| |
Care of patients with hepatitis C and HIV co-infection: Consensus Panel Recommendations
|
| |
| |
AIDS: Volume 18(1) 2 January 2004 pp 1-12
Soriano, Vincenta; Puoti, Massimob; Sulkowski, Markc; Mauss, Stefand; Cacoub, Patricee; Cargnel, Antoniettaf; Dieterich, Douglasg; Hatzakis, Angelosh; Rockstroh, Jurgeni
From the aService of Infectious Diseases, Instituto de Salud Carlos III, Madrid, Spain; bClinica di Malattie Infettive e Tropicali, Spedali Civili, Brescia, Italy; cDivision of Infectious Diseases, The Johns Hopkins University School of Medicine, Baltimore, MD, USA; dCenter for HIV and Hepatogastroenterology, Düsseldorf, Germany; eService de Medecine Interne, Hôpital de la Pitié-Salpetrière, Paris, France; fDivisione di Malattie Infettive, Ospedale Luigi Sacco, Milan, Italy; gDepartment of Medicine, The Mount Sinai Medical Center, New York, NY, USA; hDepartment of Hygiene and Epidemiology, Athens University Medical School, Athens, Greece; and iDepartment of Medicine, University of Bonn, Bonn, Germany.
Introduction
Liver disease caused by chronic hepatitis C virus (HCV) infection is now a leading cause of morbidity and mortality among HIV-infected patients in the developed world, where classic opportunistic complications of severe immunodeficiency have declined dramatically as a result of the widespread use of potent antiretroviral therapies. Over the past few years, several consensus reports have addressed the issue of viral hepatitis and HIV infection. In 2000, a group of experts in the field were invited to join the HCV-HIV International Panel. The first consensus conference took place in Paris. Two years later, the large amount of new information on HCV and HIV, as well as important changes made in the guidelines for using antiretroviral drugs, prompted us to organize another consensus conference, which was held in Barcelona in the summer of 2002. Following international recommendations for the development of clinical guidelines, the meeting was planned as a full one-day workshop in which nine experts in the field of HIV and viral hepatitis discussed a total of nine questions, which were selected in advance as the most relevant and currently conflicting topics in the management of chronic viral hepatitis in the setting of HIV infection. A draft was written and circulated among panel members during the following months. Finally, in a second meeting that took place in February 2003, a final consensus was reached, and is presented here. The statements are graded according to the Infectious Diseases Society of America scoring system, with minor changes (see Table 1).
|
|
| |
| |
 |
|
| |
| |
Influence of hepatitis C virus infection on HIV disease progression and response to antiretroviral therapy
Background
The state of permanent immune activation provided by chronic HCV infection might act deleteriously in HIV-positive individuals, favouring HIV transcription within infected cells and the more rapid destruction of CD4 T lymphocytes. On the other hand, the immune recovery seen after beginning effective antiretroviral therapy could be partly blunted in individuals with HCV infection as a result of similar mechanisms, or through the infection of immune cells by HCV itself.
Clinical studies that have examined whether there is an influence of HCV on HIV disease progression show conflicting results. Whereas some have demonstrated an association between HCV infection and faster HIV disease progression, others have not. In the Swiss cohort, HIV-positive individuals with HCV infection progressed faster to AIDS and death than those who were HCV negative. Some of the available data support a direct negative impact of HCV on HIV disease progression, although to a slight extent. In addition, HCV may negatively influence HIV disease in indirect ways, such as making the discontinuation of antiretroviral treatment more frequent because of an increased risk of liver toxicity.
Panel recommendation
HCV might act as a co-factor for HIV disease progression by several mechanisms. First, unspecific immune stimulation driven by chronic HCV infection might enhance HIV replication. Second, the infection of immune cells by HCV could favour CD4 T-cell depletion and partly blunt the immune recovery that follows successful antiretroviral therapy. Third, HCV could compromise the benefit of antiretroviral drugs as a result of a higher incidence of liver toxicity and treatment discontinuation. However, a negative impact of HCV on HIV disease progression has not been recognized in some large clinical-epidemiological studies. SCORE: C.II
Candidates for anti-hepatitis C virus treatment
Background
All HIV-infected individuals should be screened for HCV antibodies in the serum or plasma. HCV-antibody-negative but HCV-RNA-positive cases may exist, mainly in patients with severe cellular immune suppression as a result of HIV. Those with repeatedly elevated aminotransferase levels should be tested for HCV load and HCV genotype, in order to assess anti-HCV therapy.
