| |
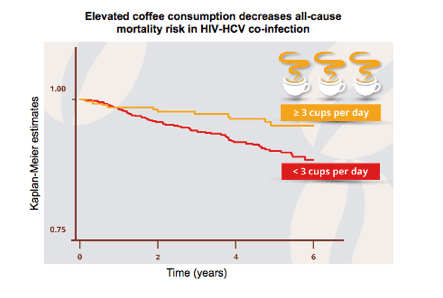
≥3 cups/day of coffee per day halves
all-cause mortality risk in patients co-infected with HIV-HCV...
|
| |
| |
Download the PDF
The benefits of coffee extracts and supplementing dietary intake with other anti-inflammatory compounds need to be evaluated in this population."
"Our findings indicate that elevated coffee consumption (≥3 cups/day) has a protective effect on all-cause mortality in patients co-infected with HIV-HCV, a population at specific risk of end-stage liver disease and greater risk of cardiovascular diseases and cancer. This would also suggest that the benefits of elevated coffee are more relevant in patients with HIV-HCV than in the general population. The benefits of coffee extracts and supplementing dietary intake with other anti-inflammatory compounds need to be evaluated in this population. Further research will help to better elucidate the causal mechanisms of this relationship and reveal whether polyphenols contained in coffee are also implicated."
" After multivariable adjustment, an 80% and 60% reduction in mortality risk was observed, respectively, in individuals who cleared HCV post-treatment (HR 0.2; CI 0.1-0.7; p = 0.011) and individuals treated but not cured (HR 0.4; CI 0.2-0.9; p = 0.036), compared with those not yet treated and those on treatment......This is the first time that such an association has been found in a population at high risk of death because of the double burden of two concomitant diseases and associated conditions. It is worth noting that HCV-related mortality was four times higher than HIV-related mortality in the study population, and that AIDS was the third largest cause of mortality in this population after non-HIV- and non-HCV-related cancer. One additional key result of our study is that an 80% reduction in mortality risk was observed in individuals who cleared HCV post-treatment compared with those not yet treated."
-------------------
Protective effect of coffee consumption on all-cause mortality of French HIV-HCV co-infected patients
Jnl of Hepatology Sept 25 2017
Maria Patrizia Carrieri1,2,,y, Camelia Protopopescu1,2,y, Fabienne Marcellin1,2, Silvia Rosellini1,2, Linda Wittkop3,4,5, Laure Esterle3,4, David Zucman6, François Raffi7, Eric Rosenthal8,9, Isabelle Poizot-Martin10, Dominique Salmon-Ceron11,12, François Dabis3,4,5, Bruno Spire1,2,
the ANRS CO13 HEPAVIH Study Group
1Aix Marseille Univ, INSERM, IRD, SESSTIM, Sciences Economiques & Sociales de la Sante & Traitement de l'Information Medicale, Marseille, France; 2ORS PACA, Observatoire Regional de la Sante Provence-Alpes-Cote d'Azur, Marseille, France; 3Univ. Bordeaux, ISPED, Centre INSERM U1219-Bordeaux Population Health, Bordeaux, France; 4INSERM, ISPED, Centre INSERM U1219-Bordeaux Population Health, Bordeaux, France; 5CHU de Bordeaux, Pole de sante publique, Bordeaux, France; 6Service de Medecine Interne, Hopital Foch, Suresnes, France; 7Infectious and Tropical Diseases Department, Nantes University Hospital, Nantes, France; 8Nice Sophia-Antipolis University, Nice, France; 9Department of Internal Medicine, L'Archet Hospital, Nice, France; 10Aix Marseille Univ, APHM Sainte-Marguerite, Service d'Immunohematologie clinique, Marseille, France; 11Service des Maladies Infectieuses et Tropicales, Hopital Cochin, AP-HP, Paris, France; 12Universite Paris Descartes, Paris, France
"Elevated coffee consumption at baseline was associated with a 50% reduced risk of all-cause mortality (hazard ratio 0.5; CI 0.3-0.9; p = 0.032), after adjustment for gender and psychosocial, behavioral and clinical time-varying factors.....Drinking three or more cups of coffee per day halves all-cause mortality risk in patients co-infected with HIV-HCV. The benefits of coffee extracts and supplementing dietary intake with other anti-inflammatory compounds need to be evaluated in this population."
