 |
 |
 |
| |
When To Begin Therapy: deferring therapy may reduce health and longevity
|
| |
| |
There were several interesting studies at the Conference that should stir the controversy around this question even more. The findings from several studies presented at Retrovirus this year suggest that deferring the start of therapy may reduce a person's ability to control HIV. This runs contrary to what many people have heard from a number of studies reported over the last 1-2 years. Evidence does appear to be mounting that delaying therapy may have a negative impact on response to therapy, but side effects and toxicities still can occur. I think these new studies, in addition to prior studies showing similar findings, make a reasonable case that delaying therapy has drawbacks.
So, although starting therapy earlier may improve chance if durable response, this is just another consideration in balancing the reasons for deferring therapy.
When starting therapy early adherence to taking HIV medications for years can be a challenge. Still, new drugs and new classes of drugs are in development. Promising development programs for entry inhibitors were reported at this Conference by Schering Plough and Bristol Myers. The first integrase inhibitors are in the early development stages from Shionogi/Glaxo and Merck. Several NNRTIs and protease inhibitors for resistant virus are in human studies. The risk of lipodystrophy and complications remain, and still must be considered in the decision of when to begin therapy. Although some HIV drugs may be less likely to contribute to body changes.
Over the course of the last several years there has been great controversy about "when to begin therapy". A bunch of studies have showed mixed results. Some show you could delay therapy until CD4 are <350 or perhaps <200 and still be equally able to achieve and sustain undetectable viral load. Most of these studies are of relatively limited followup, several years. Some of these studies have found that perhaps viral load up to 100,000 does not affect outcome-- you could have viral load of up to 100,000 without reducing your chance for achieving and sustaining viral load undetectable. However, a number of additional other studies have found the opposite-that the chance of achieving and sustaining undetectable viral load is improved when starting therapy earlier -- at >350, and chances may be further improved if CD4s are >500; that achieving durable suppression is more likely when viral load is lower; and the lower the viral load and higher the CD4 count leads to incremental benefits. Some of the new studies reported at Retrovirus and discussed below support this.
The collective result of a number of the larger studies over the last 1-2 years, prior to this year's Retrovirus, has been I think that the general public community opinion has accepted that you can delay starting therapy to when cd4s are <500 and perhaps until 200-350 and still have the same chance of delaying achieving and sustaining viral load. The studies suggesting the latter appear to have more appeal. The studies suggesting delaying therapy is a risk were smaller and presented previously. The studies saying deferring therapy will not risk less response were larger, received much more attention, were presented at large conferences more recently, and received more press coverage.
One study at this Retrovirus Conference was from Frank Pallela (Northwestern University) and the CDC found that patients delaying therapy until CD4s count is <350-500 may die earlier; the rate of death was 80% higher (p>0.3). For patients delaying therapy beyond 200-350, the increased risk of death was 3.5 times higher (p<.001). They looked at 800 patients at 8 US clinics. The followup for these patients is only 3-6 years, so this data is considered preliminary. But with continued followup I expect we would see more pronounced results similar to these.
Tim Sterling (Johns Hopkins University) reported that clinical disease progression was slower in persons with durable suppression than in persons without durable suppression when initial CD4 was < 350 (p < 0.0001) but not > 350 (p = 0.94. Among patients with durable suppression, disease progression did not differ between those with initial CD4 level < 50 vs initial CD4 51-200 (p = 0.83) or 201-350 (p = 0.32). The implication of this data to me is that good adherence which translates into durable suppression is the key, but we know that most patients are not fully adherent. Sterling concluded that durable virologic suppression on HAART was associated with decreased disease progression among persons with initial CD4 < 350, but not CD4 > 350, suggesting if you delay therapy until CD4s are <350 perhaps less than full adherence may result in accelerated disease progression compared to starting therapy earlier. Among persons with initial CD4 < 350 who achieved durable virologic suppression, disease progression did not differ among persons with initial CD4 < 50, 51-200, or 201-350. HAART could be initiated at CD4 substantially lower than 350 if durable virologic suppression is achieved. Again, this data suggests that the keys are full adherence and potency of the regimen; if you select a regimen that is potent and effective, and the patient is fully adherent, durable suppression of viral load should occur regardless of the CD4. Read the Abbott study suggesting potency is key.
