 |
 |
 |
| |
Osteoporosis Triples Risk of Later Fracture in 1000-Person US HIV Group
|
| |
| |
Osteoporosis Triples Risk of Later Fracture in 1000-Person US HIV Group
14th European AIDS Conference. October 16-19, 2013. Brussels
Mark Mascolini
Only three factors independently predicted a new fracture in a combined analysis of the US HOPS and SUN Study HIV cohorts--older age, smoking, and osteoporosis. Osteopenia did not affect fracture risk in multivariate or univariate analyses.
Several studies confirm a higher fracture rate in people with than without HIV infection. For example, in a 5826-person HIV Outpatient Study (HOPS) analysis, HOPS members 25 to 54 years old had a higher fracture rate and a higher relative proportion of fragility fractures than did a general-population comparison group [2]. Low bone mineral density (BMD) is frequent in HIV populations, but a link between low BMD and subsequent fracture had not been demonstrated in people with HIV.
To explore the possible association between low BMD and later fracture--which has been demonstrated in the general population--CDC researchers and collaborators analyzed combined data from the SUN Study and HOPS, two prospective US cohorts. They focused on people who had at least one DEXA scan to determine BMD and follow-up to the last patient contact or to June 2012 (SUN) or September 2012 (HOPS). They defined osteopenia and osteoporosis by DEXA-measured T score in the standard way, and they defined incident fracture as all fractures.
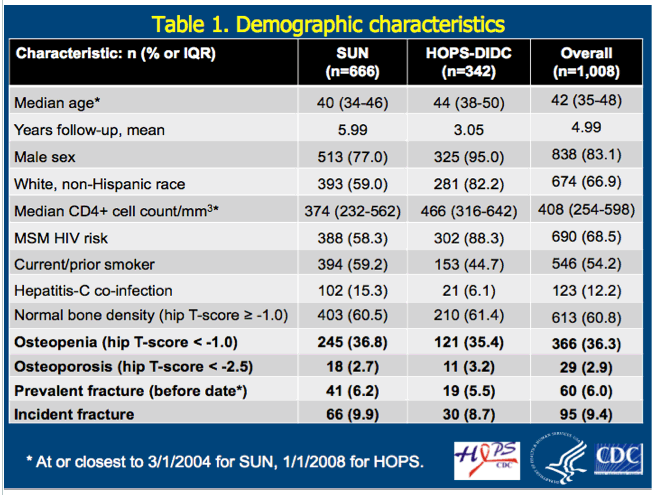
Median age of the combined 1008-person groups was 42 (interquartile range [IQR] 35 to 48), 83% were men, 68.5% men who have sex with men (MSM), and 67% non-Hispanic white. Median CD4 count stood at 408 (IQR 254 to 598). More than half of cohort members (54%) were current or former smokers, and 12% had HCV infection.
DEXA scans determined that 366 people (36.3%) had osteopenia and 29 (2.9%) had osteoporosis. Sixty people (6%) had a fracture before follow-up began.
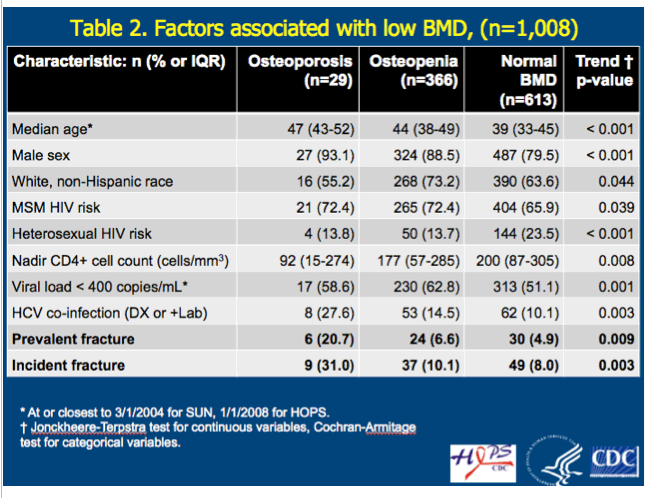
People with osteopenia or osteoporosis were significantly older and included significantly higher proportions of men, MSM, and whites. People with osteoporosis had a significantly lower average nadir CD4 count than those without osteoporosis (92 versus 200, P = 0.008). HCV infection was more prevalent in people with osteoporosis (27.6%) or osteopenia (14.5%) than in those with neither condition (10.1%) (P = 0.003).
