 |
 |
 |
| |
Weight-Based Ribavirin Improves SVR Rate for Patients >125 kg (275 lbs)
|
| |
| |
Reported by Jules Levin
AASLD, Oct 27-31, 2006, Boston, MA
Response to Peginterferon alfa-2b and Ribavirin for Chronic Hepatitis C in Patients With Body Weight ≥125 kg: Results From the WIN-R Trial
I. M. Jacobson,1 R. S. Brown, Jr,2 B. Freilich,3 N. Afdhal,4 P. Kwo,5 J. Santoro,6 S. Becker,7 A. Wakil,8 L. Griffel,9 C. Brass,9 for the WIN-R Study Group1
1Center for the Study of Hepatitis C, Weill Medical College of Cornell University, New York, New York; 2Columbia University Medical Center, New York, New York; 3Baptist Medical Center, Kansas City, Missouri; 4Beth Israel Deaconess Medical Center, Boston, Massachusetts;
5Indiana University School of Medicine, Indianapolis, Indiana;6 Atlantic Gastroenterology Associates, Egg Harbor Township, New Jersey; 7Austin Gastroenterology, PA, Austin, Texas; 8East Bay Liver Clinic, San Francisco, California; 9Schering-Plough Research Institute, Kenilworth, New Jersey
AUTHOR CONCLUSIONS
- Patients with very high body weight (≥125 kg) and high BMI (mean, 41.0 kg/m2) achieved SVR rates similar to those of patients weighing <125 kg.
- Patients weighing ≥125 kg were at least as likely to achieve an SVR as patients weighing ≦125 kg with weight-based ribavirin therapy.
- Patients weighing ≥125 kg were much more likely to achieve an SVR with weight-based ribavirin than with flat-dose ribavirin.
- Low rates of anemia and neutropenia and low dose-reduction rates probably reflect lower levels of ribavirin exposure.
- These results suggest that severe obesity should not preclude consideration of antiviral therapy for patients with chronic hepatitis C.
ABSTRACT
Purpose: In WIN-R, a US study of >4900 HCV patients from community and academic sites that prospectively compared PEG-IFN alfa-2b 1.5 _g/kg/wk + flat dosing (FD; 800 mg/d) or weight-based dosing (WBD; 800-1400 mg/d) of ribavirin (RBV), sustained virological response (SVR) rates were significantly greater with WBD than FD of RBV (AASLD'05). WBD patients weighing >105 to <125 kg received RBV 1400 mg/d and had SVR rates similar to other WBD patients. The current study evaluated SVR rates among patients weighing >125 kg, for whom data are limited, who entered the study as protocol exceptions.
Methods: In WIN-R, patients were randomized to PEG-IFN alfa-2b 1.5 _g/kg/wk (max: 150 _g/wk) + FD RBV 800 mg/d or WBD RBV: <65 kg, 800 mg/d; 65-<85kg, 1000 mg/d; 85-<105 kg, 1200 mg/d; 105-125 kg, 1400 mg/d. Genotype 1 (G1) patients received 48 wks of therapy, and G2/3 patients were randomized to 24 or 48 wks of therapy. All patients were monitored for 24 wks post-treatment. HCV RNA levels were determined by PCR (TaqMan/SPRI, LLQ 29 IU/ml) at wks 0, 24, 48 and 72. RBV dose reductions and discontinuation were required for hemoglobin <10 gm/dL and <8.5 gm/dL.
Results: In total, 42 patients >125 kg were enrolled in the trial (Table); 20 received FD RBV (800 mg/d) and 22 received WBD RBV (1400 mg/d). SVR occurred in 45% of patients-33% of G1 and 61% of G2/3 patients, rates nearly identical to those for the overall study cohort. SVR rates for the 20 FD RBV patients and the 22 WBD RBV patients were 25% and 64% overall (P=.015); 17% and 50% in G1 (P=.096), and 38% and 80% in G2/3 (P=.078). Only 2/42 (5%) had nadir Hgb <10 gm/dL and 3/42 (7%) had neutrophils <750/mm3; for the overall study cohort (n = 4913) these percentages were 16% and 20%. Dose reductions of PEG-IFN occurred in 8/42 (19%) patients and 9/42 (21%) had dose reductions of RBV.
Conclusions: In WIN-R, patients with very high body weight and BMI had SVR rates similar to those of other study patients, and like the other patients, WBD RBV conferred superior efficacy to FD RBV in these patients. The low rates of nadir hemoglobin and neutropenia and low dose reduction rates probably reflect lower levels of drug exposure. These results suggest that severe obesity should not preclude consideration of antiviral therapy for chronic hepatitis C; however, further studies of such patients are needed.