Highlights
⋅Coffee has anti-inflammatory and hepato-protective properties.
⋅Drinking three or more cups/day halves mortality risk in HIV-HCV co-infected patients.
⋅While curing HCV is fundamental, not smoking further improves survival in this group.
⋅Healthy behavior change should also be promoted after HCV clearance.
We defined the following categories for coffee consumption: low consumption (one cup/day of coffee or occasional consumption or no consumption), moderate consumption (two cups/day of coffee) and elevated consumption (at least three cups/day of coffee). Individuals with depressive symptoms were identified using gender-specific cut-off values for the CES-D score (17 for men and 23 for women).25
Among patients with documented causes of death, the main underlying causes were (Table 1): HCV-related (42.8%, n = 33, including hepatocellular carcinoma: 14.3%, n = 11), cancer not related to AIDS or hepatitis (11.7%, n = 9), AIDS-related (10.4%, n = 8), cardiovascular disease (3.9%, n = 3), overdose (3.9%, n = 3), suicide (3.9%, n = 3), and respiratory diseases (2.6%, n = 2). The cause of death was unknown in 14.3% (n = 11) of the notified cases among the study patients.
Characteristics of the study patients
The study patients' main characteristics at their last available follow-up visit are presented in Table 2. The median age of participants was 49 years (IQR: 46-52 years) and most were males (70.2%). The main HIV transmission category was intravenous drug use (63.2%) and HCV genotype 1 was predominant (53.4%). At the end of follow-up, more than half of the study patients had not yet started HCV treatment (53.3%), a minority (7%) were on treatment, while the remaining patients had completed treatment (15.7% were not cured and 24% were sustained responders). Seventeen percent had a F3-F4 fibrosis stage according to the FIB-4 index. At enrolment, 1.3% of the patients had experienced hepatocellular carcinoma and/or liver transplantation, and 2.9% had experienced indirect clinical signs of cirrhosis. With respect to HIV-related characteristics, 94.5% were receiving ART and most (82.5%) had an undetectable HIV RNA plasma viral load. Elevated coffee consumption was reported by 26.6% of the study patients at baseline, half of them (51.3%) reported low coffee consumption, and 48.8%, 17.8%, 5.9% and 24.9% reported low, moderate, elevated, and no alcohol consumption at baseline, respectively. The prevalence of regular binge drinking was 13.9%. Twelve percent of the patients had never smoked and more than a third (36.5%) reported depressive symptoms.
Background & Aims
Coffee has anti-inflammatory and hepato-protective properties. In the general population, drinking ≥3 cups of coffee/day has been associated with a 14% reduction in the risk of all-cause mortality. The aim of this study was to investigate the relationship between coffee consumption and the risk of all-cause mortality in patients co-infected with human immunodeficiency virus (HIV) and hepatitis C virus (HCV).
Methods
ANRS CO13 HEPAVIH is an ongoing French nationwide prospective cohort of patients co-infected with HIV-HCV collecting both medical and psychosocial/behavioural data (annual self-administered questionnaires). We used a Cox proportional hazards model to estimate the effect of elevated coffee consumption (≥3 cups/day) at baseline on all-cause mortality during the cohort's five-year follow-up.
Results
Over a median [interquartile range] follow-up of 5.0 [3.9-5.9] years, 77 deaths occurred among 1,028 eligible patients (mortality rate 1.64/100 person-years; 95% confidence interval [CI] 1.31-2.05). Leading causes of death were HCV-related diseases (n = 33, 43%), cancers unrelated to AIDS/HCV (n = 9, 12%), and AIDS (n = 8, 10%). At the first available visit, 26.6% of patients reported elevated coffee consumption. Elevated coffee consumption at baseline was associated with a 50% reduced risk of all-cause mortality (hazard ratio 0.5; CI 0.3-0.9; p = 0.032), after adjustment for gender and psychosocial, behavioral and clinical time-varying factors.
Conclusions
Drinking three or more cups of coffee per day halves all-cause mortality risk in patients co-infected with HIV-HCV. The benefits of coffee extracts and supplementing dietary intake with other anti-inflammatory compounds need to be evaluated in this population.
