| |
Trends in Burden of Cirrhosis and Hepatocellular Carcinoma by Underlying Liver Disease in US Veterans, 2001-2013 - Cirrhosis Doubled; Deaths Due to Cirrhosis increased 50%; HCC incidence increased 2.5 fold; HCC mortality tripled
|
| |
| |
Download the PDF here
"The national prevalence and mortality of cirrhosis in VA health care users increased approximately 2-fold and 1.5-fold, respectively, between 2001 and 2013, whereas the incidence and mortality of HCC increased nearly 3-fold. If current trends continue, our data suggest that the prevalence of cirrhosis will peak in 2021. In contrast, the incidence of HCC continues to increase, confirming worrisome predictions of rapid growth put forward by work conducted in the mid-2000s......As this HCV-infected cohort ages and accumulates more years of chronic infection, an increasing proportion will progress from hepatic fibrosis to cirrhosis, HCC, liver failure, and death. Inevitably, this burden will begin to decline in the future because the US incidence of new HCV infections decreased from 380,000 infections per year (95% confidence interval [CI], 250,000-500,000) in the 1980s5 to approximately 38,000 per year in the 1990s, and 17,000-19,000 per year after 2000.6 However, exactly when the burden of HCV-related HCC and cirrhosis will begin to decline in the United States remains unclear.
Cirrhosis prevalence nearly doubled from 2001 to 2013......an increase of 59% over the previous 13-year period. HCV-related cirrhosis resulted in the greatest increase in prevalence from 2001 to 2013 (252 to 503, respectively, per 100,000 enrollees) followed by NAFLD (80 to 161, respectively, per 100,000 enrollees).
Deaths in patients with cirrhosis increased from 83 to 126 per 100,000 patient-years, largely driven by HCV.
HCC incidence was 2.5-fold increased from 17 to 45 per 100,000 patient-years........Deaths in patients with cirrhosis increased from 83 per 100,000 VA patient-years (n = 3201) in 2001 to 126 per 100,000 VA patient-years (n = 7196) in 2013 (Figure 2D). This increase was driven almost exclusively by rising mortality in patients with HCV-related cirrhosis (from 28 to 60 per 100,000 VA patient-years, including similar increases in both "HCV+alcohol" and "HCV-no alcohol" subgroups), whereas deaths in cirrhosis patients with ALD or NAFLD did not increase appreciably (Figures 2D and 2E). The age of cirrhosis patients increased from a mean 57.3 years (SD 10.5) in 2001 to 62.4 (SD 8.4) in 2013 (Figure 2F). This increase was most prominent in HCV (52.2 to 60.2 years) and least prominent in NAFLD (64.9 to 66.8 years).
HCC mortality tripled......Deaths in HCC patients increased from 13 per 100,000 VA patient-years (n = 485 deaths) in 2001 to 37 per 100,000 VA patient-years (n = 2144 deaths) in 2013 (Figures 3C, and 3D). This increase was again driven primarily by patients with HCV-related HCC (including both "HCV+alcohol" and "HCV-no alcohol" subgroups), although modest increases also occurred in patients with ALD and NAFLD-related HCC."
----------------
Trends in Burden of Cirrhosis and Hepatocellular Carcinoma by Underlying Liver Disease in US Veterans, 2001-2013
Gastroenterology Nov 2015
Lauren A. Beste,1,2,3 Steven L. Leipertz,2 Pamela K. Green,2 Jason A. Dominitz,1,4 David Ross,5 and George N. Ioannou2,4,6
1Primary Care Service, Veterans Affairs Puget Sound Health Care System, Seattle, Washington;
2Health Services Research andDevelopment, Veterans Affairs Puget Sound Health Care System, Seattle, Washington;
3Division of General Internal Medicine,University of Washington, Seattle, Washington;
4Division of Gastroenterology, University of Washington, Seattle, Washington;
5HIV, HCV, and Public Health Pathogens Programs, Office of Public Health/Clinical Public Health, US Department of Veterans
Affairs, Washington, DC; and
6Division of Gastroenterology, Veterans Affairs Puget Sound Health Care System, Seattle,
Washington
Background & Aims
Cirrhosis and hepatocellular carcinoma (HCC) are predicted to increase in the United States but the accuracy of prior forecasts and the contributions from various liver disease etiologies remain unclear. We aimed to determine the burden of cirrhosis and HCC according to underlying cause from 2001 to 2013.