All HIV-positive individuals with chronic HCV infection should be considered as candidates for anti-HCV therapy, given their higher risk of progression to end-stage liver disease and their higher risk of liver toxicity after beginning antiretroviral therapy, compared with HIV-negative individuals. As the response to anti-HCV therapy is dependent on the CD4 cell count, ideally it should be prescribed only when the CD4 cell count is above 350 cells/mL, a threshold that is relatively easy to obtain in most instances when antiretroviral therapy is used properly. Besides, this is currently the immunological cut-off to begin antiretroviral therapy in drug-naive patients. In individuals with CD4 cell counts between 200 and 350 cells/mL, and already under long-term antiretroviral therapy, the decision to treat HCV might be considered taking into account other factors, such as the estimated length of HCV infection, the severity of liver disease, the extent of suppression of HIV replication, and classic predictors of response to anti-HCV therapy, such as HCV genotype and HCV load.
Finally, anti-HCV therapy should be deferred in individuals with CD4 cell counts of less than 200 cells/mL, because the response rate is very low in this subgroup of patients. Moreover, the risk of opportunistic infections in the short term may be high, and may worsen with anti-HCV therapy. Therefore, they should be treated with antiretroviral therapy and receive prophylaxis for opportunistic infections as a priority. Later on, when their CD4 cell counts have risen and their plasma HIV-RNA level is under control, the prescription of anti-HCV therapy should be assessed again.
Patients with previous liver decompensation (ascites, gastrointestinal bleeding, hepatic encephalopathy, etc.) should not be treated, given the higher risk of serious side-effects using the current drugs, pegylated interferon (peg-IFN) and ribavirin. These patients should be assessed for liver transplantation. However, patients with compensated cirrhosis (Child-Pugh class A) must be treated.
Individuals with a previous history of severe neuropsychiatric disorders should not be treated, because IFN can exacerbate these conditions. Individuals currently engaged in a heavy alcohol intake or illegal drug addiction practices should delay treatment, whereas all efforts should be devoted to put them into detoxification programmes. Patients on methadone are acceptable candidates for anti-HCV therapy. Up to one third of patients may need adjustments in methadone dosage. Ideally, a multidisciplinary team, including experts in addiction medicine, psychologists/psychiatrists and infectologists should take care of these patients.
Following recent National Institutes of Health Consensus Conference Recommendations, individuals with repeated normal liver enzymes might benefit from current anti-HCV therapy, particularly those infected with HCV genotypes 2 or 3. However, more data on liver damage in this subgroup of HCV-HIV- co-infected patients are needed to balance the cost-benefit of anti-HCV therapy in them.
In drug-naive individuals with HCV-HIV-co-infection, chronic hepatitis C should be treated first if the CD4 cell count does not require the initiation of antiretroviral therapy. However, in patients with CD4 cell counts greater than 350 but high plasma HIV-RNA levels (i.e. above 50,000 copies/ml), it is not clear whether the suppression of HIV replication should be done at first, deferring anti-HCV therapy to the moment when undetectable HIV viraemia is attained. In these patients, a possible greater efficacy of anti-HCV therapy then should be balanced with a higher risk of interactions between antiretroviral agents and anti-HCV drugs.
Panel recommendation
All HIV-infected individuals should be screened for HCV antibodies. Those with positive HCV serology should be tested for HCV-RNA. Individuals with positive HCV-RNA should be considered as candidates for anti-HCV treatment. A plasma HCV load and genotyping should be requested before initiating therapy. Treatment should be provided to patients with repeated elevated alanine aminotransferase levels, CD4 cell counts greater than 350, relatively low plasma HIV-RNA levels (i.e. less than 50 000 copies/ml), no active consumption of illegal drugs or high alcohol intake, and no previous severe neuropsychiatric conditions. Treatment in patients with normal alanine aminotransferase levels should be carried out in the context of study protocols or when a liver biopsy has proved the presence of clinically significant fibrosis, i.e. F2 or above. Treatment in patients with CD4 cell counts below 350 should be prescribed cautiously. The treatment of choice is the combination of peg-IFN plus ribavirin. SCORE: A.II
Liver biopsy before recommending treatment
Background
Liver histology allows the staging of HCV hepatic damage and predicts in the short-mid term who will develop cirrhosis. At the same time, it may rule out other causes of liver damage, such as haemochromatosis, alcohol-related steatosis, Wilson disease, autoimmune hepatitis, etc., although these conditions may also be recognized by other non-invasive means.
