 |
 |
 |
| |
Comorbidity prevalence and its influence on non-ARV comedication burden among HIV positive patients
|
| |
| |
Reported by Jules Levin
Infectious Diseases Society of America, IDWeek 2013, Oct 2 - 6, 2013, San Francisco, CA
Nana Koram1, Vani Vannappagari1,2, Tim Sampson1, Catherine Panozzo2,3 1GlaxoSmithKline, Research Triangle Park, NC; 2Gillings School of Global Public Health, University of North Carolina-Chapel Hill, NC; 3Global PharmacoVigilance, Sanofi Pasteur, Swiftwater, PA
from Jules: in the last email I sent which reported from an oral at IDSA from a VA study they found increased mortality associated with taking 6 or more meds for comorbidities with those taking 5 or more having a 30% higher risk for mortality. THIS STUDY found HIV+ vs IV-negs had higher proportions of comorbidities in both age groups - >50 & 18-49, all of this suggests mortality will accelerate more in HIV+ vs HIV-negs as HIV+ age past 60 years old, and the demand for services will be greater for HIV+, both medical & non-medical
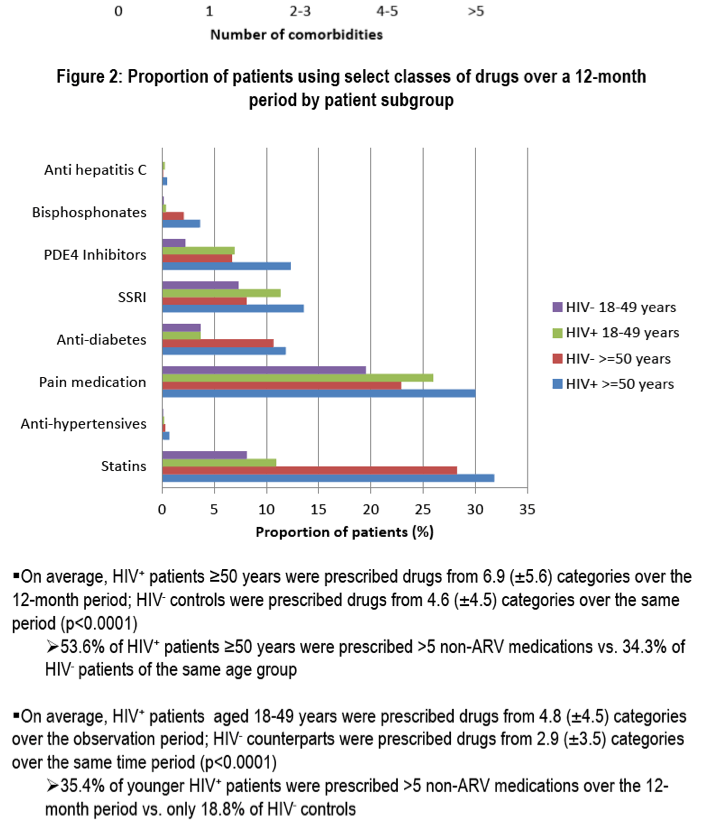
On average, HIV+ patients ≥50 years were prescribed drugs from 6.9 (±5.6) categories over the 12-month period; HIV- controls were prescribed drugs from 4.6 (±4.5) categories over the same period (p<0.0001) 53.6% of HIV+ patients ≥50 years were prescribed >5 non-ARV medications vs. 34.3% of HIV- patients of the same age group
On average, HIV+ patients aged 18-49 years were prescribed drugs from 4.8 (±4.5) categories over the observation period; HIV- counterparts were prescribed drugs from 2.9 (±3.5) categories over the same time period (p<0.0001) 35.4% of younger HIV+ patients were prescribed >5 non-ARV medications over the 12-month period vs. only 18.8% of HIV- controls

ABSTRACT
Background: Accelerated aging associated with HIV and higher comorbidity prevalence have increased non-antiretroviral (ARV) comedication burden for HIV positive (HIV+) people.
Method: We compared comorbidity prevalence and non-ARV drug burden, over a year, among age and gender matched HIV+ and negative (HIV-) patients 18-49 and ≥50 years using a comprehensive, de-identified US healthcare claims database (Clinformatics™ DataMart Multiplan (IMPACT), a product of OptumInsight Life Sciences, Inc.).
