 |
 |
 |
| |
Polypharmacy in HIV:
"Differences in calculated adherence rates of ART and non-ART medications among HIV positive veterans"
|
| |
| |
Patients who are otherwise adherent to their ART are less adherent with their non-ART medications/PDC of non-ART medications was lower than PDC of ART in a HIV clinic in VA by 8.8%....... HIV patients are growing older and are prone to develop other chronic illnesses such as diabetes and cardiovascular disease, which like HIV, require high levels of medication adherence to reach desired goals for therapy...... 2 studies at IDSA (Koram & Edelman/VA) found 60% of older patients, in mid-50s or older, were taking 5 or more medications (defined as polypharmacy, in the VA Study: After antiretrovirals, the next 5 most common medication classes were antilipemic agents, antidepressants, ACE inhibitors, beta blockers, and gastric medications, interestingly the VA study found: Those on > 5 medications had a 30% higher risk of mortality. The Koram Study reported: On average, HIV+ patients ≥50 years were prescribed drugs from 6.9 (±5.6) categories over the 12-month period.....35.4% of younger HIV+ patients were prescribed >5 non-ARV medications over the 12-month period.....HIV- controls >50 were prescribed drugs from 4.6 (±4.5) categories over the same period.....<50 only 18.8% of HIV- controls
from Jules: older patients, both HIV+ & HIV-, but also for younger HIV-neg & vets, taking polypharmacy, 50% taking 5 non-ART meds or more plus ART meds, this needs to be considered when prescribing the new HCV therapies. Although very soon we will have HCV regimens that are IFN-free and with few daily pills taken & for only 12 or 24 weeks, for some patients adding the new HCV regimens will be challenging, plus if the HIV+ individuals have to switch off their ART regimen due to drug interactions with the HAART regimen they are on to another HAART regimen for the 12 week period, these will be challenging for some patients.

Reported by Jules Levin
IDSA 2013 Oct 2-6 San Francisco, CA
Fumihiro Kodama, MD1,2, Marion Skalweit, MD, PhD1,2, Christopher Burant, PhD1,2, Amy Hirsch, PharmD1,2 1Louis Stokes Cleveland Department of Veterans Affairs Medical Center (LSCDVAMC), Cleveland, OH, 2Case Western Reserve University, Cleveland, OH
ABSTRACT
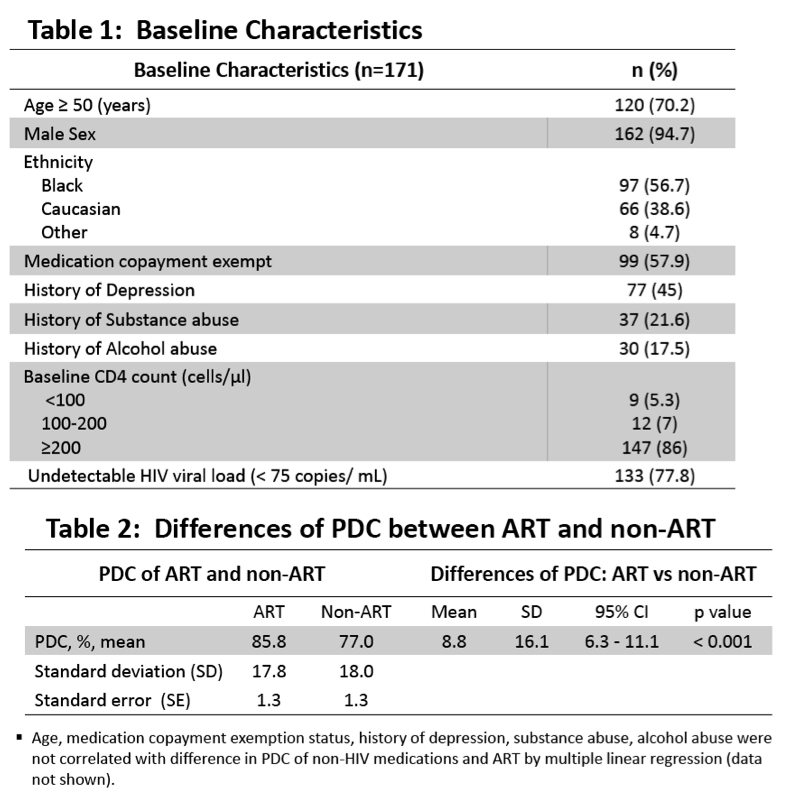
Background: As cardiovascular disease is increasingly recognized as an important cause of morbidity and mortality among HIV-infected patents, management of non-HIV chronic diseases including hypertension, diabetes mellitus, and dyslipidemia, is also becoming more important among aging HIV-infected population. Although adherence to ART has been studied extensively, adherence to non-ART medications has not. We compared adherence to antiretroviral therapy (ART) and non-ART medications among HIV-infected patients in a VA (Veterans Affairs) HIV clinic.
