| |
Treat chronic hepatitis C virus infection in decompensated cirrhosis - pre- or post-liver transplantation? the ironic conundrum in the era of effective and well-tolerated therapy Review
|
| |
| |
Download the PDF here
JNL of Viral hepatitis March 28 2016
C. Bunchorntavakul1 and K. Rajender Reddy2 1Division of Gastroenterology and Hepatology, Department of Internal
Medicine, Rajavithi Hospital, College of Medicine, Rangsit University, Bangkok, Thailand; and 2Division of Gastroenterology and Hepatology,
University of Pennsylvania, Philadelphia, PA, USA
Summary
The management of hepatitis C virus (HCV) infection in patients with decompensated cirrhosis has evolved dramatically over the past few years mainly due to the availability of all-oral antiviral regimens. The currently approved all-oral direct-acting antivirals (DAA) containing sofosbuvir, ledipasvir, daclatasvir and ribavirin, in various combinations, have shown to be safe and effective in patients with decompensated cirrhosis with sustained virological response (SVR) rates nearly comparable to those with well-compensated liver disease. Unique issues yet remain such as the challenges with renal insufficiency, tolerability of ribavirin and risk of further hepatic decompensation with a protease inhibitor-based regimen. While most patients who achieve SVR have demonstrated improvement in hepatic synthetic function over the short course of follow, the long-term beneficial effects are unknown. Further, the baseline predictors of improvement in hepatic function have not been well delineated and thus have left us in a quandary as to what we might expect with successful therapy and thus we are at a loss to well educate our patients.
The major concern, in potential liver transplant candidates, is of unintended 'harm' by achieving SVR but without improvement in hepatic function to an extent where the patients might function well. As HCV therapies are as effective in liver transplant recipients, there is a growing sentiment in some of the transplant quarters that those with decompensated liver disease and awaiting liver transplant be treated for HCV after liver transplant. This strategy would thus eliminate any concern of leaving a patient in 'no person's' land by treating HCV successfully pretransplant but not to the point of functional normalcy, while also would maintain the risk of HCC. Yet a contrarian view would be that not all patients have access to liver transplantation (LT), cannot bear the cost, have comorbidities or contraindications to LT. While the debate continues, it is essential that we develop robust predictors of improvement in liver function so that we can carefully select our patients for therapy in the context of liver transplantation.
Abbreviations
CTP
Child-Turcotte-Pugh
DAA
direct-acting antivirals
DDI
drug-drug interactions
EASL
European Association for the Study of the Liver
HCV
hepatitis C virus
IDSA
Infectious Diseases Society of America
LT
liver transplantation
RBV
Ribavirin
SVR
Sustained virological response
Introduction
In the Western World and in Japan, chronic hepatitis C virus (HCV) infection-related advanced liver disease is the most common indication for liver transplantation (LT). Despite advances in screening strategies and effective antiviral therapy, it is projected that HCV and its complications will continue to rise over the next decade or more [1-3]. The management of HCV in patients with decompensated cirrhosis and those who had a LT had been challenging in the era of interferon-based therapy due to significantly reduced treatment efficacy and increased treatment-related side effects. However, the treatment paradigm for this population has changed dramatically after the introduction of direct-acting antivirals (DAA) targeting NS3/4A, NS5A and NS5B HCV proteins. With the availability of new DAAs, treatment of HCV in patients with decompensated cirrhosis and in LT recipients is feasible with high success rates, even in those who previously failed IFN-based therapy, while there are trivial side effects and drug-drug interactions (DDI) [4, 5]. It is somewhat ironic that we had yearned for effective and well-tolerated regimens and now have entered into a debate of whether to treat HCV before or after liver transplantation.
Natural history of HCV before and after LT
Chronic HCV infection is often a slowly progressive disease leading to the development of cirrhosis in 10-40% of patients over 20-30 years of infection [6]. Once cirrhosis has developed, the disease progression remains unpredictable with an overall 1-5% annual risk of HCC and 3-6% annual risk of hepatic decompensation [6]. Following an episode of decompensation, the risk of death in the following year is approximately 15-20%, and LT generally remains the only life-saving option [5].