At Retrovirus, Abbott Labs reported an analysis of their large phase 3 study 863 in treatment-naive patients comparing nelfinavir to Kaletra. Their data suggest lower baseline CD4 and higher viral load are relevant in achieving durable viral suppression. Their data also suggests that using a more potent regimen can improve chances of achieving durable suppression, particularly if baseline CD4 is low & baseline viral load is high. The higher the viral load and the lower the CD4 count the greater the risk of not achieving durable viral suppression. They reported that if therapy is delayed using Kaletra improved the chance of achieving durable viral suppression. They found that if delaying therapy using nelfinavir can result in less capacity to achieve durable viral suppression. Last year Dupont reported findings with efavirenz on when to begin therapy, suggesting similarly regarding the effect of using a potent regimen.
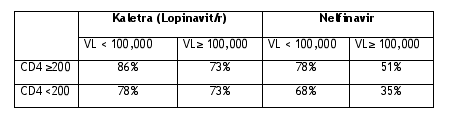
Abbott reported: in a multivariate statistical analysis, lower baseline CD4+ cell count and higher baseline viral load were associated with a higher risk of failure with nelfinavir (P < .05 for each), but neither variable was a statistically significant predictor of the durability of response to lopinavir/ritonavir (P > .2 for each). Week 96 response rates for CD4+ cell count and viral load strata within each treatment group are shown in the table.
|
|
 |
| |
Here is a link to more complete information from the Abbott poster:
If you accept that starting therapy earlier does increase the chance for a durable viral suppression, you still have to consider the impact of the development of lipodystrophy, metabolic abnormalities, and nonadherence after starting therapy. The selection of a particular regimen may affect durability and may increase the risk for lipodystrophy or metabolic abnormalities. The development of body changes (lipodystrophy) may lead some patients to stop therapy or take drug holidays. And the patient may not be willing to tell the doctor about their desire to stop therapy, or ask him/her for advice.
Of course the patient's individual situation and personal desires are still important to consider. There is no equation that spits out a choice for a regimen or an answer to when to begin therapy. But I think these newly reported studies provide patients and providers with important information to aid them in making the decision of when and with what to begin therapy.
The care provider should try to engage the patient in a comprehensive discussion and explanation about this question and the many considerations and long-term implications. However, some patients may prefer to leave the decision to their doctor, which may be risky if your doctor is not familiar with the many considerations and the new studies.
Additional Related Studies at Conference
Patient Adherence Relates to When To Begin Therapy and Nonadherence Increases Death
Starting therapy <200 CD4s increases death rate 4 times
When reading this data you should remember that many patients are nonadherent. This data suggests that for patients who are nonadherent (defined in this study as taking <75% of medications) delaying therapy presents greater risk than starting therapy earlier; particularly when CD4s are low, patients are at greater risk for progression. Julio Montaner and his research group up in Vancouver, Canada reported on 1416 treatment-naive patients who started HAART between 8/96 and 9/99. Cumulative deaths and virologic response rates were estimated using Kaplan-Meier methods. As of September 30, 2000 there were 110 deaths from HIV-related causes for a crude death rate of 7.8%.
Montaner found the experience of the HIV physician affected death:
Among patients with experienced physicians, the cumulative mortality rates at 12 months were 2.9%, 4.6%, and 0.7% for those with baseline CD4 cell counts <50, 50 - 199, and >200,respectively. Conversely, among patients with non-experienced physicians the cumulative mortality rates at 12 months were 17.6%, 9.2%, and 1.1% for those with baseline CD4 cell counts <50, 50 - 199, and >200 respectively.
Using a multivariate statistical analysis, CD4 count before starting therapy and adherence predicted outcome. But, this study did not compare the death rate between patients starting therapy below compared to above 350.
Among patients who received >75% of their prescribed medications during the first year on therapy, the cumulative mortality rates at 12 months were 7.7%, 5.6%, and 0.6% for those with baseline CD4 cell counts of <50, 50-200, and >200, respectively. In contrast, among patients who received < 75% of their medications, the cumulative mortality rates at 12 months were 13.3%, 6.3%, and 1.3% for those with baseline CD4 cell counts of <50, 50-200, and >200 CD4 cells/mm3 respectively.