Lay summary
Coffee has anti-inflammatory and hepato-protective properties but its effect on mortality risk has never been investigated in patients co-infected with human immunodeficiency virus (HIV) and hepatitis C virus (HCV). This study shows that elevated coffee consumption (≥3 cups/day) halves all-cause mortality risk in patients co-infected with HIV-HCV. The benefits of coffee extracts and supplementing dietary intake with other anti-inflammatory compounds need to be evaluated in this population.
Introduction
Patients co-infected with human immunodeficiency virus (HIV) and hepatitis C virus (HCV) are particularly vulnerable to developing liver disease due to immune activation/inflammation, exposure to antiretroviral therapy (ART) and evolution of HCV co-infection.[1], [2] In addition, HIV infection modifies the natural course of chronic hepatitis C infection, resulting in a more rapid progression to fibrosis and development of cirrhosis and end-stage liver disease.[3], [4] The impressive reduction in mortality rates since the introduction of ART has led to HCV-related causes of mortality, including end-stage liver disease, being more frequent than HIV-related causes in patients co-infected with HIV-HCV.[5], [6] Potent HCV therapeutic strategies based on direct-acting antiviral agents (DAAs) have been developed in recent years, making HCV clearance possible for nearly all treated patients.7 HCV clearance following successful HCV treatment is often accompanied by a regression of histologic lesions in co-infected patients - even with suboptimal interferon-based treatment[8], [9], [10] - and therefore reduces progression to end-stage liver disease. Accordingly, improving access to HCV treatment is crucial in reducing the burden of end-stage liver disease in patients co-infected with HIV-HCV.
Nevertheless, this population, even when cured of HCV, remains at an increased risk of death because of an accelerated aging process, which may result in cardiovascular events, cancers, and complications related to diabetes and to liver disease, for example esophageal bleeding.11
Polyphenols and caffeine in coffee have several hepato-protective properties. In people at risk of liver disease, previous research has shown that coffee consumption is associated with better liver function,12 and less fibrosis,13 cirrhosis and liver cancer.14
In patients co-infected with HIV-HCV, individuals with elevated coffee consumption (defined as drinking three cups or more per day) have a reduced risk of insulin resistance and lower levels of liver enzymes.[15], [16]
In the general population, there is also strong evidence that coffee consumption is associated with a 13-14% risk reduction in all-cause mortality, as well as a reduced risk of cancer and diabetes.[17], [18], [19], [20], [21], [22] However, the extent to which coffee consumption may be associated with a reduced risk of all-cause mortality in patients co-infected with HIV-HCV, a population where liver-associated complications and alcohol use are often present,[11], [23] remains unknown.
We used five-year follow-up data from the French ANRS CO13 HEPAVIH cohort to investigate the effect of coffee consumption on mortality risk in this population, after adjusting for clinical status (including HCV clearance) and psychosocial/behavioural factors.
Discussion
In this large prospective nationwide cohort of patients co-infected with HIV-HCV followed-up in French hospital departments, we found that elevated coffee consumption had an independent protective effect on all-cause mortality risk. This is the first time that such an association has been found in a population at high risk of death because of the double burden of two concomitant diseases and associated conditions. It is worth noting that HCV-related mortality was four times higher than HIV-related mortality in the study population, and that AIDS was the third largest cause of mortality in this population after non-HIV- and non-HCV-related cancer. One additional key result of our study is that an 80% reduction in mortality risk was observed in individuals who cleared HCV post-treatment compared with those not yet treated.
