 |
 |
 |
| |
Brief Interruption of HIV Antiretroviral Therapy in Patients with Preserved CD4 Count and Virologic Suppression is Safe and Well Tolerated
|
| |
| |
Reported by Jules Levin
IDSA Oct 17-21 2012 San Diego
Meghan Rothenberger, M.D.1, Ashley Haase, M.D.2, Alexander Khoruts, M.D.1, Gregory Beilman, M.D.3, Jeffrey Chipman, M.D.3, Ann Thorkelson, R.N.1, Cavan Reilly, Ph.D.4, Netanya Sandler, M.D.5, Daniel Douek, M.D., Ph.D. 5, Mario Stevenson, Ph.D.6 and Timothy W. Schacker, M.D.1
Departments of Medicine1, Microbiology2, Surgery3, and Biostatistics4 at the University of Minnesota and the Human Immunology Section of the Vaccine Research Center6 at the National Institutes of Health

BACKGROUND
Current combination antiretroviral therapy (cART) can suppress virus in peripheral blood but cannot cure HIV (1). When ART is withdrawn, viral rebound generally occurs quickly and disease progression resumes (2-4). Given the limitations of standard cART, new therapies are being developed to enhance immune responses against HIV such that cART can be interrupted without virologic rebound. Determining the efficacy of such novel therapies will require interruption of standard cART, yet there is controversy regarding the use of even short structured treatment interruptions (STIs) in clinical studies given safety concerns (5). We therefore assessed the safety of a short STI, similar to what could be employed in clinical studies of novel therapies, in subjects with consistently suppressed viral load (VL) and preserved CD4 T cell count.
Program Abstract
Brief Interruption of HIV Antiretroviral Therapy in Patients with Preserved CD4 Count and Virologic Suppression is Safe and Well Tolerated
Saturday, October 20, 2012
Background: Management goals for HIV are shifting from chronic viral suppression to functional cure; i.e. control of HIV in the absence of combination antiretroviral therapy (cART). Assessment of such novel treatments will require interruption of standard cART, yet structured treatment interruptions (STIs) have generally been avoided given safety concerns. This study was designed to assess the safety, as determined by resumption of virologic control after treatment re-initiation, maintenance of CD4 T cell count, and lack of clinical adverse events, of a short-term STI in patients with preserved CD4 T cell count and virologic suppression on cART.