Methods
We developed a national retrospective cohort of Veterans Affairs (VA) patients with the diagnosis of cirrhosis (n = 129,998) or HCC (n = 21,326) from 2001 to 2013. We used laboratory results, International Classification of Diseases, ninth edition (ICD-9) codes, and body mass index to identify underlying etiologies.
Results
In 2013, VA provided care to 5,720,614 individuals, of whom 60,553 (1.06%) had cirrhosis and 7,670 (0.13%) had HCC.
Hepatitis C virus (HCV) was present in an increasing proportion of cirrhosis and HCC between 2001 and 2013, reaching 48% of cirrhosis cases and deaths and 67% of HCC cases and deaths by 2013.
Cirrhosis prevalence nearly doubled from 2001 to 2013 (664 to 1058 per 100,000 enrollees), driven by HCV and nonalcoholic fatty liver disease (NAFLD).
Cirrhosis incidence ranged from 159 to 193 per 100,000 patient-years. Deaths in patients with cirrhosis increased from 83 to 126 per 100,000 patient-years, largely driven by HCV. HCC incidence was 2.5-fold increased from 17 to 45 per 100,000 patient-years. HCC mortality tripled from 13 to 37 per 100,000 patient-years, driven overwhelmingly by HCV, with much smaller contributions from NAFLD and alcoholic liver disease.
Conclusions
Cirrhosis prevalence and mortality and HCC incidence and mortality increased from 2001 to 2013, driven by HCV, with a smaller contribution from NAFLD. If current trends continue, cirrhosis prevalence will peak in 2021. Health care systems will need to accommodate rising numbers of patients with cirrhosis and HCC.
Cirrhosis and hepatocellular carcinoma (HCC) may result from any chronic liver disease, including hepatitis C virus (HCV), hepatitis B virus (HBV), alcoholic liver disease (ALD), nonalcoholic fatty liver disease (NAFLD), hemochromatosis, autoimmune hepatitis (AIH), primary biliary cirrhosis (PBC), and primary sclerosing cholangitis (PSC). These conditions account for most of the cases of cirrhosis and HCC in the United States and worldwide, but their relative contributions to the burden of chronic liver disease are unclear. It is critical to understand trends in the causes of cirrhosis and HCC in order to effectively target disease interventions and plan for future impact on health care systems.
Previous studies reported increasing prevalence and incidence of HCV-related cirrhosis and HCC in the United States1, 2, 3, 4 despite a sharp decline in new HCV infections after 19905, 6 and a declining prevalence of HCV infection since 2001.7 Previous statistical models predicted that the prevalence of HCV-related cirrhosis and the incidence of HCV-related HCC would peak around 2020.7 As NAFLD becomes increasingly common due to national epidemics of obesity and diabetes, NAFLD-related cirrhosis and HCC are also expected to increase. Trends in the US burden of cirrhosis and HCC related to HBV, ALD, and other liver diseases are less well described. Two recent studies suggested that the rate of increase in HCC incidence might be slowing down in the United States in recent years.8, 9 We aimed to determine national trends in the prevalence, incidence, and mortality of cirrhosis and HCC by underlying cause among all patients who received care in the Veterans Affairs (VA) health care system between 2001 and 2013.
Methods
Data Source: Veterans Affairs Corporate Data Warehouse
The VA health care system is composed of 154 medical centers and 875 ambulatory care and community-based outpatient clinics throughout the United States. It is the largest integrated health care provider in the country and uses electronic medical records almost exclusively. In 2013, 5,720,614 veterans received VA health care.10 We extracted electronic data for all patients in VA care from October 1, 1999 until July 21, 2014, using the VA Corporate Data Warehouse, a national, continually updated repository of data from the VA's computerized patient records.11 We extracted patient demographics, inpatient and outpatient visits, problem lists, procedures, vital signs, diagnostic tests, laboratory tests, and pharmacy prescriptions.
Human Subjects
Study activities were conducted according to the ethical guidelines of the Declaration of Helsinki. This project was performed as an approved quality improvement initiative under the auspices of the VA Office of Public Health.