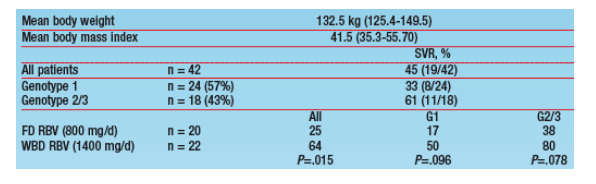
*The poster represents updated data that include patients (n = 9) who weighed 125 kg.
BACKGROUND
- Obese patients with chronic hepatitis C are at greater risk for advanced liver disease than patients of normal weight.1
- Patients whose body mass index (BMI) is >30 kg/m2 have a significantly reduced probability of attaining sustained virologic response (SVR) than normal weight or overweight patients (odds ratio, 0.24; 95% confidence interval, 0.064, 0.885).2
- Three mechanisms have been proposed to explain the reduced response to interferon (IFN)-based therapy in obese patients.1
- Obesity is an inflammatory condition resulting in abnormal immune responses and reduced biological responses to IFN alfa.
- Obesity causes insulin resistance and hepatic steatosis and fibrosis, which cause direct or indirect interference with the effect of IFN alfa.
- Obesity results in decreased bioavailability of pegylated IFN (PEG-IFN) alfa.
- According to the results of the WIN-R trial, weight-based dosing of ribavirin is important in maximizing SVR rates.3
- SVR rates were significantly higher with PEG-IFN alfa-2b (PegIntron®) plus weight-based ribavirin than plus flatdose
ribavirin (overall 44.3% vs 40.6% [P = .007] and 34.1% vs 28.9% in [P = .004] in genotype 1 [G1] patients).
- Patients weighing >105 kg to <125 kg who received ribavirin 1400 mg/d had SVR rates similar to those of other
patients receiving weight-based ribavirin who weighed 65 kg to <105 kg.
- SVR rates were not reported separately for patients weighing ≥125 kg who entered the study as protocol exceptions.
STUDY AIM
- To evaluate patients with chronic hepatitis C and body weight ≥125 kg who were treated with PEG-IFN alfa-2b plus flat-dose or weight-based ribavirin.
METHODS
Study Design
- This was a subanalysis of the WIN-R trial, which was a prospective, multicenter, community- and academic-based, open-label, investigator-initiated study conducted at 225 sites in the United States.
Patients
- Patients had chronic hepatitis C, were 18 to 70 years of age, were ≥125 kg, and were treatment naive. Additional inclusion
criteria included
- Elevated alanine aminotransferase level within 6 months before entry.
- Liver biopsy findings consistent with chronic hepatitis C within 36 months before entry.
- Compensated liver disease.
- _-Fetoprotein level ≦100 ng/mL in the year preceding entry.
- Patients with positive test results for hepatitis B surface antigen or HIV were excluded.
Treatment
- In the WIN-R trial, patients were randomly assigned to receive PEG-IFN alfa-2b 1.5 _g/kg/wk administered subcutaneously and daily ribavirin administered orally (flat dose or weight-based dose: <65 kg, 800 mg/d; 65-85 kg, 1000 mg/d; >85 kg to 105 kg, 1200 mg/d; >105 kg, 1400 mg/d) for 48 weeks (G1, G4, G5, or G6) or for 24 or 48 weeks (G2/3). All patients were monitored for 24 weeks after treatment.
- Guidelines for discontinuing, interrupting, or lowering the dose of study medication for adverse events and hematologic or biochemical abnormalities were in keeping with standard practice.
- Ribavirin dose reductions and discontinuations were required for hemoglobin levels lower than 10 g/dL and 8.5 g/dL, respectively.
Assessments
- Primary efficacy end point of the WIN-R trial was SVR, defined as undetectable (<29 IU/mL) serum HCV RNA 24 weeks after treatment.
- Secondary efficacy end point was the difference in SVR among patients with G2/3 treated for 24 or 48 weeks.
- HCV RNA levels were determined by polymerase chain reaction (PCR; lower limit of quantification 29 IU/mL; TaqMan [Applied Biosystems, Foster City, CA]; Schering-Plough Research Institute, Kenilworth, NJ) at weeks 0, 24, 48, and 72.
