 |
 |
 |
| |
High Comfort Level With STI Self-Tests in HIV Group; Results Match Provider Tests
|
| |
| |
Download the PDF here
IDWeek2017/IDSA, October 4-8, 2017, San Diego
Mark Mascolini
More than 80% of military personnel with HIV preferred collecting their own pharyngeal or rectal samples for gonorrhea or chlamydia screening in a 148-man analysis [1]. Patient and provider results proved largely concordant.
Analysis of a representative HIV-positive military group identified high frequencies of rectal and pharyngeal gonorrhea (5%) and rectal chlamydia (7.5%). US military researchers who conducted a new study noted that extragenital gonorrhea and chlamydia infection can cause no symptoms. As a result, regardless of symptoms, the CDC recommends (1) testing for rectal gonorrhea or chlamydia in men who have sex with men who had receptive anal sex in the past year and (2) testing for pharyngeal gonorrhea in men who had receptive oral sex in the past year.
Adherence to these guidelines remains variable for numerous reasons, including provider and patient discomfort with sexual history taking and testing. The military researchers hypothesized that self-testing for these infections could circumvent these barriers. They conducted this study to assess the feasibility and acceptability of self-administered rectal and pharyngeal sample collections and oral rinses in men with HIV. All received standardized oral and written instructions on sample collection and completed a related survey. (Residents of Maryland, Washington, DC, and Alaska can order these self-testing kits at https://www.iwantthekit.org/.) All men also underwent gonorrhea/chlamydia testing by their provider. Half had provider testing first; half did the self-tests first. Researchers used the same assay (GEN-PROBE APTIMA) to analyze all samples.
The study included 148 men with HIV, 40% African American and 35% Caucasian. Median age stood at 43. For extragenital gonorrhea, self-testing detected 2 additional positive pharyngeal samples and 1 additional positive rectal sample not detected in provider samples. For extragenital chlamydia, provider testing detected 1 additional positive rectal sample not detected by self-testing. An oral mouth wash using sterile water identified 3 additional gonorrhea infections.
Among survey respondents answering questions about rectal testing, 100% strongly agreed or agreed they understood self-testing instructions, 91% strongly agreed or agreed they felt comfortable collecting swabs, and 89% strongly agreed or agreed they felt comfortable collecting swabs at home. A large majority, 96%, felt confident they collected swabs as instructed. Only 18% of respondents strongly agreed or agreed that they preferred having their provider collect rectal swabs.
Among respondents answering questions about pharyngeal testing, proportions who strongly agreed or agreed were 98% for understanding instruction, 98% for comfort with collecting swabs, 94% for comfort with collecting swabs at home, and 99% for confidence they collected swabs as instructed. Only 15% preferred that their provider collect pharyngeal swabs.
The researchers concluded that self-testing for gonorrhea and chlamydia in people with HIV "is a feasible and acceptable option for collecting extragenital samples and could improve testing rates."
Reference
1. Ganesan A, Golden D, Deiss R, et al. Self-testing is a feasible and acceptable option for identifying extra-genital gonorrhea (GC) and chlamydia (CT) infections in HIV infected persons. IDWeek2017/IDSA. October 4-8, 2017. San Diego. Abstract 2256.


(POSTER PDF ATTACHED)
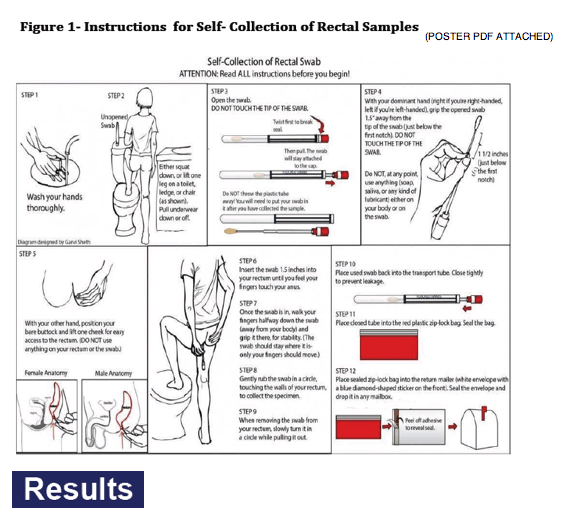
Table: 1 Performance Characteristics of Self versus Provider Administered Swabs for Identifying GC Infections
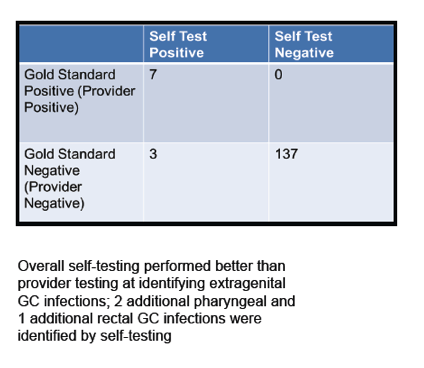
Table: 2 Performance Characteristics of Self versus Provider Administered Swabs for Identifying CT infections
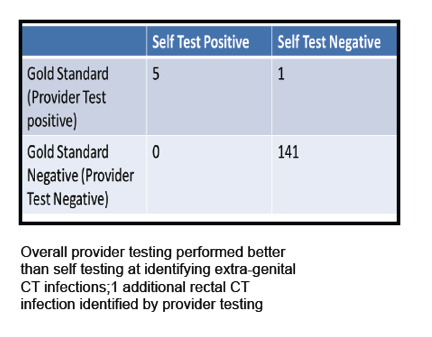
Table: 3 Results of Feasibility and Acceptability Questionnaire
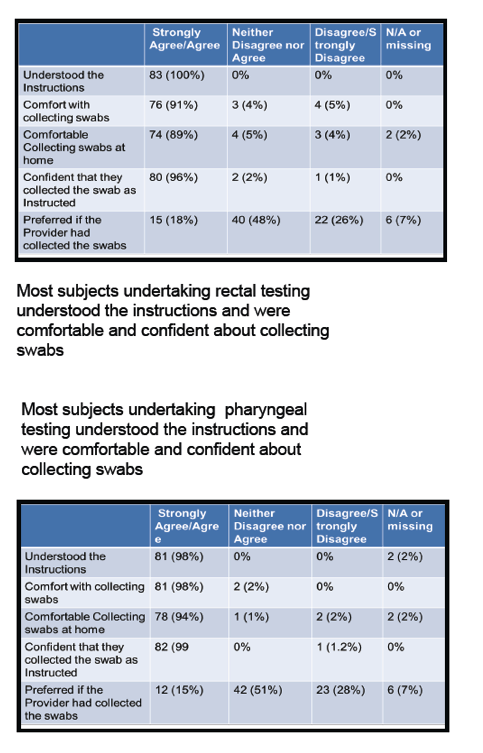
Table: 4 Performance Characteristics of an Oral Mouth wash for identifying GC/CT infections
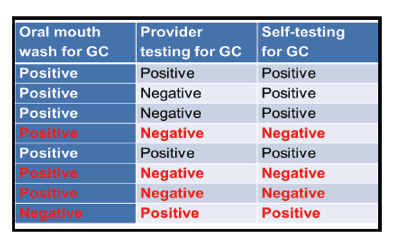
Overall the mouth wash identified three additional GC cases that were not identified by either provider or self testing, while 1 infection picked up on a pharyngeal swab was negative on the mouth wash. Of note, the two discordant results on the comparison of self vs. provider testing were positive with the mouth wash
|
| |
|
 |
 |
|
|