| |
New Study - SVR Reduces Liver Mortality & Morbidity by 75% and CVD Hospitaliztion by 30%
|
| |
| |
Download the PDF here
"patients with SVR exhibited >75% reduced risk of liver mortality and SLM (severe liver morbidity), relative to patients without SVR......We report an association between SVR and a 32% risk reduction in non liver mortality.......A second result to emphasize is the association between SVR and a 30% reduction in the risk of hospitalization for CVD, this finding provides further evidence that HCV infection is a risk factor for cardiovascular impairment......SVR was associated with significant 7.5-year ARRs (absolute risk reduction) for liver mortality, all-cause mortality, SLM, and CVD......At 7.5 years, ARRs were between 6.3% and 10.2% for liver mortality, all-cause mortality, SLM, and CVD"
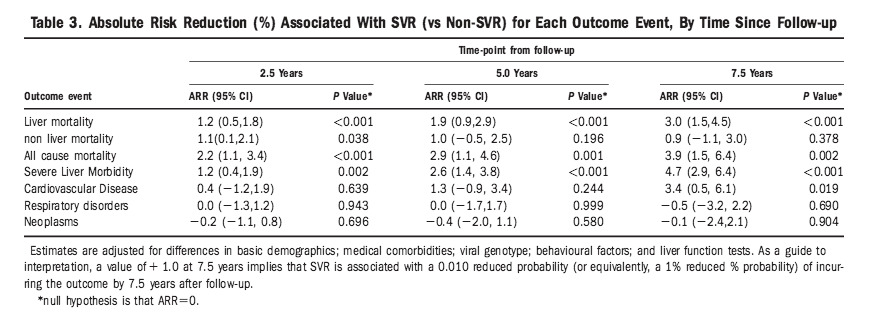
Toward a more complete understanding of the association between a hepatitis C sustained viral response and cause-specific outcomes
Hepatology Aug 2015
Hamish A. Innes,1,2 Scott A. McDonald,1,2 John F. Dillon,3 Sam Allen,4 Peter C. Hayes,5 David Goldberg,1,2 Peter R. Mills,6 Stephen T. Barclay,7 David Wilks,8 Heather Valerio,1,2 Ray Fox,9 Diptendu Bhattacharyya,10 Nicholas Kennedy,11 Judith Morris,12 Andrew Fraser,13 Adrian J. Stanley,7 Peter Bramley,14 and Sharon J. Hutchinson1,2
From the 1School of Health and Life Sciences, Glasgow Caledonian University, Glasgow, United Kingdom; 2Health Protection Scotland, Glasgow, United Kingdom;
3Ninewells Hospital and Medical School, Dundee, United Kingdom; 4University Hospital, Crosshouse, United Kingdom; 5Royal Infirmary Edinburgh, Edinburgh, United Kingdom; 6Gartnavel General Hospital, Glasgow, United Kingdom; 7Glasgow Royal Infirmary, Glasgow, United Kingdom; 8Western General Hospital, Edinburgh, United Kingdom; 9The Brownlee Center, Glasgow, United Kingdom; 10Kirkcaldy Hospital, Fife, United Kingdom; 11Monklands Hospital, Lanarkshire, United Kingdom; 12Southern General Hospital, Glasgow, United Kingdom; 13Aberdeen Royal Infirmary, Aberdeen, United Kingdom; 14Stirling Royal Infirmary, Stirling, United Kingdom
Abstract
Sustained viral response (SVR) is the optimal outcome of hepatitis C virus (HCV) therapy, yet more detailed data are required to confirm its clinical value. Individuals receiving treatment in 1996-2011 were identified using the Scottish HCV clinical database. We sourced data on 10 clinical events: liver, nonliver, and all-cause mortality; first hospitalisation for severe liver morbidity (SLM); cardiovascular disease (CVD); respiratory disorders; neoplasms; alcohol-intoxication; drug intoxication; and violence-related injury (note: the latter three events were selected a priori to gauge ongoing chaotic lifestyle behaviours). We determined the association between SVR attainment and each outcome event, in terms of the relative hazard reduction and absolute risk reduction (ARR). We tested for an interaction between SVR and liver disease severity (mild vs. nonmild), defining mild disease as an aspartate aminotransferase-to-platelet ratio index (APRI) <0.7. Our cohort comprised 3,385 patients (mean age: 41.6 years), followed-up for a median 5.3 years (interquartile range: 3.3-8.2). SVR was associated with a reduced risk of liver mortality (adjusted hazard ratio [AHR]: 0.24; P < 0.001), nonliver mortality (AHR, 0.68; P = 0.026), all-cause mortality (AHR, 0.49; P < 0.001), SLM (AHR, 0.21; P < 0.001), CVD (AHR, 0.70; P = 0.001), alcohol intoxication (AHR, 0.52; P = 0.003), and violence-related injury (AHR, 0.51; P = 0.002). After 7.5 years, SVR was associated with significant ARRs for liver mortality, all-cause mortality, SLM, and CVD (each 3.0%-4.7%). However, we detected a strong interaction, in that ARRs were considerably higher for individuals with nonmild disease than for individuals with mild disease. Conclusions: The conclusions are 3-fold: (1) Overall, SVR is associated with reduced hazard for a range of hepatic and nonhepatic events; (2) an association between SVR and behavioral events is consistent with SVR patients leading healthier lives; and (3) the short-term value of SVR is greatest for those with nonmild disease.
