| |
Hypertension in HIV
|
| |
| |
Download the PDF here
Download the PDF here
from Jules: today the NIH announced they were stopping a study in hypertension as they found that lower levels of blood pressure than had been previously recommended appeared to show more benefit but experts raised safety concerns regarding lowering the recommendations for blood pressure, I just emailed out the study results & comments, so here is a report on hypertension in HIV.
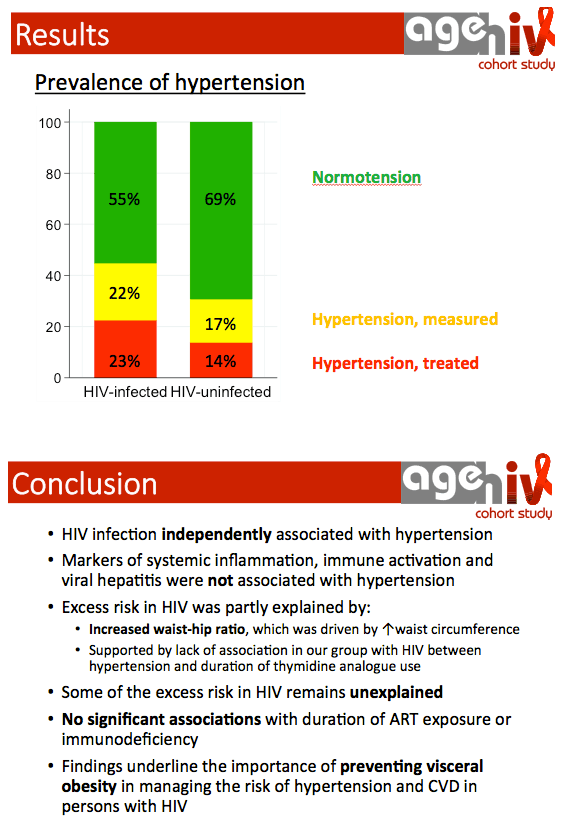
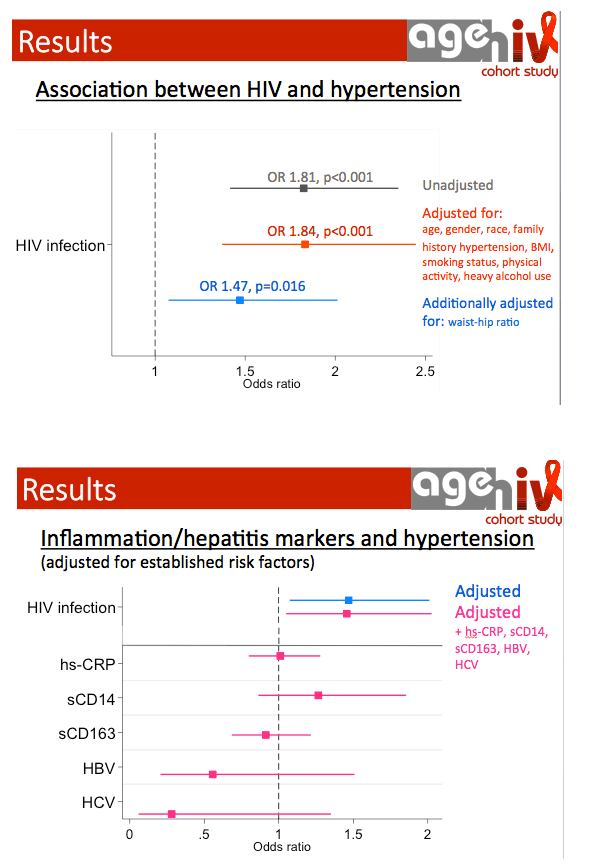
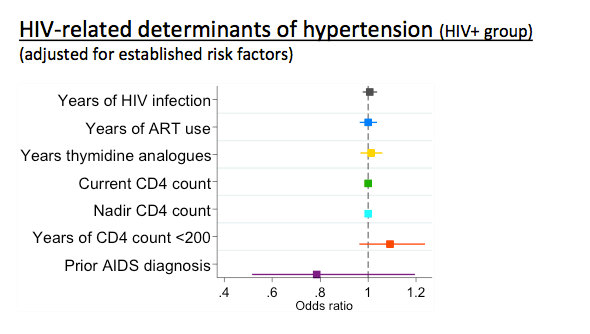
Hypertension Increased in HIV+ vs HIV-neg in Amsterdam AgehIV Cohort Study (45% vs 31%) & HIV is Independently Associated with Hypertension - (10/17/14)
Since HIV infection is associated with an increased risk for cardiovascular disease & measures of subclinical cardiac dysfunction are increasingly used to investigate the underlying etiology of this association, researchers evaluated the relationships between measures of cardiac strain & cardiac fibrosis by MRI with traditional cardiovascular disease risk factors & biomarkers of immune activation in a cohort of HIV+ adults without known cardiovascular disease compared to matched healthy controls. They found: strain indices of systolic dysfunction were impaired in HIV+ subjects, further, subclinical impairment in systolic function was associated with markers of chronic immune activation. (we know that immune activation & inflammation persist despite undetectable HIV viral load). Similar to patients with chronic heart failure, increased levels of MCP-1, a chemokine important in the regulation of monocyte & macrophage migration & a marker of immune activation, was strongly associated with impairment in cardiac function. LBP, an acute phase protein made in response to lipopolysaccharide (LPS), was also associated with impaired cardiac strain in HIV+ patients. "Our findings indicate that subclinical impairment in cardiac strain tracks with markers of chronic inflammation & immune activation, which may serve as targets for future therapeutic strategies to optimize long-term cardiovascular health in persons living with HIV".