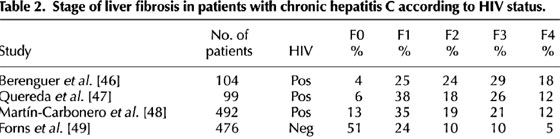
The value of liver biopsy before prescribing anti-HCV therapy is under debate. This controversy may be less justified in HCV-HIV-co-infected patients, in whom the rate of significant liver fibrosis is much higher than in HCV-monoinfected individuals (see Table 2). A priori, anti-HCV therapy will be almost always justified considering the extent of histological damage in HIV-HCV-co-infected patients. Moreover, nearly half of HCV-HIV-co-infected patients may show unexpected cirrhosis or pre-cirrhosis. The main predictor of advanced fibrosis stages seems to be the estimated duration of HCV infection. On average, nearly half of patients will have cirrhosis 25 years after the first HCV exposure. If we consider that the mean age of HCV-HIV-co-infected patients is currently 40 years, and that most are former intravenous drug users who began to exchange needles when they were on average 20 years old, it should be expected that many of them will currently show significant liver fibrosis. Therefore, if not treated, a rapid increase in liver complications among HIV-infected individuals should occur over the next decade.
|
|
| |
| |
 |
|
| |
| |
Those who defend performing a liver biopsy before treating chronic hepatitis C in HIV-co-infected patients argue that the side-effects, the risk of interactions with antiretroviral drugs and the relatively low efficacy of current anti-HCV therapy in this population are major limitations that only justify prescribing the medication for those who really need it histologically. However, given that liver damage is a dynamic process and fibrosis progression rate is accelerated in HCV-HIV-co-infected patients, supporters of this point of view should be reminded that if treatment is not offered to patients with a lack of or only minimal fibrosis, liver biopsy should be repeated at 2-3 year intervals. However, this option will face opposition from many patients and may increase the costs significantly. Accordingly, a recent analysis has pointed out the cost-effectiveness of therapy in co-infected individuals [55].
55. Kuehne F, Bethe U, Freedberg K, Goldie S. Treatment for hepatitis C virus in HIV-infected patients: clinical benefits and cost-effectiveness. Arch Intern Med 2002, 162:2545-2556.
Panel recommendation
The role of liver biopsy for treatment decision purposes is controversial in HIV-HCV-co-infected patients. The patients' reluctance to accept it or other difficulties should not defer the prescription of anti-HCV therapy once it is considered appropriate, given the faster progression to end-stage liver disease in co-infected patients. When the histological information is available for patients with HCV genotypes 1 or 4, treatment could be deferred if there is no fibrosis (F0), or in patients with F1 willing to accept a second follow-up liver biopsy. In patients with normal transaminase levels, liver biopsy should be performed before prescribing therapy. SCORE: C.III
Treatment of chronic hepatitis C in HIV-positive patients
Background
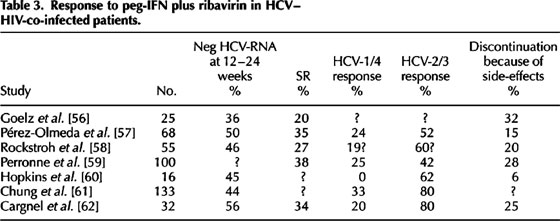
Available data from interim analysis of large ongoing clinical trials and from a few studies already completed show that response rates to anti-HCV therapy are lower in HIV-co-infected patients, even using the new peg-IFN formulations with ribavirin (Table 3). Overall, sustained response rates are in the range of 20-35%, which is approximately half the responses seen in HIV-negative individuals. It should be noted that both early virological responses and end-of-treatment responses are equally much lower in HIV-HCV-co-infected patients. Moreover, relapses also seem to be more frequent
|
|
| |
| |
 |
|
| |
| |
The reasons why anti-HCV therapy provides a poor response in the setting of HIV infection may be varied (Table 4). As both peg-IFN and ribavirin act, at least partly, as immunomodulatory agents, subtle immune defects derived from HIV infection might negatively impact on the performance of these drugs, even in patients with high CD4 cell counts and undetectable plasma HIV-RNA levels under antiretroviral therapy.
