 |
 |
 |
| |
NEW DIAGNOSES OF HIV AMONG INJECTING DRUG USERS, NEW YORK CITY 2006-2016
|
| |
| |
Reported by Jules Levin
CROI 2018 March 4-7 Boston MA
Lucia V. Torian1, Jasmine Abdelnabi1, Lisa A. Forgione1, Joel O. Wertheim21New York City Department of Health and Mental Hygiene, Long Island City, NY, USA,
2University of California San Diego La Jolla, CA, USA

Program Abstract:
Unintentional drug poisoning and overdose deaths in New York City have increased each year between 2010 and 2016. One contributing factor has been the transition of users of medical and non-medical opioid analgesics to non-injection heroin use, with rapid (median 6 months) transition to heroin injection. This has led to concern that a resurgent HIV epidemic among injecting drug users would follow, as has been seen elsewhere in the US.
We analyzed new diagnoses reported to surveillance to ascertain the trajectory, demographics and risk factors of the HIV epidemic among NYC IDU, focusing on trends among the 2,037 new HIV diagnoses with IDU as a risk factor that occurred in 2006-2016. Pairwise concordance analysis, a genetic distance-based clustering tool, was used to construct transmission networks.
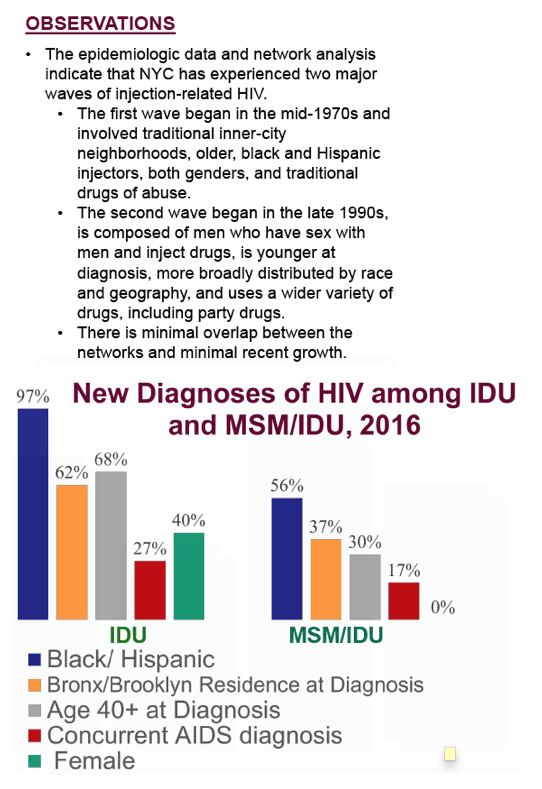
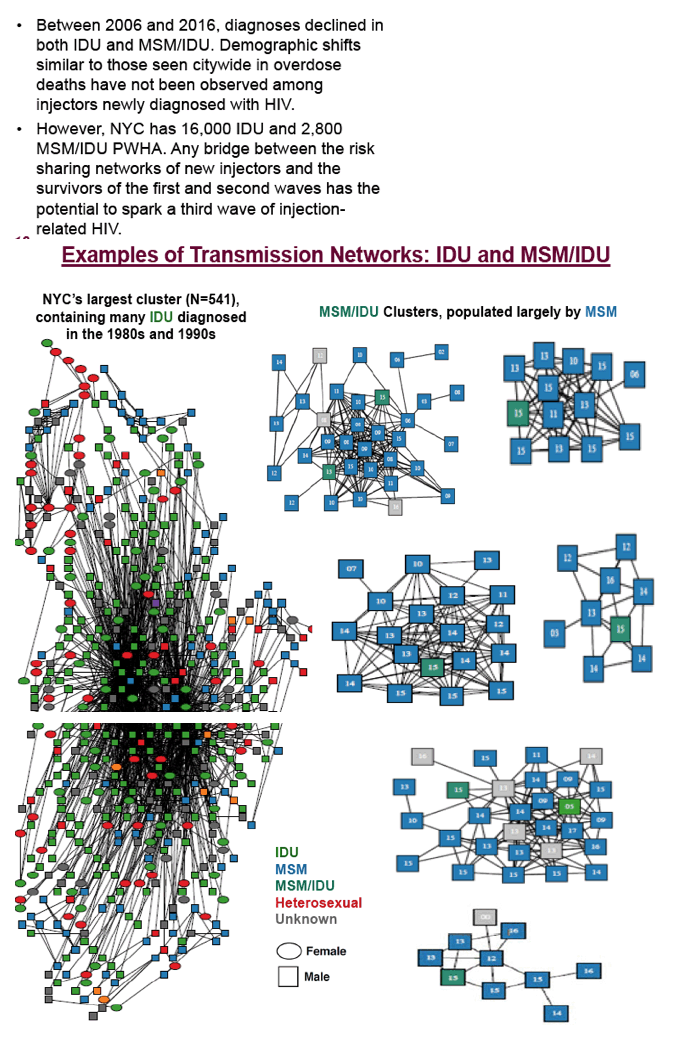
Most injection-related cases in the history of the NYC epidemic have occurred in two distinct waves. The first wave began prior to 1981, is 97% black and Hispanic, 68% aged 40+ at diagnosis, and concentrated in northern Manhattan, the South Bronx, and central Brooklyn. Its survivors occupy genetic transmission networks populated primarily by older diagnosis dates. The second wave is more recent, involves persons with the dual risk of MSM and IDU, and is more evenly distributed by race/ethnicity (40% white) and neighborhood, younger, (47% aged 20-29 and 30% aged 30-39 years), and belongs to transmission networks populated primarily by young, non-injecting, more recently diagnosed MSM. There is minimal overlap between the networks of the two waves. To date, the new heroin injectors, whose numbers and demographics are unknown, have made no discernible impact on HIV rates. In fact, during 2006-2016 new diagnoses declined 88.0% among IDU and 64.6% among MSM/IDU.
Unlike other jurisdictions, NYC has not seen an increase in HIV diagnoses attributable to IDU. However, it has a large population of people living with HIV, including more than 16,000 IDU and more than 2,600 MSM/IDU, and any bridge between the risk sharing networks of new injectors and the survivors of the first and second waves has the potential to spark a third wave of injection-fueled HIV. NYC syringe exchange programs, which reduced incidence in previous waves, as well as New York State legislation that in 2000 legalized over-the-counter syringe sales in pharmacies, may mitigate risk by facilitating safe injection among future new injectors.

|
| |
|
 |
 |
|
|