| |
Cancer Risk in HIV+
|
| |
| |
Download the PDF here
HIV Patients at More Risk of Developing 20 Cancers, Study Shows
By Simeon Bennett
Study limitation, "....The bulk of the data came from studies that followed people only after the onset of AIDS,4,9,10 and in the era of highly active antiretroviral therapy (HAART), these people comprise an increasing minority of HIV-infected people..."
July 6 (Bloomberg) -- HIV patients are at greater risk of developing one of 20 cancers, almost seven times the number of tumors previously linked to the virus, researchers said.
Scientists at the University of New South Wales in Sydney analyzed more than 440,000 people with HIV, the virus that causes AIDS, and 30,000 kidney transplant patients in studies dating to the 1970s. Both groups were several times more likely than healthy people to develop cancers linked to infections. The findings are published today in The Lancet medical journal.
The research suggests immune deficiency, which was common to both groups, is responsible for the increased risk, and may change the way HIV is treated. Patients may need earlier treatment with anti-retroviral drugs such as Abbott Laboratories' Kaletra and Merck & Co.'s efavirenz, said Andrew Grulich, who led the research at the university's National Centre in HIV Epidemiology and Clinical Research.
``Infection-related cancer will probably become an increasingly important complication of long-term HIV infection,'' the authors wrote.
In addition to cancers known to be linked to HIV, including non-Hodgkin's lymphoma, Kaposi's sarcoma and cervical cancer, the study group was more likely to develop tumors linked to infections such as human papillomavirus, including those of the mouth, penis, anus, liver, stomach, esophagus, larynx and eye, the researchers said.
The risk of developing cancers not linked to infection, such as tumors of the breast and prostate, was the same as for the general population, they said.
More Studies
The researchers will now examine people with inherited immune deficiency and those who've had other organs transplanted to see if the findings hold. Grulich said the center had applied to Australia's National Health and Medical Research Council for funding to extend the study, which it wants to start in January.
About 40 million people in the world are infected with HIV, 1 million of them in the U.S., health officials say. When untreated, the virus dismantles the human immune system, leaving patients vulnerable to lethal infections in the liver, lung, and other organs.
Recipients of kidney transplants have impaired immune systems because they take drugs to ensure their bodies don't reject the organ.
The Lancet July 7, 2007; 370:59-67
Incidence of cancers in people with HIV/AIDS compared with immunosuppressed transplant recipients: a meta-analysis
Prof Andrew E Grulich PhD a , Marina T van Leeuwen MPH a, Michael O Falster BPsych[Hons] a and Claire M Vajdic PhD a
Summary
Background
Only a few types of cancer are recognised as being directly related to immune deficiency in people with HIV/AIDS. Large population-based studies in transplant recipients have shown that a wider range of cancers could be associated with immune deficiency. Our aim was to compare cancer incidence in population-based cohort studies of people with HIV/AIDS and people immunosuppressed after solid organ transplantation.
Methods
Two investigators independently identified eligible studies through searches of PubMed and reference lists. Random-effects meta-analyses of log standardised incidence ratios (SIRs) were calculated by type of cancer for both immune deficient populations.
Findings
Seven studies of people with HIV/AIDS (n=444 172) and five of transplant recipients (n=31 977) were included. For 20 of the 28 types of cancer examined, there was a significantly increased incidence in both populations. Most of these were cancers with a known infectious cause, including all three types of AIDS-defining cancer, all HPV-related cancers, as well as Hodgkin's lymphoma (HIV/AIDS meta-analysis SIR 11·03, 95% CI 8·43-14·4; transplant 3·89, 2·42-6·26), liver cancer (HIV/AIDS 5·22, 3·32-8·20; transplant 2·13, 1·16-3·91), and stomach cancer (HIV/AIDS 1·90, 1·53-2·36; transplant 2·04, 1·49-2·79). Most common epithelial cancers did not occur at increased rates.
