| |
Cardiovascular Risk Associated With HIV Therapy: review by Judith Currier, MD
|
| |
| |
Judith S. Currier, MD
Center for AIDS Research and Education, University of California, Los Angeles, Los Angeles, California, USA
JAIDS Journal of Acquired Immune Deficiency Syndromes 2002; 31:S16-S23
A decrease in death rates from HIV infection has reflected the progress made with highly active antiretroviral therapy (HAART), which can suppress viral replication and preserve immune function. At the same time, preliminary evidence suggests that individuals infected with HIV may be at increased risk for cardiovascular disease. This article considers the cardiovascular disease risk associated with HIV infection itself, the role of antiretroviral therapy in lipid disorders and coronary heart disease (CHD) risk, and available strategies to manage dyslipidemia when it occurs.
The implications of dyslipidemia in HIV-infected individuals are not completely known, but the type, incidence, and degree of the abnormalities that are observed with this disease and its treatment may be expected to result in increased cardiovascular morbidity. Both antiretroviral therapies and untreated HIV infection are thought to produce disturbances in lipid levels. Insulin resistance, another CHD risk factor, may also be directly associated with the use of antiretroviral drugs. Lipid abnormalities and insulin resistance have an unproven but possible association with lipodystrophy, the abnormal fat redistribution observed in many patients receiving HAART therapy. Other
cardiovascular risk factors may include chronic inflammation accompanying the ongoing viral infection and endothelial dysfunction. Large studies are currently underway to determine the incidence of cardiovascular events and
atherosclerosis in HIV-infected individuals and the relative contribution of the identified risk factors, but because these are necessarily long-term studies, the data will not be available any time soon to inform current treatment
recommendations. Consequently, preliminary recommendations for the management of dyslipidemia in HIV-infected individuals should be developed from existing guidelines applicable to the general population.
VIDENCE OF RISK: SUBCLINICAL ATHEROSCLEROSIS
A number of studies have investigated the relationship between antiretroviral therapy and subclinical atherosclerosis. Several have used ultrasound to detect arterial wall changes. In a study of 102 HIV-positive patients, ultrasonography detected a higher prevalence of carotid artery lesions in the 55 patients who had received protease inhibitor (PI) therapy for at least 12 months than in the 47 HIV-positive patients who were receiving PI-sparing therapy
or who were treatment naive. The ultrasound results in the HIV-infected patients were also compared with those obtained from healthy subjects. Endothelial lesions were found in 29 of 55 patients (52.7%) receiving PI therapy and in 7 of 47 patients (14.9%) not on therapy or not receiving PIs. Thickening of the carotid artery intima was detected in 7 of 104 healthy controls (6.7%), but no atheromatous plaques were observed. Statistical analysis indicated a significant correlation between the presence of endothelial lesions and age, male sex, and hypercholesterolemia. PI therapy, smoking, and Centers for Disease Control and Prevention (CDC) stage of disease were the patient characteristics predicting increased risk of vascular lesions (p = .011, p = .022, and p = .017, respectively).
A second ultrasound study evaluated the presence of plaques in the femoral and carotid arteries of 68 HIV-negative and 168 HIV-positive individuals, 136 of whom had received PI therapy for an average of 26.8 months. Arterial plaques
were found in 93 of 168 HIV-infected patients (55%) and in 26 of 68 control patients (38%; p = .02). HIV infection, male gender, elevated low-density lipoprotein (LDL) cholesterol, older age, and smoking were associated with the
presence of plaques by univariate analysis, but the association with HIV infection did not persist in multivariate analysis. A further analysis compared the 136 HIV-infected patients receiving PI therapy with 32 non-PI-treated patients. PI therapy correlated with higher plasma lipid concentrations, and the percentage of patients with plaques was higher among HIV patients receiving PI therapy (57%) than among those not treated with PIs (50%; p = .05). However, neither univariate nor multivariate regression analysis indicated a relationship between plaque formation and PI therapy. This investigation showed that although the overall risk of plaque development might be higher in HIV-infected individuals, traditional cardiovascular risk factors are associated with plaque formation in both HIV-infected and non-HIV-infected individuals.
