 |
 |
 |
| |
Neither HIV Nor Tenofovir Tied to Low Bone Density in Large Amsterdam Study (AGEhIV Cohort)
|
| |
| |
14th European AIDS Conference. October 16-19, 2013. Brussels
Mark Mascolini
Neither HIV infection nor tenofovir use predicted low bone mineral density (BMD) in a 1100-person Amsterdam cohort of HIV-positive and negative people 45 or older [1]. Traditional risk factors, including low weight, did raise chances of lower BMD, but older men who have sex with men (MSM) had better chances of higher BMD.
Several factors, including chronic inflammation and antiretroviral therapy, may contribute to decreased BMD in people with HIV. Some research shows a greater decline in BMD with tenofovir-containing regimens [2], but the long-term impact of tenofovir and other antiretrovirals remains unclear [3]. Researchers working with Amsterdam's AGEhIV Cohort Study Group observed that many analyses of BMD in HIV-positive people are limited by lack of a comparison HIV-negative group.
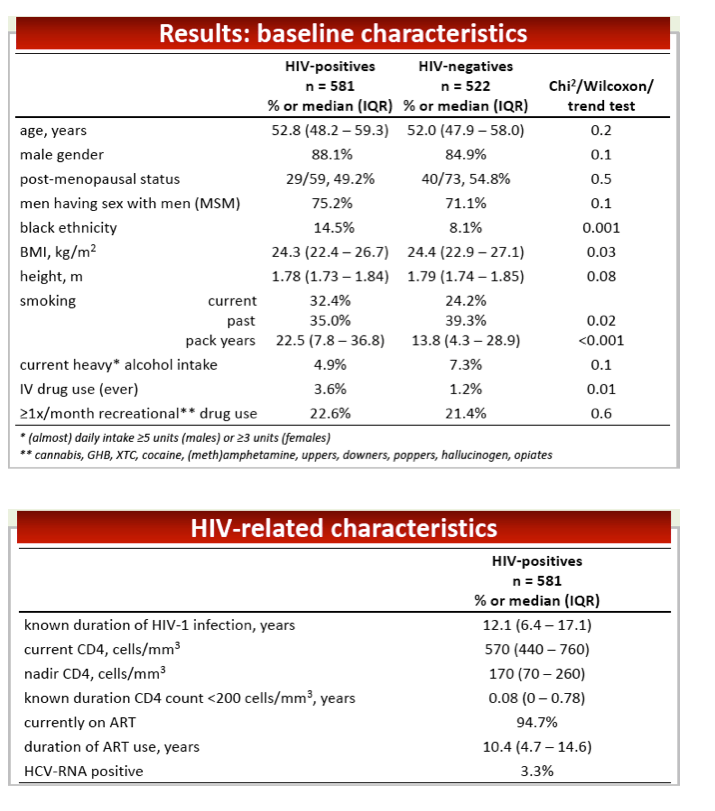
To address these issues, the AGEhIV team measured BMD at the lumbar spine, total hip, and femoral neck in a prospective cohort of 581 HIV-positive people attending an HIV outpatient clinic and 522 HIV-negative people attending the municipal sexually transmitted disease clinic and comparable to the HIV group in age, gender, and ethnicity. Median age was 52.8 in the HIV group and 52.0 in the HIV-negative group, and respective proportions of men were 88.1% and 84.9% and MSM 75.2% and 71.1%.
A higher proportion of HIV-positive people were current smokers (32.4% versus 24.2%), while more HIV-negative people were past smokers (39.3% versus 35.0%) (P = 0.02). Pack-years smoking were significantly higher in the HIV group (22.5 versus 13.8, P < 0.001). The HIV group had a significantly higher proportion of people who ever injected drugs (3.6% versus 1.2%, P = 0.01), but rates of current heavy alcohol use (4.9% and 7.3%) and recreational drug use (22.6% and 21.4%) did not differ significantly between groups.
Among people with HIV, median known duration of HIV infection was 12.1 years, current CD4 count 570, and nadir CD4 count 170. Most people with HIV (94.7%) were taking antiretroviral therapy, and median treatment duration stood at 10.4 years.