Chronic infection with the hepatitis C virus (HCV) can lead to fatal liver disease.[1] The virus can be permanently eradicated through a course of treatment, and the sustained viral response (SVR) is used as a near-term proxy for this outcome.[2] However, the primary goal of therapy is not to attain SVR per se, but to appreciably improve the patient's prognosis vis-ˆ-vis overt liver disease and putative extrahepatic sequelae.[2, 3] In this sense, SVR is a surrogate endpoint, not a clinical one.[4] Accordingly, the treatment case rests on this surrogate being of sufficient clinical value to the individual.
Observational studies thus far have found that SVR is independently associated with a reduced risk of: liver failure and liver mortality,[5] nonliver mortality,[6] all-cause mortality,[5, 7] cardiovascular disease (CVD),[8] type 2 diabetes,[9, 10] and renal disease.[8] This is encouraging, but we must continue to develop our understanding of these associations, not least to justify high treatment costs[11] and significant adverse effects with some regimens. Herein, we revisit a previous analysis,[12] this time with a larger, nation-wide post-treatment cohort attached to detailed cause-specific mortality and hospitalization data. Our broad objective was to describe the association between SVR and a diverse range of clinical events. In the course of doing so, we offer three advancements to previous work. First, we assess the absolute risk reduction (ARR) associated with SVR, recognizing that ARR gives the most clinically relevant picture vis-ˆ-vis the value of a medical intervention.[13, 14] Second, we examine whether SVR is associated with events that reflect chaotic lifestyle behaviors (in addition to events that reflect the biological sequelae of viral pathogenesis). Finally, we report the evidence for an interaction in the SVR effect according to mild versus nonmild liver fibrosis.
Patients and Methods
Treatment Cohort: Inclusion and Exclusion Criteria
The Scottish Hepatitis C Clinical Database consists of standalone Microsoft Access databases installed across the majority of Scottish HCV treatment sites (at present, installed in 16 of a possible 18 centers). These databases hold information on all aspects of HCV care and patient management, and on an annual basis, are amalgamated into a single aggregate data set. The inclusion criterion for this study was commencement of a course of antiviral therapy after January 1, 1996 (i.e., since the universal availability of HCV-RNA testing in Scotland) and a termination date preceding December 31, 2011. After applying appropriate exclusion criteria (see Supporting Fig. 1), the final cohort considered in our analyses comprised 3,385 treatment patients.
Linkage to Mortality and Hospitalization Data
Scotland holds a national database for (1) all general and acute inpatient/day case hospital admissions (SMR-01 database), (2) all mental health inpatient/day case admissions (SMR-04 database), and (3) all deaths.[11] We electronically linked patients in our HCV treatment cohort to extracts from these three databases (all three extracts were complete to December 31, 2013). This linkage involved a two-step process: First, patient identifiers held on the clinical database (forename initial, gender, surname soundex, date of birth, and post-code sector) were probabilistically matched to an individual on the Scottish Community Health Index (CHI) database. The CHI database allocates, to every individual registered with a general practitioner in Scotland, a unique number (the "CHI number").[15] Essentially, this CHI number functions as a "master index." Hence, in the second step, knowledge of each individual's CHI number enables the corresponding hospitalization and mortality records to be retrieved. This linkage was approved by the National Services Scotland Privacy Advisory Committee.