|
|
| |
| |
 |
|
| |
| |
In addition, there is a high rate of anti-HCV treatment discontinuation in some of the trials conducted in HIV-co-infected patients, even surpassing 25% of individuals recruited. Although it may reflect a higher rate of serious adverse events in this population compared with HIV-negative individuals, in whom it is usually less than 15%, it might also reflect that some HIV physicians are not quite familiar with the management of side-effects of anti-HCV therapy. Efforts to minimize side-effects with pre-emptive symptomatic treatments and the appropriate management of complications are thus critical to ensure the completion of anti-HCV therapy in most patients.
Panel recommendation
The overall response to anti-HCV therapy is lower in patients co-infected with HIV. Sustained response rates of 40-60% are seen in patients with HCV genotypes 2 or 3, but lower than 25% in those with HCV genotypes 1 or 4. Both early virological responses and relapses are less and more frequent, respectively, in co-infected patients compared with HCV-monoinfected individuals. The benefit of extending therapy (more than 6 months for HCV genotypes 2 or 3; and more than 12 months for HCV genotypes 1 or 4) in early virological responders should be examined in clinical trials. Moreover, treatment adherence should be considered a critical factor for the attainment of response and must be encouraged actively over the whole treatment period. SCORE: A.II
Monitoring the response to anti-hepatitis C virus therapy in HIV-positive patients
Background
Almost all patients who will clear HCV with anti-HCV treatment show an early virological response after beginning therapy. Therefore, an early assessment of serum or plasma HCV-RNA titres after starting treatment may permit the identification of those who would benefit from prolonging therapy and those who would not. In HIV-negative patients, those who show a decline in HCV-RNA levels greater than 2 logs or undetectable levels at 12 weeks of therapy are those who will eventually reach a sustained response. In contrast, almost none of those who show HCV-RNA declines of less than 2 logs at 12 weeks achieve that goal. Therefore, anti-HCV therapy may be discontinued at 12 weeks considering these virological criteria in early non-responders. This principle to guide HCV therapy might spare side-effects and costs in individuals with no chance of cure. In HIV-HCV-co-infected patients these considerations should be regarded as even more crucial, because interactions between antiretroviral drugs and anti-HCV therapy are frequent, and issues related to poor compliance in individuals under polymedications are of much relevance.
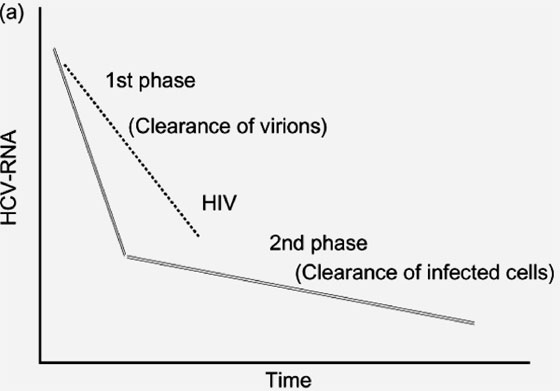
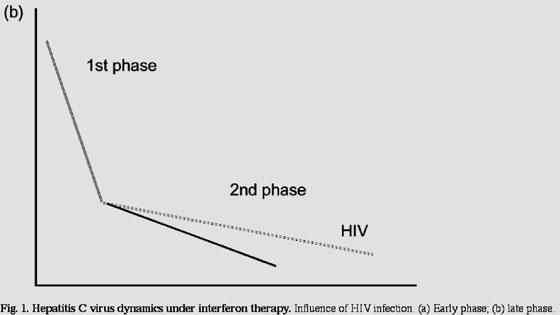
Kinetic studies suggest that HCV clearance after beginning therapy with IFN may be delayed in the setting of HIV infection (see Fig. 1a). Therefore, concern exists about the reliability of the principle of a 2-log reduction in HCV-RNA at 12 weeks: it might not work in HCV-HIV-co-infected patients. However, preliminary data suggest that despite a slower decay in HCV-RNA noticed in HIV-co-infected patients after beginning anti-HCV therapy, all patients who will reach a sustained response show a decline greater than 2 logs at 12 weeks on therapy. Therefore, the principles guiding anti-HCV therapy in HIV-negative individuals may also apply to HIV-co-infected patients (see Fig. 2). However, patients with high HCV loads may show an early good virological response, but may not reach undetectable viraemia at week 24, but will clear HCV much later. This subgroup of patients represents less than 3% of HCV-monoinfected individuals, but may be larger among HIV-co-infected patients, in whom higher baseline HCV-RNA titres are frequent and slower HCV-RNA decays on treatment have been described.