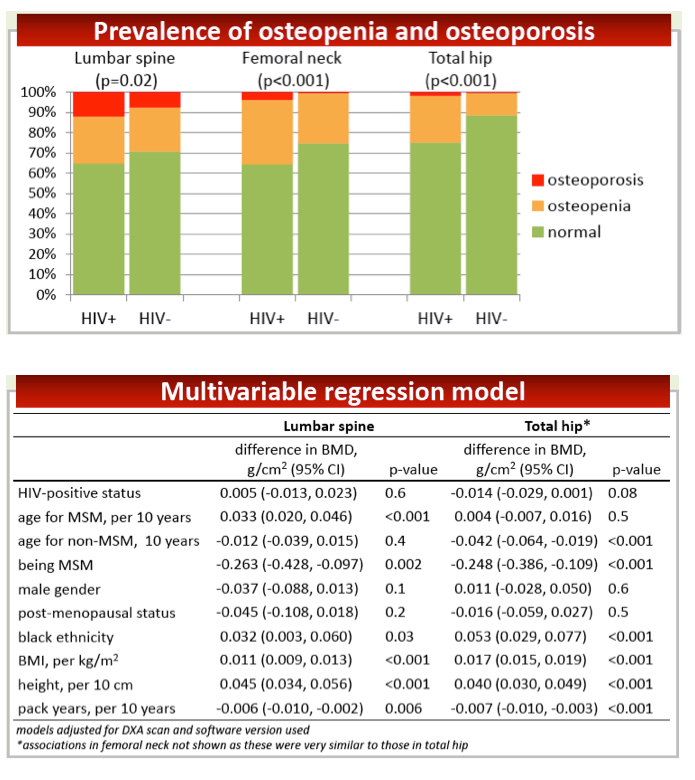
Significantly higher proportions of people with HIV had osteoporosis or osteopenia at the lumbar spine (P = 0.02), femoral neck (P < 0.001), and total hip (P < 0.001). In a multivariable regression model adjusted for age, gender, menopausal status, ethnicity, DXA-software changes, and body weight, having HIV infection was not associated with significantly lower BMD at the lumbar spine (difference 0.005 g/cm(2), P = 0.6) or total hip (difference -0.014 g/cm(2), P = 0.08). (Femoral neck values throughout this analysis were similar to those in the total hip.)
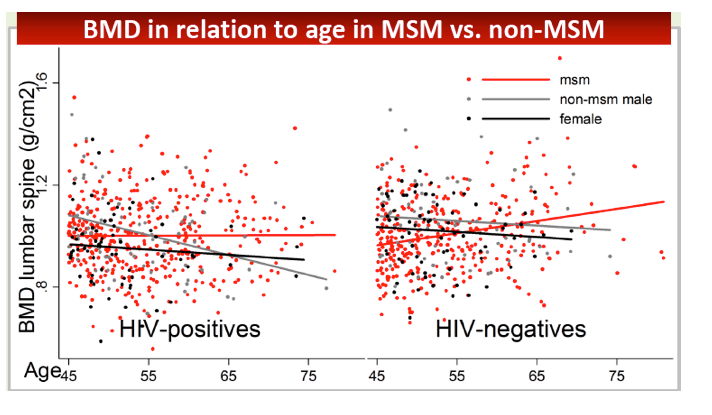
Every 10 years in age among HIV-positive and negative MSM were associated with significantly higher lumbar spine BMD (0.033 g/cm(2), P < 0.001) and nonsignificantly higher total hip BMD (0.004 g/cm(2), P = 0.5). In contrast, every 10 years of age in non-MSM were associated with significantly lower total hip BMD (-0.042 g/cm(2), P < 0.001) and nonsignificantly lower lumbar spine BMD (-0.012 g/cm(2), P = 0.4). The counterintuitive association between older age and higher BMD in MSM, the researchers suggested, "may be the result of unmeasured lifestyle and behavioral factors."
Two other factors were independently associated with lower BMD in this analysis of HIV-positive and negative cohort members: being an MSM (-0.263 g/cm(2), P = 0.002 for lumbar spine; -0.248 g/cm(2), P < 0.001 for total hip) and every additional 10 pack-years of smoking (-0.006 g/cm(2), P = 0.006 for lumbar spine; -0.007 g/cm(2), P < 0.001 for total hip). Factors that protected against BMD loss were black ethnicity (0.032 g/cm(2), P = 0.03 for lumbar spine; 0.053 g/cm(2), P < 0.001 for total hip), every kg/m(2) in body mass index (0.011 g/cm(2), P < 0.001 for lumbar spine; 0.017 g/cm(2), P < 0.001 for total hip), and every 10 cm in height (0.045 g/cm(2), P < 0.001 for lumbar spine; 0.040 g/cm(2), P < 0.001 for total hip).
An analysis focused on the HIV group found a significant association between longer time with a CD4 count below 200 and lower BMD (-0.008 g/cm(2)/y, P = 0.02) at the total hip), and HCV coinfection (-0.084 g/cm(2), P = 0.004 for total hip; -0.075 g/cm(2), P = 0.006 for femoral neck). This analysis disclosed no independent associations between known duration of HIV infection, or current or past tenofovir or protease inhibitor use at any of the three locations.
