 |
 |
 |
| |
A Pilot Study assessing Raltegravir QD versus BID
in HIV patients included in a Simplification Trial
|
| |
| |
Reported by Jules Levin
ICAAC Sept 13 2009 San Francisco
A. Mena, F. Blanco, M. Cordoba, S. Rodriguez-Novoa, J. Morello, I. Jimenez-Nacher and V. Soriano
Department of Infectious Diseases, Hospital Carlos III, Madrid.
AUTHOR CONCLUSIONS
Administration of RAL QD appears to be as effective and safe as BID, with the benefit of an improved QOL.
BACKGROUND
Raltegravir (RAL) is a potent and safe antiretroviral agent so far approved to be used BID.
However, pharmacokinetic and pharmacodynamic data support the use of RAL QD:
The daily area under the concentration-time curve instead of the trough concentration is the most relevant pharmacokinetic parameter associated with the antiviral effect of RAL.1
RAL has a very long intracellular half-life (t1/2 ∼ 29 h).
The residence time of RAL on the integrase/DNA complex is comparable or exceeding the t1/2 of the pre-integration complex within the cell, resulting in a functionally irreversible inhibition of the integrase.2
METHODS
Of 311 HIV patients who received RAL at our institution between December 2005 and January 2009, a prospective pilot study was performed in those patients with plasma HIV-RNA <50 copies/ml who replaced PIs by RAL.
Patients were allocated to receive RAL 800 mg QD vs BID according to the dosage of the other drugs included in the regimen (QD or BID).
Clinical and immuno-virological parameters, adherence and quality of life (QOL) were analyzed at baseline, month 1 and every 3 months thereafter.
Statistical Analysis. Results are expressed as percentages for categorical variables and as median and interquartile range for continuous variables. Continuous variables were compared using the Mann-Whitney U test. Proportions were compared using the chi-square test. Statistical differences were considered when p value was < 0.05.
RESULTS
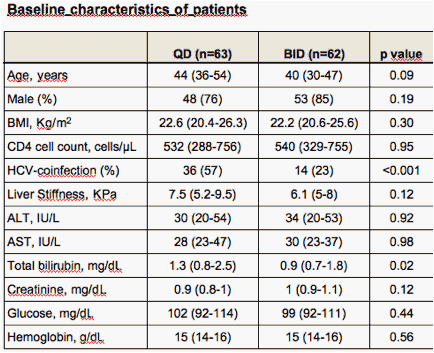
CLINICAL OUTCOMES
Median follow up was 15 (9-30) months.
Discontinuation of RAL.
-- Five patients discontinued RAL due to virological failure, 1 in the QD arm and 4 in the BID arm (p=0.74). All 5 had failed NRTI in the past.
-- Four patients discontinued RAL for other reasons: 1 voluntary withdrawal in the QD arm and 3 in the BID arm (poor adherence 2, headache 1).
-- There were no differences in CD4 T cell gains comparing the QD and BID arms.

CD4 count (cells/uL) in the QD and BID, p >0.05.
RAL was safe and well tolerated in both arms.
Adherence was >90% in both groups.
Patients on RAL QD showed a trend towards improved QOL compared to BID patients.
REFERENCES
1. McSharry, et al. 10th International Workshop on Clinical Pahrmacology of HIV Therapy. Abstract O_09.
2. Grobler, et al. 10th International Workshop on Clinical Pahrmacology of HIV Therapy. Abstract O_10.
|
| |
|
 |
 |
|
|