 |
 |
 |
| |
Week 4 Response Predicts SVR in Pegasys/RBV 16 Week Therapy Study in Genotypes 2/3
|
| |
| |
Reported by Jules Levin
AASLD, Oct 27-31, 2006, Boston, MA
Utility of virological response at weeks 4 and 12 in the prediction of SVR rates in genotype 2/3 patients treated with peginterferon alfa-2a (40KD) plus ribavirin: findings from ACCELERATE
M.L. Shiffman,1 S. Pappas,2 B. Bacon,3 E. Godofsky,4 D. Nelson,5 H. Harley,6 M. Diago,7 A. Lin,8 G. Hooper,9 S. Zeuzem10
1VCU Medical Center, Richmond, VA, USA; 2St Luke's Center for Liver Disease, Houston, TX, USA; 3St Louis University, St Louis, MO, USA; 4Bach & Godofsky, Bradenton, FL, USA; 5University of Florida, Gainesville, FL, USA; 6Royal Adelaide Hospital, Adelaide, SA, Australia;
7Hospital General, Valencia, Spain; 8Roche, Nutley, NJ, USA; 9Roche, Welwyn Garden City, UK; 10Saarland University Hospital, Homburg/Saar, Germany
Note from Jules Levin: in the ACCELERATE Study, which compared 16 & 24 weeks Pegasys/RBV 800 mg therapy, RVR (rapid viral response, week 4) predicts SVR. As well, patients with low viral load at baseline (<400,000 IU/mL) were more likely to achieve SVR. Understandably, week 12 (EVR) predicted SVR, but almost all study patients had EVR.
INTRODUCTION
The recommended treatment for patients infected with hepatitis C virus (HCV) genotypes 2 and 3 is a pegylated interferon plus ribavirin 800 mg/day for 24 weeks.[1] There are, however, continuous efforts to optimize and improve treatment strategies in order to reduce the incidence of adverse events and lower the overall cost of treatment.
On-treatment responses such as early virologic response (EVR; undetectable or ≥2-log10 drop in HCV RNA at week 12) and rapid virologic response (RVR; undetectable HCV RNA at week 4) play an important role in the optimization of treatment in patients with chronic hepatitis C. The absence of an EVR in HCV genotype 1 has been shown to be highly predictive of not achieving a sustained virologic response (SVR),[2-4] and current treatment guidelines incorporate a week-12 decision criterion where treatment may be discontinued in genotype 1 patients who fail to achieve an EVR.[5]
Additionally, recent studies in HCV genotype 1 patients have illustrated that patients who achieve an RVR have a high SVR rate, even with an abbreviated duration of treatment (24 weeks rather than 48 weeks). In these patients, the achievement of an RVR was key to achieving an SVR with a shorter period of treatment.[6,7]
The primary outcome of ACCELERATE, a large randomized trial examining 16 and 24 weeks of peginterferon alfa-2a (40KD) (PEGASYS) plus ribavirin
(COPEGUS) in patients infected with HCV genotypes 2 and 3, demonstrated that, overall, 24 weeks of therapy was associated with a significantly higher rate of SVR than 16 weeks of treatment (76% vs 65% of patients; p<0.0001).
However, some patient populations, such as those with a low baseline viral load or an RVR, achieved a high rate of SVR (>80%) with 16 weeks of treatment.
Here we analyzed data from ACCELERATE to assess (1) the proportion of patients who achieved an on-treatment virologic response (RVR and EVR) and
(2) the predictive value of such responses for an SVR in the management of patients with genotype 2 and 3 infection.
METHODS
Study Design & Patients
In ACCELERATE, treatment-naive patients with chronic hepatitis C genotype 2
or 3 virus infection were randomized to receive peginterferon alfa-2a (40KD)
180 _g/week plus ribavirin 800 mg/day for 16 or 24 weeks.
All patients had quantifiable HCV RNA (COBAS AMPLICOR HCV MONITOR Test, v2.0, limit of quantitation 600 IU/mL), abnormal alanine aminotransferase
levels, and a liver biopsy within 24 months of the start of the study.