Coffee and mortality
In recent years, the number of experimental and clinical research studies exploring the association between coffee consumption and clinical conditions has increased exponentially. The effect of coffee or coffee compounds has been studied on a series of pathologies, including Alzheimer's disease,33 inflammatory-related diseases including cancer, cardiovascular diseases, and metabolic and liver-related diseases[22], [34], [35], [36] and also on total and cause-specific mortality.[17], [18], [19], [20], [21], [22] Three or more cups of coffee per day was the threshold for coffee consumption most often associated with a lower morbidity and mortality. Although a recent meta-analysis did not show any association between coffee consumption and cancer mortality, its findings did suggest an inverse relationship between coffee consumption and all-cause mortality, as well as mortality from cardiovascular diseases.19
Cardiovascular diseases were the second largest non-HIV/non-HCV-related causes of mortality after cancer in our population. One meta-analysis showed a non-linear association between coffee consumption and the risk of cardiovascular diseases, with the lowest risk being observed in the second highest category of coffee consumption (median: 3.5 cups per day), and no association between elevated risk of cardiovascular diseases and the highest consumption category (median: 5 cups per day).36 Previous research using data from long-term follow-up prospective cohort studies showed no significant association between daily coffee consumption and coronary heart disease.37 In another meta-analysis, moderate coffee consumption was inversely associated with the risk of heart failure, the largest inverse association being observed for consumption of four servings per day.38 Moderate coffee consumption has also been shown to be weakly inversely associated with the risk of stroke.39
In addition, there is growing evidence for the hepato-protective role of coffee intake in patients with liver disease, including patients co-infected with HIV-HCV. It has already been shown that coffee consumption is associated with a reduced risk of elevated serum ALT activity12 and with a dose-dependent improvement in serum gamma glutamyltransferase and AST values, in populations at risk of liver disease.40 Coffee intake has been associated with a reduced risk of fibrosis and cirrhosis[21], [41], [42] and with a reduced risk of death in patients with cirrhosis,43 even after transplantation.44 Meta-analyses also suggest a protective effect of coffee intake on the risk of hepatocellular carcinoma in different populations, with a reduction in the risk by approximately 40%.14 It has also been hypothesized that polyphenols contained in coffee15 and chocolate45 may play a protective role in liver injury through a reduced risk of insulin resistance and reduced inflammation.46 Coffee consumption has also been shown to be inversely associated with the risk of type 2 diabetes in a dose-response meta-analysis.47
Several studies have identified preventive effects of coffee and caffeine extracts on hepatic fibrosis in standard rodent models and on the development of hepatic cirrhosis,[48], [49] for example through the inhibition of hepatic stellate cell activation.[50], [51] Caffeinated and decaffeinated coffee are similarly associated with improved liver function indicators, irrespective of the underlying disease.52 Moreover, recent reports have indicated that pure caffeine at non-toxic concentrations53 and caffeic acid54 can inhibit HCV replication in vitro.
Although HCV infection remained the most prevalent cause of death in our study population, cancer and cardiovascular diseases are becoming increasingly common causes of deaths in patients co-infected with HIV-HCV. This underlines the need to implement specific measures for the screening and management of cancer and cardiovascular diseases in this population.
HCV clearance and mortality
The effectiveness of HCV clearance on reducing mortality risk, found in this study, is consistent with results from previous research in patients with HCV and HIV-HCV co-infection. It is important to note that exposure to HCV treatment without achieving HCV clearance has also been significantly associated with reduced mortality risk, but that the reduction observed was not as great as for HCV clearers. In a multicenter cohort of 920 Italian patients with HCV-related cirrhosis, a significant reduction in the rates of liver-related complications, hepatocellular carcinoma, and liver-related mortality was found in those who achieved SVR compared with those who did not.55 A recent study including 2,743 patients with chronic HCV infection identified a significant reduction of all-cause mortality in patients who achieved HCV clearance as a result of successful treatment.56 In HIV-HCV co-infected patients, a previous study using data from the ANRS CO13 HEPAVIH cohort showed a significant association between HCV clearance and a reduction in liver stiffness, a marker of liver fibrosis.10 This result may partially explain the decrease in HCV-related mortality observed in HCV clearers. In addition, elevated coffee consumption has already been shown to increase adherence to HCV treatment and to reduce side effects57 but also to reduce self-reported symptoms.58
It is worth noting that when analysing HCV-related mortality as an outcome using a competing risk model which took into account causes of death other than HCV, elevated coffee consumption remained significantly associated with a reduced risk of HCV-related mortality (subHR 0.27; CI 0.08-0.89; p = 0.031).
Study limitations
One limitation of the present study was the difficulty of standardizing self-reported coffee intake and the lack of data about other caffeine sources and/or polyphenols. Nevertheless, our results are consistent with those obtained in the general population, which suggest a lower mortality risk from all causes in coffee drinkers compared with non-consumers.
