 |
 |
 |
| |
Week 48 efficacy of TPV/r treatment is enhanced in patients with higher numbers of genotypically available background drugs in RESIST 1 and 2
|
| |
| |
Reported by Jules Levin
8th International Congress on Drug Therapy in HIV Infection
November 12-16, 2006, Glasgow
65% (32/49) of patients in study taking Fuzeon for the first time plus 1 nuke in the background therapy to which they are sensitive achieve a treatment response.
A Lazzarin1, J. Feinberg2, M Kraft3, D Neubacher4
1San Raffaele Sci Inst, Milan, Italy; 2University of Cincinnati Medical Center, Cincinnati, OH, USA; 3Boehringer Ingelheim International GmbH, Ingelheim, Germany;
4Boehringer Ingelheim Pharma GmbH & Co. KG, Biberach, Germany
AUTHOR CONCLUSIONS
- TPV/r provided superior efficacy compared with CPI/r through 48 weeks.
- Treatment responses to TPV/r regimens improved with increasing numbers of active OBR RTIs.
- A substantial proportion of RESIST patients who took TPV/r and another new ARV, such as ENF, were able to achieve virological suppression (VL <50 copies/mL), as recommended in current guidelines.
Abstract
The RESIST trials are Phase 3, multicentre, randomised studies that demonstrated the superiority of TPV/r over comparator ritonavir-boosted PIs (CPI/r).
This analysis determined the impact of genotypically active drugs in the optimised background regimen (OBR) on the RESIST efficacy results.
Patients had ≥3-class ARV experience; ≥2 PIs; any CD4 cell count; viral load
(VL) ≥1000 copies/mL; isolates carrying ≥1 primary PI mutation and ≦2 at 33,
82, 84, 90.
The genotypic sensitivity to background RTIs (GSB), defined as the
number of NRTIs and NNRTIs to which the virus was genotypically sensitive,
was determined.
1483 patients: mean baseline VL 4.73 log10 copies/mL; CD4 cell count
195 cells/mm3.
Overall treatment response rates were 33.6% in TPV/r arm vs. 15.3% in CPI/r arm.
Use of TPV/r was consistently associated with a better treatment response than
CPI/r when combined with:
-- 0 (24.8% vs. 7.9%),
-- 1 (34.8% vs. 14.3%),
-- 2 (36.4% vs. 14.8%), or
-- ≥3 (41.4% vs. 31.6%) active OBR drugs (excluding enfuvirtide).
Other efficacy parameters such as proportions of patients with VLs <400 or
<50 copies/mL improved with increased number of active OBR ARVs. In all
comparisons, the outcomes with TPV/r were superior to those with CPI/r.

TPV/r provides superior efficacy compared with CPI/r through 48 weeks. Treatment responses to TPV/r regimens improved with increasing numbers of
active OBR ARVs.
Note: data have been updated subsequent to submission of abstract.
We conducted an analysis to determine the impact of genotypically active drugs
in the OBR on the Week 48 RESIST efficacy results.
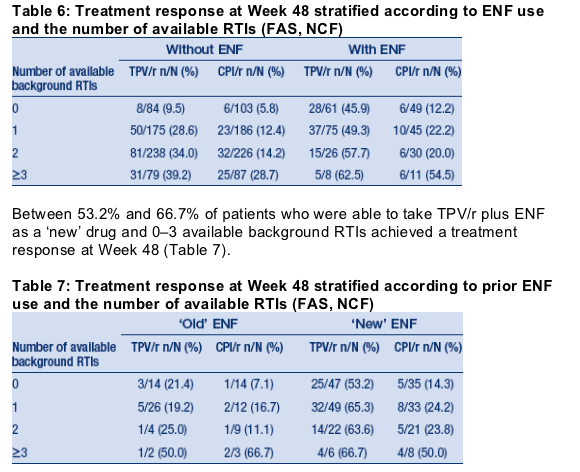
'Old' ENF refers to use of ENF prior to enrolment in RESIST; 'new' ENF refers to use of ENF for the first time in RESIST.