All efficacy analyses were conducted in the standard (per-protocol) efficacy population (all randomized patients who received at least one dose of study drug, whose treatment duration was consistent with the assigned duration and who had no major protocol deviations) and the intent-to-treat (ITT) population.
- the standard analysis was of greater applicability because, in an analysis of the ITT population, patients who withdrew prematurely from their assigned treatment duration in the longer treatment arm could bias the results in favor of showing equivalence between the two treatment durations. Here, we report outcomes in the standard population.
Assessments and end-points
The primary efficacy end-point was SVR, defined as undetectable serum HCV RNA (COBAS AMPLICOR HCV Test, v2.0, limit of detection 50 IU/mL) after a 24-week follow-up period.
-- patients without follow-up data were considered not to have achieved an SVR.
On-treatment responses (RVR and EVR) were recorded.
- an RVR was defined as undetectable HCV RNA at week 4 (COBAS AMPLICOR HCV Test, v2.0, limit of detection 50 IU/mL), while an EVR was defined as undetectable HCV RNA or ≥2-log10 drop in HCV RNA (COBAS AMPLICOR HCV MONITOR Test, v2.0, limit of quantitation 600 IU/mL) at week 12
- the association between the occurrence of on-treatment responses (RVR and
EVR) and SVR was assessed.
AUTHOR CONCLUSIONS
Despite an excellent negative predictive value (94%), the achievement of an EVR in patients with HCV genotype 2 and 3 has limited value as a guide to optimizing therapeutic regimens, as only a minority (2%) of these patients do not achieve a response after 12 weeks of treatment with peginterferon alfa-2a (40KD) (PEGASYS®) plus ribavirin (COPEGUS®).
In patients with HCV genotype 2 or 3 infection, RVR has emerged as an important on-treatment predictor of SVR, and has the potential to become a useful tool for the clinician to help optimize the therapeutic regimens in patients
infected with genotype 2 or 3.
The chance of a patient with RVR going on to achieve an SVR was 82% with 16 weeks of treatment and 90% with 24 weeks of treatment with peginterferon alfa-2a (40KD) plus ribavirin. In patients who achieve an RVR, as with patients with a low baseline HCV RNA level, a shorter duration of treatment could therefore be considered in those who find it difficult to tolerate a full course of therapy.
In contrast, patients who do not achieve an RVR have a probability of achieving an SVR of 27% and 49% with 16 and 24 weeks of treatment, respectively. Shortening treatment in these patients should be strongly discouraged. Even with 24 weeks of treatment, SVR is only achieved by approximately one-half of these patients. This suggests that patients with genotype 2/3 without an RVR should not be considered 'easy-to-cure'. The possibility that more intensive therapy will enhance SVR in these patients should be explored in future studies.
Overall, virologic response at week 4 (RVR) demonstrates potential clinical utility in predicting SVR rates and guiding treatment duration in genotype 2/3 patients treated with peginterferon alfa-2a (40KD) plus ribavirin.
RESULTS
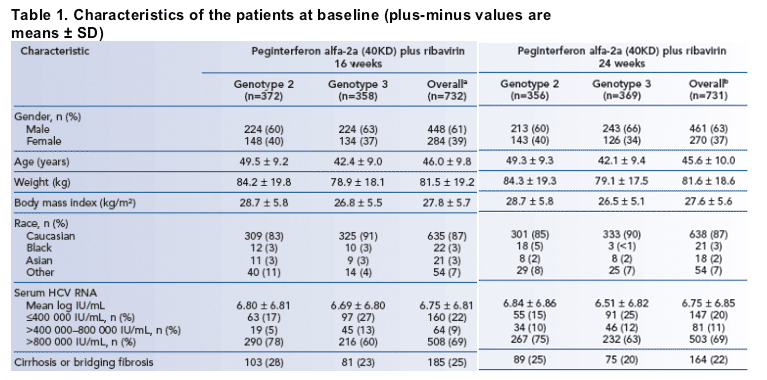
Demographic and disease characteristics for the intent-to-treat patient population
(n=1463) are summarized in Table 1 (see below). Overall, patients who received 16 and 24 weeks' treatment were well matched with regard to demographic and clinical characteristics and the distribution of HCV genotype 2 and 3 infection.