|
|
| |
| |
 |
|
| |
| |
|
|
| |
| |
 |
|
| |
| |
There is a second phase of clearance of HCV-RNA in individuals on prolonged anti-HCV therapy, which accounts for the steady destruction of infected cells (hepatocytes). A slower decay in the setting of HIV infection (see Fig. 1b) could explain why the early discontinuation of therapy might result in higher relapse rates in virological responders. Recent data support this notion, and make it necessary to reconsider how long anti-HCV therapy should be extended in HIV-HCV-positive early virological responders. This observation seems to apply particularly to HCV genotype 3, because relapses are uncommon in HIV-negative individuals infected with this genotype, whereas it occurs in up to a third of HIV-HCV-co-infected patients who receive anti-HCV therapy for only 6 months, following what is recommended in HIV-negative individuals. Further studies examining extended periods of anti-HCV therapy (i.e. 12 months in HCV genotypes 2 and 3, and up to 18 months in HCV genotypes 1 and 4) should be conducted in early virological responders to examine whether this strategy may reduce their chance of relapse.
Recent reports have shown that HCV-monoinfected patients who do not clear HCV-RNA on anti-HCV treatment, might benefit from long-term therapy with IFN alone. Maintenance therapy with IFN may provide histological improvement and even reduce the risk of hepatocellular carcinoma, and is currently being investigated as an alternative approach in large trials in HCV-monoinfected patients (HALT-C and EPIC). Whether this strategy may be considered in some HIV-HCV-co-infected individuals with advanced fibrosis who did not respond virologically to anti-HCV therapy should be investigated further. The use of lower doses of peg-IFN (half those recommended as first line) may improve tolerance and facilitate long-term administration of the drug.
Panel recommendation
Early virological response to anti-HCV therapy predicts the chance of sustained response in HIV-co-infected patients as it does in HCV-monoinfected individuals. Moreover, the use of an early timepoint for treatment decision-making seems to be equally appropriate in co-infected patients. Only patients showing a decline in serum HCV-RNA levels greater than 2 logs at 12 weeks on therapy will have chance of reaching a sustained response. Therefore, treatment might be discontinued in the rest. This is of particular relevance, given the concern about the risk of toxicity derived from interactions between anti-HCV therapy and antiretroviral drugs. SCORE: C.II
Management of adverse effects of anti-hepatitis C virus therapy in HIV-positive patients
Background
The side-effects of anti-HCV medications are common, and may be grouped into five main categories: influenza-like symptoms (headache, fever, asthenia, myalgias, decreased appetite); haematological abnormalities (mainly anaemia); neuropsychiatric disorders (depression, irritability, insomnia); gastrointestinal symptoms (nausea, diarrhoea); and inflammation at injection sites. In addition, other adverse events may develop more rarely, such as alopecia and thyroid dysfunction. Overall, they lead to treatment discontinuation in approximately 15% of HCV-monoinfected patients, and to dose reductions of either peg-IFN or ribavirin in another 20-25%. Higher treatment discontinuation rates have been recorded in some studies conducted in HIV-co-infected individuals. The lack of expertise in the management of HCV treatment-related side-effects by the doctors in charge as well as insufficient information given to patients may both have contributed to explain the high drop-out rates. These aspects should therefore be properly addressed in the future.
