| |
Effect of immunodeficiency, HIV viral load, and antiretroviral therapy on the risk of individual malignancies (FHDH-ANRS CO4): a prospective cohort study Đ CD4 & viral load matter: restore or maintain the CD4 count above 500; early treatment initiation
|
| |
| |
Download the PDF here
"Current CD4 cell count was the most predictive risk factor for all malignancies apart from anal cancer......The risk of anal cancer increased with the time during which the CD4 count was less than 200 cells per μ L (1·3 per ye"ar, 1·2-1·5; p=0·0001), and viral load was greater than 100 000 copies per mL (1·2 per year, 1·1-1·4, p=0·005)."
Lancet Oncology Oct 8 2009
http://www.natap.org/2009/HIV/100809_01.htm
"Our results suggest that cART would be most benefitcial if it restores or maintains the CD4 count above 500 cells per μL, thereby indicating an earlier diagnosis of HIV infection and an earlier treatment initiation."
Access to cervical-cancer screening programmes should be regularly offered to all HIV-positive women, and cancer-specific screening programmes, such as for lung cancer and for anal cancer, need to be assessed in HIV-infected patients.
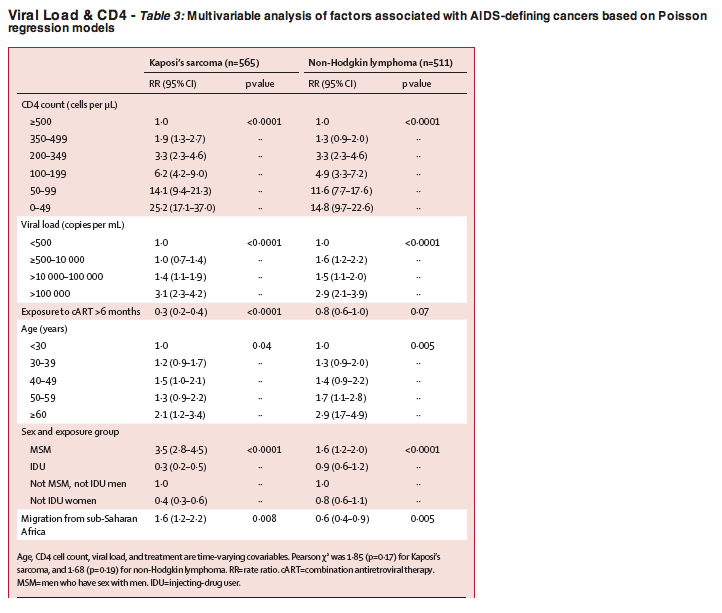
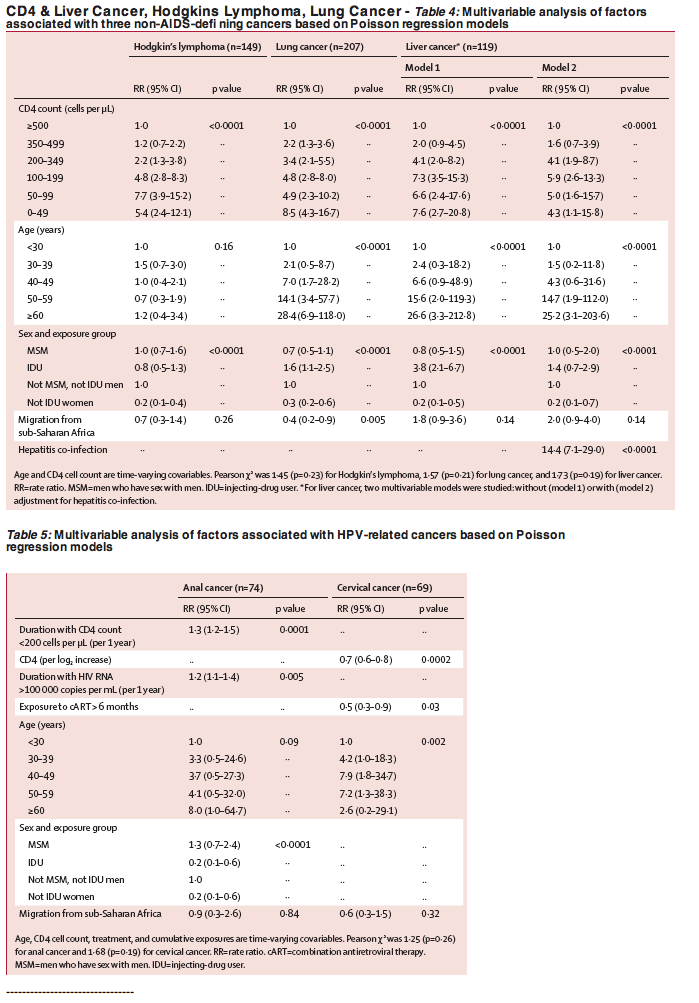
"Patients diagnosed with Kaposi's sarcoma and non-Hodgkin lymphoma had low nadir CD4 cell counts, and their median current CD4 count was less than 200 cells per μ L (table 2). Although more than half the patients diagnosed with Kaposi's sarcoma or non-Hodgkin lymphoma were receiving cART, their median viral load at diagnosis suggested frequent virological failure. At least two-thirds of patients diagnosed with one of the three non-AIDS-defining cancers were receiving cART, with a high frequency of virological efficacy, although the median CD4 count was less than 300 cells per μ L. Patients with anal cancer had a long history of HIV infection, a low nadir CD4 cell count, and a long cumulative period of immunodeficiency or high viral replication, or both; nearly all these patients were on antiretroviral therapy (table 2).The risk of anal cancer increased with the cumulative duration of CD4 counts less than 200 cells per μL and with the cumulative duration of viral load more than 5 log10 copies per mL (table 5)......In our study, HIV replication was associated with an increased risk of non-Hodgkin lymphoma, Kaposi's sarcoma, and anal cancer. Two previous studies have reported an increased risk of AIDS-related lymphoma associated with uncontrolled HIV RNA."
"We investigated the effect of immunodeficiency, viral replication, and cART on the incidence rates of both AIDS-defining and non-AIDS-defining cancers. Current CD4 cell count was the only factor predictive of Hodgkin's lymphoma, lung cancer, and liver cancer, whereas current CD4 cell count, current viral load, and absence of cART therapy were risk factors for Kaposi's sarcoma and non-Hodgkin lymphoma. Current CD4 cell count and absence of cART were both associated with cervical cancer. Finally, the risk of anal cancer increased with the time during which the CD4 count was less than 200 cells per μ L and viral load greater than 5 log10 copies per mL."
