 |
 |
 |
| |
Carotid Plaque Predicts All-Cause Mortality in Women and Men With HIV: "Association of carotid artery atherosclerosis with mortality in HIV+ women and men"
|
| |
| |
25th Conference on Retroviruses and Opportunistic Infections (CROI), March 4-7, 2018, Boston
Mark Mascolini
WEBCAST: http://www.croiwebcasts.org/console/player/37177?mediaType=slideVideo&&crd_fl=1&ssmsrq=1520618770523&ctms=5000&csmsrq=966
Ultrasound-measured carotid artery plaque predicted all-cause mortality over the following decade in women and men with HIV infection [1]. This appears to be the first study showing that carotid plaque signals a major health event in adults with HIV.
Three markers of atherosclerosis detected by carotid artery ultrasound predict cardiovascular disease and mortality in the general population: (1) carotid artery intima media thickness (cIMT), (2) plaque, and (3) arterial stiffness. But few studies have tried to trace links between these signals and cardiovascular disease or mortality in people with HIV.
To fill this gap, researchers working with the Women's Interagency HIV Study (WIHS) and the Multicenter AIDS Cohort Study (MACS) analyzed associations between cIMT, carotid artery plaque, and carotid artery stiffness and all-cause mortality over 10 years in these women and men with HIV and their sociodemographically similar counterparts without HIV infection.
WIHS began in 1994 and now includes about 5000 women at 10 US sites. MACS started in 1984 and now includes about 7000 gay or bisexual men at 4 US sites. This analysis included 1722 WIHS women (71% with HIV) and 1304 MACS men (62% with HIV), none of whom had self-reported coronary heart disease when they first had carotid ultrasound. The outcome was all-cause mortality ascertained by active surveillance or linkage to the National Death Index. The three atherosclerosis signals were (1) cIMT of the common carotid artery, (2) focal plaque in at least 1 of 6 locations, and (3) Young's modulus of elasticity, an indicator of arterial stiffness. The researchers used Cox models to explore potential associations between these three measures and time to death in analyses that accounted for HIV status, demographic and behavioral factors, cardiometabolic risk factors, and HIV variables.
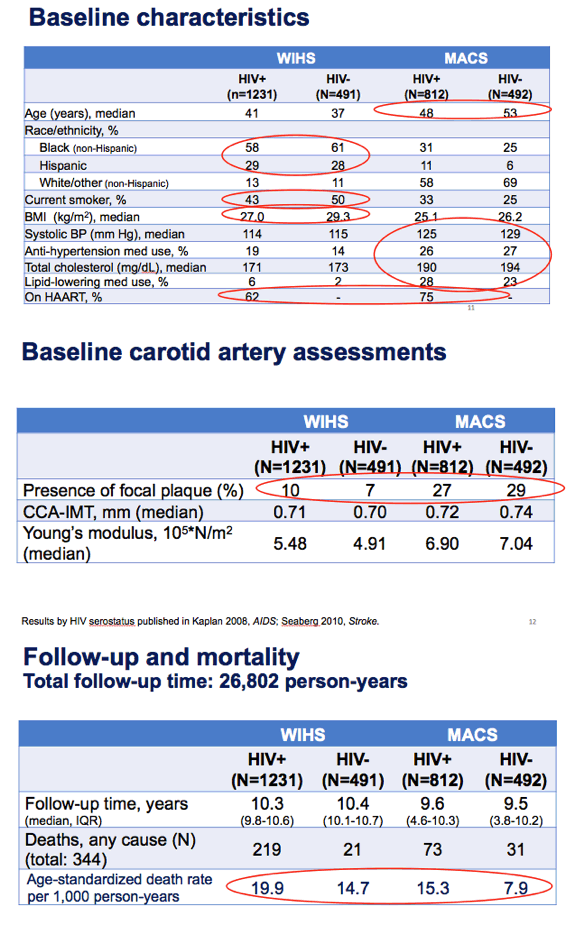
Median baseline ages in HIV-positive and negative participants were 41 and 37 in WIHS and 48 and 53 in MACS. Respective proportions of blacks were 58% and 61% in WIHS and 31% and 25% in MACS. Proportions of current smokers were 43% and 50% in WIHS and 33% and 25% in MACS. Among people with HIV, 62% in WIHS and 75% in MACS took antiretroviral therapy at baseline.