Study Population
We identified all patients who received VA health care from 2001 to 2013 and had a diagnosis of either cirrhosis (n = 129,998) or HCC (n = 21,326). For each calendar year, we identified patients who were "in care" during that calendar year, defined by having at least 1 inpatient or outpatient visit for any indication during that year and who had a diagnosis of cirrhosis or HCC recorded during or before that year. Cirrhosis was defined by the following International Classification of Diseases, ninth revision (ICD-9) codes recorded at least twice in inpatient or outpatient medical records: 571.2 (cirrhosis with alcoholism), 571.5 (cirrhosis no mention of alcohol), 456.0-456.21 (esophageal varices with or without bleeding), 567.23 (spontaneous bacterial peritonitis), 572.2 (hepatic encephalopathy), and 572.4 (hepatorenal syndrome). HCC was defined by ICD-9 code 155.0 (primary liver carcinoma), recorded at least twice in inpatient or outpatient medical records. These diagnostic definitions of cirrhosis and HCC based on ICD-9 codes derived from VA electronic medical datasets have been shown to have high agreement with review of the medical records by a physician (cirrhosis: positive predictive value of 88%; negative predictive value of 92%; HCC: positive predictive value of 94%; negative predictive value of 100%) and have been extensively used in epidemiological studies.1, 12, 13, 14, 15
Cause of Liver Disease
Diagnostic criteria used to define the underlying liver disease in patients with cirrhosis or HCC are shown in Figure 1.
Because liver disease could have more than 1 cause, especially alcohol combined with another etiology, we used the following rules to create mutually exclusive categories of underlying liver disease (Figure 1). (1) Patients with HCV infection were categorized as HCV regardless of any additional etiologies; given the high overlap between HCV infection and alcohol use disorders, the HCV group was also subdivided into those with ("HCV+alcohol") and those without ("HCV-no alcohol") comorbid alcohol use disorders. (2) ALD was identified as the cause in patients with alcohol use disorders (defined in Figure 1) and in the absence of HCV, HBV, hemochromatosis, PBC, PSC, and autoimmune hepatitis. (3) NAFLD was identified for patients without any other cause (including viral hepatitis or alcohol use disorders) who had diabetes (ICD-9 code 250-250.92, recorded at least twice16) or body mass index (BMI) ≥30 kg/m2 prior to diagnosis of cirrhosis. NAFLD-related cirrhosis does not have pathognomonic serological, radiological, or histological features (even hepatic steatosis is frequently absent after cirrhosis develops). Hence we adapted a clinical definition of NAFLD based on previous work17 that reflects the diagnostic process used in clinical practice (ie, NAFLD is suspected in the presence of risk factors such as obesity and diabetes and after exclusion of other etiologies.
Other Patient Characteristics
We ascertained age, race, ethnicity, sex, BMI, and laboratory results for serum bilirubin, creatinine, and albumin concentrations, blood platelet count and international normalized ratio (INR). Type 2 diabetes mellitus was defined by ICD-9 codes 250-250.92. Substance use disorders were defined by the presence of codes for substance abuse (305.2-305.9), dependence (304.0-304.9), or drug withdrawal (292.0). A model for end-stage liver disease (MELD) score in 2013 was calculated by the MELD formula,18 using the most recent laboratory values of total bilirubin, serum creatinine, and INR available in 2013.
Statistical Analysis
We determined the number of patients with cirrhosis or HCC who were in care (prevalence) or who had a new diagnosis of cirrhosis or HCC (incidence) or who died (mortality) each year from 2001 to 2013, categorized by cause of liver disease. We expressed these statistics as proportions of both the number of all patients with cirrhosis or HCC in care that year and the number of patients enrolled in VA care that year (obtained from the National Center for Veterans Analysis and Statistics).10 We performed the latter analysis to account for the steady increase in VA patient population from 3,843,832 in 2001 to 5,720,614 in 2013. We considered age-adjusting the incidence and prevalence of cirrhosis or HCC when comparing years 2001 to 2013 but ultimately decided against it to avoid masking the birth cohort effect of HCV in the population born between 1945 and 1965. One prevailing hypothesis for the rising incidence and prevalence of cirrhosis and HCC is the aging of the HCV-infected cohort in the United States (addressed further in Discussion) and age adjustment would inappropriately mask this birth cohort effect. When analyzing incidence, we deliberately excluded the first year (2001) and the last year (2013) of the study period: incidence was underestimated in 2013 because our data extended only to July 1, 2014, and we required the diagnosis to be recorded twice (eg, a patient presenting for the first time with cirrhosis in December 2013 might not have been seen again before July 2014); incidence was overestimated in 2001 because our data extended back only to October 1, 1999. Thus, a patient might have appeared to present with cirrhosis for the first time in 2001 when in fact he or she might have been given the diagnosis before October 1, 1999 and not represented in the interim.