Following LT, graft and patient survival are significantly reduced in HCV-positive recipients compared to HCV-negative recipients, a difference mainly accounted for by recurrence of HCV infection in the graft [7, 8]. HCV infection recurrence is universal in patients with detectable HCV-RNA at the time of LT although its severity depends on several factors [5, 8]. Typically, the liver graft is re-infected upon reperfusion and is accompanied by a rise in HCV-RNA that peaks around 3-4 months, together with phenotype of acute hepatitis in most patients [8]. Although serum transaminases and HCV-RNA generally settle down to normal or near-normal range, spontaneous viral clearance has not been observed and HCV-RNA levels are often elevated to around 10-fold to 20-fold higher than pre-LT levels by the end of the first year [5, 8].
The natural course of hepatitis C is significantly accelerated in LT recipients when compared to non-LT setting, with more than 40% progressing to cirrhosis within 10 years and approximately 50% developing liver failure shortly thereafter [5, 9, 10]. It should be noted that a subset of patients (2-9%) may develop post-LT cholestatic hepatitis C, which is characterized by persistent cholestasis of at least 4 weeks in duration, high HCV-RNA, hepatocyte ballooning, and rapid progression to graft failure in the absence of biliary and hepatic artery complications, sepsis and drug-related cholestasis [11]. The impact of immunosuppressive therapy on the natural history of recurrent HCV has not been well elucidated, although there has been evidence to suggest a neutral or small beneficial effect of cyclosporine, mycophenolate mofetil and sirolimus [8-10].
Evolving epidemiology and concerns of HCV and liver transplantation
HCV infection is currently the most common indication for LT in the United States, Japan and many countries in Europe. Based on the US database (the Organ Procurement and Transplantation Network), among 126 862 new primary registrants for LT between 1995 and 2010, 41% had HCV [12]. Although effective therapies are currently available and the prevalence of HCV has already peaked and is now declining, it is predicted that the number of cases of advanced cirrhosis, HCC and liver-related deaths will continue to rise through 2030, worldwide [13]. In addition, there is a projected increase in the incidence of HCC, in HCV-positive LT candidates, particularly in those with advancing age, which will further challenge the transplant community [12].
Before the era of DAA, LT for HCV-positive recipients was often associated with poorer outcomes, with significantly increased rate of death (HR 1.23; 95% CI: 1.12-1.35) and allograft failure (HR 1.30; 95% CI: 1.21-1.39) when compared to LT for other indications [7]. This was largely due to recurrent and aggressive course of HCV after liver transplant, and unfortunately suboptimal sustained virological response (SVR) rates (24-40%) and high side effects, associated with IFN-based therapy for recurrent HCV [10, 14, 15]. However, in the era of DAA, various regimens of all-oral DAA have demonstrated to cure recurrent HCV in >85% of all LT recipients, and probably higher if treated before advanced fibrosis has developed [16-21]. Therefore, at the present time, the outcomes of LT for HCV-positive recipients are expected to be similar, or even better, than LT for other indications, akin to the experience we have learned from LT for hepatitis B cirrhosis [22].
