 |
 |
 |
| |
Clinical Characteristics and Quality of HIV Care for Women in the United States:
Data from the Medical Monitoring Project, 2009
|
| |
| |
Reported by Jules Levin
4th International Workshop on HIV & Women, January 13-14, 2014, Washington DC
Study authors: William R. Short, Linda Beer, Ann Do, Emma Frazier, Janet Blair, Heather Bradley, Jacek Skarbinski
From Jules: in this analysis of HIV care for 1,100 HIV+ women: 38% are 40-40 yo, 31% >50 yo; 61% black; 16.9% Hispanic; 33% less than high school education; 8.6% homeless; 77% income 0-19,999$; 55% on SSI, SSDI, or other public assistance; 65% had AIDS or nadir CD4 <200; sexual behavior: 54% - any oral, vaginal or anal sex; unprotected vaginal or anal sex: 22%; unprotected vaginal or anal sex with a negative or unknown status partner 14%.
AND:
Gonorrhea screening among sexually active: 28%
Chlamydia screening among sexually active: 30%
Syphilis screening among sexually active: 49%
Cervical cancer screening: 77% (meaning 23% did not get it)
Received influenza immunization: 76% (meaning 24% did not get it)
PCP prophylaxis among those with CD4 cell count <200 cells/μl: 81% (meaning 19% did not get it)
Viral suppression: 66%
Receipt of HIV prevention counseling by a health care provider: 50%
HIV prevention counseling by a health care provider among sexually active by age:
- 18-29 years 67%
- 30-39 yrs: 60%
- 40-49 yrs: 47%
- >50: 52%
total: 55%

William R. Short, Linda Beer, Ann Do, Emma Frazier, Janet Blair, Heather Bradley, Jacek Skarbinski