Results
Characteristics of Patients With Cirrhosis or HCC in 2013
Of 5,720,614 patients in VA care in 2013, 60,553 patients (1.06%) had cirrhosis and 7,670 (0.13%) had HCC. Among patients with cirrhosis, 28,811 (48%) had HCV infection (60.9% of whom also had a chronic alcohol-related diagnosis), 18,404 (30%) had ALD, 9027 (15%) had NAFLD, 1299 (2.1%) had HBV infection, and 1737 (2.9%) had cryptogenic cirrhosis, while <1% had hemochromatosis, PSC, PBC, or AIH (Table 1). The average age was 62.4 years; 77% were white, 18% were black, and 8.7% were Hispanic. The majority (97%) were male. Gastroesophageal varices was the most common cirrhosis complication, reported in 24.9% of patients, with 6.0% of patients having a variceal hemorrhage. Ascites was the second most common complication, affecting 17.0% of patients. The mean MELD score was 9.8 (SD 6.9).
Among 7670 patients with HCC in VA care in 2013, 5225 (68%) had HCV infection (61.3% of whom also had an alcohol-related diagnosis), 873 (11%) had ALD, 1029 (13%) had NAFLD, 176 (2.3%) had HBV infection, 242 (3.2%) had cryptogenic cirrhosis, and <1% had other liver diseases (Table 2). The average age was 64 years; 69% were white, 25% were black, and 10% were Hispanic. Nearly all (99%) were male. Gastroesophageal varices was the most common cirrhosis complication in this population (22.8%), with 5.5% having a history of hemorrhage. Ascites was reported in 18.2% of patients. The mean MELD score was 11.4 (SD 7.8).
As expected by the study definition of NAFLD, those with NAFLD were older, more obese, more likely to be diabetic, and less likely to have a history of substance abuse compared to patients with HCV or alcoholic cirrhosis or HCC. Compared to patients with HCV alone, those with "HCV+alcohol" were younger (59.6 vs 61.2 years of age for cirrhosis; 60.9 vs 63.1 years of age for HCC) and had higher MELD scores (10.2 vs. 9.3, respectively, for cirrhosis; 12.1 vs. 10.9, respectively, for HCC).
Trends in Cirrhosis Prevalence, Incidence, and Mortality, 2001-2013
The prevalence of cirrhosis among VA enrollees has risen steadily each year from 664 per 100,000 enrollees (n = 25,534 cases) in 2001 to 1058 per 100,000 enrollees (n = 60,553 cases) in 2013 (Figure 2; Supplementary Table 1), representing an increase of 59% over the previous 13-year period. HCV-related cirrhosis resulted in the greatest increase in prevalence from 2001 to 2013 (252 to 503, respectively, per 100,000 enrollees) followed by NAFLD (80 to 161, respectively, per 100,000 enrollees). In contrast, the prevalence of alcoholic cirrhosis increased only modestly from 291 to 327 per 100,000 enrollees (Figure 2A). HCV and NAFLD accounted for an increasing proportion of patients with cirrhosis whereas ALD accounted for a decreasing proportion (Figure 2B). HCV became the leading cause of cirrhosis in 2004 when it exceeded ALD. Unlike the ALD group, the prevalence of cirrhosis related to the "HCV+alcohol" and "HCV-no alcohol" subgroups increased parallel with the total HCV group (Figures 2A and 2B), suggesting that trends in the "HCV+alcohol" group were driven by trends in HCV infection rather than trends in ALD.
The number of incident cases of cirrhosis has remained fairly stable between 2002-2012, ranging from 159 to 193 per 100,000 VA patient-years (Figure 2C; Supplementary Table 2). When parsed by cause of underlying liver disease, cirrhosis incidence was relatively stable for HCV and NAFLD and declined for ALD.