Another limitation of the study is that the questionnaire only explored coffee intake and consequently we were not able to address the impact of individual genetic diversity on the metabolism of coffee and related ingredients,[59], [60] or the effect of other caffeine sources and polyphenols.
Finally, it is important to note that this study is observational in nature and the associations found cannot be interpreted in terms of causality.
Conclusions
Our findings indicate that elevated coffee consumption (≥3 cups/day) has a protective effect on all-cause mortality in patients co-infected with HIV-HCV, a population at specific risk of end-stage liver disease and greater risk of cardiovascular diseases and cancer. This would also suggest that the benefits of elevated coffee are more relevant in patients with HIV-HCV than in the general population. The benefits of coffee extracts and supplementing dietary intake with other anti-inflammatory compounds need to be evaluated in this population. Further research will help to better elucidate the causal mechanisms of this relationship and reveal whether polyphenols contained in coffee are also implicated.
Materials and methods
Study design
ANRS CO13 HEPAVIH is a multicenter prospective cohort that started in 2005 and enrolled HIV-HCV co-infected adults from 21 centres throughout France, representative of the French population living with these two viruses and in care.24 Inclusion criteria in the cohort were as follows: aged 18 years or more, HIV-1 infection and chronic HCV co-infection. Patients who had already cleared HCV i.e. those who had a sustained virological response (SVR) to previous HCV treatment and (in a second enrolment phase) those who had spontaneously cleared HCV could also be included if eligible. Clinical follow-up of patients was at enrolment (M0) and yearly thereafter (every six months for patients with cirrhosis) until the end of the study (60 months, M60). All patients provided written informed consent at enrolment. The study was designed and implemented in accordance with the Declaration of Helsinki, and the protocol was approved by the ethics committee of the Cochin University Hospital in Paris.
Data collection
Medical data
A standardized medical questionnaire, completed by physicians at each clinical visit, collected biological and clinical parameters related to HIV and HCV infection, including CD4 cell count, HIV plasma RNA level, HIV CDC clinical stage, HIV transmission category, ART use, HCV treatment status and virological response, HCV genotype, serum alanine aminotransferase (ALT) and aspartate aminotransferase (AST) levels, and platelet counts. Any history of liver problems such as hepatocellular carcinoma, liver transplantation, or the presence of indirect clinical signs of cirrhosis (ascites, esophageal varices with or without bleeding, hepatic encephalopathy) was recorded at enrolment. Information about mortality and causes of death were recorded for the entire cohort and validated by an expert committee.
Data concerning patients' tobacco use were recorded at each visit during face-to-face medical interviews with physicians. Patients were asked about their experience of smoking (non-smoker, former smoker, or current smoker).
Psychosocial/behavioural data
Patients enrolled in the cohort answered a self-administered questionnaire at enrolment and yearly thereafter until M60. This questionnaire collected socio-demographic data including gender, age, having a steady partner (or not), having children (or not), employment status, and housing type. It also included behavioural characteristics such as adherence to ART and depressive symptoms, assessed using the Center for Epidemiological Studies Depression Scale (CES-D).25 In addition, the questionnaire contained items on the occurrence of 39 self-reported symptoms over the previous four weeks. Alcohol consumption in the six months prior to the visit were assessed using the AUDIT-C questionnaire.26 Coffee intake was investigated using a question referring to the six months prior to the visit, with the following five possible answers: never, occasionally, one cup/day, two cups/day, more than two cups/day (one cup corresponding to 150-200 ml).
Statistical analyses
Selection of the study population (patients and visits)
We first selected all available annual follow-up visits between M0-M60 for patients with at least one completed self-administered questionnaire. Of these patients, those who had a latest news date (corresponding either to a follow-up visit or to death) after their entry date (i.e. having at least two time points with available information during the cohort follow-up) were selected for this study. Moreover, among these patients, only those who reported their coffee consumption at baseline (i.e. at the first visit with available data from a self-administered questionnaire) were considered eligible for this analysis. The follow-up period for each eligible patient was defined as follows: the duration between the first follow-up visit with an available self-administered questionnaire (entry date) and the latest news date (corresponding either to the last visit with an available self-administered questionnaire, or to a follow-up visit without a self-administered questionnaire, or to death) with censoring at 72 months after the M0 visit.