Methods: A retrospective chart review was conducted on a cohort of HIV-infected patients followed in the HIV clinic at LSCDVAMC, prescribed both ART and non-ART medications for more than 365 days continuously by ID clinic provider between 1/1/2011 and 12/31/2012. Measures of medication adherence, calculated by proportion of days covered (PDC) based on prescription date and days of medication supply, were compared between ART and non-ART medications.
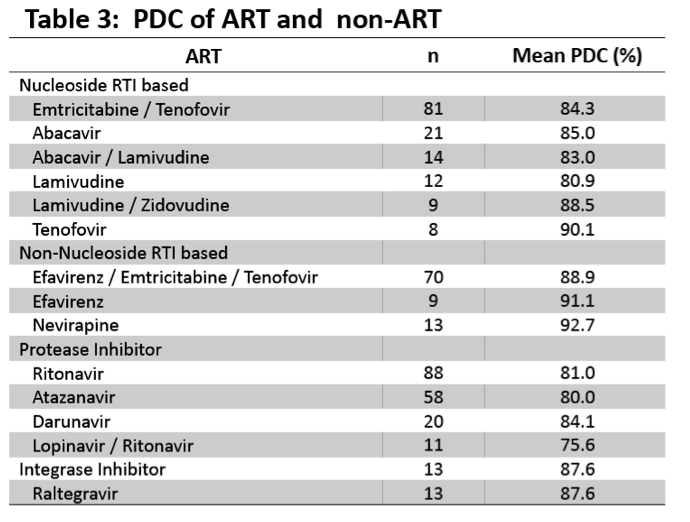
Results: Total 458 ART and 667 non-ART medications were included from 171 patients (162 men and 9 women, mean age 54.6). A paired-samples t-test comparing means of ART and non-ART medications of each patient showed a significant difference in PDC of ART (mean 85.8, SD 17.8) and PDC of non-ART medications (mean 77.0, SD 18.0), conditions; t (170), p < 0.001. Mean difference of 8.8% in PDC suggests non-ART medications covered 32.1 days less than ART in 365-days observation period.
Age, medication copayment exemption status, history of depression, substance abuse, alcohol abuse were not correlated with difference in PDC of non-HIV medications and ART by multiple linear regression.
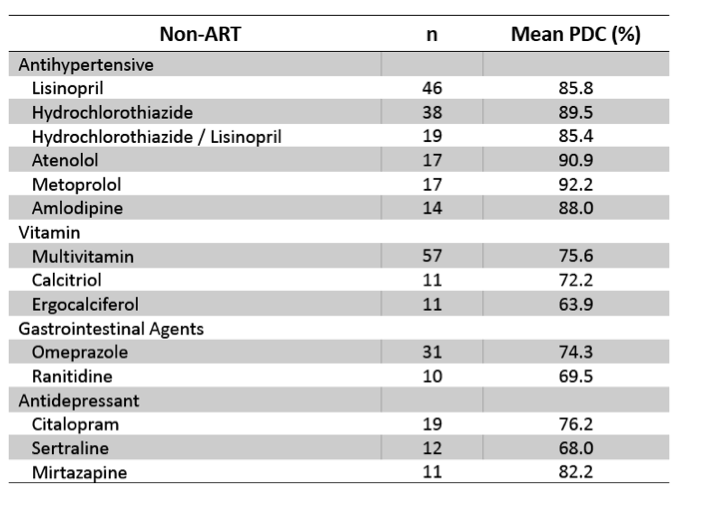
Mean PDC of major non-ART medications are; multivitamin 75.6% (n=57), lisinopril 85.8% (n=46), hydrochlorothiazide 89.5% (n=38), omeprazole 74.3% (n=31), pravastatin 80.6% (n=23), citalopram 76.2% (n=19), and hydrochlorothiazide/lisinopril 85.4% (n=19).
Conclusions: PDC of non-ART medications was lower than PDC of ART in a HIV clinic in VA by 8.8%. Patients who are otherwise adherent to their ART are less adherent with their non-ART medications. Interventions to improve medication adherence should also include non-ART medications in addition to ART.


|
| |
|
 |
 |
|
|