Several additional techniques have been used to evaluate the early signs of the atherosclerotic process in patients with HIV infection. Electron-beam computerized tomography can detect coronary calcification indicative of atherosclerosis. However, in a small pilot study in 17 HIV-positive patients who had received PI therapy for 17 to 30 months, only 5 subjects had abnormal calcium scores. In another study, a difference in the incidence of abnormal calcification was not observed between HIV-positive patients overall and those receiving PI therapy. In contrast, measurements of plasma lipids and flow-mediated vasodilation (FMD) in the brachial arteries of 37 adult HIV patients revealed a direct association between PI-induced plasma lipoprotein changes and endothelial dysfunction. Patients in the PI group had higher mean total cholesterol levels than patients receiving non-PI therapy, 220 ± 70 mg/dL vs. 171 ± 51 mg/dL, respectively (p = .007), and higher triglyceride levels, 392 ± 461 mg/dL vs. 175 ± 116 mg/dL (p = .009). Although brachial artery diameters were similar in both groups, subjects receiving PI therapy had impaired FMD, their values (2.6 ± 4.6%) contrasting with the normal values seen in the patients receiving non-PI therapy (8.1 ± 6.7%; p = .005), indicating endothelial dysfunction.
| |
 |
| |
RATES OF CORONARY HEART DISEASE
Because PIs are still relatively new, it may be too soon to confirm an association between PI-induced lipid levels and the incidence of CHD. In a preliminary report of 4541 HIV-positive patients in the Kaiser Permanente Northern California HMO database, who were followed for a median of 4.3 years, 53 hospitalizations for CHD were observed. The calculated incidence rate reported in 2001 was 5.2 per 1000 patient-years (confidence interval [CI]: 2.7, 7.7) of follow-up for non-PI-treated patients and 5.8 per 1000 patient-years (CI: 3.4, 8.2) of follow-up for PI-treated patients. The incidence rate was 2.8 per 1000 patient-years among the 41,000 random age- and sex-matched HMO members who were not known to be HIV positive, a 60% difference (7). The follow-up data show a higher overall rate for HIV-positive individuals in general but not for PI-treated patients in particular, suggesting that HIV infection per se may play a significant role in CHD.
An analysis of the French Hospital Database on HIV, containing patient chart data from 68 hospitals and 19,795 men receiving PI therapy, totalling nearly 37,000 patient-years of follow-up, found 54 incidences of myocardial infarction
(MI). Of these 54 MIs, 23 occurred in patients treated with PIs for less than 18 months, 18 occurred in subjects exposed to PIs for 18 to 29 months, and 13 occurred among individuals treated for 30 months or more. The calculated incidence rates were 8.9 ± 1.9, 19.2 ± 4.5, and 34.7 ± 9.6, respectively. The expected incidence in the general population of the same gender and age was 10.8 per 10,000 patient-years, similar to that in patients exposed to PIs for 18 months. Standard mortality ratios, controlled for background risk factors shared in the HIV-infected groups, were 2.0 for the patients receiving PIs for 18 to 29 months and 3.7 for the patients receiving PIs for 30 months or longer. There were thus relatively few MIs in this group of patients, but the results suggest a relationship between the duration of exposure to PIs, MI, and mortality, with a higher incidence among patients exposed for 18 months or longer.
In the HIV/Outpatient Study (HOPS), 15 MIs were observed among 5676 patients. Of these events, 13 occurred in patients treated with PIs, and only 2 occurred in patients not exposed to PIs. Although MI events were rare, PI use
correlated strongly with the incidence of MI. The MI odds ratio adjusted for age and the presence of other risk factors (including smoking, hypertension, and diabetes) was 4.92 (95% CI: 1.3, 32.3). Collectively, these preliminary data
suggest that PI exposure in the setting of other cardiovascular risk factors may be associated with an increase in rate of MI, but that the overall rates remain very low.
ANTIRETROVIRAL THERAPY WITH DYSLIPIDEMIA
The abnormalities in blood lipid profiles associated with HAART may be secondary to central adiposity and insulin resistance, or they may be the result of the effects of antiretroviral therapies on lipids, independent of other metabolic changes related to HIV infection or its treatment. Current PIs vary in their ability to cause dyslipidemia, whereas non-PI-containing regimens have generally been found to have less of an effect on lipids. Various studies have
investigated the association between PI therapy and dyslipidemia.