Impaired Cardiac Strain and Biomarkers of Immune Activation in HIV - (10/10/14)
CROI/2015: Impaired Cardiac Strain and Biomarkers of Immune Activation in HIV........http://www.natap.org/2015/CROI/croi_129.htm
Conclusions: HIV-infected subjects demonstrate subclinical impairment in systolic function and this is associated with markers of chronic immune activation, inflammation and tissue remodeling. Similar to patients with chronic heart failure, increased levels of MCP-1, a chemokine important in the regulation of macrophage migration and a marker of immune activation, was a strong independent predictor of impairment in cardiac function. LBP, an acute phase protein made in response to LPS, and TIMP-1, a marker of tissue remodeling, were also associated with impaired cardiac strain. Our findings indicate that subclinical impairment in cardiac strain tracks with markers of chronic inflammation and immune activation, which may serve as targets for future therapeutic strategies to optimize long-term cardiovascular health in persons living with HIV.
----------------------------
Antiretroviral medications associated with elevated blood pressure among patients receiving highly active antiretroviral therapy
AIDS April 24 2006
Crane, Heidi Ma; Van Rompaey, Stephen Ea; Kitahata, Mari Ma,b
A clear understanding of factors contributing to the development of elevated BP among HIV-infected patients is needed to target prevention efforts and help guide research that may lead to improved interventions for hypertension in this population of patients. Additional studies are needed to understand the effect of elevated BP among HIV-infected patients treated with HAART on long-term outcomes such as cardiovascular disease. Further studies are needed to examine the role of intermediate variables such as lipoatrophy and lipohypertrophy on the development of elevated BP among HIV-infected patients. Our findings emphasize the importance of monitoring BP among HIV-infected patients receiving HAART. Clinicians may want to consider the impact of cardiovascular disease risk when making treatment decisions particular among patients with additional cardiovascular disease risks.
Among the 444 patients in the study, 95 developed at least one of the BP endpoints and were classified as developing elevated BP. An increase in SBP of 10 mmHg or greater occurred in 83 individuals, 33 individuals developed an increase in DBP of 10 mmHg or greater and 11 had a new diagnosis of hypertension. Although we examined factors associated with the development of an increase in MAP, these results were similar to results obtained for DBP and are not described further
As a class, PI and NNRTI medications were not associated with the development of elevated BP in unadjusted analyses. However, when individual antiretroviral medications were examined, lopinavir/ritonavir was significantly associated with the development of elevated BP (OR, 3.0; 95% CI, 1.6-5.7; P < 0.01). In contrast, patients on atazanavir-based regimens showed a trend toward being less likely to develop elevated BP (OR, 0.3; 95% CI, 0.1-1.1; P = 0.08). Other antiretroviral medications, including ritonavir were not associated with the development of elevated BP in unadjusted analyses.
We hypothesized that the impact of lopinavir/ritonavir on the development of elevated BP was mediated, in part, through an increase in BMI. When change in BMI was added to the multivariate model, increased BMI was significantly associated with developing elevated BP (OR, 1.4; 95% CI, 1.0-1.8; P = 0.02), and the association between lopinavir/ritonavir and BP was no longer present. However, the association between atazanavir and a lower risk of developing elevated BP was present after adjusting for change in BMI (OR, 0.1; 95% CI, 0.01-0.5; P = 0.01).