Median follow-up time reached 10.3 years in WIHS women and 9.6 years in MACS men, with little difference between HIV-positive and negative participants. Over that time, age-standardized death rates per 1000 person-years were 19.9 in WIHS women with HIV, 14.7 in WIHS women without HIV, 15.3 in MACS men with HIV, and 7.9 in MACS men without HIV.
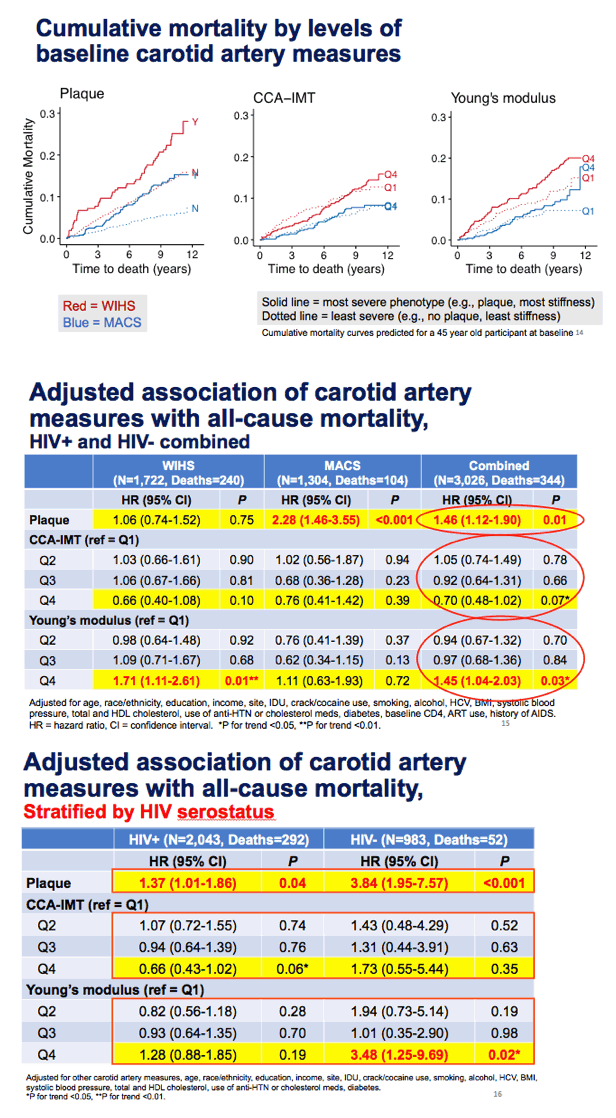
Among all participants combined, carotid plaque independently predicted death (hazard ratio [HR] 1.46, 95% confidence interval [CI] 1.12 to 1.90, P = 0.01). That association was significant in MACS men (HR 2.28, 95% CI 1.46 to 3.55, P < 0.001) but not in WIHS women. Being in the highest arterial stiffness quartile (versus the lowest) also independently predicted mortality in the whole group (HR 1.45, 95% CI 1.04 to 2.03, P = 0.03). This association was strong in WIHS women (HR 1.71, 95% CI 1.11 to 2.61, P = 0.01) but was not significant in MACS men. cIMT did not predict all-cause mortality in the overall group or in the MACS or WIHS groups separately.
Next the researchers put HIV-positive women and men in one group and HIV-negative women and men in another. Carotid plaque raised the risk of all-cause mortality in women and men with HIV (HR 1.37, 95% CI 1.01 to 1.86, P = 0.04), and that association was much stronger in HIV-negative women and men (HR 3.84, 95% CI 1.95 to 7.57, P < 0.001). Among HIV-negative people, being in the highest (versus lowest) arterial stiffness quartile more than tripled the risk of all-cause mortality (HR 3.48, 95% CI 1.25 to 9.69, P = 0.02). But arterial stiffness did not predict death in women and men with HIV. Again, cIMT did not predict death in either group.
The WIHS/MACS team believes their study "validates the use of carotid artery ultrasound in HIV-positive populations to determine markers of future mortality risk." They proposed that detecting plaque may be a particularly strong signal in people like those in WIHS and MACS, including those with HIV.
Reference
1. Hanna DB, Moon JY, Anastos K, et al. Carotid artery atherosclerosis is associated with mortality in HIV+ women and men.25th Conference on Retroviruses and Opportunistic Infections (CROI). March 4-7, 2018. Boston. Abstract 78.




|
| |
|
 |
 |
|
|