- The risk of death was 8 times greater if a patient started therapy when CD4 count was <50 compared to starting therapy when CD4 count was >200
(editorial note: Many patients are not adherent. Since it can be difficult predicting whether a patient will be adherent, waiting to start treatment until CD4s are below 200 entails a risk. In patients where adherence appears to be a potential concern, this data indicates it may be crucial for that patient to start therapy earlier. Oftentimes a patient learns about the importance of adherence after they fail their first regimen. They learn why it is important to be adherent, and perhaps this makes them adherent for their subsequent regimens. I suggest this may be a reason for starting therapy earlier. In particular, new drugs are in development and it appears, particularly after this conference, that the pipeline is for new drugs is filled for patients with resistance to the currently available drugs.
Editorial note: Finally, Montaner has previously reported from I think this same study that found that viral load before starting therapy was not relevant to your ability to achieve undetectable. However, it appears to me that he did not consider the numerous variables that affect this outcome. Overall, I do not accept that it is safe to defer therapy until viral load is >100,000 for several reasons. I'm not convinced it's "safe" to defer therapy until viral load is >60,000. This has not been well studied but there may be an increased risk for damaging the immune system & consequent risk for cancers when deferring therapy. The capacity to achieve undetectable viral load (<50) may be at risk if starting therapy with high viral load, which may be affected by the potency of the regimen and the adherence of the patient. And we know that many patients will not be adherent. For the patient will be adherent, the considerations may be different but some of the concerns are the same. Of course, again, drug side effects and toxicities are also important considerations before starting therapy.
Baseline Viral Load Predicts Initial Viral Load Decline (1 week)...
The findings from this next study suggest that if you start HAART when viral load is lower you have a better chance of achieving and sustaining long-term viral suppression. The problem is the study could not prove that better initial suppression, after 10 days, resulted into better long-term suppression. However, when trying to prove this other factors start coming into play, such as: were the patients adherent.
The findings from this study show that the lower your viral load is before starting your first HAART regimen the better your viral load decline should be after the initial 10 days on therapy. It has been suggested that if your viral load declines quickly you are more likely to achieve and sustain a long-term viral load suppression, if you maintain adherence.
Knowledgeable doctors and care providers and the PHHS Guideline recommendations recognize that a patient should achieve a 0.5 log reduction within 2 weeks and a 1 log reduction soon after that. This study tries to prove that a better viral load decline after the first 10 days following the start of therapy translates into better long-term viral suppression. They couldn't prove it. But in my opinion, it appears that a better viral load decline in the first 10 days does result in more likely sustaining of full viral suppression to <50 or 400 copies over the longer term.
The findings from this study indicate that a lower viral load when starting therapy can result in better initial viral load reduction and that ought to translate into better long-term viral suppression. Again, continued adherence is a key to long-term success. It's also important to make sure that patients do not take drugs that result in drug-drug interactions with their HAART regimen. This could also lead to viral failure.
In this study 82 patients enrolled, and 71 were evaluable for viral dynamics studies. The baseline viral load was 60,000 and CD4 count 350.
The schedule for measuring viral loads was: before starting the study drugs,
baseline (days 0), day 3 or 4, day 7, day 10 or 11, and weeks 2, 3, 4, 8, 12, 16, 24, 32, 40, and 48. Patients were randomized to receive standard dosing of abacavir 300 mg twice daily and 1 of 5 protease inhibitors- indinavir (800mg 3x/day), saquinavir (1200mg 3x/day), ritonavir (600mg 2x/day), nelfinavir (750mg 3x/day), or amprenavir (1200mg 2x/day).
The authors concluded:
- The first phase viral decay rates are strongly and negatively correlated with baseline viral load
- The second phase viral decay rates are strongly and positively correlated with baseline viral load
- In addition, the two decay rates are negatively correlated
- Other baseline factors such as baseline CD4 cell counts, CD8 cell counts and the age of patients were not correlated with viral decay rates
- Viral Decay Rates Do Not Predict long-term virologic responses
The definition of virological responses in this study were viral load rebound before week 24 or having viral load above detection limit at week 24 (> 400 copies/ml)).
This study was reported by J. Mellors, M. Lederman, and Glaxo Smith Kline (abstract 466-M).