Interpretation
The similarity of the pattern of increased risk of cancer in the two populations suggests that it is immune deficiency, rather than other risk factors for cancer, that is responsible for the increased risk. Infection-related cancer will probably become an increasingly important complication of long-term HIV infection.
Introduction
The substantial improvement in survival after HIV infection has led to increasing public health and clinical interest in long-term morbidities, including cancer, in this population. Historically, the occurrence of only three types of cancer in a person infected with HIV, namely Kaposi's sarcoma, non-Hodgkin lymphoma, and cervical cancer, has constituted an AIDS diagnosis. However, in population-based cohort studies, a few other cancers seem to occur at increased rates in people with HIV/AIDS, including Hodgkin's lymphoma, lip cancer, and possibly testicular seminoma.1-3 An increased incidence of several other cancer types has also been reported, but on the basis of the largest single study published, these have been judged as not being associated with immune deficiency.4 The investigators postulated that lifestyle and other risk factors, and not immune deficiency, could explain the increased risk of these cancers.4
Studies of cancer in other immune deficient populations, such as transplant recipients receiving iatrogenic immune suppression, have the potential to inform thinking about which cancers are truly associated with immune deficiency. Specifically, because lifestyle-related cancer risk factors probably differ substantially between these populations, if cancer incidence patterns are similar then it would probably be immune deficiency that would be primarily responsible. In the past year, two large population-based cohort studies have reported that a range of cancer types apparently occurs at increased rates in recipients of renal transplants.5,6 This finding demands a reappraisal of data on the occurrence of cancer in people with HIV/AIDS.
Our aim was to examine, using meta-analyses, cancer incidence in published population-based studies of people with HIV/AIDS, and organ transplant recipients, and to compare these findings.
Results
Seven reports of HIV-associated cancer risk, involving 444 172 people with HIV/AIDS, were included. These studies were done in the USA (two non-overlapping reports from the same study), Australia, Scotland, Italy, Switzerland, and England (table 1).2,4,9,10,15-17 The five studies of cancer risk in organ transplant recipients, including 31 977 organ transplant recipients, were done in Denmark, Finland, Sweden, Australia, and Canada (table 2).5,6,18-20 31 050 (97%) transplant recipients received a renal graft. The individual study estimates of cancer SIRs are shown in table 3 and table 4.
Figure 2 shows the SIRs for cancers related to infection with Epstein-Barr virus (EBV), human herpesvirus 8 (HHV8), hepatitis viruses B and C (HBV and HCV), and Helicobacter pylori. Hodgkin's and non-Hodgkin lymphoma occurred at markedly increased rates in both populations. The meta-analysis estimate of SIR for both Hodgkin's and non-Hodgkin lymphoma was higher in people with HIV/AIDS than in transplant recipients. Based on only two studies,4,17 the meta-analysis SIR for nasopharyngeal cancer was 2·90 (95% CI 1·80-4·66) in people with HIV/AIDS; only one case of such cancer was documented in transplant recipients.5
Figure 2. Standardised incidence ratios for cancers related to infection with Epstein-Barr virus, human herpesvirus 8, hepatitis B and C virus, and Helicobacter pylori in people with HIV/AIDS and in transplant recipients
EBV=Epstein-Barr virus. HBV=hepatitis B virus. HCV=hepatitis C virus. HHV8=human herpesvirus 8. *For AIDS-defining cancers, data from cohorts defined by an AIDS diagnosis included only those individuals who did not have that type of cancer at the time of AIDS.
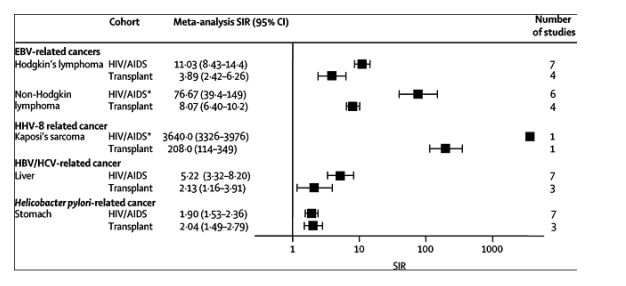
The meta-analysis SIR for Kaposi's sarcoma in people with HIV/AIDS was much higher than in transplant recipients, although the cancer occurred at markedly increased rates in both populations (figure 2). Rates of liver cancer were increased in both populations (figure 2), as were rates of stomach cancer.