This large comparative study confirms a higher prevalence of osteopenia and osteoporosis in middle-aged to older people with HIV than in a comparable HIV-negative group. But statistical analysis accounting for other risk factors did not identify HIV infection as an independent risk factor for lower BMD at any of three sites. Instead, traditional risk factors (weight, smoking, ethnicity, and older age-in cohort members who were not MSM) were associated with BMD. Among HIV-positive people, treatment with tenofovir or protease inhibitors did not significantly affect BMD.
Bone-density risk factors not analyzed in this study that may contribute to the unexpected correlation between older age and greater bone density in MSM are family history, lack of weight-bearing activity, eating disorders, dietary calcium/vitamin D, corticosteroid use, and thyroid problems.
References
1. Kooij KW, Wit FW, Bisschop PH, et al. Reduced bone mineral density is largely explained by lower body weight in HIV-positive individuals and more pronounced in younger men having sex with men, regardless of HIV-status. 14th European AIDS Conference. October 16-19, 2013. Brussels. Abstract BPD1/4.
2. McComsey GA, Kitch D, Daar ES, et al. Bone mineral density and fractures in antiretroviral-naive persons randomized to receive abacavir-lamivudine or tenofovir disoproxil fumarate-emtricitabine along with efavirenz or atazanavir-ritonavir: Aids Clinical Trials Group A5224s, a substudy of ACTG A5202. J Infect Dis. 2011;203:1791-1801.
3. Bolland MJ, Wang TK, Grey A, Gamble GD, Reid IR. Stable bone density in HAART-treated individuals with HIV: a meta-analysis. J Clin Endocrinol Metab. 2011;96:2721-2731. http://jcem.endojournals.org/content/96/9/2721.long
----------------------
Bone Loss Worse in HIV+ vs HIV-Neg, Lower Body Weight Predicts Bone Loss in MSM: "Prevalence and determinants of reduced bone mineral density in aging HIV-1-positive and HIV-negative individuals" in AGEhIV Cohort Amsterdam
Reported by Jules Levin
EACS - European AIDS Conference 2013 Oct 16-19 Brussels, Belgium

K.W. Kooij1,2, F.W. Wit1,2, P.H. Bisschop1, J. Schouten1,2, I.G. Stolte3, M. Prins3, M. van der Valk1, B.L. van Eck-Smit1, P. Lips4, P. Reiss1,2 on behalf of the AGEhIV cohort study group
1 Academic Medical Center 2 Amsterdam Institute for Global Health and Development 3 Public Health Service Amsterdam 4 VU University Medical Center, Amsterdam, the Netherlands
CONCLUSIONS
We confirm a higher prevalence of osteopenia/osteoporosis in older HIV-1-positive individuals with predominantly suppressed viremia on cART, than in uninfected persons of comparable age. After adjustment for BMI and smoking, being HIV-positive was no longer independently associated with lower BMD. Surprisingly, in MSM, regardless of HIV-status, the expected relationship between older age and lower BMD was not observed. In fact an opposite trend was seen which could not be explained by differences in measured behavioral or other characteristics. This may suggest the presence of an as yet unknown factor which has negatively impacted bone health amongst the younger MSM in our cohort.
Program Abstract
Reduced Bone Mineral Density (BMD) is Largely Explained by Lower Body Weight in HIV-positive Individuals and More Pronounced in Younger Men Having Sex with Men (MSM), Regardless of HIV-status
Objectives: Current understanding of the contribution of HIV and ART, most notably tenofovir (TDF), to bone loss, is hampered by the lack of comparable HIV-uninfected control group in many studies. We compared lumbar spine, total hip and femoral neck BMD by dual-energy X-ray absorptiometry (DXA) at study enrolment in HIV-positive and HIV-negative participants, ≥45 years, of the ongoing prospective AGEhIV cohort study.
Methods: Multivariable linear regression with multiple imputation for missing values was used to investigate associations with HIV-infection and ART, adjusting for traditional risk factors and DXA-software changes during the course of the study.