Less HIV Progression Occurs When Starting Therapy with >350 CD4s and Low Viral Load
Researchers from the University of Washington School of Medicine in Seattle (Kitahata, abstract 467-M) reported from a small study that patients who started therapy with CD4s >350 had lower rates of HIV disease progression. 209 patients were observed for average 29 months (6 to 80 months).
After controlling for the effect of antiretroviral treatment (CD4 & viral load), patients whose CD4 cell count was < 200 cells or 201- 350 cells at the initial clinic visit had higher rates of disease progression (HR= 2.42; P< 0.01; HR= 1.73, P= 0.10) than patients with a CD4 cell count >350.
Patients who started therapy when viral load was >50,000 had greater disease progression or death compared to both patients starting therapy with 10,000 to 49,999 or <10,000. Patients with <10,000 had less progression/death than patients with 10,000-49,000. These differences were not statistically significant.
Disease progression or death occurred in 28% of patients receiving PI or NNRTI- based vs. 46% of patients receiving NRTIs, and 43% of patients who did not receive antiretroviral treatment during the initial observation period
They compared patients who started therapy vs patients who did not. This was a retrospective study in a University-based specialty clinic and included patients whose first clinic visit occurred after PI availability (1995-2001). Patients had no HIV- related clinical conditions (asymptomatic) prior to or during the 6 months following the initial clinic visit (initial observation period).
Most patients were <39 years old; 90% men; 66% caucasian; 63% men who have sex with men; 75% public reimbursement.
27% started a PI regimen (n=58), 15% a NNRTI regimen (n=31), compared to 39% (n=81) who did not start therapy and 19% who started a NRTI regimen (n=39).
26% (n=54) had CD4s >500. 24% (n=51) had 350-500 CD4s. 30% (n=63) had 201-350 CD4s. And, 15% (n=41) had 200 or less CD4s. 30% (n=64) had HIV viral load >50,000. 27% (n=56) had 10,000-49,999. 10% (n=21) had 3,000-9,999. 19& had 50-2,999. 8% had <10,000 (BLQ). And, 6% had <500 BLQ.
The authors summarized that longer term followup is needed to better assess clinical benefit of treatment and that the small size of this study limits the generalizability of the results. Clinical benefit of starting therapy earlier must be balanced with long-term risks associated with antiretroviral medications when making decisions about when to begin therapy.
Effect of Initial CD4 Response On Viral Load After Viral failure
Steve Deeks reported that patients with a greater initial CD4 increase after starting HAART tended to have a greater increase in viral load after virologic failure. He speculated that a large initial CD4 response may increase the number of target cells available for HIV, thus encouraging viral replication.
Total HIV Viral Load Over Time Predicts Death & AIDS Events
In an interesting study from the Swiss HIV Cohort Study (Eggar, abstract 471-M), researchers looked at the amount of viral load a patient has over time and how that might predict disease progression. Eggar examined the area under the viral load curve (AUC) as a measure of average viral burden and assessed its value as a predictor of clinical progression. They also examined cumulative drug exposure. A total of 2,324 patients who started HAART between Sept 1, 1995, and Nov 30, 1998, who had a CD4 count and viral- load measurement within 3 months before starting HAART and at least one follow- up visit were included. The median viral burden over time was log 2.80 (630 copies/ml) copies (interquartile range 2.67 to 3.37).
The risk of progression to a new AIDS event or death was strongly related to viral burden over time. Kaplan- Meier probabilities at 5 years were:
• 7.2% for patients with viral burdens of less than 3.0 log copies/ ml per year,
• 20.6% for viral burdens of 3.0 log to 3.99 log,
• 38.7% for viral burdens of 4.0 log to 4.99 log and
• 79.1% for patients with viral burdens of 5 log or greater
Baseline CD4 cell count, a history of IVDU, and older age also predicted
disease progression, but baseline viral load, clinical stage, treatment history, and sex did not. Drug exposure increased with increasing viral burden.
Viral burden over time was a stronger determinant of clinical progression than viral response in the first year after initiating HAART. Kaplan- Meier probabilities at 5 years:
• 11.0% for patients who achieved and maintained undetectable viral loads,
• 15.9% for patients who achieved undetectable concentrations but had a viral
rebound,
• 51.5% for patients who never achieved undetectable concentrations.
