 |
 |
 |
| |
HIV Control Rate Lower in Women
Than Men in Inner-City Vancouver
|
| |
| |
"women were less likely to achieve virologic suppression (p=0.016)."
10th IAS Conference on HIV Science (IAS 2019), July 21-24, 2019, Mexico City
Mark Mascolini
In a Vancouver HIV population with high rates of illicit drug and alcohol use, women controlled HIV with antiretroviral therapy significantly less often than men [1]. Type of antiretroviral therapy and demographic variables did not appear to explain this HIV suppression difference.
Previous large studies found better HIV suppression rates in men than women in the United States [2,3]. CDC analysis of more than 12,000 participants in the US Medical Monitoring Project charted significantly higher viral suppression rates in the past 12 months in white men (69%) than in white women (62%, P = 0.005), Hispanic women (58%, P < 0.001), or black women (55%, P < 0.001) [3].
To get a better understanding of viral suppression rates and comorbidities among women and men in Vancouver, Canada, clinical researchers retrospectively analyzed their vulnerable inner-city population [1]. They defined viral suppression as a viral load below 40 copies. All women and men were enrolled in a multidisciplinary program to address medical, social, psychological, and addiction-related needs.
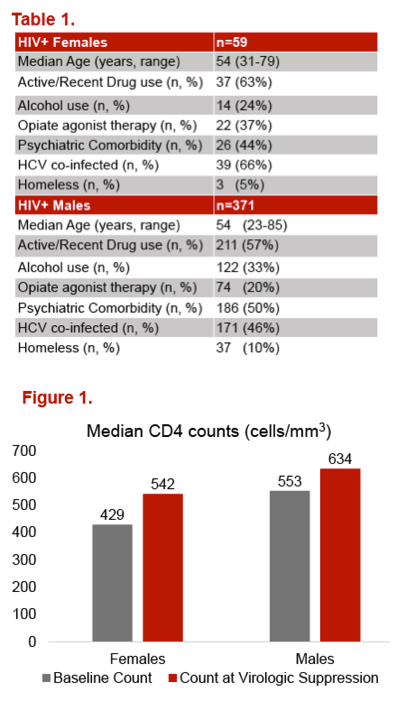
The 59 women and 371 men studied at the Vancouver Infectious Diseases Centre had median ages of 54 (range 31 to 79) and 54 (range 23 to 85). Women and men included high proportions with active/recent drug use (63% and 57%), alcohol use (24% and 33%), opiate agonist therapy (37% and 20%), psychiatric comorbidity (44% and 50%), HCV coinfection (66% and 46%), and homelessness (5% and 10%). Median CD4 count was nonsignificantly lower in women than men at baseline (429 versus 553) and at virologic suppression (542 versus 634).
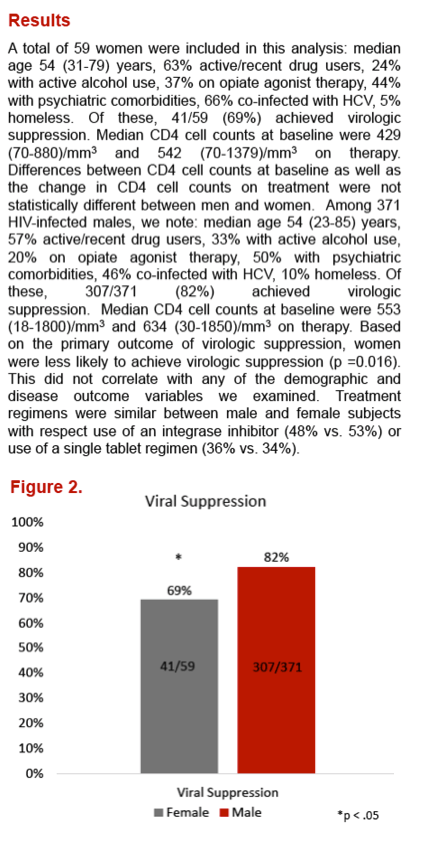
Forty-one of 59 women versus 307 of 371 men achieved virologic suppression, a significant difference (69% versus 83%, P = 0.016). None of the other variables assessed explained the viral suppression difference between women and men. Neither did proportions of women and men taking an integrase inhibitor (48% and 53%) or a single-tablet regimen (36% and 34%).
Ongoing work is addressing other behavioral traits, notably antiretroviral adherence, that may explain the virologic response difference between these Vancouver women and men. In the US Medical Monitoring Project, higher recent viral suppression rates in white men than other groups could be traced to "differences in antiretroviral therapy use and adherence, demographic characteristics, and social determinants of health such as poverty, education, and insurance" [3].
References
1. Magel T, Holeksa J, Thiam A, Truong D, Conway B. HIV-infected women: Medical co-morbidities and rates of virologic suppression. 10th IAS Conference on HIV Science (IAS 2019), July 21-24, 2019, Mexico City. Abstract TUPED749.
2. Crepaz N, Tang T, Marks G, Mugavero MJ, Espinoza L, Hall HI. Durable viral suppression and transmission risk potential among persons with diagnosed HIV infection: United States, 2012-2013. Clin Infect Dis. 2016;63:976-983.
3. Beer L, Mattson CL, Bradley H, Skarbinski J; Medical Monitoring Project. Understanding cross-sectional racial, ethnic, and gender disparities in antiretroviral use and viral suppression among HIV patients in the United States. Medicine (Baltimore). 2016;95:e3171.

|
| |
|
 |
 |
|
|