 |
 |
 |
| |
Framingham Cardio Risk Score Twice Higher in Premenopausal Women With HIV
|
| |
| |
IDWeek2017/IDSA, October 4-8, 2017, San Diego
Mark Mascolini
Premenopausal women with HIV had a twice higher 10-year Framingham cardiovascular risk score than a comparison group of similarly aged women without HIV [1]. Women with HIV had significantly lower "good" high-density lipoprotein (HDL) cholesterol than HIV-negative women.
Cardiovascular risk rises in women in the general population as they lose the cardioprotective effect of estrogen. But less is known about changing cardiovascular risk as women approach the menopause [2] and particularly about potential differences between middle-aged women with and without HIV. To address these issues, researchers from Cooper University Hospital in Camden and Temple University in Philadelphia conducted this retrospective study.
The study included 9635 women between 18 and 55 years old who had not reached the menopause and had no history of myocardial infarction. Cross-sectional data came from the National Health and Nutrition Examination Survey (NHANES) from 1999 through 2014. Researchers compared components of the Framingham cardiovascular risk score in 25 women with HIV and 9610 HIV-negative women. They also compared provider advice to modify cardiovascular risks and women's stated attempts to make such changes.
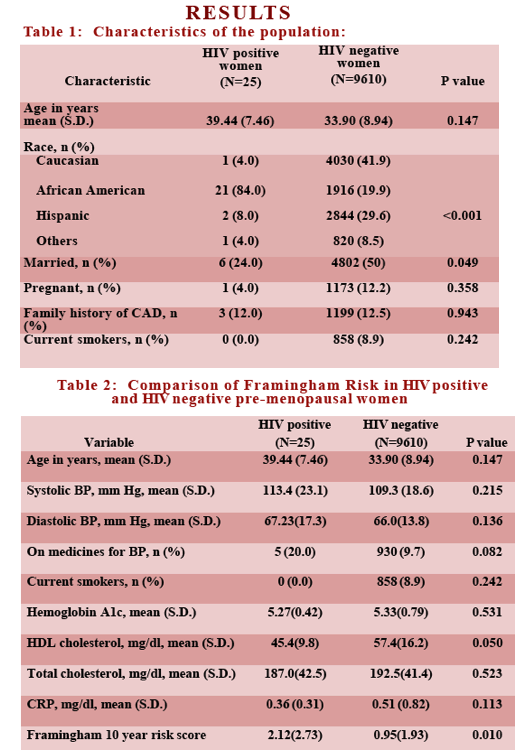
Women with HIV were nonsignificantly older than HIV-negative women (average 39.4 versus 33.9 years, P = 0.147). The HIV group included a higher proportion of blacks (84% versus 19.9%) and lower proportions of Hispanics (8% versus 29.6%) and whites (4% versus 41.9%) (P < 0.001). A significantly lower proportion of women with HIV were married (24% versus 50%, P = 0.049). But HIV-positive and negative women did not differ significantly in proportion with a family history of coronary artery disease (12% and 12.5%) or diabetes (4% versus 5.6%), or proportion of current smokers (0% and 8.9%).
Women with HIV had a twice higher 10-year Framingham cardiovascular risk score than did HIV-negative women (2.12 versus 0.95, P = 0.010). Still, the 10-year risk in these middle-aged women was relatively low (a score of 2.12 means cardiovascular disease is expected to develop in 2 of every 100 women over the next 10 years). Two risk score components largely drove this difference-lower "good" HDL cholesterol in women with HIV (average 45.4 versus 57.4 mg/dL, P = 0.050) and a higher proportion taking blood pressure drugs (20% versus 9.7%, P = 0.082). As already noted, age was marginally older in the HIV group. Women with and without HIV did not differ substantially in systolic or diastolic blood pressure, current smoking status, hemoglobin A1c, total cholesterol, or C-reactive protein (an inflammation marker).
The researchers did not report a multivariate analysis to determine whether HIV infection independently predicted cardiovascular disease in these women. They did report that significantly higher proportions of HIV-positive women got provider advice to exercise (28% versus 13%, P = 0.027) and to modify their diet (28% versus 13.3%, P = 0.031). But the HIV-positive and negative groups did not differ significantly in proportions who reported trying to exercise (24% versus 18.9%) or trying to change their diet (32% versus 24.5%).
The investigators noted that their analysis is limited by the small number of women with HIV, the retrospective design of the study relying on self-reported data, and lack of data on HIV load or antiretroviral therapy. Because the Framingham score does not account for HIV status, the authors underline the need for methods to stratify cardiovascular risk in HIV populations.
References
1. Raza A, Malayala V. A comparative analysis of cardiovascular risk in HIV sero-positive and sero-negative pre-menopausal women. IDWeek2017/IDSA. October 4-8, 2017. San Diego. Abstract 573.
2. El Khoudary SR. Gaps, limitations and new insights on endogenous estrogen and follicle stimulating hormone as related to risk of cardiovascular disease in women traversing the menopause: a narrative review. Maturitas. 2017;104:44-53.


|
| |
|
 |
 |
|
|