The genotypic sensitivity to background RTIs (GSB) was defined as the number
of RTIs to which the virus was genotypically sensitive. Susceptible NRTIs and
NNRTIs in the OBR contributed to the GSB. A GSB score of 0.25 indicated susceptibility to one RTI; 0.5 indicated susceptibility to two RTIs; and 0.75 indicated susceptibility to three RTIs.
Results
Patient population
The baseline characteristics were similar in both studies and both treatment
arms (Table 1).
Table 2 summarises the number of patients in each GSB stratum in the RESIST
studies.
Treatment response at Week 48
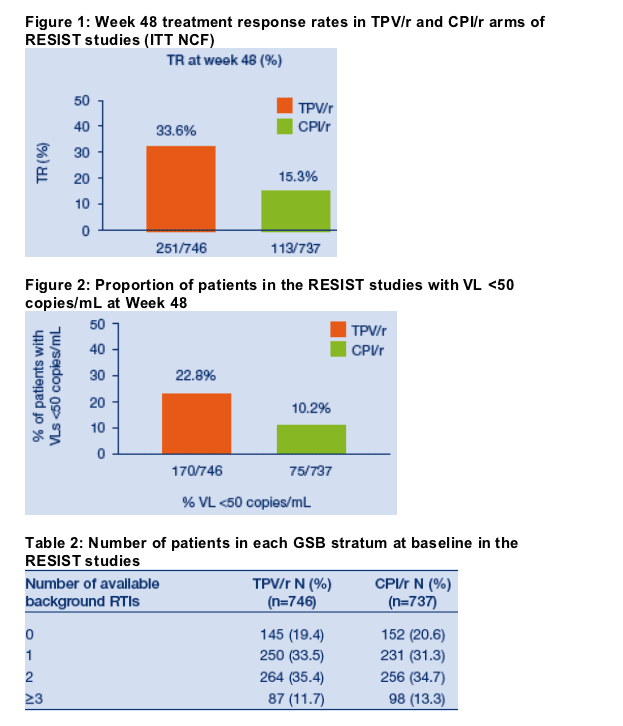
At Week 48, the TR was significantly better in the TPV/r arm: 33.6% (251/746)
vs. 15.3% (113/737) in the CPI/r arm (p<0.0001) (Intent to Treat Non-completer
= Failure [ITT NCF]) (Figure 1). The odds of achieving a TR was significantly
higher in patients treated with TPV/r than in patients taking CPI/r (odds ratio
(OR): 2.79; p<0.0001).
At Week 48, the proportion of patients with a VL <400 copies/mL was 30.4%
(227/746) in TPV/r patients compared to 13.8% (102/737) in the CPI/r patients
(p<0.0001). The proportion of patients with a VL <50 copies/mL at Week 48 was
22.8% (170/746) in the TPV/r arm and 10.2% (75/737) in the CPI/r arm (p<0.0001) (Figure 2).

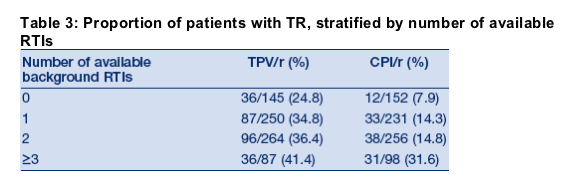
Impact of availability of RTIs on treatment response rates
Treatment with TPV/r was consistently associated with a better treatment
response than CPI/r when combined with 0 (24.8% vs. 7.9%), 1 (34.8% vs.
14.3%), 2 (36.4% vs. 14.8%), or ≥3 (41.4% vs. 31.6%) active OBR drugs
(excluding ENF) (Table 3).
The results of a logistic regression analysis for TR at Week 48 showed that the
odds ratio (OR) significantly increased as the number of available background
RTIs increased from 0 to 1, 2 or 3 (p<0.0001) (Table 4).