"At least two-thirds of patients diagnosed with one of the three non-AIDS-defining cancers were receiving cART, with a high frequency of virological efficacy, although the median CD4 count was less than 300 cells per μ L. Patients with anal cancer had a long history of HIV infection, a low nadir CD4 cell count, and a long cumulative period of immunodeficiency or high viral replication, or both; nearly all these patients were on antiretroviral therapy (table 2)."
"The risk of both Kaposi's sarcoma and non-Hodgkin lymphoma increased as the CD4 cell count fell and viral replication rose
"The risk of the three non-AIDS-defining cancers increased with decreasing CD4 cell counts (table 4). The risk of Hodgkin's lymphoma increased for CD4 count less than 350 cells per μ L and peaked at 50-99 cells per μ L. The risk of lung cancer was doubled by CD4 counts in the range 350-499 cells per μ L, and continued to increase thereafter as the CD4 cell count fell. The risk of liver cancer was raised at CD4 count less than 500 cells per μ L, and then reached a plateau at less than 200 cells per μ L (table 4). The risk of anal cancer increased with the cumulative duration of CD4 counts less than 200 cells per μ L and with the cumulative duration of viral load more than 5 log10 copies per mL (table 5). A higher CD4 cell count was associated with lower risk of cervical cancer, whereas patients receiving cART were half as likely to develop this cancer"
--------------------------------
Incidence and Timing of Cancer in HIV-Infected Individuals Following Initiation of Combination Antiretroviral Therapy......CD4 count at ART initiation was also an independent predictor of cancer
Clinical Infectious Diseases Advance Access published June 4, 2013
Elizabeth L. Yanik1, Sonia Napravnik1,2, Stephen R. Cole1, Chad J. Achenbach3, Satish Gopal2,
Andrew Olshan1, Dirk P. Dittmer4, Mari M. Kitahata5, Michael J. Mugavero6, Michael Saag6,
Richard D. Moore7, Kenneth Mayer8, W. Christopher Mathews9, Peter W. Hunt10, Benigno
Rodriguez11, Joseph J. Eron2
1Department of Epidemiology, University of North Carolina, Chapel Hill, NC; 2Department of
Medicine, University of North Carolina, Chapel Hill, NC; 3Department of Medicine, Northwestern
University, Chicago, IL; 4Department of Microbiology and Immunology, University of North
Carolina, Chapel Hill, NC; 5Department of Medicine, University of Washington, Seattle, WA;
6Department of Medicine, University of Alabama, Birmingham, AL; 7Department of Medicine,
Johns Hopkins University, Baltimore, MD; 8Fenway Community Health Center, Boston, MA;
9Department of Medicine, University of California, San Diego, CA; 10 Department of Medicine,
University of California, San Francisco, CA 11Department of Medicine, Case Western Reserve
University, Cleveland, OH
Abstract
Background. Cancer is an important cause of morbidity and mortality in individuals infected with human immunodeficiency virus (HIV), but patterns of cancer incidence after combination antiretroviral therapy (ART) initiation remain poorly characterized.