Pharmacologic properties of DAA in patients with cirrhosis and liver transplantation
Since 2011, several DAA have been approved for the treatment of HCV worldwide, with three mechanisms of actions (NS3/4A protease inhibitors, NS5A inhibitors and NS5B polymerase inhibitors) and a spectrum in efficacy, viral resistance and pharmacokinetic profile. (Table 1) With the exception for sofosbuvir, which is excreted by the kidneys, almost all DAA are metabolized by the liver and thus their metabolism may be altered in patients with significant hepatic impairment. The pharmacokinetics of sofosbuvir and daclatasvir do not appear to change significantly in patients with moderate or severe liver impairment and therefore can be used in patients with decompensated cirrhosis without the need of dose adjustment. [23-25] A fixed-dose combination of paritaprevir/ritonavir/ombitasvir plus dasabuvir and RBV appears to be safe in patients with compensated cirrhosis, but should not be used in decompensated patients due to the risk of developing further hepatic impairment. Similarly, simeprevir is not recommended in Child-Turcotte-Pugh (CTP) class B and C cirrhosis [23-25]. A fixed-dose combination of grazoprevir/elbasvir is not recommended in patients with CTP class B and C cirrhosis due to the significantly increased grazoprevir plasma concentration and the increased risk of transaminitis [26]. Ribavirin (RBV) has extensive volume of distribution and is eliminated mainly through the kidneys [27]. Its concentration is not significantly altered in patients with cirrhosis. However, the incidence and severity of RBV-induced anaemia appears to be increased in patients with cirrhosis due to multiple factors such as baseline hypersplenism-related anaemia, decreased production of erythropoietin, blunt bone marrow response, nutritional deficiency and occult gastrointestinal blood loss [27]. Therefore, the use of RBV-containing DAA regimens in cirrhosis needs careful monitoring of anaemia and, in those with decompensated cirrhosis, it is suggested to start with lower doses (e.g. 600 mg/day) and gradually adjusted to full dose of 1000-1200 mg/day based on haemoglobin and creatinine levels [16, 18, 28].
Drug-drug interactions between DAA and immunosuppressive agents were a concern with the use of first-generation DAAs, such as boceprevir and telaprevir [5]. However, treatment of HCV in LT recipients is now feasible with newer generation DAA and with low potential for drug-drug interactions [5, 23, 25]. Dose adjustments of tacrolimus or cyclosporine are not required when co-administered with sofosbuvir, ledipasvir, daclatasvir and RBV. Ritonavir is a strong CYP3A inhibitor and the dose of calcineurin inhibitors must be adjusted when co-administered with ritonavir-boosted DAA regimen [21, 25]. It should be noted that concomitant use of simeprevir with calcineurin inhibitors does not significantly affect the levels of calcineurin inhibitors, but results in an increase in plasma concentrations of simeprevir (approximately twofold with tacrolimus and sixfold with cyclosporine), and therefore, co-administration of simeprevir with cyclosporine is not recommended [23]. Co-administration of grazoprevir/elbasvir and tacrolimus did not affect grazoprevir or elbasvir exposures, but resulted in about 40% increase in tacrolimus exposure, and therefore, frequent monitoring of tacrolimus levels is recommended if this DAA combination is used [29]. However, co-administration of grazoprevir/elbasvir with cyclosporine is not recommended due to a significant increase in grazoprevir plasma concentration (about 15-fold) [29] (Table 1).
Treatment of HCV in patients with decompensated cirrhosis
Efficacy of the available treatment regimens
Treatment of HCV is strongly recommended for patients with advanced fibrosis and compensated cirrhosis as an SVR in this high-risk group has been shown to decrease the risk of progressive fibrosis and even regressed fibrosis in some cases, thus decreasing the incidence of hepatic complications. Additionally, successful HCV therapy is associated with a decreased incidence of HCC, although the risk is not eliminated [6, 30-32]. In addition, successful viral eradication in those with decompensated liver disease independently reduces portal hypertension, decreases clinical decompensation and improves survival, which may further facilitate, delay, or, in a small proportion of patients, avoid LT, as well as prevent HCV recurrence following LT. [30, 31, 33] In the era of IFN-based therapies, the treatment outcomes in patients with decompensated cirrhosis had been disappointing due to low efficacy (SVR 7-30% for genotype 1, and 44-57% for genotype 2/3) and high rates of treatment-related side effects (led to dose reduction in 40-70% and treatment discontinuation in 13-40%) [15, 20]. Therefore, IFN-based therapies, including DAA plus PEG-IFN and RBV, should not be used in patients with decompensated liver disease, particularly if their CTP score is >7 or MELD score >18 [5, 10, 34].