Probability of Progression to New AIDS Event or Death, using Kaplan-Meier curves:
- 22 times greater if average viral load was 100,000 or higher compare to 0 to 2.9 log (1000 copies)
- 6.5 times if average viral load was 10,000 to 100,000, compared to 0 to 2.9 log
- 3.3 times greater if average viral load was 1,000 to 10,000, compared to 0-2.9 log
Abbott Link DATA:
Study Design
Study 863 was a phase III, randomized, double-blind clinical trial comparing the safety and antiviral activity of Kaletra (LPV/r) + d4T + 3TC vs. that of nelfinavir (NFV) + d4T + 3TC in antiretroviral-naive patients. There was no minimum CD4
cell count or maximum viral load restriction in this study. 653 patients were randomized to receive-
• LPV/r 400/100 mg BID + NFV placebo TID + d4T/3TC (n=326) or
• LPV/r placebo BID + NFV 750 mg TID + d4T/3TC (n=327)
Patients were allowed to switch NFV/NFV placebo dosing from TID to BID after FDA approval of the BID dosing regimen, which occurred after all patients reached Week 24. After all patients reached Week 60, patients were unblinded and continued on open-label randomized therapy.
Efficacy
Durability of response for the two treatment regimens was assessed by examining the time to loss of virologic response. This was defined as the first of two consecutive viral load measurements above 400 copies/mL following any value <400 copies/mL. If the final available value was the first rebound value above 400 copies/mL, the patient was considered a virologic failure at that point. Patients who never achieved viral load <400 copies/mL were considered
virologic failures on Day 0. Data through Week 96 are presented in this analysis.
The effects of baseline CD4 cell count and baseline viral load on the time to loss of virologic response were analyzed using the Cox proportional hazards model within each treatment group. Kaplan-Meier response rates through Week 96 were examined within each treatment group by 5 commonly used categories of CD4 cell counts (<50 cells/mm3, 50 to <200 cells/mm3, 200 to <350 cells/mm3, 350 to <500 cells/mm3, and 500 or more cells/mm3) and by approximate quintiles of baseline viral load.
RESULTS
Overall Virologic Response
Through up to 96 weeks of treatment, LPV/r-treated patients demonstrated significantly longer time to loss of virologic response than NFV-treated patients (p<0.001, Cox proportional hazards model, Figure 1).
Time To Loss of Virologic Failure
From week 0 of the start of this study there was a separation between the Kaletra and nelfinavir regimens in terms of virologic failure. Nelfinavir patients started failing at a quicker pace. The trend continued. At week 96, 79% in the Kaletra arm had not failed therapy vs 58% in the nelfinavir arm.
Baseline CD4 Cell Count and Viral Load as Univariate Predictors of Response
The Cox proportional hazards model was used to assess the relationship between baseline CD4 cell count/viral load and virologic response within each treatment group. In univariate analyses, lower baseline CD4 count and higher baseline viral load were statistically significantly associated with a higher risk of failure for NFV-treated patients but not for LPV/r-treated patients (Table 1).
|
|
 |
| |
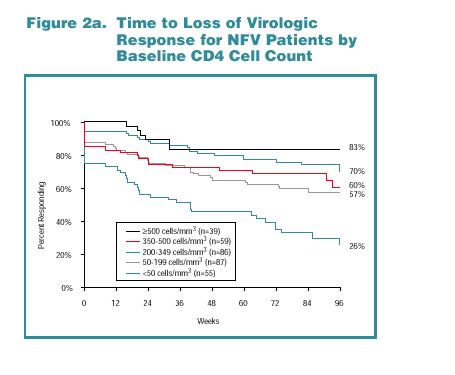
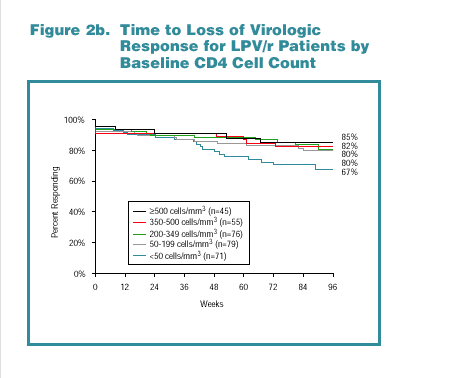
Kaplan-Meier response rates by baseline CD4 cell count category are shown for NFV-treated patients in Figure 2a and for LPV/r-treated patients in Figure 2b.