Methods. We evaluated the incidence and timing of cancer diagnoses among patients initiating ART between 1996 and 2011 in a collaboration of 8 US clinical HIV cohorts. Poisson regression was used to estimate incidence rates. Cox regression was used to identify demographic and clinical characteristics associated with cancer incidence after ART initiation.
Results. At initiation of first combination ART among 11 485 patients, median year was 2004 (interquartile range [IQR], 2000-2007) and median CD4 count was 202 cells/mm3 (IQR, 61-338). Incidence rates for Kaposi sarcoma (KS) and lymphomas were highest in the first 6 months after ART initiation (P < .001) and plateaued thereafter, while incidence rates for all other cancers combined increased from 416 to 615 cases per 100 000 person-years from 1 to 10 years after ART initiation (average 7% increase per year; 95% confidence interval, 2%-13%).
Lower CD4 count at ART initiation was associated with greater risk of KS, lymphoma, and human papillomavirus-related cancer. Calendar year of ART initiation was not associated with cancer incidence.
Conclusions. KS and lymphoma rates were highest immediately following ART initiation, particularly among patients with low CD4 cell counts, whereas other cancers increased with time on ART, likely reflecting increased cancer risk with aging. Our results underscore recommendations for earlier HIV diagnosis followed by prompt ART initiation along with ongoing aggressive cancer screening and prevention efforts throughout the course of HIV care.
Given the many changes that can occur after ART initiation, including immune reconstitution, HIV replication, aging, and ongoing exposure to carcinogens, cancer incidence over time following ART initiation is expected to be dynamic. Additionally, improvements in access to HIV testing and linkage to care as well as changes in the timing of ART initiation may impact the timing and incidence of cancer diagnoses in treated patients. In a large, diverse U.S. cohort of HIV-infected patients in care, the Centers for AIDS Research (CFAR) Network of Integrated Clinical Systems (CNICS), we evaluated trends in cancer incidence rates over time after ART initiation to inform cancer screening and prevention efforts for the HIV population in the ART era. We further identified patient characteristics associated with these trends that may provide insights into the etiology of cancers occurring in HIV-infected populations.
The most common ADC was KS with an IR of 304 per 100,000 person-years (95% CI: 258-358), while the most common NADC was anal cancer with an IR of 69 per 100,000 person-years (95% CI: 49-98). Among women, the most common NADC was breast cancer (IR: 128 per 100,000 person-years; 95%CI: 75-221).
The incidence of all non-KS, non-lymphoma cancers combined increased by 7% each year from ART initiation (95% CI: 2%-13%; p=0.009), from 416 to 615 cases per 100,000 person-years in years 1 and 10 post-ART initiation respectively.
Low CD4 count was also associated with high incidence of lymphomas and HPV-related cancers, but for these cancers, associations with CD4 count were consistent across time (both P for interaction with time >0.20) (Figure 2).
Discussion
This study of 11,485 patients from a multi-site U.S. clinical cohort of HIV-infected patients revealed distinct patterns of cancer incidence following ART initiation. This likely reflects varying etiologic contributions of aging, immunosuppression, and prior antiretroviral exposure, to the occurrence of specific cancer types. By contrast, cancer incidence did not appear to change over calendar time among ART initiators suggesting that the incremental improvements in ART regimens during the modern ART era have not had dramatic effects on cancer incidence.
| |
| |
| |
|
|
|