 |
 |
 |
| |
Cardiovascular Disease in HIV
Written by Carl J. Fichtenbaum, MD
Associate Professor of Clinical Medicine
University of Cincinnati College of Medicine
|
| |
| |
At this year's Retrovirus Conference (Feb 10-14, 2003, Boston, MA) at Oral Session 26 there were four important talks on the risk of cardiovascular disease. The first two covered epidemiology of cardiovascular disease and the latter two were focused on progression of atherosclerosis.
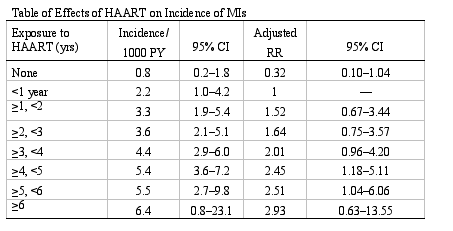
The first talk (abstract 130) presented the initial results from the D:A:D study. This highly anticipated study is the first prospective, observational trial specifically designed to answer the question of whether protease inhibitors and/or potent antiretroviral therapy is associated with a greater risk of myocardial infarctions. The study was specifically powered to demonstrate a 2-fold increase in the risk for MIs (100 incident MIs = minimum event number). This is a collaborative study involving 11 patient cohort groups from Europe, Australia and U.S. (n=23,490 subjects). Friis-Moller and colleagues reported results after 1 year of observation. Enrollment began in July 1999 through April 2001. Follow up was completed by February 2002. The overall median age was 39 years; 76% were men; and 60% had reported lifetime smoking history. Any use of PIs was reported by 67%, median 2.6 yrs duration. During 36,479 patient-years follow up, 129 MIs developed according to WHO criteria (note: 45% were definite; 55% were possible MIs). Of these, there were 36 fatal MIs. The overall incidence was 3.5 per 1000 PYRs. 114 of those affected were men and the median age was 48 years.
|
|
 |
| |
There were several multivariate models created:
- Age, male gender, prior CHD, ever smoker, and CART - current potent antiretroviral therapy (risk: 1.26 per year, 95% CI 1.12-1.41) are associated with MI, adjusted for family history, BMI, HIV risk factor, cohort, and race.
- The second model adjusted for the above risk factors showed that total
cholesterol (Relative Risk=1.16, 1.04-1.30) & diabetes mellitus (RR=2.35, 1.36-4.05) were associated with MI, whereas triglycerides & blood pressure were not. Curiously, lipodystrophy (self-defined) was inversely correlated with MI (RR=0.61, 0.39-0.95), (note from Jules Levin: this finding was puzzling to all observers at the conference as well as the presenter I think. The finding was that persons with lipodystrophy were not at risk for MI if they had lipodystrophy).
The authors concluded that HAART was associated with a 27% relative increase in the rate of MI per year of exposure over the first 7 years of use.
This is a very powerful cohort specifically designed to answer the question of whether HAART increases the risk of MI. This is in contrast to the widely quoted study by Bozzette et al (NEJM, 2003) that was a retrospective review of the VA database that did not find any association between PI use and MIs. It is important to note that study design is critical. Some weaknesses of the D:A:D study include the definitions of MI (many cases were possible); prior CHD was not characterized well in the presentation and may play a larger role in influencing the event rate; some of the sites have not obtained fasting lipid levels confounding interpretation; and the definition of smoking is not standard. Nevertheless, despite these shortcomings, this remains the most powerful cohort study designed to answer this question and these results suggest that HAART is associated with a greater risk for MI.
More perspectives by david Wohl on Lipodystrophy, cosmetic surgery (New Fill for facial fat loss), bone studies (Fosomax for bone loss), buffalo humps & the FRAM Study, and Metabolics at the Retrovirus Conference and on the D:A:D Study:
http://www.natap.org/2003/Retro/day44.htm
And....
