 |
 |
 |
| |
Body Changes, Diabetes, Fatty Liver & HIV & HCV
|
| |
| |
Reported by Jules Levin
Here are a series of studies reported at the AASLD liver meeting just completed in Boston (Oct 29-Nov 2, 2004) which address issues related to lipodystrophy, insulin resistance, fatty liver & increased mortality. Although this is a liver conference many of these issues are of direct relevance to HIV+ individuals. HAART and diet can lead to lipid abnormalities & insulin resistance. In addition to increased risk for heart disease, these conditions are also associated with advancing liver disease. A study below by Don Kotler discusses increased risk for lipoatrophy on HCV therapy IFN/RBV. A study below by Jacqueline Capeau finds people with HIV lipodystrophy are more likely to have fatty liver, which is associated liver disease. In HCV, fatty liver & diabetes is associated with liver disease. There is no reason that these conditions should affect HIV+ individuals any differently. People with both HIV & HCV or HBV appear at double the risk for body changes, fatty liver, diabetes, and increased risk for advancing liver disease & reduced response to interferon therapy for HCV. Studies show that patients with fatty liver have a reduced response rate to interferon/ribavirin therapy for HCV.
STEATOHEPATITIS (fatty liver) IS ASSOCIATED WITH INCREASED HEPATIC EXPRESSION OF SREBP-1 IN HIV-INFECTED PATIENTS WITH ANTIRETROVIRAL THERAPY-LINKED LIPODYSTROPHY
Maud Lemoine, Véronique D Barbu, Jean Philippe Bastard, INSERM U402/Université Pierre et Marie Curie, Paris, France; Dominique Wendum, Service d'Anatomo-pathologie, Hôpital Saint-Antoine, Paris, France; Mustapha Maachi, INSERM U402/Université Pierre et Marie Curie, Paris, France; François Paye, Service de Chirurgie Viscerale, Hôpital Saint-Antoine, Paris, France; Raoul Poupon, Service d'Hépatologie, Hôpital Saint-Antoine, Paris, France; Pierre-Marie Girard, Service de Maladies Infectieuses, Hôpital Saint-Antoine, Paris, France; Chantal Housset, Jacqueline Capeau, INSERM U402/Université Pierre et Marie Curie, Paris, France; Lawrence D Serfaty, Service d'Hépatologie, Hôpital Saint-Antoine, INSERM U402/Université Pierre et Marie Curie, Paris, France
Lipodystrophy is a frequent side effect of antiretroviral therapy in HIV-infected patients. Due to the association with insulin resistance, lipodystrophic patients are at risk of steatohepatitis. PPARs and SREBP-1, transcription factors involved in hepatic glucose and lipid metabolism, are presumed to play a role in steatosis. In rodents, treatment with the protease inhibitor ritonavir causes increased hepatic expression of SREBP-1 and steatosis. We therefore examined liver pathological changes and expression of PPARα, PPARγ1, γ2 and SREBP-1 in HIV-infected patients with lipodystrophy.
Methods: Three groups of patients were studied. Group 1: 9 HIV patients with lipodystrophy (median age 43, male sex 8, CD4 355, BMI 23), under antiretroviral therapy (including ritonavir in 5, nelfinavir in 3), alcohol intake lower than 20g/d, without HBV or HCV infection, who had liver biopsy because of elevated transaminases; Group 2: 9 patients with NAFLD, age and BMI matched with Group 1 (median age 43, male sex 5,BMI 24); Group 3: 10 controls without steatosis who underwent liver surgery (median age 59, male sex 8, BMI 23.6). All patients had determination of serum fasting glucose, insulin, triglycerides, leptin and adiponectin levels. Hepatic expression of PPARs and SREBP-1 was assessed by real time RT-PCR.
Results: HIV and NAFLD patients compared with controls had higher insulin levels (median 6.9 and 15.7 vs 2.8 mU/l, P<0.05) and lower adiponectin levels (median 5.2 and 6.4 vs 12 µg/ml, P<0.05). Leptin levels were higher only in NAFLD patients. Liver histology in HIV infected patients showed steatohepatitis in 4/9 cases, associated with portal fibrosis in all cases. Hepatic expression of SREBP-1 was higher in HIV patients than in NAFLD or control patients (median 90 vs 50 and 40 104 cop/µg RNA respectively, P<0.05). HIV-infected patients with steatosis had significantly higher SREBP-1 expression than those without steatosis (median 175 vs 85 104 cop/µg RNA, P<0.05). Hepatic expression of PPARα, PPARγ1, and PPARγ2 was not significantly different between the 3 groups.
Conclusion: In HIV-infected patients with antiretroviral-related lipodystrophy 1) steatohepatitis is frequent; 2) hepatic SREBP-1 mRNA is overexpressed as compared to NAFLD patients or to controls; 3) SREBP-1 overexpression is associated with steatosis; 4) expression of PPARs genes is not significantly modified. These results suggest that SREBP-1 contributes to the pathogenesis of fatty liver in HIV-infected patients with lipodystrophy.