A study in 21 healthy volunteers showed the effects of the PI ritonavir on plasma lipids to be independent of any effects that might be mediated by HIV itself. The 21 patients were randomized to receive either placebo (n = 8) or ritonavir 300 mg, 400 mg, and 500 mg twice a day on study days 1, 2, and 3 through 14, respectively (n = 13). After 14 days of treatment with ritonavir, mean total cholesterol levels had increased from 169 ± 11 mg/dL at baseline to 209 ± 16 mg/dL (p < .001), and triglyceride levels had increased from 110 ± 12 mg/dL at baseline to 270 ± 60 mg/dL (p < .01). No changes in these levels occurred in subjects receiving placebo.
An investigation of 93 patients in the Swiss HIV Cohort Study who received ritonavir (n = 46), indinavir (n = 26), or nelfinavir (n = 21) found differential effects on plasma lipid concentrations associated with each of the PIs; specifically, the changes observed with ritonavir were larger than those seen with either of the other two drugs, especially with respect to triglycerides. The analysis included data from 28 patients who were not receiving PI therapy who served as a comparison group. The mean duration of PI treatment for patients in the study was 470 ± 22 days. No changes in high-density lipoprotein (HDL) cholesterol concentrations occurred during the period of evaluation. Baseline levels of total, HDL, and LDL cholesterol did not differ among the PI-treated patient groups, but PI-naive patients had higher baseline HDL cholesterol levels (46 ± 4 mg/dL vs. 39 ± 0.0 mg/dL, p = .05). The increase in total cholesterol was 77 ± 12 mg/dL with ritonavir, 31 ± 8 mg/dL with indinavir, and 46 ± 0.8 mg/dL with nelfinavir, compared with 4 ± 8 mg/dL in the PI-naive group. The analysis also assessed the proportion of patients in each treatment group at the end of the study who had total cholesterol levels greater than the 240-mg/dL threshold for increased incidence of CHD in epidemiologic studies. These proportions were 44% of patients in the ritonavir group, 35% in the indinavir group, 33% in the nelfinavir group, and 14% among PI-naive patients. The greatest increases in triglyceride levels occurred in patients receiving ritonavir. Finally, whereas only 1 patient had a highly atherogenic lipid profile (total cholesterol >240 mg/dL, triglycerides >204 mg/dL, and HDL cholesterol <35 mg/dL) at baseline, this profile was found in 9 of 46 ritonavir patients (20%), 2 of 26 indinavir (8%), 1 of 21 (5%) nelfinavir patients, and 1 of 28 (4%) PI-naive patients at study end.
Combination treatment with lopinavir/ritonavir also results in elevated lipids. In a study of 100 patients receiving the lopinavir/ritonavir combination, the mean increases in total cholesterol (49 mg/dL) and in triglycerides (111 mg/dL) were both significant at week 48 compared with baseline values. In 68% of the patients (56/82) who had baseline total cholesterol levels <200 mg/dL, the levels did not rise above 240 mg/dL during the 48 weeks of the study, and in 73% of the patients with baseline triglyceride levels <250 mg/dL, these values remained below 400 mg/dL. Genetic factors may predispose some patients to the lipid-elevating effects of HIV drugs.
The dyslipidemia associated with PIs, however, may not be class specific. An investigational PI, atazanavir, has not shown the same lipid effects. Changes in both fasting LDL cholesterol and triglyceride levels seen in a phase II study
comparing atazanavir and nelfinavir in 464 patients were significantly smaller for atazanavir. Median changes in total cholesterol at 24 weeks were +2.97 mg/dL for the atazanavir group and +28.94 mg/dL for the nelfinavir group. At
16 weeks, median changes in LDL cholesterol were -4.99 mg/dL and +27.99 mg/dL for atazanavir and nelfinavir, respectively. Also at 16 weeks, triglyceride levels had fallen by a median of 3 mg/dL in the atazanavir patients but had increased by 30 mg/dL in the nelfinavir patients.
Antiretroviral regimens that do not include PIs generally have smaller effects on lipid profiles. With nevirapine, a nonnucleoside reverse transcriptase inhibitor (NNRTI), favorable changes in lipid profiles were seen in a subset of 31
patients enrolled in the Atlantic Study who were receiving this agent in combination with stavudine and didanosine. After 24 weeks, increases in HDL cholesterol levels and in particle size and a decrease in the total cholesterol/HDL cholesterol ratio were observed in the nevirapine arm but not in patients receiving either indinavir or lamivudine along with stavudine and didanosine. Experience with efavirenz has also shown a rise in HDL cholesterol levels after initiation of therapy.