Methods: 14 HIV-infected individuals with CD4 count >350 cells/mm3 and virologic suppression on cART were enrolled in an STI treatment protocol designed to characterize HIV reservoirs. All subjects underwent interruption of cART at study initiation. Peripheral blood CD4 count and HIV viral load were assessed 3 times weekly while off of cART. Once HIV RNA was detected in peripheral blood, samples for the reservoir study were collected, genotype was obtained and cART was restarted. CD4 count and HIV viral load were followed weekly until viral load was undetectable then intermittently for up to 90 days.
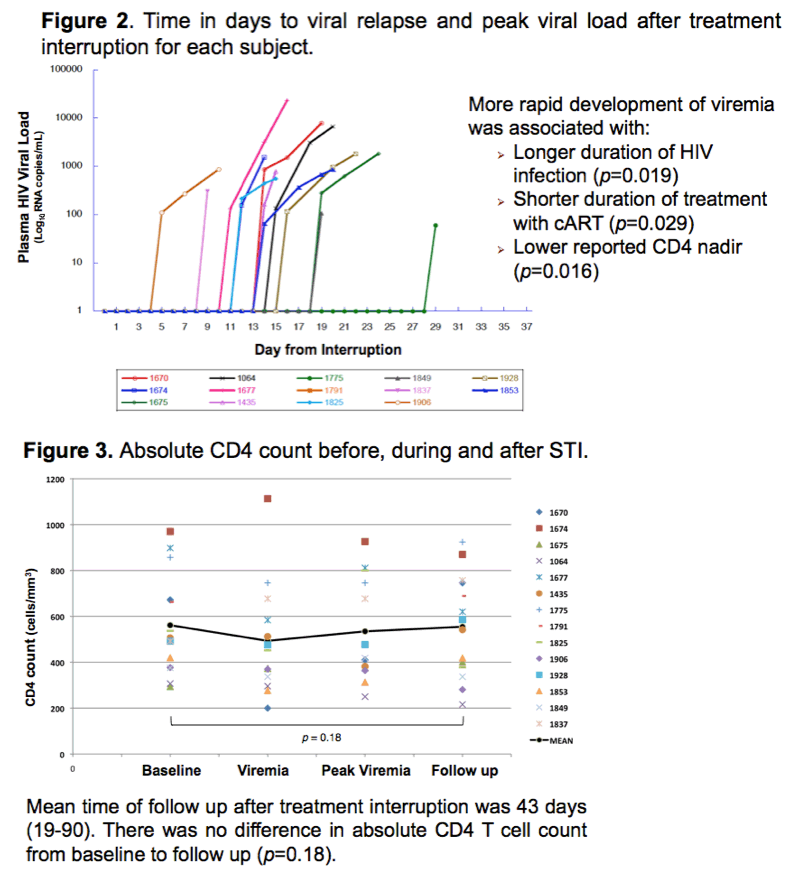
Results: After cART discontinuation, median time to HIV viremia was 14 days (range 5-29). At cART re-initiation, median viral load was 871 copies/mL (60-23,402 copies/mL). Longer duration of HIV infection and lower reported CD4 nadir were associated with more rapid virologic rebound (p=0.019 and 0.016). Longer lifetime exposure to ART was associated with more prolonged time to viremia (p=0.029). Once cART was restarted, all subjects achieved peripheral blood viral suppression, with median time to suppression being 14 days (7-47). CD4 count at treatment resumption did not differ from study initiation (p=0.18), no new resistance-conferring mutations were detected in any subject and none had symptoms associated with reactivation of viral replication. No subjects developed virologic failure during post-STI follow up period.
Conclusion: Brief interruption of cART in patients with preserved CD4 count and virologic suppression is safe for the evaluation of novel therapies to test for cure of HIV.
Study Design
Between July 2009 and July 2011, 14 subjects were enrolled in an STI treatment protocol developed to characterize HIV reservoirs in patients on cART. Subjects who were >18, virally suppressed at least 12 months and had CD4 count >350 cells/mm3 were eligible to enroll.
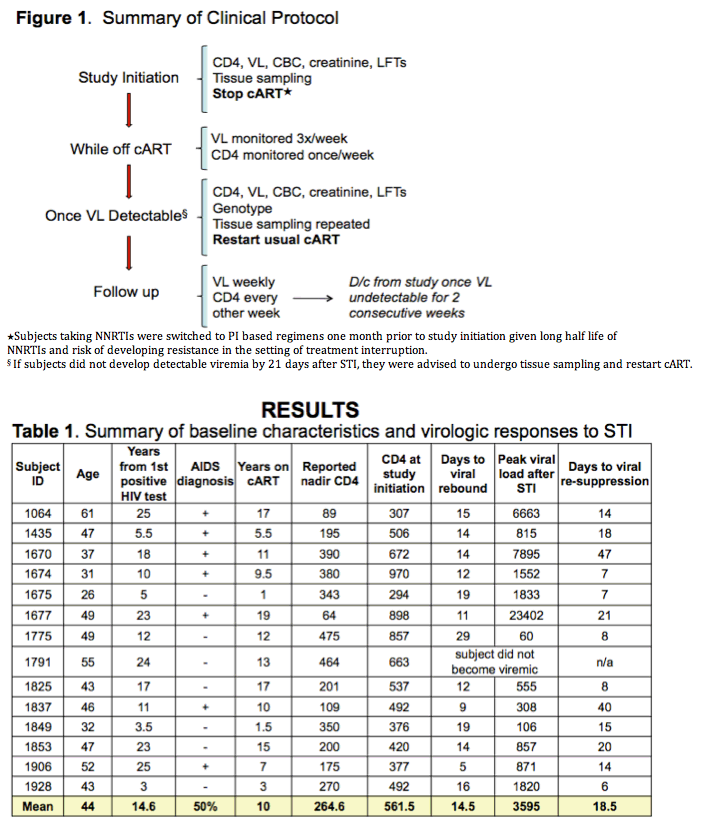
4 subjects were on NNRTIs (switched to PI based regimens one month prior to study initiation), 3 were on raltegravir and the remainder were on PIs. Subject 1791 did not become viremic during STI and was put back on cART on day 22. Subject 1775 chose to stay off of therapy until viral rebound occurred at day 29. Once virally suppressed, all subjects remained suppressed. No new resistance mutations were detected on genotype obtained during viremia and no subjects experienced symptoms associated with virologic rebound.

|
| |
|
 |
 |
|
|