Deaths in patients with cirrhosis increased from 83 per 100,000 VA patient-years (n = 3201) in 2001 to 126 per 100,000 VA patient-years (n = 7196) in 2013 (Figure 2D). This increase was driven almost exclusively by rising mortality in patients with HCV-related cirrhosis (from 28 to 60 per 100,000 VA patient-years, including similar increases in both "HCV+alcohol" and "HCV-no alcohol" subgroups), whereas deaths in cirrhosis patients with ALD or NAFLD did not increase appreciably (Figures 2D and 2E). The age of cirrhosis patients increased from a mean 57.3 years (SD 10.5) in 2001 to 62.4 (SD 8.4) in 2013 (Figure 2F). This increase was most prominent in HCV (52.2 to 60.2 years) and least prominent in NAFLD (64.9 to 66.8 years).
Trends in HCC Incidence and Mortality, 2001-2013
Incident cases of HCC increased from 17 per 100,000 VA patient-years (n = 746) in 2002 to 45 per 100,000 VA patient-years (n = 2532) in 2012 (Figure 3A and Supplementary Table 3). This increase was driven almost exclusively by HCV-related HCC (including both "HCV+alcohol" and "HCV-no alcohol" subgroups), whose incidence increased from 8 to 30 per 100,000 VA patient-years, while the incidence of ALD and NAFLD-related HCC increased only slightly. HCV accounted for an increasing percentage of HCC cases from 2002 to 2012, reaching 67% of cases in 2012, followed by NAFLD (15%) and ALD (12%) (Figure 3B). There was little increase in the mean age of patients with HCC between 2001 and 2013 (62.1 to 64.0 years, respectively) with similar trends for HCV, alcohol, and NAFLD (Figure 3E).
Deaths in HCC patients increased from 13 per 100,000 VA patient-years (n = 485 deaths) in 2001 to 37 per 100,000 VA patient-years (n = 2144 deaths) in 2013 (Figures 3C, and 3D). This increase was again driven primarily by patients with HCV-related HCC (including both "HCV+alcohol" and "HCV-no alcohol" subgroups), although modest increases also occurred in patients with ALD and NAFLD-related HCC.
Comparison of Incidence and Mortality of HCC and Cirrhosis, 2001-2013
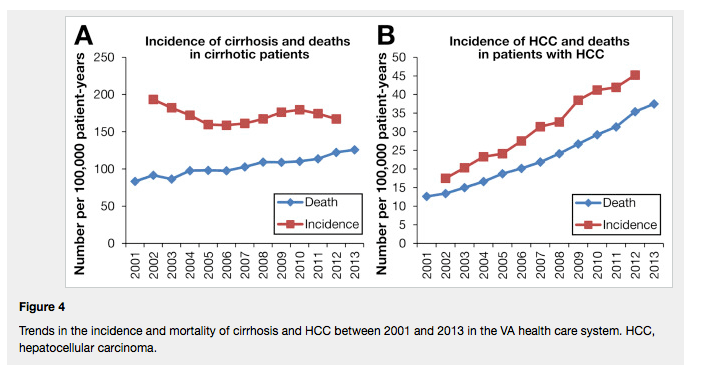
Figure 4 shows that mortality increased over time in patients with cirrhosis on average by 5 more deaths per 100,000 patient-years every year from 2010 to 2013. If the incidence of cirrhosis remains stable at ~167 per 100,000 patient-years (the level in 2012), then the mortality in cirrhotic patients, which was 126 per 100,000 patient-years in 2013, should exceed 167 in ~8 years or 2021 (167 - 126/5 = 8.2). Assuming constant trends regarding rate of progression to cirrhosis, death from cirrhosis complications, and treatment of chronic liver disease, the prevalence of cirrhosis should begin to decline in 2021 since mortality will exceed incidence. Similar calculations limited to patients with HCV show that the mortality of HCV-infected cirrhotic patients should exceed the incidence of HCV-related cirrhosis in ~7 years or 2020. Figure 4 also shows that, in contrast to cirrhosis, HCC-related incidence is increasing at least as rapidly as HCC-mortality without any obvious plateau in either incidence or mortality.
Discussion
The national prevalence and mortality of cirrhosis in VA health care users increased approximately 2-fold and 1.5-fold, respectively, between 2001 and 2013, whereas the incidence and mortality of HCC increased nearly 3-fold. If current trends continue, our data suggest that the prevalence of cirrhosis will peak in 2021. In contrast, the incidence of HCC continues to increase, confirming worrisome predictions of rapid growth put forward by work conducted in the mid-2000s.7
These trends were dominated by a rise in HCV-related cirrhosis and HCC, with a much smaller contribution from NAFLD and ALD. As of 2013, HCV infection (with or without concomitant alcohol-use disorders) accounted for a predominant and still-increasing proportion of the burden of cirrhosis and HCC (48% of cirrhosis and 68% of HCC cases), followed by ALD (30% of cirrhosis and 11% of HCC) and NAFLD (15% of cirrhosis and 13% of HCC), while all remaining causes combined accounted for 7% of cirrhosis and 7% of HCC cases.