Over the past few years, several all-oral DAA regimens have been evaluated in patients with decompensated cirrhosis and with promising outcomes in terms of safety and efficacy in Phase II/III and real-world studies. (Table 2) Accordingly, the American Association for the Study of Liver Diseases (AASLD) and Infectious Diseases Society of America (IDSA), and the European Association for the Study of the Liver (EASL) guidelines recommend that in those with decompensated cirrhosis, all-oral DAA regimens containing sofosbuvir, ledipasvir, daclatasvir and RBV, according to the HCV genotypes, can be used [23, 25]. (Table 3) These recommended all-oral combination regimens are generally associated with SVR rates similar or slightly lower to that of patients without decompensated cirrhosis [23-25]. The multicenter Phase III ALLY-1 study evaluated a 12-week course of daclatasvir 60 mg daily, sofosbuvir 400 mg daily and RBV (initially 600 mg/day, adjusted to 1000 mg/day based on haemoglobin levels) in HCV genotype 1-6 patients (about 70% were genotype 1) with advanced cirrhosis (n = 60) or had post-LT HCV recurrence (n = 53) [18]. In advanced cirrhosis cohort, SVR was achieved in 92%, 94% and 56% of patients with CTP-A (n = 12), CTP-B (n = 32) and CTP-C (n = 16), respectively [18]. Most patients improved their MELD scores following treatment. In post-LT cohort, SVR was achieved in 92% of patients without the need for dose modification of immunosuppressive agents. Among those with genotype 3 (n = 17), SVR rate was 83% in those with advanced cirrhosis and 91% in the post-LT cohort [18]. The regimen was well tolerated, with few treatment-unrelated serious adverse events.
In SOLAR-1 study, 108 treatment-naive and treatment-experienced patients with HCV genotypes 1 and 4 who had decompensated cirrhosis (59 had CTP-B and 49 had CTP-C) were randomized to receive daily fixed-dose combination sofosbuvir/ledipasvir and RBV (initial dose of 600 mg, increased as tolerated) for 12 or 24 weeks [16]. SVR was achieved in 87% and 89% of patients treated for 12 and 24 weeks, respectively. Majority of patients improved their CTP and MELD scores following treatment. Five patients died during the study, and none were attributed to antiviral treatment. Grade 3 or 4 side effects developed more commonly in the 24-week arm (34%) than in the 12-week arm (15%) [16]. In a preliminarily report of SOLAR-2 study, a fixed-dose combination sofosbuvir/ledipasvir and RBV for 12-24 weeks was associated with SVR rates of 87-96% and 72-85% in HCV genotype 1 patients with cirrhosis CTP-B (n = 46) and CTP-C (n = 38), respectively [17]. An integrated safety analysis of sofosbuvir/ledipasvir and RBV among >600 patients in the SOLAR studies demonstrated that the regimen was safe and well tolerated [35]. Severe adverse events (28-30%) and death (5%) were consistent with anticipated liver disease progression, and there was no additional treatment-related morbidity and mortality, apart from RBV-induced anaemia [35].
In addition, a report from the NHS England Early Access Program has confirmed the efficacy of a 12-week course of sofosbuvir plus a NS5A inhibitor, either ledipasvir or daclatasvir, with or without RBV for HCV genotype 1 or 3 in over 400 patients with decompensated cirrhosis [36]. The administration of sofosbuvir plus RBV before LT has also been noted to prevent post-LT HCV recurrence in an open-label study of 61 patients with CTP-A and HCV of any genotype who were on wait lists for LT for hepatocellular carcinoma [37]. The interim analyses of the French[38] and European[39] Multicenter Compassionate Use Programs reported that 12- to 24-week adminstration of sofosbuvir plus daclatasvir, with or without RBV, was safe and resulted in high SVR rates in cirrhotic patients with HCV genotype 3 (SVR12 89-94% in CTP-A and 70-82% in CTP-B/C patients).
