 |
 |
 |
| |
HIV Care Cascade Analysis Not So Dire in Large US Healthcare System
|
| |
| |
20th Conference on Retroviruses and Opportunistic Infections, March 3-6, 2013, Atlanta
Mark Mascolini
Linkage to HIV care and retention in care after diagnosis may not directly affect rates at which HIV-positive US patients start antiretroviral therapy (ART) or reach an undetectable viral load, according to a 16,816-patient analysis in the Kaiser Permanente healthcare system [1]. The findings suggest that linkage and retention estimates do not always reflect how many HIV-positive people start and respond well to treatment.
HIV care proceeds through a series of steps--often called an engagement cascade--starting with HIV diagnosis and proceeding through linkage to care, retention in care, prescription of ART, and reaching an undetectable viral load [2,3]. Each of these steps presents a challenge to an HIV-positive person and to the health workers who try to guide them through consistent care. Typically, researchers consider attainment of each step dependent upon attainment of the preceding step, so that people are counted as reaching an undetectable viral load only if they first meet certain definitions of getting linked to care, remaining in care, and getting an antiretroviral prescription.
But researchers from the Kaiser Permanente healthcare system, which provides care in eight states and Washington, DC, argued that people who do not meet the definition for one step in the cascade may actually complete subsequent steps successfully. "Thus," they maintained, "requiring sequential success may underestimate actual success in later stages, and can misguide policy and planning." They conducted this study to test their hypothesis that a rigidly applied cascade model underestimates the success of HIV care in the United States, at least in a healthcare system in which everyone has equal access to care.
The investigators identified everyone in the Kaiser healthcare system diagnosed with HIV, at least 13 years old, and with at least 8 months of Kaiser membership in the year 2010. They assessed success in achieving each of the four steps of the engagement cascade after diagnosis, defined as follows:
Linked to care: For new patients, first visit to a qualified provider or CD4 measurement within 90 days of being identified as HIV positive; for previously established patients, at least one medical visit during 2010
Retained in care: At least two medical visits separated by at least 60 days
Filled ART prescription: Filled prescriptions for an antiretroviral combination meeting the Department of Health and Human Services definition of ART
Achieved viral suppression: Viral load below 200 copies any time during 2010, or viral load below 200 copies at last measure in 2010
Next the Kaiser team determined success in achieving these four steps by two methods: (1) a "dependent" method in which success of a later stage requires success in all earlier stages, and (2) an "independent" method in which success in each stage is measured separately
The study involved 16,816 HIV-positive people, 87% of them male, and 61% between 35 to 54 years old. Median CD4 count at HIV diagnosis stood at 391 and 83% had their CD4 count measured every 6 months. Median ART adherence stood at 94%.
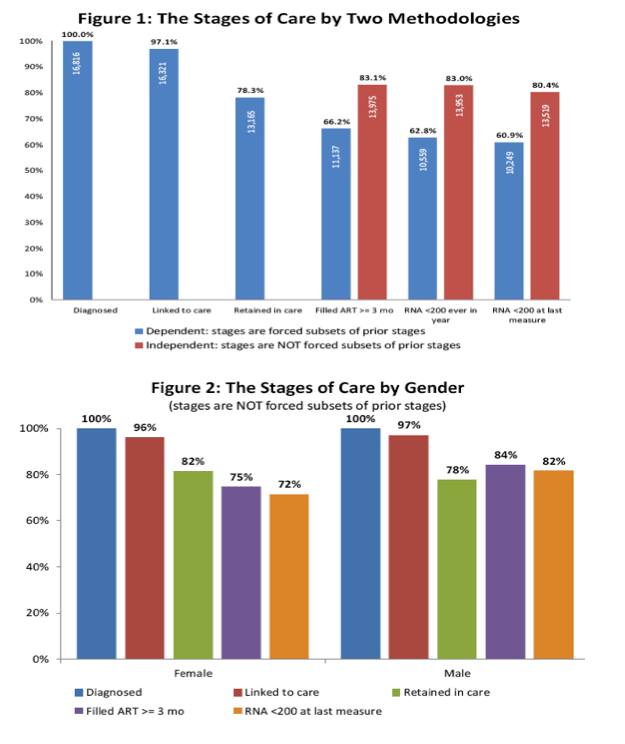
By the dependent method, the 100% of people diagnosed with HIV plunged to 66% who filled their ART prescription and to below 63% with an undetectable viral load in the last step of the cascade. In contrast, by the independent method, 83% filled their ART prescription and almost that many had an undetectable viral load:
-- Diagnosed: 100% dependent method
-- Linked to care: 97.1% dependent
-- Retained in care: 78.3% dependent
-- Filled ART prescription: 66.2% dependent vs 83.1% independent
-- Viral load below 200 ever in 2010: 62.8% dependent vs 83.0% independent
-- Viral load below 200 at last measure in 2010: 60.9% dependent vs 80.4% independent
The 17% difference in the filled ART prescription step was highly statistically significant (P < 0.001), as was the 20% difference in viral suppression rates ever in 2010 (P < 0.0001).
Using the independent calculation method, the Kaiser team found gender-based differences in several steps of the engagement cascade:
-- Linked to care: 97% male vs 96% female, P = 0.01
-- Retention in care: 78% male vs 82% female, P < 0.001
-- Filled ART prescription: 84% male vs 75% female, P = 0.02
-- Achieved viral suppression: 82% male vs 72% female, P < 0.001
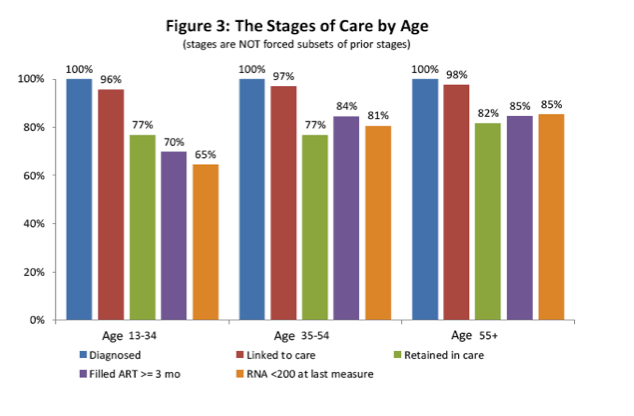
Older age was significantly associated with a higher rate of filling ART prescriptions (P < 0.001) and achieving viral suppression (P < 0.001), but not linking to care (P = 0.88) or retention in care (P = 0.07). (See Figure 3 in poster linked below for details.)
The Kaiser researchers cautioned that their estimates of success may not apply to all clinical settings and health insurance plans. They concluded that "success in later stages of the HIV care cascade is not necessarily dependent on success in earlier stages." The gender- and age-based differences in the engagement cascade suggest that stratifying such analyses by gender and age can yield helpful insights into the success of HIV care.
References
1. Horberg M, Hurley L, Towner W, et al. HIV spectrum of engagement cascade in a large integrated care system by gender, age, and methodologies. 20th Conference on Retroviruses and Opportunistic Infections. March 3-6, 2013. Atlanta. Abstract 1033. http://www.retroconference.org/2013b/PDFs/1033.pdf
2. Centers for Disease Control and Prevention. CDC fact sheet: HIV in the United States: The stages of care. 2012.
3. Gardner EM, McLees MP, Steiner JF, Del Rio C, Burman WJ. The spectrum of engagement in HIV care and its relevance to test-and-treat strategies for prevention of HIV infection. Clin Infect Dis. 2010;52:793-800. http://cid.oxfordjournals.org/content/52/6/793.long
|
| |
|
 |
 |
|
|