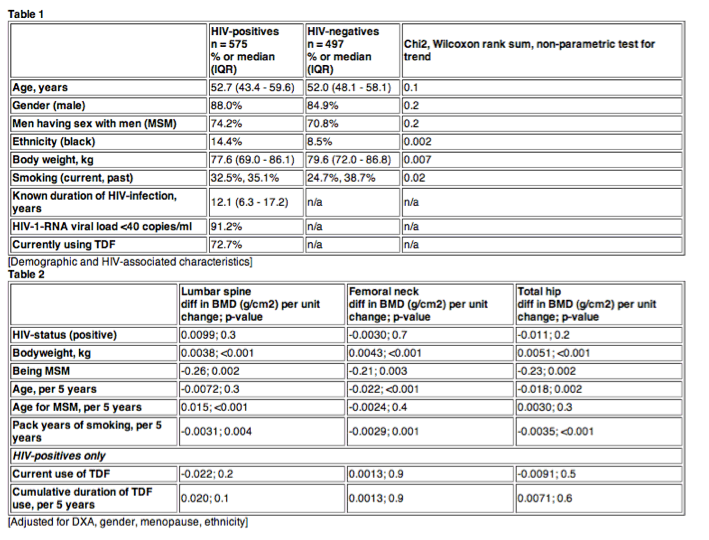
Results: Demographic and HIV-associated characteristics are shown in Table 1. Prevalence of osteoporosis or low BMD for age was higher in HIV-infected (14.4 vs. 8.1%, p=0.001). After adjustment for age, gender, menopausal status, ethnicity and DXA-software changes, HIV-infection remained significantly associated with lower femoral neck and total hip BMD (-0.020g/cm2, p=0.02 and -0.030g/cm2, p=0.001), but not with lumbar spine BMD. Upon further adjustment for bodyweight the association with HIV was no longer significant. A strong interaction was observed between age and being MSM: in non-MSM older age was associated with lower BMD, whereas in MSM this association was not present or even reversed, independent of HIV-status and traditional risk factors (Table 2). In those with HIV no significant association was found between cumulative or current use of TDF and BMD at any site.
Conclusion: We confirmed a high prevalence of osteoporosis and low BMD for age in HIV-positives, but also found a high prevalence in otherwise comparable uninfected persons.
Reduced BMD was not independently associated with HIV or TDF use, but could largely be explained by lower average bodyweight. Lower BMD associated with younger age in MSM needs further investigation and may be the result of unmeasured lifestyle and behavioral factors.
BACKGROUND
An increased prevalence of osteopenia and osteoporosis has been reported in HIV-1-infected individuals.1 The pathogenesis of HIV-associated low bone mineral density (BMD) is most likely multifactorial. Contributing factors may be lower average body weight in HIV-positive individuals2, antiretroviral therapy (ART) and persistent inflammation. First initiation of ART has been associated with a reduction in BMD. This is more pronounced for regimens containing tenofovir disoproxil fumarate (TDF)3 and it is unclear whether this effect persists4. A limitation of many studies conducted to date is the lack of a comparable HIV-uninfected control group.
1 Brown TT, Qaqish RB. AIDS. 20: 2165-74. 2006. 2 Bolland MJ, et al. J Clin Endocrinol Metab. 92: 4522-28. 2007. 3 McComsey GA, et al. JID. 203:1791-801. 2011. 4Bolland MJ, et al. J Clin Endocrinol Metab. 96: 2721-2731. 2011.
OBJECTIVES
Objectives were to assess BMD and the prevalence of osteopenia/ osteoporosis in comparable cohorts of HIV-1-positive and HIV-negative individuals, aged ≥45 years and to investigate whether HIV-1 and HIV-related characteristics are independently associated with BMD.
METHODS
581 HIV-1-positive individuals were enrolled at a single center HIV-outpatient clinic. 522 HIV-negative participants, comparable regarding age, gender and ethnicity were recruited from the municipal health service sexually transmitted disease clinic. Bone mineral density of the lumbar spine (L1-L4), total hip and femoral neck was measured by dual-energy X-ray absorptiometry. Additional potential determinants of BMD were assessed by physical exam, standardized questionnaire and different laboratory tests. Historical ART- and other relevant HIV-associated data were available through the ATHENA cohort.
Prevalence of osteopenia/osteoporosis in all three locations was based on T-score in post-menopausal women and men ≥50. In pre-menopausal women and men <50 osteoporosis was considered present if Z-score was ≤-2 (low BMD for age). Determinants of BMD were assessed by multivariable linear regression analysis, using multiple imputation for missing covariates.
HIV-related characteristics and BMD
Analyzing the HIV-1-positive cohort separately, independent associations were observed between a longer duration of a CD4 count below 200 and lower BMD in the total hip (-0.008 g/cm2/yr, p=0.02) and between HCV-RNA positivity and lower BMD in total hip (-0.084 g/cm2, p=0.004) and femoral neck (-0.075 g/cm2, p=0.006). No independent association was found between known duration of HIV-1 infection, current or past use of TDF or protease inhibitors and reduced BMD in any of the three locations.
|
| |
|
 |
 |
|
|