The haematological abnormalities may be caused either by peg-IFN or ribavirin. Anaemia caused by ribavirin is typically mild and caused by extravascular haemolysis, and is accompanied by an increase in reticulocytes. Although ribavirin dose reductions may allow the incidence of anaemia to be reduced, the usefulness of recombinant erythropoietin has been highlighted in these patients. Supplements of folinic acid are advisable. Otherwise, the dose of ribavirin should be reduced to half when the haemoglobin level drops below 10 g/dl, and it should be discontinued if it falls below 8.5 g/dl. However, ribavirin exposure seems crucial for attaining a higher sustained response rate, particularly in patients carrying HCV genotype 1; therefore any effort to keep patients on adequate doses of the drug (i.e. using recombinant erythropoietin) should be favoured.
Leukopenia, especially neutropenia and less frequently lymphocytopenia, may develop with peg-IFN. In particular, patients should be informed in advance of the risk of decreases in their CD4 cell counts. In most instances they affect the absolute CD4 cell number but not the percentage of these cells. Moreover, it reverses after discontinuing IFN therapy. With respect to neutropenia, the use of therapeutic growth factors, such as granulocyte colony-stimulating factor may be considered and eventually preferred over reducing peg-IFN doses, particularly in patients with HCV genotype 1.
Panel recommendation
Anti-HCV therapy causes fever, malaise, asthenia, depression, etc. in the majority of cases. Patients should be informed in advance about these side-effects and how to prevent and manage them (paracetamol for influenza-like symptoms, etc). The treatment of depression should be considered as soon as symptoms begin to develop. Peg-IFN may produce significant CD4 T-cell declines and neutropenia, which are reversible after discontinuing it. Ribavirin may cause anaemia within the first 12 weeks of therapy. Doctors should improve their expertise in the management of these side-effects, trying to keep patients on therapy as long as no serious toxicities develop. SCORE: A.I
Toxicity caused by interactions between antiretroviral drugs and anti-hepatitis C virus therapy. How to avoid it?
Background
As anaemia is a frequent side-effect of ribavirin use, attention should be paid to those patients who are taking zidovudine, also known to produce anaemia. In patients with zidovudine-related anaemia this drug should thus be discontinued before prescribing ribavirin. Alternatively, close monitoring of haemoglobin values over the first 6 weeks of therapy is warranted.
Mitochondrial damage results from the inhibition of mitochondrial polymerase gamma by nucleoside analogues. Ribavirin can enhance the intracellular concentrations of phosphorylated didanosine metabolites, and result in a higher risk of toxicity. Several cases of pancreatitis or lactic acidosis have been reported, and a warning from the US Food and Drug Administration has been released advising on the risk of giving ribavirin and didanosine concomitantly. Therefore, patients who begin treatment with ribavirin should avoid the use of didanosine. Alternatively, the close monitoring of serum lactate and amylase levels are warranted, and patients should be informed in advance of any symptoms potentially associated with lactic acidosis (abdominal discomfort, fever, malaise, nausea, vomiting). The role of stavudine in the development of lactic acidosis in these patients has also been highlighted in the APRICOT trial, although to a lesser extent.
More recently, cases of hepatic decompensation, some of them fatal, have been reported in individuals receiving ribavirin with didanosine. All were individuals with cirrhosis, and hypothetically didanosine and ribavirin acted synergistically, leading to liver failure. Therefore, the concomitant administration of didanosine and ribavirin should be contraindicated in patients with advanced liver fibrosis.
Finally, several observations have highlighted the fact that ribavirin could potentiate subcutaneous fat loss when used concomitantly with some nucleoside analogue, mainly stavudine. In this form, severe weight loss mimicking the progression of lipoatrophy could be another characteristic side-effect derived from the interaction of ribavirin and antiretroviral drugs. Patients should be informed in advance about the risk of this complication and, when possible, drugs with a lower lipodystrophic profile should be prescribed.