Significantly more people with osteoporosis than with osteopenia or neither condition already had a fracture when follow-up began (20.7% versus 6.6% versus 4.9%, P = 0.009), and significantly more people with osteoporosis had a new fracture during follow-up (31% versus 10.1% versus 8%, P = 0.003).
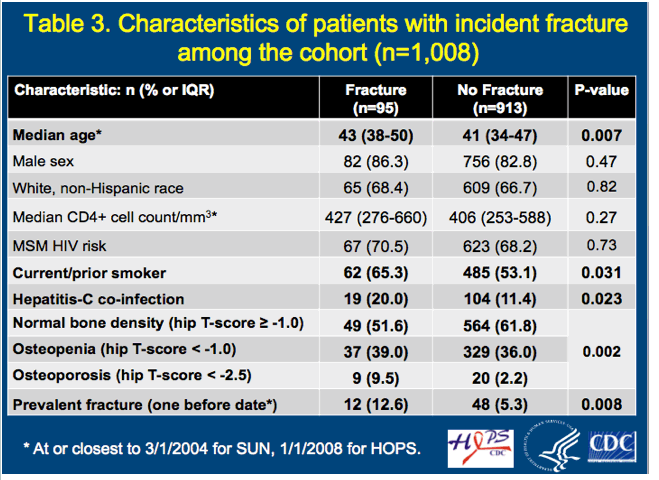
During a median follow-up of 5 years, 95 people (9.4%) fractured a bone. Fractures were most common in the rib/sternum (18), hand (17), foot (15), and wrist (11). Compared with people who did not break a bone during follow-up, those who did were significantly older (median 43 versus 41, P = 0.007) and more likely to be a current or former smoker (65.3% versus 53.1%, P = 0.031), to have HCV infection (20.0% versus 11.4%, P = 0.023), and to have a previous fracture (12.6% versus 5.3%, P = 0.008).
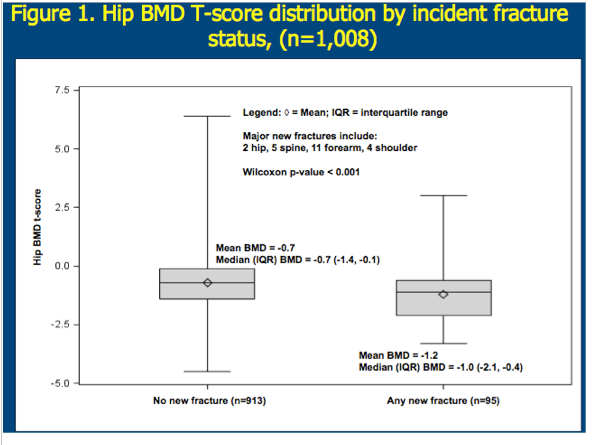
People with a new fracture were less likely to have normal bone density (T score > -1) and more likely to have a T score below -2.5, indicating osteoporosis (P = 0.002). Median BMD was -1.0 (IQR -2.1 to -0.4) in people who broke a bone during follow-up and -0.7 (IQR -1.4 to -0.1) in those who did not.