|
|
| |
 |
 |
| |
| |
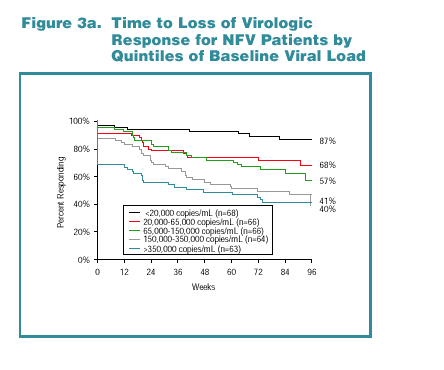
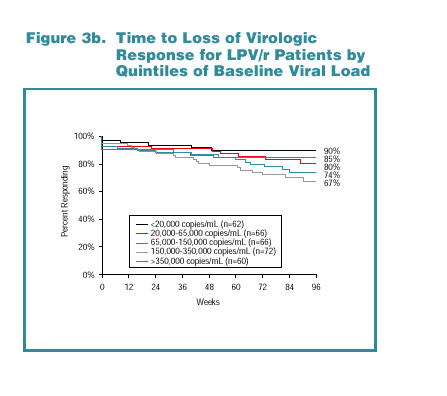
Kaplan-Meier response rates by baseline viral load category are shown for NFV-treated patients in Figure 3a and for LPV/r-treated patients in Figure 3b. Notably, among LPV/r-treated patients, the highest viral load stratum (baseline viral load >350,000 copies/mL) demonstrated the second-highest response rate (85%) through 96 weeks.
|
|
 |
 |
| |
Discussion
In accordance with several previous reports (Staszewski 1999, Paredes 2000, Grabar 2000, LeMoing 2002), this analysis demonstrates that among NFV-treated patients, those with lower baseline CD4 cell counts and higher baseline viral loads had a significantly shorter time to loss of virologic response compared to other patients. In contrast to this, and similar to a
previous analysis of a phase II study of LPV/r, baseline CD4 cell count and viral load did not demonstrate a statistically significant effect on response among LPV/r-treated patients. Differences between treatment groups in the time to loss of virologic response were largest among patients most likely to initiate treatment based on current treatment guidelines. For example, among patients with baseline CD4 <200 cells/mm 3, a group for whom guidelines universally recommend therapy initiation (DHHS 2002, Pozniak 2001, Carpenter 2000), the percentages of patients maintaining response through Week 96 were 74% for the LPV/r group vs. 44% for the NFV group (p<0.001). At CD4 counts above 200 cells/mm 3, guidelines vary, but treatment initiation is generally recommended or considered for patients with CD4 <350 cells/mm3 or viral load >55,000 copies/mL; in this subgroup, the percentages of patients maintaining response through Week 96 were 76% for the LPV/r group and 53% for the NFV group (p<0.001). In some of these analyses of LPV/r-treated patients, a trend toward statistical significance was observed, suggesting that with a longer duration of follow-up, the effect of baseline characteristics on response to LPV/r may become statistically significant. In fact, if the subgroups in Figure 2b are combined so that patients with <50 CD4 cells/mm 3 are compared to
the remaining LPV/r-treated subjects, a statistically significant difference is observed (Week 96 response rates were 67% [n=55] vs. 82% [n=271], p=0.03, Cox proportional hazards model). The relative impact of baseline CD4 cell count on response to other agents, such as efavirenz, indinavir, atazanavir, and indinavir/ritonavir, has been less well characterized, since subjects with very low CD4 cell counts have commonly been excluded from participation in these
trials (Tashima 2001, Sanne 2001, Schranz 2001). Both the risk and the consequences of treatment failure should be considered in evaluating antiretroviral regimens. For example, even if criteria for virologic failure are met, isolated viral "blips" or viral rebound during a temporary treatment
interruption may not represent a "true" virologic failure. In a recent report on the current study (Bernstein 2001), among patients with detectable viral load and available genotype at any time during Weeks 24-96, significantly more NFV-treated than LPV/r-treated patients demonstrated protease inhibitor resistance (43% vs. 0%, p<0.001) and lamivudine resistance (81% vs. 37%, p<0.001) These findings suggest that in addition to the less durable virologic response observed in the NFV group compared to the LPV/r group in this study, response to subsequent treatment regimens for NFV-treated patients may be undermined due to the higher rate of protease inhibitor and lamivudine resistance.