RESULTS
Patient Baseline Demographics and Flow
- In total, 51 patients, each weighing ≥125 kg, were enrolled in the WIN-R trial (Table 1 and Figure 1).
- Mean body weight was 131.2 kg, and mean BMI was 41.0 kg/m2.
- 53% (27/51) of patients had G1, and 47% (24/51) had G2/3.
- 45% (23/51) of patients received flat-dose ribavirin (800 mg/d), and 55% (28/51) received weight-based ribavirin (1400 mg/d).

End-of-Treatment Responses
- Overall, 61% (31/51) of patients were responders at the end of treatment, and 39% (20/51) were nonresponders.
SVR Rates
- Overall, SVRs occurred in 47% (25/51) of patients who weighed ≥125 kg.
- 30% (8/27) of patients with G1 and 67% (16/24) of patients with G2/3 achieved an SVR, percentages nearly identical to those for the overall WIN-R study cohort.
- Patients weighing ≥125 kg have a significantly increased probability of achieving an SVR with weight-based ribavirin than with flat-dose ribavirin (odds ratio = 3.532; 95% confidence interval = 1.099, 11.358; P = .0342).
- SVR rates were higher in G1 and G2/3 patients receiving weight-based ribavirin than in those receiving flat-dose ribavirin, though the differences did not achieve statistical significance. Overall 30% receiving FD RBV vs 61% receiving WBD RBV had SVR (p=.0342); for G! 15% FD vs 43% WBD; for G@/3 FD was 50% vs 79% for WBD. BUT< these results appear to be driven by the improved SVR rates in patients of >105 kg (about 220 lbs) while in lower weight patients there was no apparent difference between FD or WBD as you can see in Figure 4 below.
- Low numbers of patients in these groups may preclude meaningful statistical analysis.
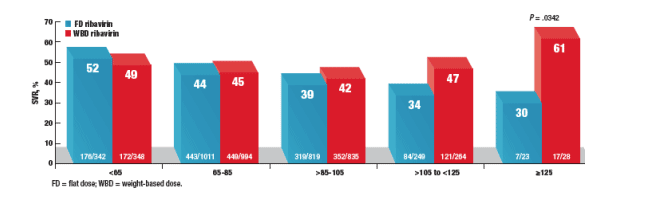
- Compared with patients weighing <125 kg, the greatest difference in SVR rates between weight-based and flat-dose ribavirin was observed among those weighing ≥125 kg (Figure 4).
Figure 4. Sustained virologic response (SVR) rates of patients weighing <125 kg and ≥125 kg in the WIN-R trial
For patients with weights <65 kg, 65-85 kg, and 85-105 kg there is no difference in SVR rates between using FD or WBD ribavirin. In the weight groups of 105-125 kg & >125 kg the SVR rates are better when using WBD: 47% (121/264) vs 34% (84/249); in the >125 kg group: 30% (7/23) in FD vs 61% (17/28) in WBD achieved SVR.
Safety Analysis
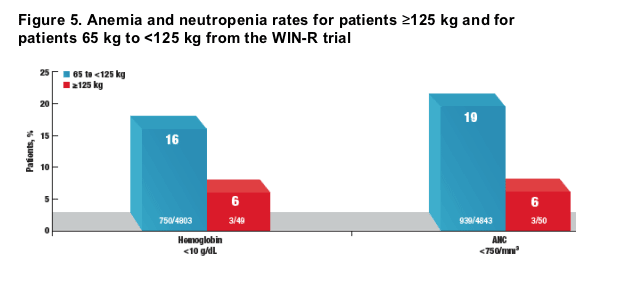
- Hemoglobin levels decreased below 10 g/dL in only 6% (3/49) of patients, and absolute neutrophil counts were lower than 750 cells/mm3 in 6% (3/50) of patients who were >125 kg(Figure 5).
- In the WIN-R study, 16% (750/4803) of patients had hemoglobin levels lower than 10 g/dL, and 19% (939/4843) of patients had absolute neutrophil counts lower than 750 cells/mm3 in the overall study cohort (n = 4913).
- Dose reductions of PEG-IFN occurred in 9 of 51 (18%) patients, and dose reductions of ribavirin occurred in 10 of 51 (20%).
References
1. Charlton MR et al. Hepatology. 2006;43:1177-1186.
2. Bressler BL et al. Hepatology. 2003;38:639-644.
3. Jacobson IM et al, and the WIN-RS Group. Hepatology. 2005;42(suppl):749A.
|
| |
|
 |
 |
|
|