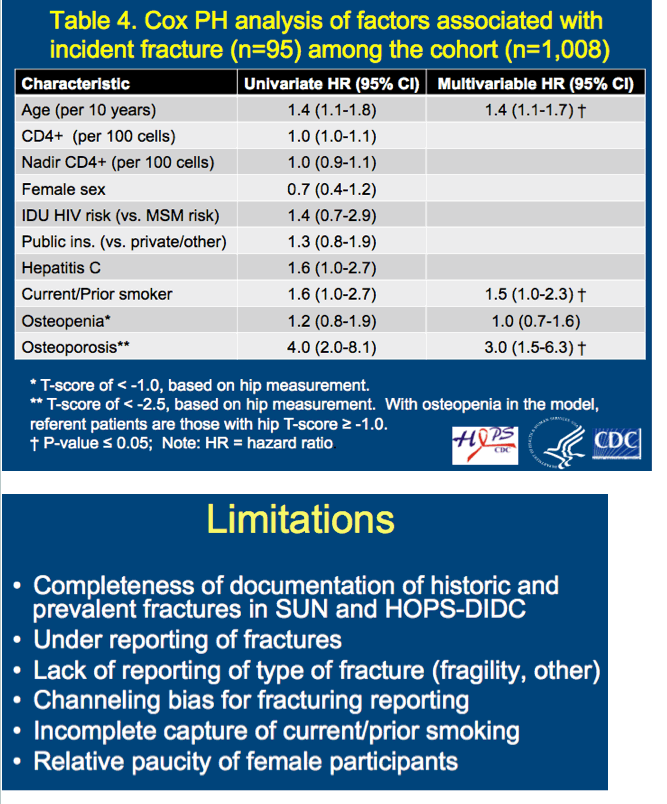
Multivariate analysis identified three factors associated with a higher risk of fracture during follow-up. Osteoporosis tripled the risk (adjusted hazard ratio [aHR] 3.0, 95% confidence interval [CI] 1.5 to 6.3), every additional 10 years of age raised the risk 40% (aHR 1.4, 95% CI 1.1 to 1.7), and current or former smoking upped the risk 50% (aHR 1.5, 95% CI 1.0 to 2.3) (P < 0.05 for all associations). Factors not independently associated with incident fracture in this analysis were osteopenia, current or nadir CD4 count, gender, injection drug use versus MSM transmission risk, public versus private insurance, and HCV infection.
The HOPS/SUN team noted that this analysis is limited by their inability to distinguish fragility fractures from other fractures. They questioned whether fracture reporting and smoking data were complete in these patients and suspected underreporting of fractures. The investigators suggested that channeling bias my affect their results: people referred for DEXA scanning may be those with more fracture risk factors. They also cautioned that women made up only 17% of the study group. Because the analysis found a strong association between osteoporosis and subsequent fracture in this relatively young population, the researchers suggested that DEXA screening may be a valuable clinical tool in people with HIV.
References
1. Battalora L, Buchacz K, Armon C, et al. Low bone mineral density is associated with increased risk of incident fracture in HIV-infected adults. 14th European AIDS Conference. October 16-19, 2013. Brussels. Abstract PS1/4.
2. Young B, Dao CN, Buchacz K, Baker R, Brooks JT; HIV Outpatient Study (HOPS) Investigators. Increased rates of bone fracture among HIV-infected persons in the HIV Outpatient Study (HOPS) compared with the US general population, 2000-2006. Clin Infect Dis. 2011;52:1061-1068. http://cid.oxfordjournals.org/content/52/8/1061.long
----------------------------------
Reported by Jules Levin
Low Bone Mineral Density (& increasing age) is Associated with Increased Risk of Incident Fracture in HIV-infected Adults
Reported by Jules Levin, 14th European AIDS Conference; October 16-19, 2013; Brussels, Belgium
Linda A. Battalora1, Kate Buchacz2, Carl Armon3, Edgar T. Overton4, John Hammer5, Pragna Patel2, Joan S. Chmiel6, Kathy Wood3, Timothy J. Bush2, John T. Brooks2, Benjamin Young7,8 for the HIV Outpatient Study (HOPS) and SUN Study Investigators
1Colorado School of Mines; 2Centers for Disease Control and Prevention; 3Cerner Corporation; 4University of Alabama School of Medicine; 5Denver Infectious Disease Consultants; 6Feinberg School of Medicine, Northwestern University; 7APEX Family Medicine; 8International Association of Providers in AIDS Care
Although the prevalence of both low bone mineral density (BMD) and bone fractures are increased among HIV-infected adults compared with the general population, no study has yet characterized their causal association in the context of HIV infection.