The Phase II IMPACT study evaluated the combination of simeprevir, sofosbuvir and daclatasvir for 12 weeks in 40 HCV patients with genotype 1 or 4 and cirrhosis (19 CTP-A and 21 CTP-B) [40]. The SVR rate was 100% without serious adverse events (although simeprevir is not recommended for decompensated cirrhosis) [40]. In a retrospective experience of sofosbuvir plus simeprevir with or without RBV for HCV genotype 1 patients with cirrhosis (30% CTP-B), treatment was very well tolerated and SVR was achieved in 78% of patients [41]. In a retrospective cohort of 160 cirrhotic patients with HCV genotype 1 treated with sofosbuvir and simeprevir, with or without RBV, for 12 weeks, SVR was achieved in 73% of patients with CTP-B/C vs 91% of those with CTP-A (P < 0.01). Patients with cirrhosis CTP-B/C had more early treatment discontinuations (11% vs 1%), adverse events requiring hospitalization (22% vs 2%), and hepatic decompensating events (20% vs 3%), when compared to those with CTP-A (all P < 0.01) [42].
The multicenter Phase III ASTRAL-4 study evaluated a fixed-dose combination of a pangenotype regimen of sofosbuvir and velpatasvir once daily in three different regimens in 267 patients with HCV genotypes 1-6 (78% were genotype 1) and CTP-B cirrhosis. Overall, SVR rates were 83% among patients who received 12 weeks of sofosbuvir-velpatasvir, 94% among those who received 12 weeks of sofosbuvir-velpatasvir plus ribavirin, and 86% among those who received 24 weeks of sofosbuvir-velpatasvir [28]. The most common side effects in all groups were fatigue (29%), nausea (23%) and headache (22%), although anaemia, diarrhoea and insomnia were more common among the patients who received sofosbuvir-velpatasvir plus ribavirin [28]. A preliminary Phase II/III C-SALT study revealed that grazoprevir 50 mg/day plus elbasvir 50 mg/day for 12 weeks was well tolerated and highly effective (SVR 90%) in 30 patients with CTP-B cirrhosis and HCV genotype 1 [26]. In a pharmacokinetic study, grazoprevir exposure was slightly higher in patients with CTP-B cirrhosis receiving 50 mg dose compared to noncirrhotic patients receiving 100 mg dose, whereas the pharmacokinetics of elbasvir (50 mg) was similar in both populations [26].
Effects on liver function following treatment and predictors of virological response
Taken together the data from major clinical trials in HCV patients with decompensated cirrhosis (801 patients with 83.5% SVR rates), it is quite clear that successful antiviral therapy significantly improved liver function as determined by MELD and CTP scores in the majority of patients: 60% had an improvement in MELD score from baseline, 17% had no change, and 23% had a worsening in the MELD score [16-18, 26, 28, 36, 40]. (Table 4) The magnitude of improvement in MELD scores varied highly with a median of 2 points (range 1-17 points); 34% had ≥4 point improvement. [16-18, 26, 28, 36, 40] These beneficial effects from the treatment may potentially benefit individual LT candidates by removing them from wait list and also may have a substantial impact on the national waiting list and organ availability [43]. For example, of the 250 decompensated patients who achieved SVR in the SOLAR studies, 60% had an improvement in MELD scores from baseline to post-treatment week 12, and 61% (41/67) with baseline MELD ≥15 had a post-treatment week 12 MELD improvement to <15 [44]. As more and more data emerge, it should be noted that the long-term follow-up data on course of hepatic function more than 6 months after treatment are currently limited. Further, available data in patients with more advanced liver disease (CTP score >12 or MELD score >20), so-called end-stage liver disease, are also limited, partly because this highly vulnerable population were often precluded or enrolled in relatively small numbers in the aforementioned clinical trials. Thus, we should be aware that these estimates of SVR and improvement in MELD or CTP score may have limitations in those patients with high MELD scores and/or CTP-C liver disease.
