DM) versus the fact that people with HIV are living longer and developing age-related complications such as DM and heart disease. However, several studies have demonstrated glucose intolerance and insulin resistance in HIV infected patients taking protease inhibitors as well as HIV seronegative controls taking protease inhibitors. Increased risk of DM has been reported in patients receiving HAART for HIV infection in large retrospective databases and among patients with HCV. Given the large number of HIV infected patients co-infected with HCV, Dr. Butt and colleagues sought to describe the relationship between the 2 infections and DM.
They conducted a respective review of an observational Veteran’s Administration (VA) database on 33,280 HIV+ veterans and 38,232 HIV- controls in care between October 1996 and September 2001. Demographics, dates of HCV, HIV, DM, entry into care and alcohol and drug diagnoses data was retrieved. Having a history of DM prior to 1996 was excluded. Cox regression analysis was used to determine risk by estimating hazard ratios for DM separately among those with and without HIV infection.
The average age was 44 years with 97% male. The percent of patients having DM by presence or absence of infection is as follows:
--HIV positive, HCV negative 13%
--HIV positive, HCV positive 19.3%
--HIV negative, HCV negative 20.5%
--HIV negative, HCV positive 24.2%.
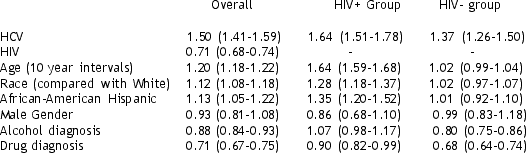
The overall In univariate analyses of the entire sample, HCV, age, and minority race were associated with increased risk of DM; HIV, alcohol abuse and drug abuse were associated with decreased risk of DM (p<0.05). After adjustment for other factors and stratification by HIV status (see table), the risk of DM associated with HCV was greater among HIV infected individuals than among those not infected with HIV (HR: 1.64 vs. 1.37). Similarly, the risk of DM associated with age (HR: 1.64), and Black (HR: 1.28) and Hispanic race (HR: 1.35) were only significant among those with HIV infection. Alcohol and drug use diagnoses were not associated with DM, which may reflect malnutrition and lower body mass index (BMI) in these patients.
|
|
| |
| |
 |
|
| |
| |
The investigators concluded HIV infection appears to increase the risk of DM associated with established risk factors including HCV infection, age, and minority race. Given the increased risk of DM occurring in individuals with co-infection, it seems reasonable that clinicians intensify their efforts for screening for DM in this population. It is interesting to note that the cohort of HIV positive, HCV negative patients were less likely to have DM compared to those without either infection or HCV infection alone. The investigators were unable to evaluate the effects of BMI, family history, individual ART regimens and duration of HCV and HIV disease. It is difficult to make any causal relationship between HIV and HCV. Why was HIV itself associated with the lowest number of cases of DM? This is in contrast to other studies suggesting HIV itself and/or its therapies are associated with DM. The fact that older age and minority race was associated with DM is not surprising as this is consistent with the American general population.
Note from Jules Levin: other studies have shown about 6% DM in general population and 13% in HIV+, but as mentioned above, why did HIV+ individuals have lowest rate of DM? This study in VA population found 13% in HIV+ but 20% in HIV-neg/HCV-neg. Perhaps, something is wrong with data (not analyzed well) or the VA population is sick. The study does find similarly to other studies that HCV is associated with DM, and HCV/HIV co-infected persons are at greater risk for insulin resistance and diabetes.
Abstract: H-1716. B7-H1 and IL-10 in HIV Infection: Association with Progression of Disease and Development of Diabetes in HAART-Treated Patients.
M. BIASIN1, M. SCHENAL1, M. CESARI2, F. FASANO1, A. BEARDO1, D. TRABATTONI1, B. GOLDBERG3, A. GORI2, M. CLERICI1
1 Università Milano, Milano, Italy, 2 Malattie Infettive H. L. Sacco, Milano, Italy, Milano, Italy, 3 3International DNCB Study Group, CA, USA, S. Francisco, CA.
Diabetes developing in HIV infected patients taking HAART may be secondary to host inflammatory responses to therapy. A decreased interleukin-10 (IL-10) and increased tumor necrosis factor alpha (TNF-_) cytokine response is associated with diabetes in the elderly. The ligation of B7-H1 to its receptor on T cells results in the preferential production of IL-10. This study investigated B7-H1 and IL-10 expression in HIV infected individuals who develop diabetes as a consequence of HAART.
HIV antigen- (gag) and mitogen- (LPS) stimulated IL-10 and TNFa production and intracellular concentration (ICC), as well as B7-H1, CD80 and CD86 expression and mRNA were measured in peripheral blood mononuclear cells (PBMC) of 22 healthy controls (HC) and 20 HIV infected, HAART-treated individuals in whom diabetes did (N=10; DM) or did not (N=10; no DM) develop. The duration of HIV infection was 10 years in both groups with those with DM having received an average of 5.4 years of HAART compared with 6.3 years for those without DM. 7/10 with DM received a PI compared with 6/10 without DM. The median CD4 count was 541 cells in the DM group compared with 444 cells in the non –DM group.
The investigators demonstrated the following: 1).B7-H1 expression and mRNA were augmented in HIV patients; 2) increased IL-10 production in these patients is induced by B7-H1-expressing CD14+ cells; 3) an inverse correlation is detected between B7-H1 expression and CD4 cell counts, whereas the upregulation of B7-H1 is directly associated with HIV plasma viremia; 4) B7-H1/CD80 and B7-H1/CD86 mRNA ratios are increased in PBMC of HIV patients compared to HC. Comparison between diabetic and non diabetic HAART-treated patients showed that: 1) IL-10 production by PBMC was lower in DM patients; 2) B7-H1-expressing and IL-10-producing CD19+ cells were diminished in DM patients; and 3) TNFa ICC was augmented in CD4+ T cells of DM individuals.
They concluded that in HIV infection, aberrant antigen presentation by APCs exhibit increased B7-H1 expression that can result in IL-10 overproduction, which is partly responsible for T lymphocytes unresponsiveness and loss of protective immunity; while low IL-10 production is a risk factor for diabetes in HIV infected individuals on HAART. While I agree that this cytokine pattern is associated with diabetes in the elderly and was shown in those patients developing DM on HAART, I cannot attribute these findings to HAART itself. Obviously not everyone develops DM and as these investigators show, it is only those with these host responses that develop DM. How do we know that this cytokine pattern developed as a consequence of HAART and was not pre-existing in these individuals. Were these individuals more likely to develop DM regardless of HIV and its therapy? Although the investigators showed differences between the HIV subjects compared with HIV seronegative controls, they did not show differences of HIV without DM compared with the HIV seronegative control population. They compared the whole HIV cohort regardless of presence or absence of DM to the controls. Further study is warranted to understand the significance of these findings.
|
|
| |
| |
|
|
|