Increases in HCV-related cirrhosis and HCC in the United States can largely be explained by the natural history of HCV infection. Most HCV-infected persons currently living in the United States were born between 1945 and 1965 and were infected as young adults between 1970 and 1990.19, 20 As this HCV-infected cohort ages and accumulates more years of chronic infection, an increasing proportion will progress from hepatic fibrosis to cirrhosis, HCC, liver failure, and death. Inevitably, this burden will begin to decline in the future because the US incidence of new HCV infections decreased from 380,000 infections per year (95% confidence interval [CI], 250,000-500,000) in the 1980s5 to approximately 38,000 per year in the 1990s, and 17,000-19,000 per year after 2000.6 However, exactly when the burden of HCV-related HCC and cirrhosis will begin to decline in the United States remains unclear.
Previous studies reported increases in HCV-related cirrhosis and HCC before the time period of this study or predicted future increases.1, 2, 21 National studies done in the United Kingdom reported an increase in the age-adjusted incidence of cirrhosis between 1998 and 2009, although alcohol accounted for 61.9% of cirrhosis in that population compared to only 11.3% for viral hepatitis (even though cause of disease was assigned hierarchically to viral hepatitis first, just as in our study).22 As such, UK projections regarding future burden of disease may not extrapolate to the US population. Two recent US studies based on Surveillance, Epidemiology and End Results (SEER) 18 registries, covering 28% of the US population, suggested that the rate of increase in HCC incidence might be decelerating in recent years8, 9. Njei et al9 reported that, although HCC incidence increased by an age-adjusted annual percent of change (APC) of 5.8% from 2000 to 2005 and 4.3% from 2005 to 2009, the APC was only 1.3% from 2009 to 2011. Using SEER 18 data, Altekruse et al8reported a higher age-adjusted APC in HCC incidence during 2000-2007 (5.4%) than 2007-2010 (2.3%). However, they also reported that HCC-related mortality in the entire United States (not just the SEER regions) was increasing at an age-adjusted APC of 2.1% between 2000 and 2010 without any sign of decline. The differences in HCC incidence and mortality between SEER regions versus the United States as a whole raise concerns that SEER may not accurately reflect the US population with respect to HCC. SEER data lack information on causes of underlying liver disease, so no conclusions can be drawn for relative trends in HCV- versus non-HCV-related liver diseases. Most importantly, age adjustment in the SEER studies likely attenuated the increase in HCC incidence and mortality that is related to the aging of the HCV-infected cohort nationally.
Our data suggest that the prevalence of all cirrhosis will begin to decline in 2021 and specifically HCV-related cirrhosis in 2020. With regard to HCC, we found an increasing incidence and mortality (both overall and HCV-specific) through 2013, with no sign of decline in the annual rate of increase, in contrast to the aforementioned SEER-based studies.8, 9 Therefore, our results do not allow us to predict when HCC rates might start declining but suggest that the HCC epidemic may be greater and more protracted then predicted by previous studies.
ALD was the second most common cause of cirrhosis and HCC in the VA after HCV infection. Elimination of ALD could impact up to 28.6% of cirrhosis incidence and 11.4% of HCC, not counting potential benefits to the 60.9% of HCV patients with comorbid alcohol use disorders. Despite VA's efforts to identify and address problem alcohol use, including standardized annual alcohol use disorders screening and brief interventions to treat alcohol use disorders, rates of ALD-related cirrhosis and HCC have remained stubbornly constant. If anything, our data underestimate the true impact of ALD because we defined it only in the absence of other known liver diseases. It is likely that ALD contributes to the development of cirrhosis among patients categorized under other etiologies, especially those with HCV-infection and cirrhosis, of whom 60.9% had a history of comorbid alcohol abuse. Our data underscore the high morbidity and mortality of alcohol use disorders and the need for renewed attention to alcohol as a preventable cause of liver disease.