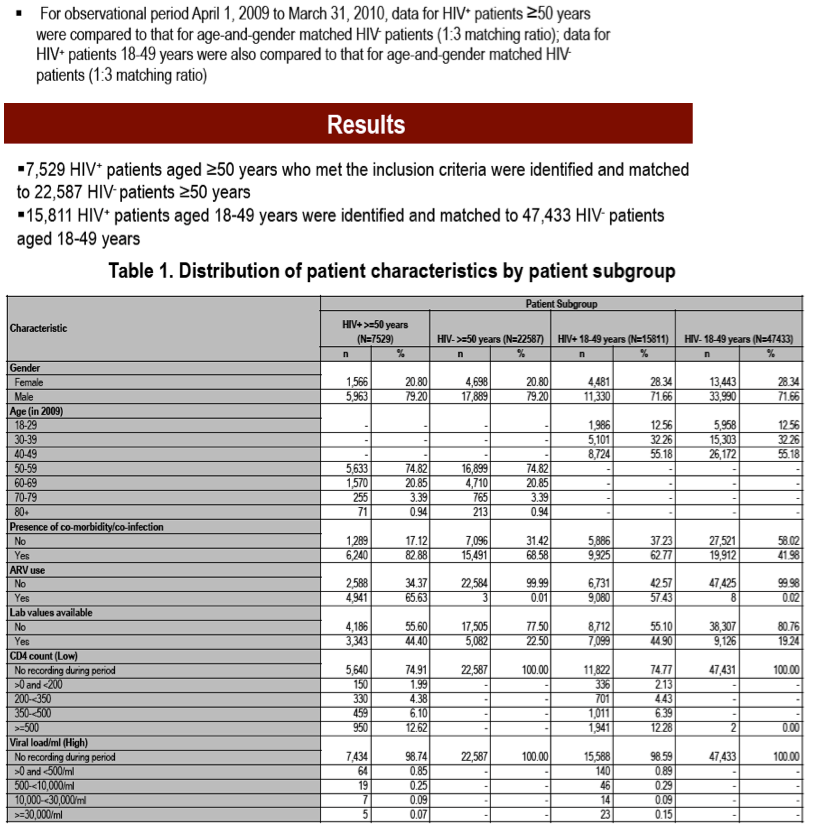
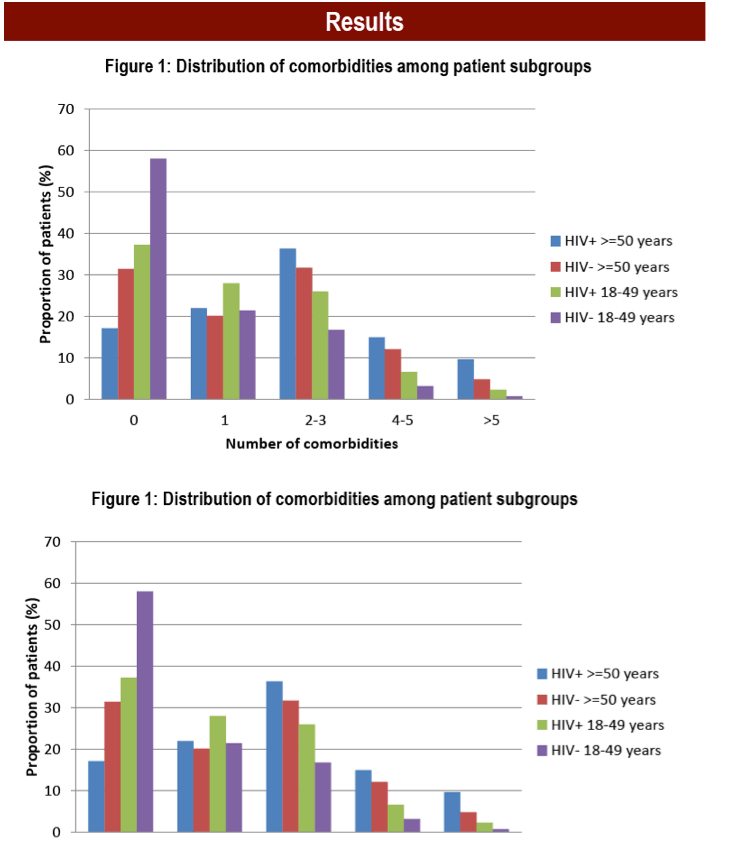
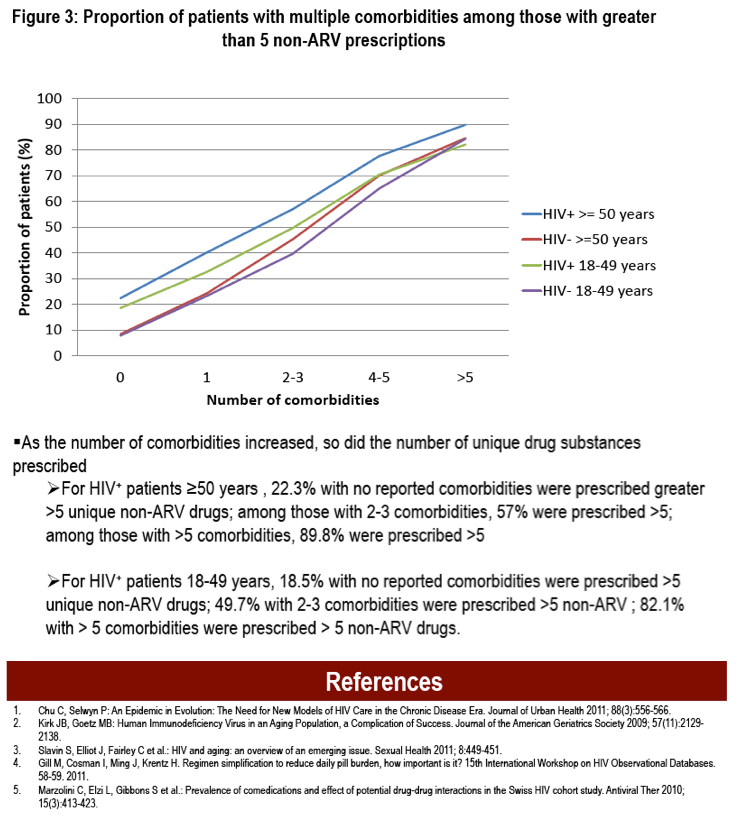
Results: We identified 15811 HIV+ patients aged 18-49 and 47433 matched controls; 7529 HIV+ patients ≥ aged 50 and 22587 matched controls. For HIV+ patients aged 18-49, 72% were male; 57% received antiretroviral therapy (ART); 63% had ≥1 comorbidities (controls: 42%), 28% had 1 only, 26% had 2-3, 7% had 4-5, 2% had >5. For HIV+ patients aged ≥50, 79% were male; 66% received ART; 83% had ≥1 comorbidities (controls: 69%), 22% had 1 only, 36% had 2-3, 15% had 4-5, 10% had >5. For patients aged 18-49, cases were prescribed a mean of 4.8 (±4.5) drug classes over a year [controls: 2.9 (±3.5); p<0.0001]. Cases were prescribed a median of 4 [interquartile range (IQR): 1-7] non-ARV unique drugs [controls: 2 (IQR: 0-4)]; 35% of cases were prescribed >5 unique drugs (controls: 19%). For those aged ≥50, cases were prescribed a mean of 6.9 (±5.6) drug classes [controls: 4.6 (±4.5); p<0.0001]. Cases were prescribed a median of 6 (IQR: 3-10) drugs [controls: 3 (IQR: 1-7)]; 54% of cases were prescribed >5 drugs (controls: 34%). For HIV+ patients aged ≥50, 40% of those with 1 comorbidity were prescribed >5 non-ARV drugs. For those with 2-3 comorbidities, 57% were prescribed >5 drugs; for those with 4-5, 78% were prescribed >5 drugs; for those with >5, 90% were prescribed >5 drugs. For HIV+ patients aged 18-49, 33% with 1 comorbidity were prescribed >5 non-ARV drugs; 50% of those with 2-3 comorbidities were prescribed >5; 70% of those with 4-5 comorbidities were prescribed >5; 82% with >5 comorbidities were prescribed >5.
Conclusions: Compared to controls, HIV+ patients were more likely to have ≥1 comorbidities, were prescribed significantly higher numbers of non-ARV drugs and drug classes, and were more likely to be prescribed >5 non-ARV drugs. Number of comorbidities was linearly associated with number of unique drugs prescribed.

|
| |
|
 |
 |
|
|