Patients on atazanavir, efavirenz, nelfinavir, and indinavir had significantly lower adjusted odds of developing elevated BP compared with patients receiving lopinavir/ritonavir (Table 4). These results were similar when change in BMI was included in the model for all medications except for efavirenz, for which the change in risk was no longer statistically significant.
Patients with a CD4+ cell count � 200 cells/μl were significantly more likely to develop elevated BP compared with patients with a CD4+ cell count > 200 cells/μl (OR, 2.0.....Patients with a CD4+ cell count < 50 cells/μl were more than twice as likely to develop elevated BP compared with patients with a CD4+ cell count > 200 cells/μl (OR, 2.4; 95% CI, 1.2-4.8; P = 0.02).
An increase in BMI while receiving HAART was significantly associated with developing elevated BP (OR, 1.3 per kg/m2 increase; 95% CI, 1.1-1.6; P = 0.006). No association was found between the development of elevated BP and baseline HIV-1 RNA level, family history of hypertension, baseline BMI, HIV risk factor, or smoking status."
-----------------
Commentary
Hypertension in HIV patients
De Socio, Giuseppe VLa; Schillaci, Giuseppeb
aUnit of Infectious Diseases, Hospital 'Santa Maria della Misericordia', Perugia, Italy
bUnit of Internal Medicine, Angiology and Arteriosclerosis, University of Perugia, Perugia, Italy.
AIDS 2006
In their interesting article, Crane et al. [1] reported an increase in blood pressure among patients treated with HAART. Systolic blood pressure (SBP) during treatment with HAART, but not diastolic blood pressure, was significantly higher compared with SBP measured before initiating HAART. Among protease inhibitors (PI), lopinavir/ritonavir was associated with the greatest risk of mainly systolic elevations in blood pressure. In this work, the authors did not report specifically whether pulse pressure was different before and after therapy.
Pulse pressure is considered a more sensitive measure of risk than other indexes of blood pressure [2]. Probably, many of the patients reported had an increase in pulse pressure. The increase in SBP and pulse pressure is primarily caused by an increase in large-artery stiffness and an associated increase in wave reflection amplitude. There is increasing evidence that pulse pressure is an independent predictor of the risk of coronary heart disease compared with mean arterial pressure [3]. Recent data suggest that HIV-infected patients under HAART including a PI have higher values of aortic stiffness than a matched group of HIV-uninfected control subjects, and that pulse wave velocity increased with longer exposure to PI treatment [4]. With increased arterial stiffness, central SBP increases and diastolic blood pressure falls in the central arteries as a consequence of earlier wave reflection, which shifts the augmentation of blood pressure from diastole to systole. Augmentation of central pressure is a direct determinant of increased cardiac workload and of diminished myocardial perfusion, and has recently been implicated as a powerful risk factor for cardiovascular events independently of pulse pressure and other risk markers [5].
PI treatment might selectively contribute to increase aortic stiffness. The changes in arterial stiffness may partly mediate the association between the use of PI and cardiovascular risk in patients with HIV infection. Crane et al. [1] reported that increased body mass index was significantly associated with elevated blood pressure in their patients, but do not report whether their patients met the criteria for the metabolic syndrome. We suggest that the metabolic syndrome might represent a link between the use of HAART and arterial stiffness, reflected by a selective increase in SBP and pulse pressure. In our opinion, this would be valuable information, because the metabolic syndrome is both a side-effect of PI [6] and an important determinant of large-artery stiffness [7]. In other words, PI therapy may contribute to increase arterial stiffness and the risk of developing the metabolic syndrome and the associated cardiovascular risk.
--------------------
Antiretroviral medications associated with elevated blood pressure among patients receiving highly active antiretroviral therapy
AIDS April 24 2006
Crane, Heidi Ma; Van Rompaey, Stephen Ea; Kitahata, Mari Ma,b
From the aDepartments of Medicine, University of Washington, Seattle, Washington, USA.
bHealth Services, University of Washington, Seattle, Washington, USA.
Abstract
Objective: To examine the effect of antiretroviral agents and clinical factors on the development of elevated blood pressure (BP).
Methods: Observational cohort study of patients initiating their first HAART regimen. We evaluated mean BP prior to HAART and while receiving HAART in relation to antiretroviral classes and individual agents, and demographic and clinical characteristics including change in body mass index (BMI) while on HAART. We used logistic regression analysis to examine factors associated with elevated BP [� 10 mmHg increase in systolic BP (SBP), diastolic BP (DBP) or new diagnosis of hypertension].