Outcome Events Examined
We used Scotland-wide hospitalization and mortality data, obtained through electronic record linkage, to define 10 outcome events. Each event was determined through the International Classification of Disease (ICD) code recorded in the principal position of the cause of death/discharge diagnosis (Supporting Table 1). The 10 events considered can be subdivided into three classes as follows.
Liver-Related Events
HCV infection has a well-established deleterious impact on liver functioning.[1] Thus, our primary outcome events of interest were liver mortality and hospitalization for severe liver morbidity (SLM); the latter was defined as decompensated liver cirrhosis or hepatocellular carcinoma.
Putative Extrahepatic Manifestations of Infection
HCV infection may impact systemic health. Thus, in line with a previous analysis by Lee et al.,[16] we expanded our list of outcome events to include hospitalization for CVD, respiratory disorders, and neoplasms (excluding liver cancer). In addition, we further obtained data on nonliver and all-cause mortality.
Negative Control Events
We defined a negative control as an outcome that viral persistence is unlikely to cause through cellular pathogenesis, and hence be statistically associated with, given complete adjustment for confounding. We selected three negative controls a priori. These were: hospitalization for an acute instance of drug intoxication, hospitalization for an acute instance of alcohol intoxication, and, last, hospitalization for injury incurred through violence (violence-related admissions are commonly alcohol related.[17, 18] Our assertion is that these outcome events, collectively, function as a barometer of extreme lifestyle exposures.
Primary Exposure Variable
The primary exposure variable in this study was SVR attainment, defined as remaining polymerase chain reaction (PCR) negative for viral RNA for at least 6 months after terminating therapy. Nonresponders, relapsers, and end-of-treatment-responders without a PCR test ≥6 months after completing treatment were all classified as non-SVR. Data-entry staff input SVR status onto the clinical database through applying these definitions to routinely performed PCR test data.
Statistical Analyses
A survival analysis approach underpins our methodology throughout. For each individual, follow-up began 9 months after the end date of the first treatment episode (the 9 months thereby factors in 6 months for SVR eligibility and a 3-month grace period for the patient to receive their PCR test). Follow-up ceased at the date of the first instance of the specified outcome (if that occurred at all) or at the censoring date. We censored follow-up at the earliest date of either (1) mortality, (2) retreatment for initially non-SVR persons, but only if that retreatment episode resulted in SVR by April 1, 2013 (the date the clinical database was complete until), or (3) December 31, 2013 (i.e., the date hospitalization and mortality data were complete until). As a preliminary step, we generated cumulative incidence and Kaplan-Meier's curves for each study outcome (Supporting Figs. 2-5). Thereafter, our analysis takes the form of three strands, each examining the clinical benefit of SVR attainment from a distinct angle.
Analysis 1: Hazard Reduction Associated With SVR
Taking the time to the first instance of each outcome event as our dependent variable, we used Cox's regression to determine the cause-specific hazard reduction for SVR versus non-SVR attainment. We then assessed the extent to which this reduction attenuates after adjustment for a range of covariates. The covariates we controlled for were subdivided in to six categories, as follows:
1. Basic demographics (age group and gender)
2. Medical comorbidities (diagnosis of liver cirrhosis and Charlson Comorbidity Index [CCI])
3. Viral factors (viral genotype only)
4. Behavioral factors (ever intravenous drug use; maximum alcohol consumption sustained for at least 6 months; and past hospitalization for alcohol intoxication, drug intoxication, or violence-related injury)
5. Liver function tests (aspartate aminotransferase [AST]-to-platelet ratio index [APRI] and gamma-glutamyl transferase [GGT])