PATIENT EVALUATION AND RISK ASSESSMENT
Preliminary guidelines for the management of dyslipidemia in HIV infection have been published by the AIDS Clinical Trials Group. Management of dyslipidemia and cardiovascular risks in patients with HIV should employ a number of preliminary assessment tools and possible plans of action. Along with routine testing of plasma lipids and glucose, blood pressure should be regularly measured. An assessment of the 10-year CHD risk should be calculated using risk calculators available in the revised National Cholesterol Education Program (NCEP) guidelines. The level of background cardiovascular risk should be considered when initial antiretroviral regimens are chosen. Intervention with
lipid-lowering agents, aspirin, and antihypertensive drugs might be considered based on established thresholds for adults not infected with HIV. Finally, potential drug interactions should be anticipated and avoided.
In the absence of adequate information from clinical studies in HIV patients, the best source of guidance for the management of dyslipidemia is the NCEP guidelines. The Adult AIDS Clinical Trials Group (ACTG) Cardiovascular Focus Group guidelines recommend treating dyslipidemia secondary to either HIV infection or HIV infection treatment according to current NCEP guidelines, with emphasis on the caveat that drug-drug interactions be avoided.
PDF format of ACTG Metabolic Complications Guides is available for you to download at the NATAP website Lipodystrophy Section:
www.natap.org/lipo.htm
The primary target of therapy, according to NCEP guidelines, is the LDL cholesterol level, because LDL elevations have been consistently implicated as a major cause of CHD. Recent clinical trials have clearly shown that lowering LDL cholesterol reduces CHD risk. The NCEP classification of cholesterol and triglyceride levels is given in Table 3. Additional factors are known to increase CHD risk at any LDL cholesterol level, including smoking, hypertension, HDL
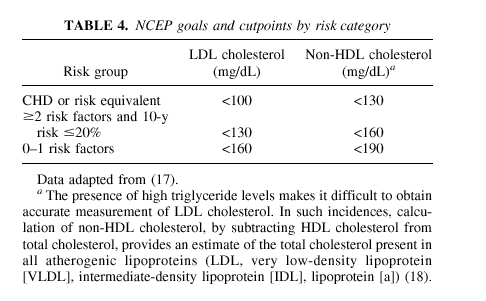
cholesterol below 40 mg/dL, family history of premature CHD, and age. The current NCEP recommendations for intervention are based on the presence of additional risk factors and either LDL or non-HDL cholesterol levels (Table 4). If fasting triglyceride values are in excess of 400 mg/dL, the calculation of LDL cholesterol will be unreliable. The non-HDL cholesterol level is calculated by subtracting the HDL cholesterol value from the total cholesterol value,
yielding the total of all atherogenic cholesterol-containing lipid components. The NCEP recommends non-HDL cholesterol as a secondary therapy target for individuals whose triglyceride levels are [ge]200 mg/dL.
New features of the NCEP Adult Treatment Panel III (ATP III) report are summarized in Table 5. The most significant changes include recognition of multiple metabolic risk factors as criteria for interven-tion. Specifically, the
presence of diabetes mellitus is now considered equivalent to the presence of CHD in calculating CHD risk, as is the presence of peripheral artery disease, symptomatic carotid artery disease, and abdominal aortic aneurysm.
Metabolic syndrome is also included as a secondary target of risk-reduction therapy, after LDL cholesterol. This syndrome consists of a constellation of symptoms including abdominal obesity, triglyceride levels [ge]150 mg/dL,
hypertension, insulin resistance, and low HDL cholesterol. The metabolic syndrome is of particular interest because of similarities with many of the clinical features of lipodystrophy seen in patients receiving HAART.
| |
 |
| |
MANAGING DYSLIPIDEMIA IN THE SETTING OF HIV INFECTION
In HIV-infected patients with elevated cholesterol or triglyceride levels, nonpharmacologic interventions should be tried first unless the patient has existing CHD or total cholesterol levels >400 mg/dL. These interventions are the same as those recommended for HIV-negative individuals and include smoking cessation, limitation of alcohol intake, instituting a low-fat diet, and increasing exercise (16). Dietary supplements may also be helpful. Omega-3 fatty acid supplements decrease triglyceride synthesis and may be effective in reducing triglyceride levels. Niacin is effective in reducing triglycerides, but the side effects-flushing, pruritus, and insulin resistance-make it undesirable as a first-line therapy.