BODY COMPOSITION AND METABOLIC EFFECTS OF ANTIVIRAL TREATMENT OF HEPATITIS C INFECTION
Irina Kaplounov, Ellen S Engelson, St. Luke's-Roosevelt Hospital, New York, NY; Safak Reka, SUNY Downstate Hospital Center, Brooklyn, NY; Donald P Kotler, St. Luke's-Roosevelt Hospital, New York, NY
Background: Previous studies have documented body composition and metabolic alterations in chronic hepatitis C infection, in the presence or absence of HIV co-infection, but have not systematically looked at the response to therapy with Interferon and Ribavirin.
Methods: We examined the effects of 3 months of pegylated interferon + ribavirin on body weight, body composition, glucose metabolism and lipid metabolism in 9 mono-infected (4 female) and 9 co-infected (3 female) subjects, and examined the influence of HIV status and the relationship to HCV antiviral effects. Measurements at baseline and after 12 weeks of therapy included body composition by anthropometry and BIA, fasting glucose and insulin plus calculation of HOMA and QUICKI indices, fasting triglycerides, cholesterol, and HDL, and HCV RNA.
Results: Mean body weight fell by 2.7 kg (p<0.001), with a significant loss of 2.1 kg fat (p<0.001) but not fat-free mass. Waist (p<0.05) and hip circumferences (p<0.005) fell, while mean waist-to-hip ratio was unchanged. Subjects became less insulin resistant (mean HOMA 8.7 vs. 6.1, p<0.05). Total cholesterol (183 vs. 163 mg/dl, p<0.05) and HDL (40 vs. 30 mg/dl, p=0.005) concentrations fell, while LDL cholesterol and triglycerides did not change. Therapy was also associated with increased serum soluble TNF receptors I (1187 to 1680 pg/ml) and II (3941 to 5263 pg/ml), both p<0.001. The changes were quantitatively similar in mono-infected and co-infected subjects. Fourteen of the 18 subjects had a >2 log decrease in plasma HCV RNA content. The nutritional and metabolic changes were similar in patients who did and did not have a viral response, except responders lost significantly more fat than non-responders (1.8 kg vs. 0.3 kg, p<0.01).
Summary: Therapy with interferon and ribavirin promotes lipoatrophy and dyslipidemia, but decreases insulin resistance. These alterations are not affected by HIV serostatus.
DIABETES INCREASES THE RISK OF HEPATOCELLULAR CARCINOMA IN THE UNITED STATES: A POPULATION BASED CASE-CONTROL STUDY
Jessica A Davila, Robert O Morgan, Yasser Shaib, Houston Center for Quality of Care and Utilization Studies, Houston, TX; Katherine A McGlynn, Division of Cancer Epidemiology and Genetics, Bethesda, MD; Hashem B El-Serag, Houston Center for Quality of Care and Utilization Studies, Houston, TX
Purpose: Diabetes has been associated with an increased risk of hepatocellular carcinoma (HCC) in studies of referred patients. This is the first population-based case-control study in the United States to examine this association while adjusting for other major risk factors related to HCC.
Methods: Using the newly created and validated SEER-Medicare linked data, we identified patients age 65 years and older diagnosed with HCC and randomly selected non-cancer controls between 1994-1999. Only cases and controls with continuous Medicare enrollment for 3-years prior to the index date were examined. Inpatient and outpatient claims files were searched for diagnostic codes indicative of diabetes, hepatitis C virus (HCV), hepatitis B virus (HBV), alcoholic liver disease, and hemochromatosis. HCC patients without these conditions were categorized as idiopathic. Unadjusted and adjusted odds ratios were calculated in logistic regression analyses.
Results: We identified 2,061 HCC patients and 6,183 non-cancer controls. Compared to non-cancer controls, patients with HCC were younger (76 vs. 78 years), male (66% vs. 36%), and non-white (34% vs. 18%). The proportion of HCC patients with diabetes (43%) was significantly greater than non-cancer controls (19%).
In multiple logistic regression analyses that adjusted for demographics features and other HCC risk factors (HCV, HBV, alcoholic liver disease, and hemochromatosis), diabetes was associated with a 3-fold increase in the risk of HCC.
In a subset of patients without these major risk factors, the adjusted odds ratio for diabetes declined but remained significant (adjusted OR = 2.87; 95% CI: 2.49-3.30). A significant positive interaction between HCV and diabetes was detected (p<0.0001).
Similar findings persisted in analyses restricted to diabetes recorded between 2 and 3-years prior to HCC diagnosis.