Panel recommendation
Interactions between antiretroviral drugs and ribavirin may be harmful. Given the higher risk of pancreatitis and lactic acidosis in all treated patients as well as of liver decompensation in cirrhotic individuals, didanosine should be avoided when taking ribavirin. On the other hand, zidovudine should be used with caution when ribavirin is given, because both may produce anaemia. Patients should be advised of the possibility of experiencing severe weight loss, mimicking a rapid progression of lipoatrophy, probably as a result of a potentiation of mitochondrial damage in the subcutaneous fat tissue taking ribavirin and some nucleoside analogues. SCORE: A.II
Hepatotoxicity of antiretroviral drugs
Background
Grade 3 or 4 liver enzyme elevations occur on average in 5-10% of patients who start triple antiretroviral therapy. The rate is significantly higher in patients with underlying chronic hepatitis C. Moreover, some drugs (i.e. nevirapine, ritonavir at full doses) cause hepatotoxicity more frequently than others. Therefore, liver function tests should be closely monitored in individuals who initiate antiretroviral treatment, particularly when some of the drugs mentioned above are administered to patients with chronic hepatitis C.
Cumulative toxicity may explain the steady liver enzyme elevations when using some drugs. If not apparent shortly after beginning therapy, it may become manifest later, often after 6 months on therapy. This has been seen with drugs such as nevirapine.
Liver enzyme elevations after antiretroviral treatment may occur by other mechanisms than the direct injury of the drug(s) prescribed. Immune reconstitution phenomena and hypersensitivity reactions may account for some additional cases. In patients with low CD4 cell counts or high HIV-RNA titres, successful anti-HIV therapy may enhance immune responses to a degree that hepatic cells harbouring HCV antigens may be recognized and destroyed massively. As long as the patient remains asymptomatic and transaminase levels do not rise above 10-fold the limit of normal values (grade 4 toxicity), treatment could be continued with the close monitoring of laboratory values, because a return of liver enzymes to baseline values occurs in most cases. These episodes of immune-related hepatitis, however, are quite rare. On the other hand, allergic phenomena that may develop shortly after exposure to nevirapine, abacavir or amprenavir may be accompanied by liver enzyme elevations in the context of a more generalized reaction. The presence of underlying chronic hepatitis C does not seem to play a role in the occurrence of this phenomenon.
Liver toxicity may also occur as a consequence of mitochondrial damage in patients receiving nucleoside analogues, particularly stavudine and didanosine. Histological features of hepatic steatosis are frequent in this setting and are more common in women and obese individuals.
Panel recommendation
Liver enzyme elevations after beginning antiretroviral therapy are more frequent in patients with underlying chronic hepatitis B and C. Therefore, drugs with more hepatotoxic profiles (i.e. nevirapine, ritonavir) should be used cautiously in co-infected patients. Treatment should be discontinued in patients with symptoms or grade 4 increases in aminotransferase levels. In certain cases, immune reconstitution phenomena may lead to increases in transaminase levels after starting potent anti-HIV therapy. The close monitoring of these patients during the first weeks may enable them to remain on therapy, because they experience a progressive resolution of liver abnormalities without discontinuing treatment. SCORE: A.II
Liver transplantation in HIV-co-infected patients
Background
HIV-infected patients with end-stage liver disease develop classic complications of decompensated cirrhosis, including ascites, jaundice, gastrointestinal bleeding, spontaneous peritonitis and encephalopathy. The only treatment available at this stage is orthotopic liver transplantation (OLT). Initial attempts before the introduction of highly active antiretroviral therapy (HAART) regimens provided very poor results. Those reports showed that only a small percentage of transplanted HIV-positive recipients maintained good organ function, whereas most experienced an accelerated course to AIDS. Since the introduction of HAART, HIV-infected liver transplant recipients have improved their short and mid-term survival. Now, the outcome of transplantation is no longer compromised as long as HIV infection is controlled with HAART in the post-transplant period.