Heart to HAART, perspectives on these cardiovascular risk studies in HIV by Judith Aberg:
http://www.natap.org/2003/Retro/day19.htm
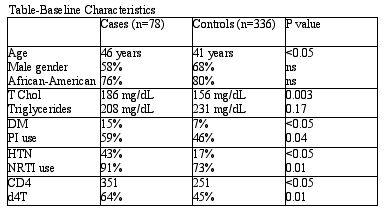
A second cohort study (retrospective) from the Johns Hopkins Database (Abstract 132) was presented by Moore and colleagues. This was a case-control study (5 controls per case matched by date of enrollment and duration of follow up). Subjects without CHD and CVD risks were randomly selected as controls. Criteria for entry included > 90 days of use of antiretrovirals. Data on use of cigarettes was not available. Of the 2,671 patients followed for 7,330 person-years after January 1, 1996, there were 43 CHD events: 5.9 event/1000 PYRs; and 37 CVD events: 5.0 events/1000 PYRs. In contrast, event rates from NHANES data (persons without HIV) were lower, respectively: 2/1000 PYRs and 3/1000 PYRs.
|
|
 |
| |
In the multivariate model, age (RR=1.18), hypertension (RR=3.18), total cholesterol (RR=1.4) and d4T use (RR=2.51) were independently associated with CHD/CVD. PI use was not independently associated (RR=1.61, 0.92-2.77). No data was available on the nadir CD4.
The authors conclude that event rates are higher than NHANES data but no clear association demonstrated with protease inhibitors. They also suggest that NRTIs may be a factor along with other known CHD risk factors. This study is hampered by design where data collection for known cardiovascular risk factors was not standardized. Further, there was no difference in the HIV-1 RNA levels between cases and controls suggesting that adherence to therapy may be hard to track thus confounding conclusions about antiretroviral therapy use. Retrospective, case-control studies are limited in their ability to generate conclusions.
The last two studies evaluated carotid intima thickness, a proxy measure for progression of atherosclerosis in the HIV-uninfected population. Carotid IMT has been shown in 5 independent studies to be predictive of clinical cardiovascular events in both asymptomatic as well as symptomatic individuals.
The first study was by Currier et al (Abstract 131). In this prospective study, triads (total 45 triads, 135 subjects) were created of HIV infected persons taking PIs for ≥ 2 years; HIV infected persons not taking PIs; and HIV seronegative controls. Each triad consists of 3 persons: an HIV-infected person taking a PI (median
duration of PI use was 216 weeks); an HIV-infected person not taking PI; an
HIV-negative person. Patients in this study will be followed over time. The
data presented here is the baseline data for the beginning of the study.
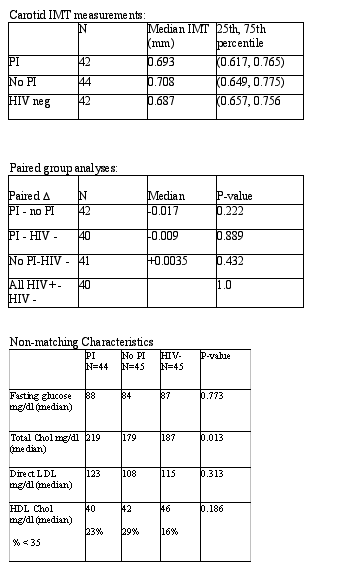
Each triad was matched by cardiovascular risk factors: Age within 5 years; Race; Sex; Blood pressure status (either normal or hypertensive); Smoking status (never, current, or former); Menopausal status. The objectives of this study were: To compare differences in baseline intima-media thickness of the carotid artery between HIV-infected subjects on PI therapy and subjects not receiving PI therapy; To compare differences in baseline IMT between HIV-infected and HIV-uninfected subjects; and To examine predictors of baseline IMT. Subjects were excluded if they had a family history of MI, diabetes mellitus, prior CHD or uncontrolled hypertension. Carotid IMT was measured at the point of laminar flow.