Figure 3 shows the SIRs for cancers related to, or possibly related to, infection with human papillomavirus (HPV). Meta-analysis SIRs at each HPV-related anogenital site were increased in both populations. For vulval and penile cancers, the risk was substantially lower in people with HIV/AIDS than in transplant recipients. Conversely, for anal cancer the meta-analysis SIR was much higher in people with HIV/AIDS than in transplant recipients. Meta-analysis SIRs were increased for cancers of the oral cavity and pharynx in both populations. Although non-melanoma skin cancer occurred at increased rates in both populations, it was more markedly increased in transplant recipients than in people with HIV/AIDS (figure 3). A similar pattern was seen for lip cancer. Other possibly HPV-related cancers were increased in both populations, including cancer of the oesophagus, larynx, and eye (figure 3).
Figure 3. Standardised incidence ratios for cancers related to, or possibly related to, human papillomavirus infection, in people with HIV/AIDS and in transplant recipients
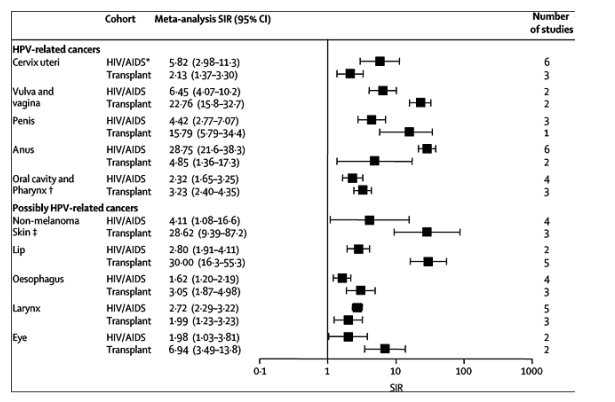
HPV=human papillomavirus. *For the AIDS-defining cancer (cervical cancer), data from cohorts defined by an AIDS diagnosis included only those individuals who did not have cervical cancer at the time of AIDS. Excluding lip and nasopharynx. Any measure of non-melanoma skin.
Most common epithelial cancers occurred at the same rate as the general population, or were less common (figure 4). For prostate cancer, risk was decreased in people with HIV/AIDS, and was no different from population rates in transplant recipients. Colorectal cancer was not increased in people with HIV/AIDS but was increased in transplant recipients. Breast and ovarian cancer rates were no different from population rates in both populations. By contrast, rates of lung cancers were increased in both populations.
Several other cancers occurred at increased rates in both people with HIV/AIDS and transplant recipients, including kidney cancer, myeloma, leukaemia, and melanoma (figure 5). A few cancers occurred at increased rates in transplant recipients only, including cancer of the bladder and thyroid. Cancers that occurred at increased rates in people with HIV/AIDS only included brain cancer and testicular cancer.
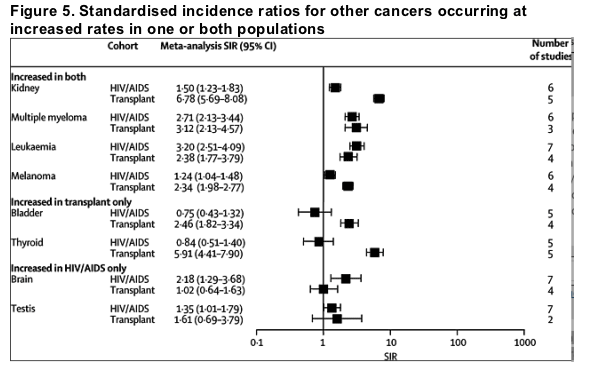
We found no statistical evidence of publication bias (webappendix). One of the studies4 contributed by far the most cancer cases in the HIV/AIDS meta-analysis, but the meta-analysis SIRs remained largely unchanged when this study was excluded. The sensitivity analyses showed that the site-specific meta-analysis SIRs were in general robust to the exclusion of any one study from the meta-analysis. For cancer of the testis and for anal cancer, exclusion of one study9 would have resulted in significantly higher meta-analysis SIRs, but the direction of effect remained the same.