6. Full adjustment (all covariates within categories 1-5).
Liver cirrhosis is typically diagnosed through a combination of liver biopsy, transient liver elastography, abdominal ultrasound, clinical examination, and routine liver function tests. Maximum alcohol consumption was defined as the self-reported highest amount of alcohol consumed, for a sustained period of time (at least 6 months), before first appointment at a specialist liver clinic. The occurrence of a past hospital episode for acute drug intoxication, alcohol intoxication, and violence-related injury was determined through historical hospitalization data dating back to January 1, 1980. We calculated the CCI to gauge each patient's comorbidity burden at baseline.[19] The CCI assigns a score of 1-6 for each comorbidity present, with a higher score denoting greater severity: A metastatic solid tumor, for example, carries a score of 6, renal disease carries a score of 2, whereas uncomplicated diabetes incurs a score of 1. The final CCI for an individual is the total of these scores. We used historical hospitalization data dating back to January 1, 1980 to determine the presence/absence of the various comorbidities at baseline (as per the ICD codes set out by Quan et al.[20]). We extracted all liver function tests recorded on the clinical database within 2 years of starting treatment. We calculated the mean AST level and mean platelet count in order to infer the APRI. We used a cut-off point of 0.7 to distinguish mild fibrosis (i.e., Metavir F0-F1) from moderate/severe fibrosis (i.e., F2-F4).[21] We also determined the mean level of GGT, given that this was previously found to be an important determinant of SVR attainment in Scotland.[22] Cox regression assumes proportional hazards; we verified this assumption graphically and through Schoenfeld's residual test. In analysis 1, we calculated the cause-specific hazard ratio [HR], which is the appropriate measure to inform whether SVR is an etiological determinant of the outcome event in question. Yet, because it does not consider competing mortality risks, it may not provide the best indication on whether the said outcome will actually occur by a given time point[23]Ñwe address this perspective in analysis 2.
Analysis 2: Absolute Risk Reduction Associated With SVR
We determined the ARR associated with SVR attainment, using the time to the first instance of each outcome event. Because mortality, which may differ between SVR and non-SVR groups, can have a bearing on an individual's risk of experiencing the event in question, we treated death as a competing event in our base-case ARR calculations (however, we also performed a sensitivity analysis where these competing risks were ignored). Cumulative incidence functions stratified by SVR status provide a visual representation of ARR (see Supporting Figs. 2 and 3); but these curves are not corrected for dissimilarity in potential confounders (i.e. age, CCI, and so on) between the SVR and non-SVR groups. We determined the adjusted association between SVR and ARR by generating pseudovalues of the cumulative incidence function and modeling these values directly in a generalized linear model (GLM) with a Gaussian link.[24, 25] We assessed three time points: 2.5, 5.0, and 7.5 years. Adjustment was based on the same range of covariates described in analysis 1. Finally, in this analysis, we only considered outcome events that HCV infection can plausibly cause by cellular pathogenesis (hence, we did not compute ARRs for negative control events).
Analysis 3: Interaction According to Mild Versus Nonmild Liver Disease
The Scottish clinical database records data on liver function tests performed during clinical follow-up. However, these data can be incomplete, principally because tests are numerous and entered onto the database manually. Accordingly, a pretreatment APRI score was available for only 62% of our cohort (see Table 1), even though we expect an AST and platelet count to have been performed for the vast majority. Given that a complete case analysis can introduce bias and reduce statistical power,[26] we imputed plausible values where APRI was unknown using the multiple imputation method.[26, 27] Each missing APRI score was replaced with a set of plausible values reflecting the uncertainty over the right value to impute. We generated 25 imputed APRI scores (categorized as <0.7 vs. ≥0.7) for each missing value using a logit model incorporating all factors outlined in Supporting Table 3 as independent variables. We used these imputed data to gauge whether the association between SVR and each outcome event differs according to mild fibrosis (as indicated by APRI <0.7) versus moderate/advanced fibrosis (APRI ≥0.7). Thus, analysis 1 was supplemented by adding an SVR*APRI interaction term to each fully adjusted Cox regression model. Similarly, analysis 2 was supplemented by adding an SVR*APRI interaction term to each fully adjusted GLM.
Results
Description of Cohort
The cohort was male dominated (70.2% of male gender) and relatively young (41.6 years; standard deviation: 9.6). Liver cirrhosis had been diagnosed in a minority of 8.4% (Table.1). Most persons were known to have acquired infection through intravenous drug use (57.8%). A history of alcohol abuse (defined as a history of drinking >= 50 units/week for a sustained period) was self-reported in 20.2%, and a similar proportion had been hospitalized in the past for a violence-related injury (18.4%). SVR was initially attained in 53.9%, and 7.3% of initial non-SVRs later attained SVR in retreatment by April 2013. APRI score was missing in 38.0% of individuals. Where this score was known, 51.8% had a value <0.7. The median follow-up per patient was 5.3 years (interquartile range: 3.3-8.2). The number of outcome events observed ranged from 102 (liver mortality) to 404 (hospitalization for CVD; see Supporting Table 3).