Conclusions
⋅ The effects of lower baseline CD4 cell counts and higher baseline viral load levels on the durability of virologic response to a LPV/r-based regimen were generally nonsignificant.
⋅ Among NFV-treated patients, durability of virologic response was highly statistically significantly associated with lower baseline CD4 cell counts and higher baseline viral load levels.
⋅ Clinical trial designs that do not reflect current guidelines for treatment initiation in antiretroviral-naive patients have important limitations:
- Inclusion of patients with higher CD4 cell counts focuses on a population less likely to initiate therapy and may undermine the ability to detect differences between treatment groups.
Similarly, exclusion of patients with advanced HIV disease, such as those with CD4 counts <50 cells/mm3, may overestimate the treatment effect and decrease the ability to differentiate between treatment regimens.
⋅ Both the risk and the consequences of virologic failure should be considered in evaluating treatment regimens.
Baseline CD4 Cell Count and Viral Load as Multivariate Predictors of Response
The Cox proportional hazards model was used to assess the relationship between baseline CD4 cell count/viral load and virologic response within each treatment group. In a multivariate model, lower baseline CD4 count and higher baseline viral load were statistically significantly associated with a higher risk of failure for NFV-treated patients. Neither variable was significantly associated with response among LPV/r-treated patients (Table 2).
|
|
 |
| |
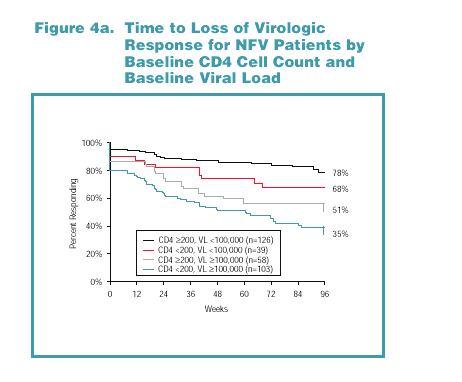
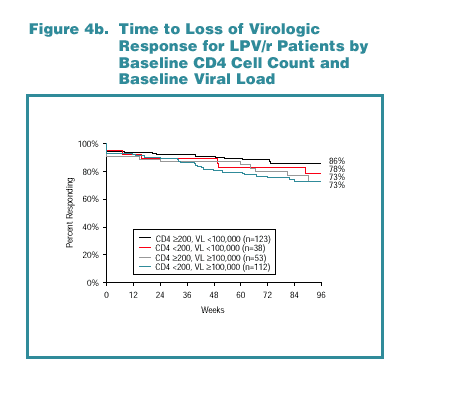
To explore the relationships demonstrated in the analysis shown in Table 2, patients were stratified by baseline CD4 cell count (above or below 200 cells/mm 3) and viral load (above or below 100,000 copies/mL). Kaplan-Meier response rates through Week 96 are shown for each stratum in Figure 4a for NFV-treated patients and Figure 4b for LPV/r-treated patients.
|
|
 |
 |
| |
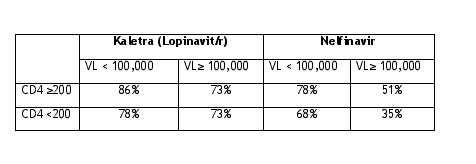
CD4 and Viral Load Predict Ability to be Undetectable - Week 96
This more simple table displays that CD4s and viral load affected the ability to be undetectable at week 96. For patients with viral load above or lower than 100,000 they appeared to respond better to therapy if they started when CD4s were above 200. This was most apparent for patients receiving nelfinavir. Viral load mattered also. Patients with >100,000 viral load when they started therapy were less able to be undetectable. Some of the differences in response may not be statistically significant but appear to show trends. Upon referral to data above the differences are only statistically significant for nelfinavir. The differences for patients taking Kaletra may be too small to be significant. But significance might be reached after additional years of followup.
|
|
 |
| |
|
 |
 |
|
|