Discussion
Our data indicate that an extensive range of cancers occurs at increased incidence both in people with HIV/AIDS and in transplant recipients. The pattern of increased risk was much the same in both populations. Many-but not all-of the cancers that occurred at increased rates were those with a known or suspected infectious cause. Rates of most of the common epithelial cancers were not increased. Our meta-analysis suggests that the range of infection-related cancers associated with immune deficiency is much wider than previously appreciated and that a range of infectious organisms seems to be implicated.
EBV has been conclusively linked to certain forms of non-Hodgkin lymphoma (including non-Hodgkin lymphoma in immune deficient populations), to Hodgkin's lymphoma, and to nasopharyngeal carcinoma. Both non-Hodgkin and Hodgkin's lymphoma occurred at greatly increased rates, and were more common in people with HIV/AIDS than in transplant recipients. Based on very limited data, rates of nasopharyngeal cancer were slightly increased in people with HIV/AIDS, but there were insufficient data in transplant recipients. None of the studies included were from the Asian countries where nasopharyngeal cancer is common. HHV8 is recognised as a necessary cause of Kaposi's sarcoma,21 and this cancer occurred at greatly increased rates in both populations. High-risk HPV types are recognised as necessary causes of cancer of the cervix, as causing a large proportion of other anogenital cancers, and causing a minority of cases of cancer of the oral cavity and oropharynx.11 All of these cancers occurred at increased rates in both populations. Both HBV and HCV are recognised as causing liver cancer, and this cancer occurred at increased rates in both populations. H pylori is estimated to cause over 60% of all stomach cancer11 and rates were roughly doubled in both populations.
Some types of cancer that were increased in both populations do not have well-accepted associations with infectious organisms. Rates of lip cancer and non-melanoma skin cancer were enormously increased in transplant recipients, and were increased less substantially in people with HIV/AIDS. High levels of infection with epidermodysplasia verruciformis HPV subtypes have been described in squamous cell carcinoma of the skin in immune-suppressed individuals, but their role in carcinogenesis is uncertain.22 HPV infection could also explain the increased risks of cancer of the larynx and eye (largely conjunctiva) in both populations, since these cancers are thought to be possibly related to HPV infection.11,23 The increased rates of leukaemia in both populations could indicate infection with an unknown organism.24 In renal transplant recipients, increased rates of myeloma, and kidney and bladder cancer are also present during and before dialysis, reflecting a cause of end-stage renal disease rather than a consequence of immune deficiency.5
For most of the common epithelial cancers, including cancer of the colon, rectum, breast, ovary, and prostate, there was little evidence of increased risk in either population. However, rates of lung cancer were increased in both populations. In kidney transplant recipients, the magnitude of the increase in lung cancer rates is much greater after transplantation than during dialysis,5 suggesting that immune deficiency could have a direct role. There is weak evidence of an association between this neoplasm and HPV infection,25 and our finding suggests that further research is needed into the veracity of this finding.