Matching Characteristics for PI group; No PI group and HIV negative group: % men were well matched (91%, 89% and 89%, respectively); white race (77%, 76%, 76%, respectively); median age (42, 41 & 42 years, respectively); and smoking (never=55%, 56%, & 56%, respectively / current=23%, 22% & 22%, respectively).
|
|
 |
 |
| |
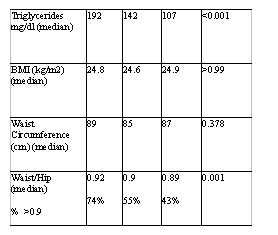
In the Univariate analyses age (per yr) P=0.001; HDL cholesterol (per 10-unit increase) P=0.02; waist circumference (per 1-cm increase) P=0.02; and BMI P=0.004 were all associated with higher Carotid IMT.
|
|
 |
| |
The authors conclude that in this baseline analysis of a matched cohort, controlling for known CV risk factors, PI-treated patients (median duration 216 wks) did not have increased values for carotid IMT when compared to HIV-infected patients not on PI or to HIV-uninfected controls.
Factors associated with increased IMT in multivariate analysis included low HDL cholesterol, elevated TG (when HDL was low), older age, and increased BMI. PI-treated patients were more likely to have increased total cholesterol, TG, and low HDL compared to the other 2 groups, but we were not able to show an association between these lipid changes and increased carotid at this baseline analysis. Longitudinal follow-up of this cohort is ongoing to assess changes in IMT over time.
This is a very important study that was well-controlled, done in a highly respected laboratory that has produced two other major studies of Carotid IMT. One factor that is curious is the greater thickness of all cohorts compared to other published trials of similar persons. The thickness of these measures corresponds with those seen in trials of persons with known coronary artery disease. Nevertheless, this provides some reassurance that short-term use of PIs in low risk patients did not accelerate development of atherosclerosis.
The last study was from SFGH, Dr. Hsue and colleagues (Abstract 139lb). This was a prospective longitudinal study of 106 subjects on PI based ART at baseline. The first 22 subjects have been followed for one year. The objective was to determine the predictors of IMT progression. The Carotid IMT was measured at 6 different points and the average IMT was a summation of those points. The mean age was 45; 83% male; median duration of known HIV was 11 years; median CD4:=354; median PI use=4 years.
The baseline mean carotid IMT: 0.90 + .27 mm
Predictors of >IMT included: Age, LDL, HTN, and Nadir CD4 <200.
Factors that were not predictive were CRP, fibrinogen, HDL, TG, or duration of HIV.
The Mean IMT progression was 0.1mm/yr. 41% of this subgroup had HTN.
Predictors of progression were Age and duration of PI use.
The authors concluded that traditional risk factors and nadir CD4 were associated with higher Carotid IMT indicating that HIV disease may play some role. There was progression with PI use. One disturbing factor in this study was the Carotid IMT measurement was very high. It is not clear if there is a problem with the methodology. It would be difficult to believe progression rates of 0.1 mm/year which are indicative of severe atherosclerosis.
How do we resolve the disparate findings of these latter two studies? The exclusion of subjects with diabetes or a family history of CHD, and the closely matched groups studied may explain why Currier's results (ACTG A5078) results differ from other studies that have suggested an impact of PI use on development of atherosclerosis. Of note, the baseline findings in Currier's study do not preclude an impact of therapy-related lipid changes on carotid IMT over longer periods of time (note from Jules Levin: baseline values mean this study is just getting started and patients will be followed. Over years we may see different results, as this shorter term follow-up may be too brief to see increased carotid IMT). Differences in the Carotid IMT measurement (Currier measured at site of laminar flow; Hsue (SFGH) measured six points at turbulent flow on each carotid and then took average) may also explain disparate findings.
Based upon the results of these studies the assessment and management of cardiovascular risk factors should still be recommended in HIV-infected patients in a manner similar to the general population. More carefully controlled, longitudinal studies are needed to resolve this debate.
|
|
| |
|
 |
 |
|
|