Virologic response at weeks 4 (RVR) and 12 (EVR)
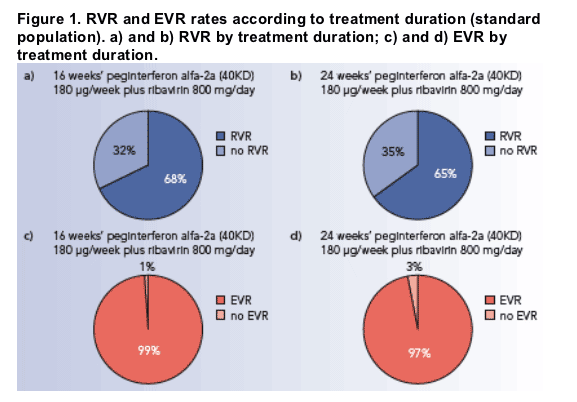
An RVR was achieved by 68% and 65% of patients in the 16- and 24-week treatment arms, respectively (Figure 1a and b).
An EVR was achieved by 99% and 97% of patients in the 16- and 24-week arms, respectively (Figure 1c and d).
Predictive value of RVR
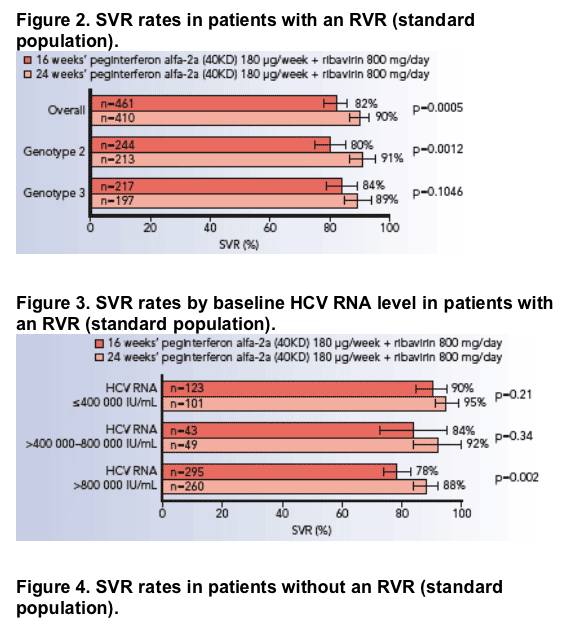
The achievement of an RVR was strongly predictive of achieving an SVR after both 16 and 24 weeks of treatment.
- patients with an RVR who received 16 weeks of treatment had a high rate of
SVR (82%) (Figure 2)
- patients with an RVR who received 24 weeks of treatment achieved a rate
of SVR that was 8% higher than that in patients who received 16 weeks of
treatment (90%; p=0.0005) (Figure 2).
In patients who achieved an RVR, those with a low viral load (≦400 000 IU/mL) had a high probability of achieving an SVR (≥90%), irrespective of treatment duration (Figure 3).
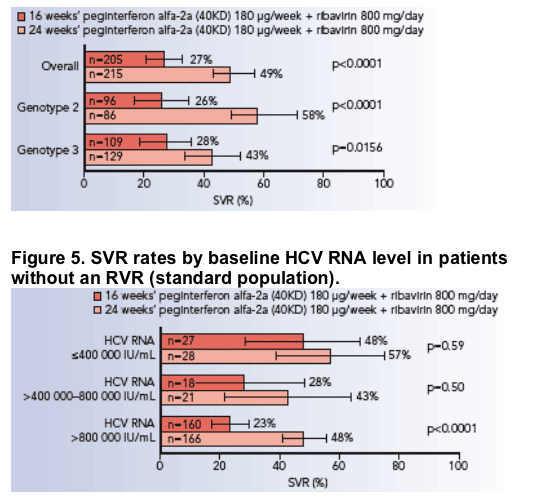
In patients without an RVR, 24 weeks of treatment was superior to 16 weeks overall (p<0.0001) and for each genotype (Figure 4) and baseline HCV RNA level
(Figure 5).
|
| |
|
 |
 |
|
|