Of interest and of some concern, during the short course of follow-up, is that a smaller proportion of patients with decompensated cirrhosis had no improvement or continued to show further increases in MELD score following successful treatment, indicating that there may be a point of no return for recovery in hepatic function in those who present with quite advanced liver disease. The magnitude of progressive worsening in MELD scores following successful treatment has varied with a median of 1 point (range 1-13 points); 54% had +1 and 28% had +2 increase in MELD scores [16-18, 26, 28, 36, 40]. Unfortunately, to date, there have been no reliable predictors of virological response and liver function outcomes following antiviral therapy in patients with decompensated cirrhosis. A subanalysis of the NHS Early Access Program suggested that hepatic function is more likely to improve among patients younger than 65 years if the albumin was more than 3.5 g/dL [36]. A retrospective Australian Compassionate Use Program (TOSCAR Study) used sofosbuvir plus daclatasvir (without RBV) for 24 weeks in 92 patients with decompensated cirrhosis and MELD ≥15 and reported that hepatic functions improvement after therapy was limited to those with baseline MELD scores <20, suggesting that this is perhaps the point of no return for improvement [45]. Further analyses of Phase II/III studies in those with advanced liver disease are needed to identify robust and reliable clinical predictors of favourable outcomes after SVR, while a long-term follow-up study (up to 5 years) evaluating the durability of SVR and the progression or regression of liver disease after successful treatment is currently ongoing (NCT01457755).
Controversies in treatment of patients with decompensated cirrhosis prior to LT
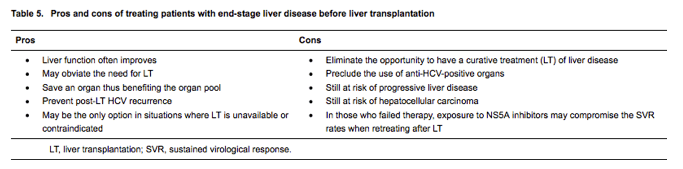
The decision to treat HCV in patients with decompensated cirrhosis to maximize survival should be individualized, together with a consideration of the expected waiting time to LT and the organ pool in each region. It is debatable whether those with decompensated cirrhosis with MELD >20 should be treated before LT with aim to cure and achieve functional improvement, or to prevent post-LT recurrence, or should such patients be monitored until LT, and treatment initiated at the time of established recurrence of HCV [25]. There are several pros and cons to be considered when deciding on HCV therapy in the peri-transplant population. [Table 5] In the situation where there are challenges with access to LT or LT is contraindicated, HCV treatment would be recommended for all patients with decompensated cirrhosis with the hope and expectation that there would be functional and quality-of-life improvement and prolonged survival. However, if LT was accessible, the decision of HCV treatment is more complicated and the cons of treating patients with decompensated cirrhosis should be taken into consideration and an informed decision should be made, while intuitively and ethically it would seem that treating an infectious disease pre-transplant would be the wise choice. (Fig. 1)
Although the currently available treatment regimens for patients with decompensated cirrhosis are associated with high SVR rates, there are still lower than that of treating early HCV recurrence after LT. For those who fail antiviral therapy before LT, the occurrence of resistance-associated variants, especially for NS5A, may compromise the SVR when retreating after LT. Further, in such cases of NS5A resistance, protease inhibitors may be challenging in LT recipients due to drug-drug interaction with calcineurin inhibitors, thus providing fewer options of antiviral regimens for such patients. It should also be noted that even with successful therapy, the risk of progressive liver disease and hepatocellular carcinoma is not eliminated, and the chance of facilitating a LT in such patients may be further delayed due to the improvement in their MELD scores and may preclude them from receiving anti-HCV-positive organs. It appears that the Hepatology community is at the crossroads of a challenging dilemma. While we yearned for years for effective, safe and well-tolerated HCV therapies, we have now created a conundrum on timing of HCV therapy. There is an urgent need to identify predictors of clinical response after successful HCV therapy and long-term outcomes for the Hepatology community to well inform our patients on what might be the expectations with treatment and whether it is wise to wait till after transplant to treat them. The debate, though, may only be applicable to a small group of liver transplant eligible patients while the majority of patients around the World with decompensated liver disease would be ideal candidates for successful therapy with the expectation of improved hepatic function and longer survival.
|
|
| |
| |
|
|
|