Apart from shared immune deficiency, there are various possible explanations for the similarity in the pattern of cancer incidence between the two populations. One is heightened medical surveillance for cancer, although the absence of increased risk for breast and prostate cancer-two cancers commonly diagnosed through screening-argues against this bias. Another possible explanation is shared lifestyle and other cancer risk factors. However, rates of tobacco smoking are substantially different between these two populations, being similar to those in the general population in kidney transplant recipients,5,26 and around double population rates in people with HIV/AIDS.27 Despite this marked difference, meta-analysis SIRs for tobacco-related cancer were not consistently higher in the HIV/AIDS cohorts. Differences in cancer risk factors could nevertheless explain some differences in cancer patterns. For example, the higher exposure to sexually transmitted oncogenic viruses in people with HIV/AIDS28 probably explains their higher rates of Kaposi's sarcoma and liver and anal cancer.
The two greatest strengths of our study are its statistical power, and the comparison between two populations that do not share lifestyle and host cancer risk factors. We believe that the striking similarity in patterns of increased cancer risk that we have shown indicates that immune deficiency is the probable explanation for the increased cancer risk. This interpretation is by contrast with that from the largest single study of cancer risk in people with HIV/AIDS,4 (2001) which found no relation between immune deficiency-as measured by CD4 count at AIDS diagnosis-and risk of most of types of cancer. We believe that CD4 count at AIDS diagnosis could be an insensitive indicator of association with immune deficiency. First, the relation between cancer risk and degree of immune deficiency might not always be linear, and could be different for different types of cancer. For example, the striking increase in risk of HPV-related cancers seen in long-term transplant recipients5,6 suggests that even modest immune suppression, if present for long enough, could increase the risk of these cancers. Second, CD4 count at AIDS diagnosis might not be an accurate or unbiased measure of immune function at cancer onset. The initiation of antiretroviral therapy can lead to pronounced and prolonged increases in immune function.29
In comparing the data between these two populations, some limitations in the source data must be considered. First, our data from transplant recipients came almost exclusively from renal transplant recipients. However, the fact that increases in cancer incidence in renal transplant recipients are largely confined to the post-transplant period5 suggests that it is immune suppression-rather than chronic renal disease or dialysis-that accounts for the increased cancer risk. Second, whereas the transplantation studies were of fairly homogeneous design, the studies of people with HIV/AIDS varied considerably. The bulk of the data came from studies that followed people only after the onset of AIDS,4,9,10 and in the era of highly active antiretroviral therapy (HAART), these people comprise an increasing minority of HIV-infected people. In the studies of people with HIV/AIDS, most reports included person-years in the 5 years before AIDS,2,4,10 but others included only the post-AIDS period,9,17 and the duration of the post-AIDS follow-up varied. Since immune deficiency varies considerably during the natural history of HIV infection, and is also affected by treatment, the degree of immune deficiency probably varied across the HIV/AIDS studies. Although most of the studies covered both the pre-HAART and post-HAART eras, the only study that compared non-AIDS-defining cancer rates before and after HAART found that rates of most non-AIDS-defining cancers did not change.9 Third, some studies did not report data covering all cancer types. Nonetheless, there was no demonstrable publication bias. A fourth issue concerns comparing meta-analysis SIRs between the two populations. Since each SIR is based on a different set of standard rates, differences in the age and sex structure of the populations could confound simple interpretation of differences in meta-analysis SIRs. For that reason, we concentrated on the interpretation of patterns of increased risk rather than focusing on individual meta-analysis SIRs.
About 40 years ago, Burnet proposed the immunological surveillance theory of cancer,30 which postulated that the immune system was responsible for the recognition of specific antigens present on the surface of cancer cells and the destruction of the emerging cancer clone. A functional immune system was seen as having a key role in the prevention of the emergence of clinical malignancy. The theory predicted that immune deficient populations should experience high rates of cancer of all types. Clearly, this is not the case, and until now, it has been concluded that only a few viral-associated cancers are related to immune deficiency.24 The increased rates of cancers we have found at a very large range of sites suggests a broader than previously appreciated role for the immune system in the prevention of cancers related to infection. If immune deficiency is associated with such a broad range of cancer types, then cancer is likely to become an increasingly important cause of morbidity in people with HIV/AIDS.