Analysis 1: Hazard Reduction Associated With SVR
The largest cause-specific hazard reductions were observed with regard to hepatic events (Table 2). For liver mortality and SLM, the fully adjusted hazard ratio (FAHR) was 0.24 (95% confidence interval [CI]: 0.14-0.42; P < 0.001) and 0.21 (95% CI: 0.13-0.35; P < 0.001), respectively. SVR was also associated with nonhepatic events, notably with regard to nonliver mortality (FAHR, 0.68; 95% CI: 0.49-0.95; P = 0.026) and CVD (FAHR, 0.70; 95% CI: 0.57-0.87; P = 0.001). No association was noted for respiratory disorders and neoplasms (P = 0.61 and 0.92, respectively). SVR was associated with two of the three negative control outcomes tested; SVR patients exhibited a 49% hazard reduction for violence-related injury (FAHR, 0.51; 95% CI: 0.33-0.78) and a 48% hazard reduction for alcohol intoxication (FAHR, 0.52; 95% CI: 0.34-0.80). Across all outcomes, we observed minimal attenuation in the SVR cause-specific HR after adjustment for medical comorbidities, viral factors, behavioral factors, and liver function tests.
Discussion
Analysis 1 demonstrates that, in this cohort as a whole, SVR was associated with a reduction in the cause-specific risk of a broad range of outcomes. Consistent with the principally hepatic nature of HCV infection, the greatest divergences were observed for liver-related events. After full adjustment for confounding, patients with SVR exhibited >75% reduced risk of liver mortality and SLM, relative to patients without SVR. Yet, significant associations were not confined to hepatic events alone. We report an association between SVR and a 32% risk reduction in nonliver mortality (P value: 0.026). This concurs with a similar finding in a cohort of human immunodeficiency virus-coinfected patients in Spain,[6] but has not been rigorously examined for HCV monoinfection until now. A second result to emphasize is the association between SVR and a 30% reduction in the risk of hospitalization for CVD; this finding provides further evidence that HCV infection is a risk factor for cardiovascular impairment.[8, 28] We found no association between SVR and hospitalization for respiratory disorders or nonhepatic neoplasms. One explanation of this null finding is the absence of a true effect. However, our definition of neoplasms and respiratory disorders was broad, and we cannot rule out that true, more-specific associations lie within these wide discharge categories.
A valuable dimension to this study is our description of the ARR associated with SVR (see analysis 2). ARR provides the most clinically relevant picture vis-ˆ-vis the value of a medical intervention.[9, 10] Importantly, after 7.5 years of follow-up, SVR was independently associated with ARRs of 3.0%-4.7% for CVD, liver mortality, all-cause mortality, and SLM. In contrast, the association between SVR and ARR for nonliver mortality was smaller (0.9%) and not statistically significant (P = 0.38)Ñassumedly, this equivocal result is the product of a relatively low underlying event rate, combined with a relatively marginal cause-specific HR.
Persons with mild disease represent the bulk of the general infected population,[29] and there is increasing emphasis on diagnosing and treating this subpopulation. U.S. birth cohort screening is a case in point because ~50% of persons due to be identified (equating to 750,000 individuals) are expected to have mild fibrosis.[30] But, in spite of this predominance, the value of an SVR for individuals with mild disease has not been established. Analysis 3 provides an initial look into this issue. Overall, in our cohort, we found that an SVR was associated with significant 7.5-year ARRs for liver mortality, all-cause mortality, SLM, and CVD (see Table 3). Yet, when ARRs were examined separately according to mild versus nonmild disease, we observed strong bimodality. In other words, ARR was apparent to a great extent in individuals with nonmild disease, but to a minimal and equivocal extent in individuals without (see Fig. 2). Arguably, this is an unsurprising result; SLM and liver mortality tend to occur only after liver cirrhosis is established, and it generally takes decades, not 7.5 years, to reach this stage from a point of mild disease. Nevertheless, these findings should reassure patients with mild disease and guide them apropos how urgently to embark onto treatment and at what cost to their immediate quality of life. Conversely, it is worth reiterating that individuals with nonmild disease do appear to profit appreciably from SVR in the short term. At 7.5 years, ARRs were between 6.3% and 10.2% for liver mortality, all-cause mortality, SLM, and CVD. In a context of "sticker shock" drug prices[11] and finite health budgets, this benefit disparity might lend credence to strategically prioritising SVR attainment in those with moderate-to-advanced fibrosis [31]Ñbut a greater evidence base is needed.