Results: Among 444 patients who had 4592 BP readings, 95 patients developed elevated SBP (n = 83), elevated DBP (n = 33), or a new diagnosis of hypertension (n = 11) after initiating HAART. In multivariate analysis, patients on lopinavir/ritonavir had the highest risk of developing elevated BP [odds ratio (OR), 2.5; P = 0.03] compared with efavirenz-based regimens. When change in BMI was added to the model, increased BMI was significantly associated with elevated BP (OR, 1.3; P = 0.02), and the association between lopinavir/ritonavir and elevated BP was no longer present. Compared with lopinavir/ritonavir-based regimens, patients receiving atazanavir (OR, 0.2; P = 0.03), efavirenz (OR, 0.4; P = 0.02), nelfinavir (OR, 0.3; P = 0.02), or indinavir (OR, 0.3; P = 0.01) had significantly lower odds of developing elevated BP.
Conclusions: Treatment with lopinavir/ritonavir is significantly associated with elevated BP, an effect that appears to be mediated through an increase in BMI. Patients receiving atazanavir were least likely to develop elevated BP. The impact of antiretroviral medications on cardiovascular disease risk factors will increasingly influence treatment decisions.
Introduction
The decline in mortality resulting from widespread use of highly active antiretroviral therapy (HAART) in the developed world has been accompanied by an increase in metabolic complications including dyslipidemia, impaired glucose metabolism, and body morphology abnormalities, which can result in significant morbidity among HIV-infected individuals [1-6]. The increasing prevalence of metabolic complications has raised concerns about the effect of HAART on patients' risk of cardiovascular disease. Hypertension is an important risk factor for cardiovascular disease, but little is known about the impact of HAART on blood pressure (BP).
Previous studies examining the effect of HAART on BP have reported conflicting results [7-12]. One study suggested a lower risk of hypertension among HIV-infected patients receiving protease inhibitors (PIs) compared with HIV-uninfected individuals [13]. Other studies have shown an association between antiretroviral medications, in particular PIs, and the development of elevated BP [12,14,15]. A large cross-sectional study found that non-nucleoside reverse transcriptase inhibitor (NNRTI) or PI use was associated with hypertension, but this association did not persist after adjusting for baseline factors such as age [16]. Little is known about the effect of individual antiretroviral medications on BP. Seaberg and colleagues reported a higher prevalence of systolic hypertension (> 140 mmHg) associated with longer duration of HAART [9]. The investigators did not detect differences in risk of hypertension associated with individual medications but the study was limited by patient self-reported measurement of medication use.
We conducted this study of HIV-infected patients initiating their first HAART regimen to examine the associations between antiretroviral medications and elevated BP.
Methods
Study setting
This study was conducted on the University of Washington (UW) HIV cohort, a longitudinal observational study of HIV-infected patients who receive primary care in the UW Harborview Medical Center HIV clinic from 1 January 1995 to the present. The UW HIV clinic is the largest single provider of medical care to HIV-infected individuals in the northwestern US. Patients provide informed consent and are followed until death or relocation from the UW. To date, 2236 patients have been enrolled into the cohort, contributing over 9000 person-years of follow-up time, with loss to follow-up averaging 10%.
Study participants
All HIV-infected patients 18 years of age or older who were PI and NNRTI naive when they enrolled in primary continuity care and initiated their first HAART regimen between 1 June 1998 and 1 February 2005 were eligible for the study. Subjects were required to have at least 4 months of follow-up after initiating HAART, which was defined as antiretroviral medication regimens containing three or more drugs including either a PI or an NNRTI. In addition, patients had to have at least three BP values before initiating HAART, at least three BP values while on their initial HAART regimen, and no diagnosis of hypertension prior to instituting HAART. Data collection for this study ended 1 June 2005. The study was approved by the UW institutional review board.