Outcome
The study outcome was deaths from all causes occurring between M0 and M72 among eligible patients.
Explanatory variables
The following explanatory variables were tested in the multivariable analysis to adjust for known predictors of mortality and possible confounders. The AUDIT-C questionnaire was used to calculate the number of alcohol units (AU) consumed per day for individuals who reported current alcohol consumption. One AU was defined as a standard drink, containing 11-14 g of alcohol and corresponding to one small bottle of beer, one medium glass of wine, or a shot of distilled spirits. We used the following categories for average daily alcohol consumption: no consumption, low consumption (≤1 AU/day), moderate consumption (1-3 AU/day for women and 1-4 AU/day for men), and elevated consumption (>3 AU/day for women and >4 AU/day for men).27 Regular binge drinking was defined as drinking at least 5 AU on one occasion at least once a week. We defined the following categories for coffee consumption: low consumption (one cup/day of coffee or occasional consumption or no consumption), moderate consumption (two cups/day of coffee) and elevated consumption (at least three cups/day of coffee). Individuals with depressive symptoms were identified using gender-specific cut-off values for the CES-D score (17 for men and 23 for women).25 A score above these cut-off values was taken to be indicative of having depressive symptoms. Patients who reported living in hotels, accommodation centers, on the street or in therapeutic apartments were considered to have unstable housing.
Adherence to ART was assessed according to the methodology established by the AIDS Clinical Trial Group28 using a three-level score (high, moderate and low adherence) based on a validated algorithm using ART doses - both those prescribed and those actually taken - during the previous four days, as described elsewhere.29 The fibrosis-4 (FIB-4) index, which is calculated by age, AST, ALT and platelet count, was used as a non-invasive marker of liver fibrosis, using the intervals defined by the cut-off values 1.45 and 3.25 which corresponding to F0-F1, F2 and F3-F4 Metavir stages, respectively.30
Except for gender, HCV genotype, HIV transmission category, smoking status, coffee and alcohol consumption (which were measured at baseline), all the other explanatory variables were evaluated at each visit and used as time-varying covariates in the statistical analyses.
Statistical methods
The all-cause mortality rate was computed as the number of deaths occurring between M0 and M72 divided by the number of person-years during the study period (computed as the sum, for all patients, of the number of years between entry date and latest news date, i.e., death, latest news visit or censoring). The 'last observation carried forward' method was used to impute the values for the explanatory variables when they were missing (i.e., at clinical visits without self-administered questionnaires).
The association between baseline coffee consumption and mortality was assessed after adjustment for potential predictors and confounding factors, using a Cox proportional hazards model with robust standard errors. Potential adjustment variables with a p value <0.20 (Wald test) in the univariate analyses were considered eligible for inclusion in the multivariable analysis. A backward selection procedure, based on the Wald test, was then used to identify the adjustment variables in the final multivariable model (variables were considered significantly associated with the outcome if the p value ≤0.05). The final multivariable model was adjusted for gender and age, irrespective of their p values. The presence of confounding factors was evaluated by removing each non-significant variable, one at a time, and noting the effect on the coefficients for the remaining variables (the eliminated variable was considered to be a confounder and included in the final model if at least one of the coefficients for the remaining variables changed by more than 25%). The proportional hazards assumption was tested in the final multivariable Cox model by examining the rescaled Schoenfeld residuals.31
In order to verify whether different follow-up durations could have an impact on our results, we identified two subgroups of patients with different follow-up durations (last follow-up visit <48 months vs. last follow-up visit ≥48 months) and performed a secondary analysis using a shared-frailty Cox model, each subgroup having a specific baseline hazard ratio (HR). Further details about the shared-frailty Cox model are provided elsewhere.32
Stata/SE 12.1 software (StataCorp LP, College Station, USA) was used for all the analyses.
For further details regarding the materials used, please refer to the CTAT table.
Results
Study population
The selection of the study population (patients and visits) is presented in the flow chart in Fig. 1. Among the 1,246 patients included in the cohort between 2005 and November 2014, 1,051 completed at least one self-administered questionnaire during follow-up. Of these, 1,028 had both a latest news date after their entry date and available coffee consumption data at baseline, and were thus eligible for analyses (study population).