Methods
Search strategy and selection criteria
We followed published guidelines for meta-analyses of observational studies.7 To be eligible for inclusion, studies had to meet the following criteria: (1) they were cohort studies of people with HIV/AIDS, or of solid organ transplant recipients; (2) they included mainly adults; and (3) they collected data on incident cancer through cancer registers in developed countries. Studies that accepted other cancer diagnoses without confirming that these were notified to a cancer registry were not included to ensure an unbiased comparison of cohort cancer incidence rates to the general population with standardised incidence ratios (SIRs).
Two of the authors (AEG and CMV) searched for articles reported up to March, 2007, in PubMed, with combinations of the search terms "HIV", "AIDS", "transplant", "cancer", "cohort", and "linkage", and a search of reference lists of relevant papers. For people with HIV/AIDS, a broad search identified 69 potentially relevant papers, 46 of which were excluded: 37 after review of the title and nine after review of the abstract. For transplant recipients, the broad search identified 92 papers, 84 of which were excluded after title review and two after abstract review. Reviews were done by AEG and CMV; disagreements were resolved by mutual discussion and no disagreements required adjudication. Thus, 23 papers for people with HIV/AIDS and six papers for transplant recipients met the criteria and were reviewed in full. There were no articles in languages other than English which, based on the abstract review, met the criteria. One small HIV/AIDS study presented data that were internally contradictory with respect to the number of cancers expected and the SIR; contact with the author was attempted but was unsuccessful, so the study was excluded.8 For studies that had more than one report, the most recent report of cancer incidence for each specific cancer site was used where there was a possibility of overlapping data. After this exclusion, there were seven reports of cancer incidence in people with HIV/AIDS, and five in transplant recipients (figure 1).
Statistical analysis
For each study, we abstracted the observed and expected number of cancer cases by cancer site or grouping of sites; this step was done by one investigator (AEG) and checked by two others (CMV, MOF). Frequently, the number of expected cases was not presented, but could be calculated by dividing the number of observed cases by the reported SIR. Across the studies, there was some variation in the nomenclature and grouping of cancer sites. We used International Classification of Disease codes when available to ensure that cancers of the same sites were pooled.
A slightly different method of analysis was required for AIDS-defining cancers. For studies for which the point of cohort entry was the diagnosis of AIDS,4,9,10 by definition no follow-up was available when the cancer diagnosis was concurrent with AIDS diagnosis. Thus, for these studies, only data on AIDS-defining cancers occurring in the post-AIDS period were included. For studies for which cohort entry was HIV diagnosis, data for the entire follow-up period were included. Additionally, for Kaposi's sarcoma, because almost all cases occurred in people with HIV infection in all countries in which the studies were based, data were only included if the report used a pre-AIDS population rate of Kaposi's sarcoma to calculate a SIR.5,9
We postulated that the cancers that occurred at increased rates would be mostly infection-related cancers; we thus grouped cancers by known or suspected infectious cause.11 Additionally, we specifically considered incidence rates of the most common epithelial cancers, and other cancer types that occurred at increased rates in one or both populations.
Study-specific SIRs for each cancer type were calculated by dividing the number of observed cases by the number expected, and were combined by use of both fixed and random-effects models to estimate the overall pooled estimates.12 Tests for heterogeneity between study results were done with Cochran's Q statistic.13 Due to the presence of significant heterogeneity in the meta-analysis SIRs for several cancer sites for people with HIV and people with organ transplantation, only the results for the random-effects model are reported.
The effect of individual studies on the meta-analysis SIRs was assessed by re-estimating the overall effect after omitting each study. The potential for publication bias was graphically explored through the production of funnel plots, and tested for significance with Egger's test for asymmetry.14 All statistical procedures used a two-sided significance level of 0·05, and were done with Stata version 8.2.
Role of the funding source
There was no funding source for this study. All authors had access to all the data. The corresponding author had final responsibility for the decision to submit for publication.
|
|
| |
| |
|
|
|