| |
Cure setbacks force HIV researchers to reset sights
|
| |
| |
Download the PDF here
"Measuring the reservoir in blood isn't enough, however, because virus can often lurk in harder to access tissues like the lymph nodes, gut, and spinal fluid. (Timothy Ray Brown had each of these assessed, and the Boston patients and the Australian transfusion recipient had gut biopsies, but none of these tissues was tested in the Mississippi child.) It's possible that remote sites offer reservoirs safe harbor from ARVs or immune attack. "

Science 1 August 2014:
Aids Conference
Cure setbacks force HIV researchers to reset sights
Jon Cohen
http://www.sciencemag.org/content/345/6196/495.full?sid=b8dc59da-994e-4267-b50f-cbfefdd09c4d
A year ago it likely would have been heralded as a stunning advance. An Australian man who became infected with HIV by a blood transfusion in 1981 may have naturally "cleared" the virus, researchers reported here last week at the 20th International AIDS Conference. If so, he would be just the second person to be cured of an HIV infection.
But recent setbacks have made other researchers extra cautious. Over the past year, three HIV-infected people who received widespread attention for apparently clearing their infections had the virus come roaring back-in one case more than 2 years after it seemed to have disappeared. And so, at the end of the presentation by immunologist John Zaunders of the Sydney, Australia-based Kirby Institute for Infection and Immunity in Society, Daniel Kuritzkes of Brigham and Women's Hospital in Boston jumped to the microphone to question why Zaunders spoke of "possible clearance" of the virus. "It's certainly an intriguing case," Kuritzkes said. But he cautioned Zaunders and everyone else at the session that a major shift in thinking was under way. "No question that this patient is in sustained remission, but you can't ever discern that there's not virus there," Kuritzkes said.
At the weeklong conference here, where the 13,600 attendees collectively mourned the six delegates killed in the Malaysia Airlines crash in Ukraine, cureresearch still dominated the scientific agenda. But the recent failures-a child in Mississippi and two bone marrow transplantation patients, whom Kuritzkes helped analyze-highlighted the huge challenges that remain and triggered a heightened sensitivity to words like "clearance" and "cure." Kuritzkes and several others urged their colleagues to take a page from the cancer field, which typically reserves the word "cure" for patients who have remained in remission for at least 5 years.
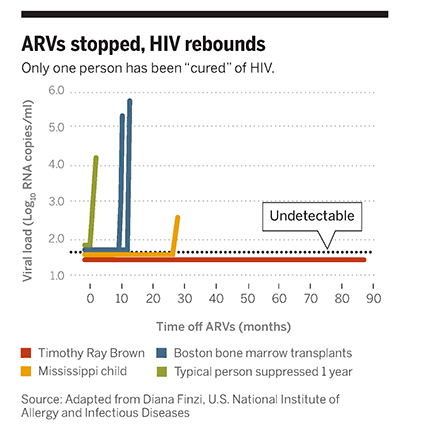
The only person researchers widely agree has been cured is Timothy Ray Brown, known as the "Berlin patient," who stopped taking antiretroviral (ARV) drugs in February 2007 (Science, 13 May 2011, p. 784) and has remained virus-free until today. But Brown was unusual: He developed leukemia and twice had his own immune system destroyed so that he could receive two bone marrow transplants, both from a rare donor who had cells resistant to HIV.
Ordinarily, cocktails of potent ARVs reduce the virus to such low levels that it becomes undetectable in the blood on standard tests. But it lurks in small reservoirs of cells that harbor latent HIV DNA in their chromosomes. When these "fully suppressed" people stop taking the drugs, the virus usually returns to high levels in a few weeks. Researchers had hoped that the Mississippi child, infected by her mother in utero or at birth and started on aggressive treatment before she was 2 days old, had a reservoir so small her body could clear it while on ARVs. But the virus returned 27 months after she stopped taking her drugs. Similarly, investigators suspected that when doctors prepared the two Boston patients for their bone marrow transplants by destroying their existing immune systems, they eliminated so many infected cells that ARVs could clear the rest. Within 8 months of stopping ARVs, however, HIV came back in both men.