Sources of data
The University of Washington HIV information system (UWHIS) captures longitudinal data on the UW HIV cohort and was the source of data for this study. The UWHIS integrates comprehensive clinical data from all outpatient and inpatient encounters including standardized HIV-related information collected at enrollment (initial clinic visit) regarding a patient's prior antiretroviral treatment and diagnosis history. Demographic, clinical, laboratory, medication, and socio-economic data are obtained from the UW electronic medical record and other institutional data sources. The majority of patients in the UW HIV cohort receive all their medications from the on-site pharmacy. Detailed prescription fill/refill data for all outpatient medications and inpatient discharge medications dispensed anywhere in the UW system are obtained directly from the UW pharmacy system. Laboratory data are downloaded directly from the UW laboratory medicine system and include results of all tests performed as part of routine clinical care. Clinician data entry is limited to documenting diagnoses addressed at each clinical encounter from a constrained web-based list of standardized diagnoses. Clinical patient data such as BP, height, and weight are routinely collected and integrated in the UWHIS.
Measurement of blood pressure
BP is measured at all clinic visits by nursing staff using a mercury sphygmomanometer. Although clinic protocol does not require a 5-min seated waiting period before measuring BP as is considered ideal [17], flow through the clinic results in patients being seated on average for at least 5 min before check-in.
Definition of outcomes
We evaluated the change in mean systolic blood pressure (SBP) and diastolic blood pressure (DBP) and mean arterial pressure [MAP = (2 x DBP + SBP)/3] measured prior to initiating HAART and while receiving HAART. A change in mean SBP, DBP, or MAP of at least 10 mmHg was considered clinically significant. We evaluated mean BP measurement during two time periods to decrease the effect of variability of individual BP readings. A new diagnosis of hypertension confirmed by treatment with an antihypertensive medication was an additional end point for analysis. We examined an alteration in any BP endpoint as a combined outcome of elevated BP defined as a 10 mmHg or greater increase in SBP, DBP, or a new diagnosis of hypertension. We then examined each individual BP outcome. There were too few individuals who developed a new diagnosis of hypertension to examine this endpoint individually. We examined the development of isolated SBP (without an elevation in DBP), and an elevation in SBP accompanied by an elevation in DBP. We also examined elevated SBP or a new diagnosis of hypertension, and elevated DBP or a new diagnosis of hypertension. We combined hypertension with elevations in SBP and DBP as an endpoint for analysis in order to examine patients experiencing the full spectrum of BP elevations.
Statistical analysis
We examined the association between development of BP outcomes and demographic characteristics (age, risk factor for HIV transmission, race, sex, family history of hypertension) and clinical characteristics [CD4+ cell count nadir, baseline HIV-1 RNA level, hepatitis C virus (HCV) infection indicated by either presence of HCV antibody or HCV RNA; and body mass index (BMI)]. We examined the association between BP outcomes and antiretroviral medications including individual medications and medication classes [nucleoside (-tide) reverse transcriptase inhibitors (NRTIs), NNRTIs, and PIs]. Antiretroviral medications were categorized into mutually exclusive and exhaustive groups. Patients receiving regimens with two PIs, boosted PI regimens, or regimens with both an NNRTI and a PI were grouped by their non-ritonavir PI. Patients receiving fosamprenavir were grouped with patients taking amprenavir, and patients receiving emtricitabine were grouped with patients taking lamivudine. We examined ritonavir use as a separate variable. We evaluated patients taking any dose of ritonavir together, and also categorized patients as either receiving full dose ritonavir (greater than 400 mg per 24-h period) or a boosting dose of ritonavir (400 mg or less per 24-h period). We calculated BMI using the traditional Quetelet index: weight divided by height squared (kg/m2) [18]. Baseline BMI was categorized as underweight (< 18.5 kg/m2), normal (18.5-24.9 kg/m2), overweight (25-29.9 kg/m2), and obese (� 30 kg/m2). Change in BMI was measured as the difference between BMI prior to receiving HAART, and the BMI at the final visit while receiving the initial HAART regimen or at the end of the study period, whichever came first.
We performed bivariate analysis of associations with development of BP outcomes using chi-squared tests for categorical variables and t-tests for continuous variables. We used multivariate logistic regression to examine independent predictors of the development of BP outcomes. Efavirenz and lopinavir/ritonavir were used in separate models as reference categories to examine the effects of individual PIs and NNRTIs on outcomes. NRTIs were never administered singly and so were examined as pairs. Effect modification was assessed with the use of interaction terms. We hypothesized that the effect of antiretroviral medications on development of BP outcomes was mediated, in part, through a change in BMI and tested this hypothesis by examining the effect of BMI on model results. Two-tailed P values of < 0.05 were considered significant for all statistical tests.