NAFLD was the third most common cause of cirrhosis and HCC, accounting for approximately 18% of cirrhosis incidence and 14% of HCC incidence. Given the rising rates of obesity and diabetes, the main risk factors for NAFLD, one might expect a greater proportional increase in NAFLD-related cirrhosis and HCC. The obesity and diabetes epidemics are likely to indirectly impact HCV-related cirrhosis and HCC almost as much as they impact NAFLD-related cirrhosis and HCC, since obesity and diabetes increase the risk of HCV-related cirrhosis and HCC.23, 24, 25 Thus, the increases in HCV-related cirrhosis and HCC are driven both by the new infections that occurred between 1970 and 1990 and, to a lesser extent, by the increasing prevalence of obesity and diabetes; whereas increases in NAFLD-related cirrhosis and HCC are likely driven primarily by increasing prevalence of metabolic risk factors.
Much of the incidence of cirrhosis and HCC is preventable. Treatment of alcohol-use disorders can forestall ALD, and improvements in NAFLD risk factors (eg, obesity, diabetes) may reduce nonalcoholic steatohepatitis (NASH)-related cirrhosis and HCC. As of 2012, HCV (with or without concomitant alcohol use disorders) is implicated in 46.7% of cirrhosis incidence and 66.7% of HCC incidence. To date, however, antiviral treatments for HCV have had a negligible impact on the incidence and mortality of HCV-related cirrhosis and HCC at a population level before 2013. As of 2013, only 23% of HCV-infected patients in VA care ever received antiviral treatment of whom the majority were not cured.26 Treatment rates are even lower in the general US population, estimated at 13%, with only 5% to 6% of all HCV-infected people having been cured.27, 28 Furthermore, the patients who were cured may not represent those most at risk for cirrhosis and HCC, as treatments before 2013 were very poorly tolerated and had much lower response rates in patients with cirrhosis or advanced fibrosis. Multiple, highly effective, well-tolerated, direct antiviral agents have been available since November 2013. For the first time, most future cases of HCV-related cirrhosis or HCC are now, in theory, preventable. In addition, patients with cirrhosis can be offered antiviral treatment to prevent cirrhosis-related HCC or death. Dramatic reductions in the incidence and mortality of HCV-related HCC and cirrhosis may now be achievable, but only if greater proportions of HCV-infected patients undergo successful antiviral treatment. Currently the main obstacle to achieving this goal is the prohibitive cost of antiviral treatments. Unless the costs of HCV antiviral treatment decline and the rates of HCV antiviral treatment increase substantially in the United States, the majority of patients at risk for HCV-related mortality in the next 10 to 20 years will die without receiving curative antiviral treatment.
Because the VA population is overwhelmingly male, our results may be generalizable to other US males, who compose the majority of cirrhosis cases and roughly three-quarters of HCC cases in the United States as a whole.9 Not surprisingly, absolute rates of cirrhosis and HCC incidence, prevalence, and mortality in VA patients are higher than those of unselected US males, as the VA population is enriched in risk factors for both cirrhosis and HCC and it represents patients enrolled in medical care. However, the trends over time in rates of cirrhosis and HCC, especially within disease categories, likely do reflect trends in the US male population. For example, our finding that HCV-related HCC incidence (including both "HCV+alcohol" and "HCV-no alcohol") more than tripled from 2002 to 2012, would lead us to expect a similar relative increase in the male US population with HCV, since the aging of the HCV cohort is occurring simultaneously in both populations.
Whether the relative proportions of HCC and cirrhosis attributed to each cause of underlying liver disease reflect the male US population requires careful consideration, since this depends on the prevalence of each cause in the VA relative to the United States. The prevalence of HCV infection in the VA (~4% in 1998 to 200029) is approximately double that of comparable age and sex groups of US population.26 The main risk factor for NAFLD, obesity, is more common in the VA than in the US population,30 and the prevalence of diabetes is double in VA.16 Alcohol use disorders are considered more common in the VA than in the general US population, although a recent very large study reported similar rates of alcohol use and almost identical rates of "unhealthy" drinking based on AUDIT-C scores among VA (45% in men, 37% in women) and US populations (46% in men and 35% in women).31 Although current population-based estimates of liver disease etiology in the general United States are sparse, the Chronic Liver Disease Surveillance Network reported a similar distribution of etiologies for incident cases of cirrhosis from 1999-2001 compared to 2002 VA data (32.6% vs 39% for HCV, 43.9% vs 39% for ALD, and 14.7% vs 12% for NAFLD).32 Therefore, the relative proportion of cases of cirrhosis or HCC attributed to these 3 main causes of liver disease is likely similar between the VA and US populations, with a somewhat greater contribution of HCV infection in the VA.