"We've learned now that the virus can be there but under control for a very long time," said Sharon Lewin, an HIV cure researcher at the Burnet Institute here and co-chair of the conference. "But prolonged remission is only the short-term goal. I do think a cure has to be the aspirational goal."
To outright cure an infection, many researchers have promoted a "shock and kill" strategy that aims to flush the virus out of hiding by forcing the sleeping HIVDNA inside of chromosomes to wake up and produce new viruses. Theoretically, that would lead to the destruction of the infected cells, and ARVs would keep the virus from infecting new ones. At the meeting, Ole Schmeltz Sogaard of Aarhus University in Denmark reported that a cancer drug on the market, romidepsin, could lead to such robust bursts of virus in people suppressed by ARVs for years that HIV became detectable on standard blood tests. The study involved just six participants and did not claim to reduce the reservoirs in any of them. But it's "actually a big step," Lewin said. Sogaard and co-workers now plan to repeat the clinical experiment with both the drug and an HIV vaccine that, they hope, will boost the immune response against the virus and help deplete reservoirs.
A major hurdle facing shock and kill: Available tests can't reliably determine whether an intervention has actually reduced the reservoir's size. "Right now, the assays we have are pretty expensive, they require a lot of blood, and we're not exactly sure what they measure," said immunologist Nicolas Chomont of the Vaccine & Gene Therapy Institute of Florida in Port St. Lucie. Chomont presented a novel assay his team has developed that is relatively cheap, requires only 10 milliliters of blood, and, he contends, more meaningfully quantifies small amounts of virus than anything available. He designed it to overcome problems with the two most commonly used tests to measure reservoir size. One, which cultures blood from an infected person with uninfected cells and measures production of new viruses, vastly underestimates the reservoir. The second one grossly over estimates the size because it uses the polymerase chain reaction (PCR) to detect HIV genetic material-including hordes of mutated viral DNA that produces "dead-end" viruses, which are not viable and thus of little concern.
Chomont's new assay, dubbed TILDA, also relies on PCR but selects critical HIV genetic signatures needed for replication that often are missing in the DNA that codes for dead-end viruses.
Steven Deeks, an HIV cure researcher at the University of California, San Francisco, says if TILDA proves its worth in rigorous studies, it could spur investment in the field from wary pharmaceutical companies. "Industry is not engaged because there's no validated way to measure the reservoir," Deeks said. "How are we going to define cure, and how are the regulators going to define cure?"
Measuring the reservoir in blood isn't enough, however, because virus can often lurk in harder to access tissues like the lymph nodes, gut, and spinal fluid. (Timothy Ray Brown had each of these assessed, and the Boston patients and the Australian transfusion recipient had gut biopsies, but none of these tissues was tested in the Mississippi child.) It's possible that remote sites offer reservoirs safe harbor from ARVs or immune attack. With that in mind, virologist Brandon Keele of the National Cancer Institute in Frederick, Maryland, described a new strategy to track reservoirs in different parts of the body. Working in a monkey model, Keele and his co-workers engineered thousands of nearly identical versions of SIV, the monkey AIDS virus, which they can distinguish by means of small genetic differences that serve as unique barcodes.
The researchers have injected swarms of these SIVs into monkeys, which they plan to treat with ARVs to reduce the viruses to undetectable levels. After several months, they'll stop treatment and perform blood tests, biopsies, and, ultimately, necropsies on the animals to see if the barcodes can reveal the source of the rebounding virus.
Just where the virus hid during the Mississippi child's 27 months of remission is one of the case's baffling mysteries. In the wake of the setback, the National Institute of Allergy and Infectious Diseases (NIAID) is redesigning a study of HIV-infected newborns that would use a similarly aggressive ARV regimen shortly after birth and then, at some point, take them off drugs and see whether the virus rebounds. Trial designers have heatedly debated whether to add tissue sampling to the protocol, but sensitivities about subjecting children to the procedures have nixed it for now. "We've got to rethink that," says NIAID Director Anthony Fauci, who is not on the trial design team. The field needs answers, not more anecdotes of cures, he says. "I'm maintaining a deep degree of humility.
Jon Cohen is a writer in Melbourne, Australia.
|
|
| |
| |
|
|
|