Results
Study entry criteria were met by 444 patients who had a total of 4592 BP readings. Mean age of study patients at first visit was 35 years, 84% were men, mean CD4+ cell count was 163 cells/μl, and 53% had a peak viral load > 100 000 copies/ml (Table 1). Mean BMI for the study cohort was 24.1 kg/m2 prior to initiation of HAART. At baseline, 7% of patients were underweight, 56% had a normal BMI, 27% were overweight, and 10% were obese.
Initial HAART regimens were evenly divided between patients receiving PI- (n = 239, 54%) and NNRTI-based regimens (n = 237, 53%); 32 patients (7%) received both a PI and an NNRTI (Table 2). A few patients received regimens containing two full dose PIs, (ritonavir combined with saquinavir, n = 17, 4%), or regimens with boosted PIs (lopinavir/ritonavir, n = 47, 11%; atazanavir with ritonavir, n = 18, 4%; amprenavir with ritonavir, n = 4, 1%). Study patients were on their initial HAART regimen for a mean of 13.5 months. Duration of initial HAART regimen did not differ by sex, race, HIV transmission risk factor, or HCV status.
The mean SBP measured among the study cohort during treatment with HAART was significantly higher compared with the mean SBP measured prior to initiating HAART (124.6 versus 121.6 mmHg; P � 0.001). The mean DBP during treatment with HAART and prior to initiating HAART were similar (74.1 versus 73.7 mmHg; P = 0.5). Mean SBP was significantly lower among women compared with men, both prior to initiating HAART (116.1 versus 122.4 mmHg; P = 0.004) and during treatment with HAART (118.9 versus 124.6 mmHg; P = 0.006). No statistically significant differences were observed in BP values based on risk factor for HIV acquisition, self-reported racial group, or HCV status.
Among the 444 patients in the study, 95 developed at least one of the BP endpoints and were classified as developing elevated BP. An increase in SBP of 10 mmHg or greater occurred in 83 individuals, 33 individuals developed an increase in DBP of 10 mmHg or greater and 11 had a new diagnosis of hypertension. Although we examined factors associated with the development of an increase in MAP, these results were similar to results obtained for DBP and are not described further.
In unadjusted analyses, age over 40 was significantly associated with development of the combined endpoint of elevated BP [odds ratio (OR), 1.7; 95% confidence interval (CI), 1.0-2.8; P = 0.05]. African-Americans tended to be more likely than whites to develop elevated BP (OR, 1.6; 95% CI, 0.9-2.6; P = 0.09). Patients with a CD4+ cell count � 200 cells/μl were significantly more likely to develop elevated BP compared with patients with a CD4+ cell count > 200 cells/μl (OR, 2.0; 95% CI, 1.2-3.3; P = 0.009). The mean BMI prior to initiating HAART in study subjects with a CD4+ cell count < 50 cells/μl was nearly 2 kg/m2 lower than those with a CD4+ cell count � 50 cells/μl (23.0 versus 24.8; P = 0.003). BMI measurements were available for 380 study patients (86%). An increase in BMI while receiving HAART was significantly associated with developing elevated BP (OR, 1.3 per kg/m2 increase; 95% CI, 1.1-1.6; P = 0.006). No association was found between the development of elevated BP and baseline HIV-1 RNA level, family history of hypertension, baseline BMI, HIV risk factor, or smoking status.
Duration of initial antiretroviral regimen was shorter among patients on atazanavir-based regimens (P = 0.01) compared with those on efavirenz-based regimens. Patients on amprenavir-based regimens had the largest increase in BMI while on their initial HAART regimen (1.1 kg/m2) compared with patients on efavirenz (0.5 kg/m2), but this difference was not statistically significant. Patients on lopinavir/ritonavir were more likely to be older (37 versus 35 years; P = 0.05). Use of other antiretroviral medications did not differ by age, race, sex, duration of initial HAART regimen, change in BMI, hepatitis C status, or CD4+ cell count.
As a class, PI and NNRTI medications were not associated with the development of elevated BP in unadjusted analyses. However, when individual antiretroviral medications were examined, lopinavir/ritonavir was significantly associated with the development of elevated BP (OR, 3.0; 95% CI, 1.6-5.7; P < 0.01). In contrast, patients on atazanavir-based regimens showed a trend toward being less likely to develop elevated BP (OR, 0.3; 95% CI, 0.1-1.1; P = 0.08). Other antiretroviral medications, including ritonavir were not associated with the development of elevated BP in unadjusted analyses.