ABSTRACT
Background: Women comprise an estimated 25% of persons living with HIV infection in the United States, but there are no recent nationally representative estimates of the clinical characteristics of and quality of care received by these women. Establishing these estimates provides a national benchmark in
order to characterize patterns of HIV care and monitor changes in care over time among HIV- infected women.
Material &Methods: The Medical Monitoring Project (MMP) is a nationally representative cross-sectional survey of HIV-infected adults ≥ 18 years of age receiving outpatient medical care in the United States and Puerto Rico. Using data collected via in-person interviews and medical record abstractions among women receiving HIV care in 2009, we assessed their clinical characteristics and quality of care in the year prior to interview.
Results: We obtained matched interview and medical record data for 1,139 HIV-infected women, who were estimated to represent 114,527 HIV-infected women who received outpatient medical care in 2009 in the United States and Puerto Rico.
In all, 83% of women reported taking antiretroviral therapy (ART) and only 66% had a recent viral load test result that was undetectable or <200 copies/ml.
A majority of women received at least two CD4 T-cell tests (87%), influenza immunization (76%), and were prescribed PCP prophylaxis (82%) when their CD4 T-cell count fell below 200 cells/ul. Most women reported receiving cervical cancer screening (77%).
However, too few sexually active HIV-infected women received recommended screening for syphilis (49%), gonorrhea (28%), or Chlamydia (30%).
Only 50% of HIV-infected women reported receiving counseling from their healthcare provider about ways to prevent transmission of HIV and sexually transmitted infections (STIs). Among sexually active women, 67% of those aged 18-29 years compared to 53% of those aged >50 years reported receiving HIV and STI risk-reduction counseling.
Discussion: Because of differences between women and men in physiological and socioeconomic factors, treating women with HIV requires recognition by providers of these differences, as well as key standards of care that are unique to women. Despite the fact that the majority of women reported taking ART, only two-thirds were virally suppressed. Although most HIV-infected women in care received adequate CD4 T-cell monitoring, influenza immunization, and PCP prophylaxis, many women did not receive guideline-recommended STI screening and counseling. Too few sexually active HIV-infected women received HIV and STI risk-reduction counseling, especially older women. Efforts to improve adherence to clinical guidelines may help improve treatment of HIV-infected women in the United States.
BACKGROUND &
OBJECTIVES
Women compromise an estimated 25% of persons living with HIV in the United States
Numerous clinical guidelines are available to assist in providing quality care
There are no recent nationally representative estimates of the clinical characteristics of and quality of care received by HIV infected women
Study objective
- Provide a national benchmark to characterize patterns of care among HIV infected women
METHODS
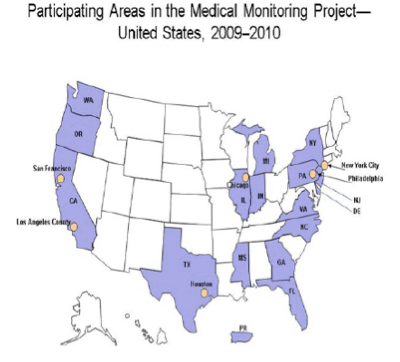
The Medical Monitoring Project (MMP) is a national supplemental surveillance system that monitors clinical outcomes and behaviors among U.S. HIV-infected persons in care through interview and medical record abstraction in 23 health department jurisdictions
Uses 3-stage clustered sampling design to produce nationally representative estimates
Of 603 sampled facilities, 461 participated in MMP (facility response rate 76%), and of 9,338 sampled persons (patient response rate 51%) completed an interview and had their medical records abstracted
This analysis includes data on 1,139 female participants who are estimated to represent 114,527 HIV-infected women in care in the United States from January to April 2009
2009 data were used to estimate percentage of patients who received recommended care based on National and Multiagency HIV Care Quality Measures (Horberg et al. CID 2010)
All analyses accounted for clustering, unequal selection probabilities, and non-response
RESULTS
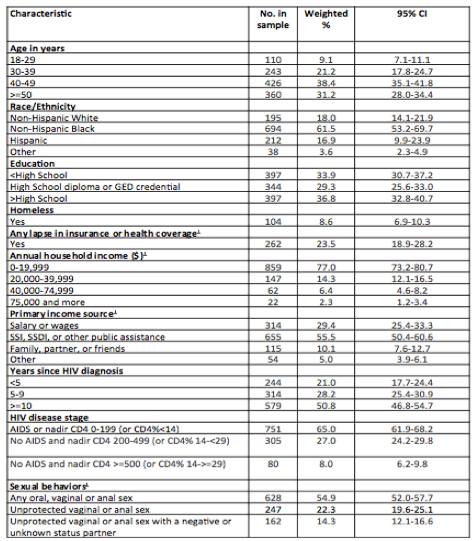
1 Past 12 months
CI=confidence interval; HIV=human immunodeficiency virus; GED=general
educational development; SSDI=social security disability insurance; SSI=Social Security Supplemental Income.
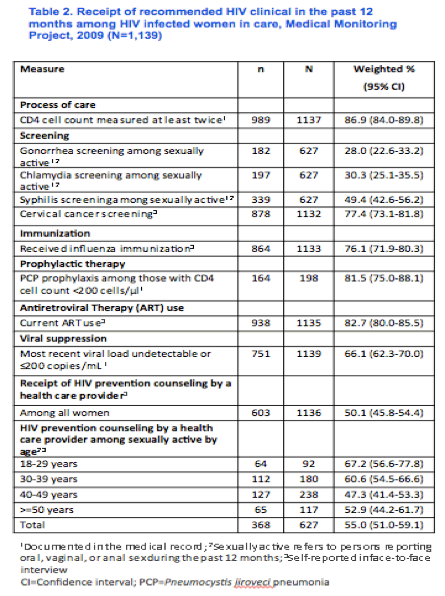
DISCUSSION
Although 82.7% were taking ART, only 66.1% had a suppressed viral load
Quality of HIV care delivered varied by intervention
- High: 86.9% adequate CD4 monitoring
- Low: 28.0% tested for gonorrhea
Most HIV-infected women in care received adequate CD4 T-cell monitoring, influenza immunization, and PCP prophylaxis,
Too few sexually active HIV-infected women received screening for STIs
Only 55 percent of sexually active women reported receiving counseling from their provider about preventing HIV and STD transmission, and this varied by age.
CONCLUSIONS
Although the quality of clinical care was high, only two out of three women were virally suppressed
Most women received recommended HIV-specific services (e.g., CD4 monitoring, PCP prophylaxis)
Most women received clinical services important to help people living with HIV remain healthy (e.g., influenza immunization, cervical cancer screening)
Many women did not receive guideline-recommended STI screening and counseling
Too few sexually active HIV-infected women received HIV and STI risk-reduction counseling, especially older women
Additional efforts are warranted to improve quality of HIV care in the United States for women, especially delivery of interventions aimed at reducing HIV transmission such as STD screening and provider risk reduction counseling
LIMITATIONS
Potential for non-response bias given moderate overall response rates
Potential for recall bias as some measures (influenza vaccination and cervical cancer screening) assessed using interview
Medical record abstraction conducted only at sampled facility and not all facilities where a participant might have received care
ACKNOWLEDGEMENTS
We would like to thank the MMP participants, the staff at participating MMP facilities, the staff at the 23 health jurisdictions, and the entire Clinical Outcomes Team at the Centers for Disease Control and Prevention

|
| |
|
 |
 |
|
|