Causes of death
In the 72 months from enrolment, a total of 97 deaths were notified in the cohort, 77 of these occurring in the 1,028 patients of the present study. The distribution of causes of death was similar between patients in the study and all the patients included in the cohort (Table 1). Median (interquartile range [IQR]) follow-up duration for study patients was 5.0 (3.9-5.9) years, representing 4,700 person-years. The mortality rate was 1.64/100 person-years (95% confidence interval [CI] 1.31-2.05).
Among patients with documented causes of death, the main underlying causes were (Table 1): HCV-related (42.8%, n = 33, including hepatocellular carcinoma: 14.3%, n = 11), cancer not related to AIDS or hepatitis (11.7%, n = 9), AIDS-related (10.4%, n = 8), cardiovascular disease (3.9%, n = 3), overdose (3.9%, n = 3), suicide (3.9%, n = 3), and respiratory diseases (2.6%, n = 2). The cause of death was unknown in 14.3% (n = 11) of the notified cases among the study patients.
Characteristics of the study patients
The study patients' main characteristics at their last available follow-up visit are presented in Table 2. The median age of participants was 49 years (IQR: 46-52 years) and most were males (70.2%). The main HIV transmission category was intravenous drug use (63.2%) and HCV genotype 1 was predominant (53.4%). At the end of follow-up, more than half of the study patients had not yet started HCV treatment (53.3%), a minority (7%) were on treatment, while the remaining patients had completed treatment (15.7% were not cured and 24% were sustained responders). Seventeen percent had a F3-F4 fibrosis stage according to the FIB-4 index. At enrolment, 1.3% of the patients had experienced hepatocellular carcinoma and/or liver transplantation, and 2.9% had experienced indirect clinical signs of cirrhosis. With respect to HIV-related characteristics, 94.5% were receiving ART and most (82.5%) had an undetectable HIV RNA plasma viral load. Elevated coffee consumption was reported by 26.6% of the study patients at baseline, half of them (51.3%) reported low coffee consumption, and 48.8%, 17.8%, 5.9% and 24.9% reported low, moderate, elevated, and no alcohol consumption at baseline, respectively. The prevalence of regular binge drinking was 13.9%. Twelve percent of the patients had never smoked and more than a third (36.5%) reported depressive symptoms.
The characteristics of the study population according to the three categories of coffee consumption at first available patient follow-up visit are presented in Table 3.
Factors associated with mortality
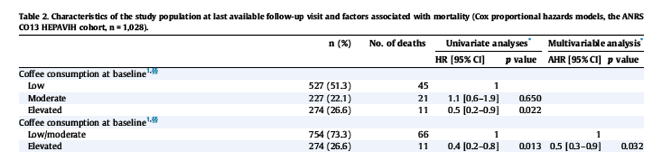
The crude and adjusted HR for the factors associated with mortality are reported in Table 2.
In the multivariable model adjusted for socio-demographic, behavioural and clinical factors (including severe fibrosis and HCV treatment status), elevated coffee consumption at baseline (≥3 cups/day) (HR 0.5; CI 0.3-0.9; p = 0.032) was associated with a lower mortality risk, along with reporting never smoking (HR 0.3; CI 0.1-1.0; p = 0.051). After multivariable adjustment, an 80% and 60% reduction in mortality risk was observed, respectively, in individuals who cleared HCV post-treatment (HR 0.2; CI 0.1-0.7; p = 0.011) and individuals treated but not cured (HR 0.4; CI 0.2-0.9; p = 0.036), compared with those not yet treated and those on treatment. The other factors independently associated with higher mortality risk were: not having a steady partner, severe fibrosis (FIB-4 >3.25), HIV clinical stage C, and CD4 cell count ≤200 cells/mm3, a history of hepatocellular carcinoma and/or liver transplantation at enrolment, and a history of indirect clinical signs of cirrhosis at enrolment.
In the secondary analysis using the shared-frailty Cox model with different baseline HR according to follow-up duration, we found similar results concerning the association between elevated coffee consumption and reduced mortality risk (data not shown).
| |
| |
| |
|
|
|