Previous studies tend to rationalize the association between SVR and improved prognosis through mechanisms of viral pathogenesis. An alternative explanation (though not a mutually exclusive alternative) is that SVR patients differ behaviorally from non-SVR patients over the course of follow-up.[32] Our examination of "negative control" outcome events supports this theory. We found that the risk of hospitalization for alcohol intoxication and violence-related injury was lower among SVR patients than non-SVR patients. These associations reflect, presumably, a disparity in lifestyle behaviors. Given our efforts to control for any baseline differences between SVR and non-SVR patients, we tentatively offer a hypothesis that SVR facilitates a positive change in lifestyle. Possibly, lifestyle change accounts for some of the superior prognosis apparent among our SVR population. Thus, SVR affects prognosis directly (by halting viral pathogenesis), but perhaps indirectly as well (through stimulating behavior change). We propose two phenomena that might underpin such lifestyle reform.
1. Hawthorne effect: Treatment is a tribulation through which patients are intensively coached (by medical and nursing staff). SVR patientsÑwho tend to remain under close observation for at least a yearÑmay be more susceptible to a persisting "Hawthorne effect" (note: the Hawthorne effect, in a medical context, has previously been defined as: "a motivational response to the interest, care, and attention received through observation and assessment"[33]).
2. Epiphany effect: The euphoria of clearing HCV galvanizes one into adopting healthier lifestyle practices. Indeed, this chimes with a recurrently voiced patient vignette: that SVR attainment invokes a "renewed sense of purpose and determination."[34] What we have dubbed here as the "epiphany effect" is in a similar vein to the "teachable moment"[35]Ñreferring to "windows of opportunity" within which patients are more receptive to the notion of behavioral reform.
Treatment is evolving, and soon regimens will entail as standard: >90% SVR rates, short duration courses, minimal side effects, and minimal patient coaching.[3]It is worth pointing out that the influence of the epiphany/Hawthorne effect is likely to deteriorate in this future era; that is, any benefit hitherto incurred through behavioral change is unlikely to apply in a new climate where patients view SVR attainment as a given.
This study has several strengths. First, we examined a diverse range of outcome events and, in this way, have been able to paint a comprehensive picture vis-ˆ-vis the clinical benefit associated with SVR. Second, our study combines a large number of patients with an average per-patient follow-up in excess of 5 years. This affords us good statistical power. Third, our study is generalizable to "real-world" treatment patients. In fact, we estimate that our cohort includes >80% of all HCV treatment initiates in Scotland between 1996 and 2011. Thus, our results are safe from the selection bias that may creep into studies recruiting cohorts from specialist academic centers. The final key strength to highlight is our initial examination of whether the value of SVR differs according to mild versus nonmild diseaseÑuntil now, an area terra incognita. However, this study has limitations as well as strengths. The SVR cause-specific HR was resilient to adjustment for medical comorbidies, viral genotype, behavioral factors, and liver function tests (see Table 2). Nevertheless, we cannot rule out bias through unmeasured (i.e., residual) confounding. On a related note, it should be highlighted that some important cofactors were missing outright from this analysis (body mass index, steatosis, and socioeconomic status). A second limitation is that we rely upon ICD codes to define our outcome events; however, this coding process can be subject to errors,[36] so it is possible that some outcome events among our cohort have been misclassified. Furthermore, our hospitalization data do not extend to data on accident and emergency attendance. This might particularly exclude negative-control-type events, but it is unclear whether and how the omission of these data would bias our results. Another caveat is that SVR in our study refers, effectively, to diagnosed SVR status. This is subtly distinct from true SVR status because some individuals could have attained SVR but not have been diagnosed as such. Discord between diagnosed and true SVR status is possible for patients who become lost to follow-up and do not receive the requisite PCR testing. From a previous analysis utilizing the Scottish clinical database together with enhanced data collected from medical records, we know that a problematic group are end-of-treatment responders that do not reappear for their subsequent SVR test.[22] But these patients constitute a minority (<5% of all those commencing treatment), so we would not expect this issue to affect our conclusions. Finally, we were not able to correct for individuals that incur health outcomes outside Scotland. Emigration in this cohort will be minimal; nevertheless, there is a risk of a bias if the likelihood differs according to SVR status.
In conclusion, SVR is associated with a reduced risk for a range of hepatic and nonhepatic events. To some extent, this could reflect an improved behavioral profile in those achieving SVR. Finally, our data indicate that the short-term value of SVR is greatest for patients with nonmild disease.
|
|
| |
| |
|
|
|