In multivariate analyses adjusting for age, race, sex, HCV status, and duration of initial HAART regimen (Table 3), patients receiving lopinavir/ritonavir-based regimens were more than twice as likely to develop elevated BP compared with patients on an efavirenz-based regimen (OR, 2.5; 95% CI, 1.1-5.7; P = 0.03), and patients receiving atazanavir-based regimens were less than half as likely to develop elevated BP, although this result was not statistically significant (OR, 0.4; 95% CI, 0.08-1.7; P = 0.2). Patients with a CD4+ cell count < 50 cells/μl were more than twice as likely to develop elevated BP compared with patients with a CD4+ cell count > 200 cells/μl (OR, 2.4; 95% CI, 1.2-4.8; P = 0.02). No effect modification was found when interactions between individual antiretroviral medications and CD4+ cell count, age, race, or sex were included in the model. We hypothesized that the impact of lopinavir/ritonavir on the development of elevated BP was mediated, in part, through an increase in BMI. When change in BMI was added to the multivariate model, increased BMI was significantly associated with developing elevated BP (OR, 1.4; 95% CI, 1.0-1.8; P = 0.02), and the association between lopinavir/ritonavir and BP was no longer present. However, the association between atazanavir and a lower risk of developing elevated BP was present after adjusting for change in BMI (OR, 0.1; 95% CI, 0.01-0.5; P = 0.01).
Patients receiving lopinavir/ritonavir were more than twice as likely to develop an elevation in SBP or a new diagnosis of hypertension (OR, 2.4; 95% CI, 1.0-5.6; P = 0.04) (Table 3). We compared the risk of developing elevations in SBP not accompanied by elevations in DBP with the risk of developing elevations in both SBP and DBP in fully adjusted models. Lopinavir/ritonavir was associated with over three times the risk of developing an isolated elevation in SBP (OR, 3.3; 95% CI, 1.3-8.5; P = 0.01), and not with an elevation in both SBP and DBP. A low CD4+ cell count was associated with over four times the risk of developing an elevation in both SBP and DBP (OR, 4.7; 95% CI, 1.6-14.1; P = 0.005).
Patients on atazanavir, efavirenz, nelfinavir, and indinavir had significantly lower adjusted odds of developing elevated BP compared with patients receiving lopinavir/ritonavir (Table 4). These results were similar when change in BMI was included in the model for all medications except for efavirenz, for which the change in risk was no longer statistically significant.
Patients who developed elevated BP were less likely to have received zidovudine (OR, 0.5; 95% CI, 0.3-0.8; P = 0.007), and more likely to have received tenofovir (OR, 1.9; 95% CI, 1.1-3.2; P = 0.02) in unadjusted analyses. We did not find an effect of other NRTIs on elevated BP. When we included NRTIs in the adjusted model, we found that tenofovir/lamivudine (n = 67) was associated with an increased risk of developing elevated BP (OR, 2.3; 95% CI, 1.0-5.2; P = 0.046) compared with zidovudine/lamivudine (n = 145) controlling for individual PIs, NNRTIs, race, sex, age, CD4+ cell count, duration of HAART regimen, and HCV infection. No significant effect was seen for the combination of stavudine/lamivudine (n = 142). When the change in BMI during HAART was also included, the association between tenofovir/lamivudine and the development of elevated BP was no longer significant (OR, 1.8; 95% CI, 0.6-5.6; P = 0.3).
Discussion
We found a two-fold increase in the risk of developing elevated BP among patients receiving lopinavir/ritonavir compared with those receiving efavirenz-based regimens. In addition, our results suggest that the increased risk associated with lopinavir/ritonavir was mediated, at least in part, through an increase in BMI. In contrast, patients receiving atazanavir-based regimens had a lower risk of developing elevated BP compared with patients receiving efavirenz or lopinavir/ritonavir even after adjusting for change in BMI. Regimens containing tenofovir/lamivudine were associated with an increased risk of developing elevated BP compared with those containing zidovudine/lamivudine controlling for other drugs in the regimen. We also found that patients with lower CD4+ cell counts were significantly more likely to develop an elevated BP while on HAART.