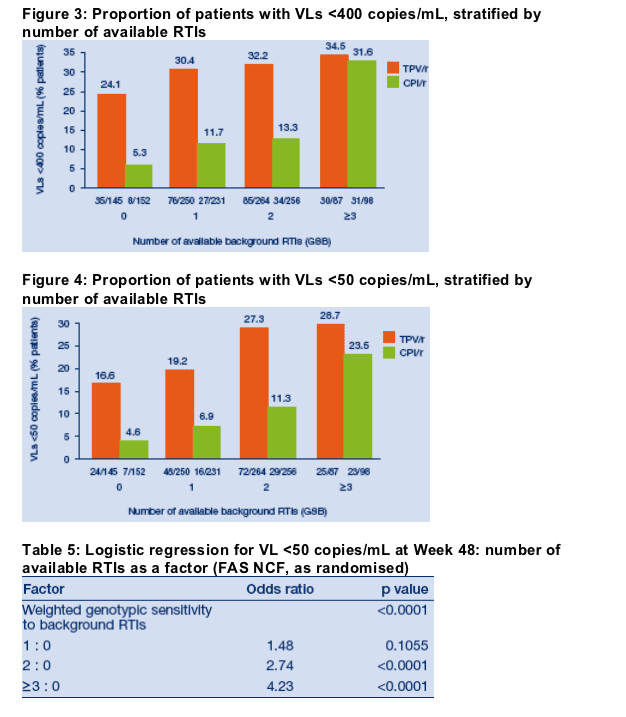
Other efficacy parameters, such as proportions of patients with VLs <400 or <50 copies/mL, improved with increased number of active OBR RTIs (Figure 3 and Figure 4). In all comparisons, the outcomes with TPV/r were superior to those with CPI/r.
Table 5 presents the results of a logistic regression analysis for achieving a VL <50 copies/mL at Week 48 using weighted genotypic sensitivity to background RTIs as a factor. The chances of achieving an undetectable VL increased significantly as the number of genotypically available drugs increased.
Impact of enfuvirtide on treatment response
Achieving a TR response at Week 48 with TPV/r or CPI/r in the absence of ENF was highly dependent on the weighted genotypic sensitivity to background RTIs, i.e. the number of active RTIs in the OBR (Table 6). When ENF was included in the OBR, 45.9-62.5% of TPV/r patients achieved a TR, regardless of the weighted genotypic sensitivity to background RTIs (Table 6). A comparable response in patients taking a CPI/r was achieved only when ENF was co-administered with at least three other genotypically sensitive RTIs (weighted genotypic sensitivity to background RTIs ≥0.75).
References
1. Hicks, C.B., et al. Durable efficacy of tipranavir-ritonavir in combination with
an optimised background regimen of antiretroviral drugs for treatmentexperienced HIV-1-infected patients at 48 weeks in the Randomized
Evaluation of Strategic Intervention in multi-drug reSistant patients with Tipranavir (RESIST) studies: an analysis of combined data from two
randomised open-label trials. Lancet, 2006. 368(9534): p. 466-75.
2. Farthing, C., et al. Tipranavir/r demonstrates superior and durable treatment
response compared with comparator PI/r in highly treatment experienced (HTE) patients: Week 96 RESIST 1 and 2 results. In 46th Interscience Conference on Antimicrobial Agents and Chemotherapy (ICAAC). 2006. San Francisco. Abs. H-1385.
3. Markowitz, M., et al. Safety and efficacy of tipranavir, a non-peptidic protease inhibitor, in multiple PI-failure patients (BI 1182.2). In 1st IAS Conference on HIV Pathogenesis and Treatment. 2001. Buenos Aires. Abstract 3.
4. Markowitz, M., et al., Long-Term Efficacy and Safety of Tipranavir Boosted With Ritonavir in HIV-1-Infected Patients Failing Multiple Protease Inhibitor Regimens: 80-Week Data From a Phase 2 Study. J AIDS, 2006. In press.
|
| |
|
 |
 |
|
|