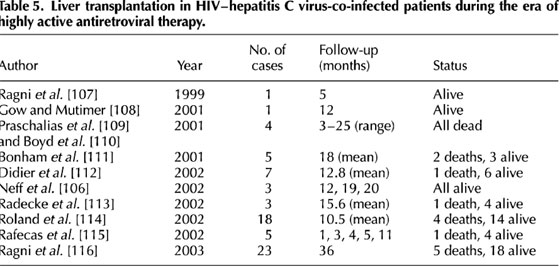
Table 5 summarizes the experience with OLT in HIV-infected patients during the HAART era. Although cases came from different institutions, the criteria used for liver transplantation were quite similar. In general, candidates did not have prior history of opportunistic infections, CD4 cell counts greater than 100 and undetectable plasma HIV-RNA on HAART. Alternatively, in subjects with detectable viremia, they had available drugs for successful treatment in the post-OLT period. There were at least 17 patients with end-stage liver disease due to chronic hepatitis C who underwent OLT and 12 (70%) remained alive, some of them up to 2 years. In one of the largest series, Roland et al. in 18 cases of OLT in HIV-positives has reported a survival rate at 1 year similar to that found at the United Network for Organ Sharing (UNOS), 92% versus 87.9%, respectively. Similar rates were seen for graft survival, 83% versus 81.4%. These findings have been confirmed at 3 years in a more recent report
|
|
| |
| |
 |
|
| |
| |
The information available so far may be summarized in the following points: (i) The risk of opportunistic infections in the post-transplant period is very low when HIV replication is well controlled with HAART, maintaining most cases with undetectable viral loads. Furthermore, CD4 cell counts remain stable or even increase with HAART. Therefore, the use of standard immunosuppressive therapy in patients with well-controlled HIV infection does not increase their susceptibility to opportunistic infections or malignant conditions. (ii) Cyclosporin and tacrolimus can inhibit HIV replication in vitro and mycophenolate mofetil may potentiate the antiviral efficacy of abacavir. The benefit of these interactions is currently being explored. (iii) There are important pharmacokinetic interactions between some antiretroviral drugs, protease inhibitors (PI) and non-nucleoside reverse transcriptase inhibitors and immunosuppressive agents, mainly cyclosporin and tacrolimus. PI may increase the levels of cyclosporin and tacrolimus, whereas non-nucleoside reverse transcriptase inhibitors may reduce their levels, because of their opposing effects over the cytochrome p450. These interactions have caused some episodes of acute rejection in patients who stopped PI while taking calcineurin-inhibitors. Therapeutic drug monitoring of immunosuppressive agents is mandatory when taking antiretroviral drugs. (iv) Hepatotoxicity associated with a HAART regimen can also be observed in liver allografts, and liver function should be closely monitored. (v) HCV recurrence is very frequent after OLT, and leads to cirrhosis in nearly 20% of cases within 5 years. The rapid progression of HCV-related liver disease in HIV-infected recipients represents a major drawback and the main reason for a shorter life expectancy of these patients. Standard anti-HCV therapy must be prescribed as early as possible (1-3 months after OLT) following the recommendations stated in point 3. In addition, other approaches such as pre-emptive therapy (i.e. using IFN shortly before transplantation in the case of living donors) should be explored; and (vi) As survival in the waiting list seems to be much shorter in HIV-co-infected patients, strategies to make available liver transplantation sooner after a patient's assignment to this procedure should be underlined.
Panel recommendation
All HIV-infected patients with end-stage liver disease as a result of HCV should be considered as candidates for liver transplantation as long as they do not have advanced HIV disease. In those with severe immunodeficiency (< 100 CD4) the control of HIV replication and immune restoration should be prioritized. The evaluation and the pre and postoperative medical management of HIV-positive candidates for OLT must include an interdisciplinary team composed of a hepatologist, infectologist, surgeons, psychologists, social workers and members of alcohol, heroine and cocaine detoxification programmes. HIV-positive candidates should have CD4 cell counts greater than 100 and plasma HIV-RNA levels below 200 copies/ml, or the chance of becoming undetectable using optional drugs for successful treatment after transplantation. Moreover, they should have abstained from the consumption of alcohol and illegal drugs for at least 6 months. Patients with a good immunological response to HAART but a previous history of AIDS-related opportunistic infections or neoplasms (including Kaposi's sarcoma, cervical carcinomas and anal squamous carcinomas) deserve special attention, given the potentially higher risk of relapses of those conditions using immunosuppressors. SCORE: B2.
Sponsorship: This work was supported in part by grants form AIES, Schering-Plough and RIS (Red project 173).
|
|
| |
| |
|
|
|