Antiretroviral medications
We did not find an association between development of elevated BP and treatment with PIs or NNRTIs as a class. The impact of NRTIs as a class could not be examined since all patients received NRTIs as part of their HAART regimen. Among PIs, lopinavir/ritonavir was associated with the greatest risk of mainly systolic elevations in BP. Systolic hypertension is an important predictor of cardiovascular disease in the general population [17,19], which raises concern about cardiovascular disease risk among patients receiving lopinavir/ritonavir. We did not find an association of ritonavir with the development of elevated BP in unadjusted analyses or adjusted models suggesting the increased risk associated with lopinavir/ritonavir could be attributed to lopinavir. There were too few patients treated with amprenavir to fully examine its relationship to elevated BP. However, all patients treated with amprenavir developed elevated BP as well as a substantial increase in BMI. The effect of amprenavir appeared to be predominantly on DBP, a well-known cardiovascular risk factor [20]. Although we did not find a significant risk of elevated BP for all patients treated with indinavir, a subset of patients receiving indinavir who did develop an elevated BP had the largest increase in BP among the cohort (> 40 mmHg increase in SBP while on HAART). One possible explanation for these findings is that large elevations in BP among a subset of patients receiving indinavir may represent secondary hypertension via a renal pathway. Taken together, our results suggest that specific PIs affect BP through different mechanisms. Additional studies will be needed to clarify the extent individual PIs impact BP via different mechanisms such as changes in BMI and renal affects.
Zidovudine monotherapy has been reported to be associated with a reduced hypertension risk among women [21]. In our study, patients receiving tenofovir and lamivudine were more likely to develop elevated BP than patients receiving zidovudine and lamivudine. It is not possible to determine whether this was due to a decreased risk among those receiving zidovudine, or increased risk among those receiving tenofovir, or a combination of both effects. Tenofovir has been associated with a decline in renal function [22] that could lead to elevations in BP. Our results suggest that the increase in risk associated with tenofovir was mediated through a change in BMI.
Clinical and demographic characteristics
Previous studies have not found an association between HIV RNA level, or CD4+ cell count, and hypertension [10,11,21]. In our study, lower CD4+ cell count was an independent predictor of developing elevated BP after adjusting for age and other factors, and this effect appeared to be mediated through a change in BMI. Patients with a low CD4+ cell count are more likely to have experienced wasting prior to initiating HAART, which would result in their having a greater change (increase) in BMI after treatment with HAART and yet have a low absolute BMI.
This is supported by our finding that patients with a CD4+ cell count < 50 cells/μl had a lower BMI prior to initiating HAART than those with a higher CD4+ cell count. Sex and African-American race are associated with hypertension in the general population [23,24]. Prior studies have found conflicting effects of demographic characteristics on hypertension among HIV-infected patients [7,10,16]. We found higher SBP among HIV-infected men compared with women before and after initiation of HAART, and a trend toward an increased risk of elevated BP among African-Americans.
Strengths and limitations
The strengths of our study include long-term follow-up, comprehensive clinical data, and precise and accurate antiretroviral treatment data from the UW HIV Cohort captured in the UWHIS. We defined our outcome based on change in BP rather than using an arbitrary cut-off value such as 140/90 mmHg. Studies conducted over the past 20 years, in numerous patient populations, have demonstrated a continuous relationship between elevations in SBP and DBP and cardiovascular disease and death, and that this association is not driven by a particular cut-off value [20]. Our findings are generalizable to similar populations of patients in routine care who represent a broader range of characteristics than patients who enroll in clinical trials. As the cohort continues to be followed, additional information will become available on newer antiretroviral agents.
As with any observational study, there is the concern for unknown or unmeasured confounding factors for which adjustment is not possible. However, potential confounding is minimized in our study by comparing changes over time within individuals rather than examining study patients in relation to control patients. Measurement of BP in the clinical care setting may not be conducted in a uniform manner. We limited the impact of random measurement error by using the average of at least three BP readings before and after HAART treatment. However, the use of average BP does not allow us to assess the length of time on therapy necessary for a patient to develop an elevation in BP. Finally, information regarding other potential risk factors for hypertension such as genetic factors, physical activity, diet, and daily alcohol and tobacco consumption were not available.
Conclusions
A clear understanding of factors contributing to the development of elevated BP among HIV-infected patients is needed to target prevention efforts and help guide research that may lead to improved interventions for hypertension in this population of patients. Additional studies are needed to understand the effect of elevated BP among HIV-infected patients treated with HAART on long-term outcomes such as cardiovascular disease. Further studies are needed to examine the role of intermediate variables such as lipoatrophy and lipohypertrophy on the development of elevated BP among HIV-infected patients. Our findings emphasize the importance of monitoring BP among HIV-infected patients receiving HAART. Clinicians may want to consider the impact of cardiovascular disease risk when making treatment decisions particular among patients with additional cardiovascular disease risks.
|
|
| |
| |
|
|
|