 |
 |
 |
| |
CD4 Count Predicts Fatal Non-AIDS Cancers: Traditional Malignancies May also be AIDS-Related
|
| |
| |
CROI, Feb 2007, Los Angeles
Reported by David Alain Wohl, MD Đ University of North Carolina
"....Low CD4 cell counts, we are learning, risk a host of badness from cardiovascular disease, liver problems and malignancies...."
Since 1993, the Centers for Disease Control and Prevention (CDC) have included a number of malignancies in the case definition of AIDS. Invasive cervical carcinoma, KaposiŐs sarcoma and certain lymphomas, when emerging in a person with HIV-infected, qualify as AIDS-defining conditions. However, as individuals living with HIV infection live longer there has been growing concern that other cancers - more often seen in the aging general population - would increase among HIV+ persons.
Researchers from the D:A:D cohort, a large prospective observational study of HIV-infected patients in Europe, Australia and the US, examined all deaths due to malignancy that have occurred among the participants to compare the rates of fatal AIDS-defining and non-AIDS-defining cancers and identify factors associated with each.
The D:A:D cohort has largely been preoccupied with study of the other major worry for HIV-infected persons and their clinicians Đ cardiovascular disease. With over 23,000 participants and more than 104,000 patient years of follow-up, the cohort provides a unique opportunity to examine relatively rare clinical events like heart attacks, strokes and fatal cancers. In this analysis the non-AIDS-defining cancers they looked at were lung, anal, hematologic (except non-HodgkinŐs lymphoma), upper airway, urogenital, gastrointestinal, breast, central nervous system, sarcoma and skin.
The D:A:D patients have a median age of approximately 40 years, are mostly male (-75%) and over 50% either smoke or have a history of smoking. The racial breakdown of the cohort is not clear and it is likely there are less persons who are Black than would be found in a purely US cohort.
Overall, there were 305 fatal cancers: 112 AIDS-related and 193 non-AIDS-defining malignancies. Therefore, only 37% of fatal cancers were due to cancers considered AIDS-related. The rate of non-AIDS cancers was higher than that for AIDS-related cancers (1.79 versus 1.05 per 1000 patient years of follow-up). The types of cancers that developed are shown in the figure below.
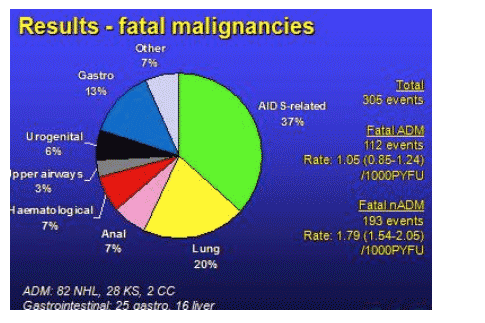
There were a number of differences between those who developed AIDS-defining and non-AIDS-defining malignancies. Those developing the AIDS-related cancers were younger (median age 43 years versus 52 years), had a lower CD4 cell count nadir (30/mm3 versus 87/mm3), a lower CD4 cell count prior to death (75/mm3 versus 211/mm3) and a higher HIV RNA level (3.8 log10 copies/mL versus 2.3 log10 copies/mL). In addition, they were less likely to be receiving HAART at the time of death (47% versus 61%).
One of the most impressive findings was the observation that cancers not previously considered AIDS-associated increased in incidence as the CD4 cell count declined.
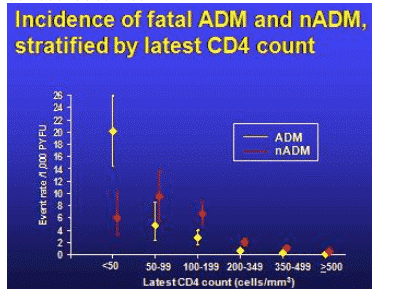
Other factors associated with non-AIDS-defining cancers included smoking and hepatitis B virus infection. For AIDS cancers, being homosexual was associated with increased risk. Excluding anal cancers did not change the relative risk of non-AIDS cancers with decreasing CD4 cell counts.
Conclusion: The finding that more severe immunodeficiency was a risk factor for AIDS-defining cancers independent of age and other known risks was expected, that low CD4 cell count was also a strong risk factor for non-AIDS-defining cancers was more surprising. Fortunately, as in the case for heart attacks in this cohort, fatal cancers were rare with only 305 patients dying from such cancers out of over 20,000 people. However, the incidence of malignancies will certainly increase as the cohort ages.
The upshot is that clinicians and persons living with HIV infection must be aware of the added risk for non-AIDS cancers, especially at lower CD4 cell counts. Clinicians must be aggressive in screening for cancers of the breast, cervix, colon, anus and prostate. For patients, these data add to the long list of reasons to quit smoking. There are an increasing number of approaches to smoking cessation and HIV docs need to become as familiar with these as we are lipid-lowering therapy.
The study also adds to the chorus of studies singing the praises of HIV therapy. The immune system does more than protect the body from infection. Cancer cells often are considered to be Ônon-selfŐ and can be attacked by T-cells. Therefore, it makes sense that the loss of these cells during HIV infection could yield a higher risk of cancers beyond those first identified as being related to AIDS. Low CD4 cell counts, we are learning, risk a host of badness from cardiovascular disease, liver problems and malignancies. Treatment is looking better all the time.
|
| |
|
 |
 |
|
|