HCC and especially cirrhosis may remain occult for significant periods of time before presenting clinically. HCV-infected patients are more likely than those with NAFLD or ALD to undergo liver ultrasound or other diagnostic testing in the course of routine care, and therefore have more opportunity to be diagnosed earlier with cirrhosis or HCC. VA has diagnosed a greater proportion of its HCV-infected patients (~80%)26 as a result of screening efforts compared to the general US population (50%).28 Due to VA's superior screening rates for HCV, the proportion of cases of cirrhosis and HCC attributed to HCV may appear higher than that of the US population. Though this effect stems from relative underdiagnosis of cirrhosis and HCC in patients with ALD and NAFLD, the result is an apparent enhancement in the proportion of cases of cirrhosis or HCC attributed to HCV in the VA as well as in the general US population. This effect in no way invalidates the observed trends in HCV-related cirrhosis and HCV: it does suggest a need for more comprehensive HCV testing in the general United States and for accurate diagnosis of cirrhosis and HCC in patients with non-viral disease etiologies.
Our results are limited by definitions of cirrhosis and HCC based on ICD-9 codes derived from VA medical records. These diagnostic definitions have high agreement with physician medical record review and have been extensively used in epidemiological studies.1, 12, 13, 14, 15 It would be impracticable to conduct a nationally representative study in which the diagnosis of cirrhosis or HCC is individually confirmed or excluded prospectively by a series of predetermined laboratory tests, imaging studies, physical examination findings and histological examination of a liver biopsy over a period of 13 years. It is likely that cases of early cirrhosis with preserved liver function and no clinical manifestations were missed by our definition, such that, if anything, we underestimated of the true prevalence of cirrhosis. Such cases of early cirrhosis are notoriously difficult to diagnose with certainty in the absence of a liver biopsy, which is not performed in the majority of patients. We assigned the causes of underlying liver disease based on the "gold standard" virological and serological tests for HCV and HBV and on ICD-9 codes for hemochromatosis, autoimmune hepatitis, PBC, and PSC. NAFLD- and ALD-related cirrhosis are often difficult to diagnose in clinical practice because they lack pathognomonic laboratory or histological markers. We used diagnostic definitions of ALD (based on alcohol use disorders) and NAFLD (based on obesity or diabetes) in the absence of viral hepatitis to reflect what is done in clinical practice, recognizing that these definitions do not capture cases of ALD or NAFLD that overlap with viral hepatitis. Therefore, in the case of ALD we also reported patients with HCV with or without alcohol use disorders separately. Further work to refine the alcohol subgroup and discriminate between active and past use would be valuable to discriminate the role of alcohol more accurately. Lastly, though we reported mortality in patients with cirrhosis or HCC, we are unable to ascertain the number of deaths directly attributable to liver disease as opposed to competing extra-hepatic causes. Future work is needed to assess the causes of death in the cirrhosis and HCC population.
We considered the possibility that our observations could be biased by an influx of persons with HCV into the VA health care system during the study period. However, the number of HCV-infected patients in VA care has been approximately constant from 2009 to 2013, with ~175,000 patients with known HCV viremia in care each year.33 In fact, because the overall population of patients in VA care is increasing every year from 3,843,832 in 2001 to 5,720,614 in 2013 (see Supplementary Table 1, Supplementary Table 2, Supplementary Table 3), the prevalence of HCV infection in the VA is declining, as it has been in the general US population, since 2001.7 Therefore, the increase in HCV-related cirrhosis and HCC has occurred despite a decreasing prevalence of HCV.
Our results illustrate that cirrhosis incidence remained approximately stable from 2001 to 2013 but prevalence and mortality continue to increase. In contrast, HCC incidence increased dramatically. HCV is the overwhelming driver of these trends, with smaller contributions from ALD, NAFLD, and other liver diseases. Opportunities to modify patient-level risk factors such as alcohol use, NAFLD risk factors, and particularly HCV infection within the VA and other US health care systems offer promise for mitigating the current and projected burden of liver disease in the United States.34, 35, 36 The increasing burden of cirrhosis and HCC highlights the need for greater efforts to address their causes at a population level.
|
|
| |
| |
|
|
|