RESULTS
· Presence of baseline osteoporosis is strongly associated with increased risk of incident fracture in this population of relatively young HIV-infected adults
· Similar to previous analysis (Young 2011), fracture risk is associated with increasing age
CONCLUSIONS
· In a large convenience sample of relatively young HIV-infected adults in the U.S., low baseline BMD and increasing age were strongly associated with elevated risk of incident fracture.
· Early detection of low BMD or risk of low BMD provides opportunity for earlier intervention to prevent fractures in HIV-infected patients.
ABSTRACT
Objectives: Although the prevalence of both low bone mineral density (BMD) and bone fractures are increased among HIV-infected adults compared with the general population, no study has yet characterized their causal association in the context of HIV infection.
Methods: We analyzed available dual energy X-ray absorptiometry (DEXA) values of the hip (left femoral neck) and clinical data collected prospectively during 2004-2012 from two CDC-sponsored HIV cohort studies, the HOPS and the SUN Study. We assessed factors associated with low BMD (osteopenia or osteoporosis, defined by T-scores of -1.0 to >-2.5, and ≤ -2.5, respectively), using the Jochkheere-Terpstra test for ordered alternatives for continuous variables and the Cochran-Armitage test for categorical variables. We analyzed the association of low BMD with subsequent incident fractures using Cox proportional hazards regression.
Results: Among 1008 patients (median age 42 [interquartile range (IQR)35-48] years, 83% male, 67% non-Hispanic white, median CD4+ cell count [CD4] 408 cells/mm3 [IQR 254-598]), 36.3% (n=366) had osteopenia and 2.9% (n=29) osteoporosis. During 5,032 person-years of observation after DEXA scanning, 95 incident fractures occurred, predominantly rib/sternum (n=18), hand (n=17), foot (n=15) and wrist (n=11).
Low BMD was significantly (p< 0.05) associated with age, lower nadir CD4, history of fracture, and male-male sex HIV transmission risk. In unadjusted analyses, age, current or prior tobacco smoking, hepatitis C co-infection, history of fracture, and low BMD (osteopenia or osteoporosis) were significantly associated with increased hazard of a new fracture.
In multivariable analyses, only osteoporosis (adjusted hazard ratio [aHR] 3.04, 95% confidence interval [CI]1.47-6.30) and age (aHR 1.35 per 10 years, 95% CI 1.07-1.70) remained associated with incident fracture. (from jules: and current/prior smoking, see Table 4.
Conclusion: In a large convenience sample of HIV-infected adults in the U.S., low baseline BMD and increasing age (from Jules: and smoking current/prior, see Table 4.) were strongly associated with elevated risk of incident fracture, highlighting the potential value of DEXA screening in this population.
Limitations
· Completeness of documentation of historic and prevalent fractures in SUN and HOPS-DIDC
· Under reporting of fractures
· Lack of reporting of type of fracture (fragility, other)
· Channeling bias for fracturing reporting
· Incomplete capture of current/prior smoking
· Relative paucity of female participants


BACKGROUND
·Low bone mineral density (BMD) is linked to increased fracture risk in the general population (NOF 2010; Kanis 2000; Walker Harris 2012)
·Low BMD is common among people living with HIV (Tebas 2000; Mondy 2003; Brown 2006; Overton 2007)
·Increased bone fracture rates seen in multiple HIV cohorts (Triant 2008; Yin 2010; Young 2011; Bedimo 2012; Hansen 2012; Womack 2013)
·To date, no data link low BMD to incident fracture risk in HIV+ populations
OBJECTIVES
·Characterize association between baseline BMD (defined by T-score normal, osteopenia, and osteoporosis) and incident fractures in HIV-infected adults



|
| |
|
 |
 |
|
|