Because lipid disturbances are less pronounced with non-PI-antiretroviral agents, switching from a PI-based regimen may lessen the chance of incurring dyslipidemia. In NNRTI-naive patients, substituting nevirapine or efavirenz for PI therapy resulted in improvements in plasma lipid levels. A switch to abacavir has also been shown to improve lipid profiles; however, it may also result in treatment failure in the setting of prior nucleoside failure.
| |
 |
| |
The fibrates, gemfibrozil and fenofibrate, are effective in reducing triglyceride levels and also in increasing HDL cholesterol. In addition, they increase concentrations of lipoprotein lipase and are somewhat effective in lowering LDL cholesterol. These agents are not expected to interact with PIs in the treatment of patients with HIV. Fenofibrate may have fewer side effects and be more effective in lowering LDL cholesterol; however, the data are sparse, and no comparative study of the two fibrates in patients with HIV has been performed. A recent randomized, blinded study, however, evaluated gemfibrozil in combination with a low-saturated-fat diet for reduction of elevated triglyceride levels in 36 male HIV patients receiving PI-containing therapy. After 12 weeks of treatment, patients taking gemfibrozil
had lowered their triglyceride levels (-118 mg/dL), whereas triglyceride levels were increased in placebo patients, whose sole means of lipid lowering was the diet (+33 mg/dL). Although this difference approached statistical significance (p = .06), only one patient's triglyceride levels returned to normal. Gemfibrozil thus had an effect in these patients, but it may not be one that confers long-term clinical benefit.
HMG-CoA reductase inhibitors, or statins, are the standard of care for lowering cholesterol levels in the general population. Some studies with these agents have been performed in HIV patients. The effectiveness of pravastatin plus
dietary advice was evaluated in 31 male patients in an open-label, 24-week trial comparing this treatment with dietary advice alone. All of the patients had baseline viral loads <500 copies/mL and total cholesterol levels >252 mg/dL and were receiving PI-containing therapy. By week 24, total cholesterol in the group receiving pravastatin plus dietary advice had decreased by 46 mg/dL (17.3%), which was a statistically significant decrease compared with baseline (p < .05). In the group receiving dietary advice alone, the reduction was 12 mg/dL (4%). The difference between the two treatment arms approached statistical significance (p = .051). The change observed in total cholesterol in each group was based completely on decreases in LDL cholesterol. HDL cholesterol rose by 23 mg/dL in both groups, but this
increase was not statistically significant.
Although atorvastatin is generally not used alone for the treatment of elevated triglycerides, there is evidence that both atorvastatin monotherapy as well as atorvastatin in combination with gemfibrozil are effective in lowering total
cholesterol and triglyceride levels in HIV-infected patients receiving PI therapy. Caution has been advised, however, regarding the combined use of fibrates and statins because of the risk of myopathy.
Drug-drug interactions between statins and PIs are important to consider when choosing a statin to treat dyslipidemia in patients receiving PI therapy. All PIs interact with the cytochrome P450 (CYP) system, which metabolizes the majority of statins. The potential for significant drug-drug interactions precludes the use of most statins in patients treated with PIs. Because of extensive metabolism by CYP, lovastatin and simvastatin are not recommended at all for lipid-lowering therapy in PI-treated patients. Pravastatin is the only statin that is not significantly metabolized through the CYP system, and thus its use in PI-treated patients is not likely to lead to deleterious drug interactions with PIs. Table 7 summarizes the currently available statins and comments on their use in HIV-infected patients.
SUMMARY
Current evidence suggests that HIV infection and HAART regimens have the potential to increase the risk of atherosclerosis and CHD. The magnitude of the increase is not well defined at present. Currently available PIs can cause
dyslipidemia that is prompt, marked, and sustained. In the absence of adequate data from HIV-infected individuals, the ACTG Cardiovascular Focus Group guidelines recommend treating PI-associated dyslipidemia according to current NCEP recommendations, with the caveat that drug-drug interactions be avoided. Diet and exercise interventions should be considered and studied further in patients infected with HIV. Cardiovascular risk assessment should also be incorporated into routine HIV care, and initial regimens should be individualized accordingly, with consideration given to the potential lipid effects of the proposed therapy. Statins and fibrates should be used with caution until more data on their efficacy in this patient population are available. New agents for the treatment of HIV infection that do not contribute
to dyslipidemia are likely to improve the current situation. In this regard, atazanavir seems to hold promise. Further research in this area is strongly warranted.
| |
| |
 |
 |
|
|
|