Conclusions: Diabetes is associated with a 2 to 3-fold increase in the risk of HCC, regardless of the presence of other major HCC risk factors. Findings from this population-based study support a causal relationship between diabetes and HCC.
THE IMPACT OF DIABETES MELLITUS AND STEATOSIS ON HEPATIC FIBROSIS AND INFLAMMATION IN HCV PATIENTS
Bashar M Attar, Franjo Vladic, Gonzalo Pandolfi, Erik Chinga-Alayo, Amila Orucevic, Arthur T Evans, Brendan M Reilly, John H. Stroger Hospital of Cook County, Chicago, IL
The prevalence of type II diabetes mellitus (DM) is higher in HCV patients than in the general population. The impact of DM on liver fibrosis and inflammation has not been fully illustrated.
AIM: To evaluate the prevalence of DM and steatosis (fatty liver) in HCV patients and assess the grade and stage on their liver histology.
Patients and Methods: 373 patients were evaluated (59% African American, 20% White, 21.4% Hispanic; 41% women). Of these, 218 patients had liver biopsy (60% African American, 17% White and 23% Hispanic; 34% women). The liver histology was compared using METAVIR classification. The following parameters were evaluated: presence of steatosis, serum albumin, serum creatinine, platelet count, AST, ALT, Alkaline phosphatase, Gamma-glutamyl-transpeptidase (GGT), DM, HCV serotype, HCV viral load, age, sex and race.
Results: Diabetes mellitus was prevalent in 19% (70/373) of patients. The prevalence of DM increased from 5% to 33% as hepatic histologic grades increased from 1 to 4, respectively (p=0.057). There was no trend of increasing prevalence of DM with histologic fibrosis stage. The presence of steatosis was not associated with higher degrees of inflammation or fibrosis. When grade and stage categories were combined, DM had a more pro-fibrogenic and inflammatory effect (p<0.05). All DM patients had liver histology which revealed fibrosis, inflammation or both.
Conclusion: The prevalence of diabetes is high in patients with HCV, regardless of race. Patients with DM were more likely to have higher degrees of liver inflammation and fibrosis. The presence of steatosis was not related to these findings.
THE NATURAL HISTORY OF NONALCOHOLIC FATTY LIVER DISEASE: A POPULATION BASED STUDY; mortality is higher due to nonalcoholic fatty liver disease and associated with insulin resistance/diabetes.
Leon Adams, James Lymp, Jenny St Sauver, Ariel Feldstein, Keith Lindor, Steven Brown, Paul Angulo, Mayo Clinic, Rochester, MN
Background: The long-term significance of nonalcoholic fatty liver disease (NAFLD) is not well defined. The few natural history studies reported to date, include small numbers of highly selected populations. A study from a specialist center found the occurrence of cirrhosis, overall death and liver related death to be 15%, 36% and 7% respectively during a mean follow up of 8.3 years. It remains uncertain if such rates can be applied to patients from the community. Hence, we conducted a population based study to examine in NAFLD patients 1) overall mortality compared to the general population; and 2) liver related morbidity and mortality.
Methods: A total of 435 residents in Olmsted County, Minnesota diagnosed with NAFLD in 1980-1999 were identified using the diagnostic index of the Rochester Epidemiology Project. This index links all diagnoses from health care providers in Olmsted County. Over 90% of the population is seen by a health care provider at least once every 3 years enabling thorough ascertainment and follow-up. NALFD was confirmed by imaging or liver biopsy. Other causes of liver disease or secondary causes of NAFLD were excluded. Follow up of liver related morbidity and cause of death was determined by review of medical records and death certificates up to December 2003. Survival was compared with the general Minnesota population of the same age and gender. Hazard ratios (risk of death) for prognostic variables were determined by multivariate Cox regression analysis.
Results: The 435 patients [213 (49%) men, 222 (51%) women] had a mean age of 49 ± 15 years. Patients were followed for a mean of 7.6 ± 4.0 years (range 0.1-23.5). Only 21 (5%) patients were diagnosed with cirrhosis: 8 (1.9%) at initial diagnosis and 13 (3.1%) during follow-up. Thirteen (3.1%) cirrhotics developed complications, including 1 requiring transplantation and 2 developing liver cancer. Overall 53 (12.6%) patients died. Survival was significantly lower than the general population [standardized mortality ratio 1.34 (95% CI 1.00-1.76) p<0.05]. To examine patients with at least 10 years of follow up, 161 patients diagnosed in 1980-1993 were analyzed. As follow-up lengthened, survival worsened compared to the general population [SMR 1.55 (95% CI 1.11-2.11) p=0.005]. Age (HR per decade 2.2, 95% CI 1.7-2.7), glucose intolerance/diabetes (HR 2.6, 95% CI 1.3-5.2) and cirrhosis (HR 3.1, 95% CI 1.2-7.8) were associated with increased risk of death. Liver disease was the third leading cause of death occurring in 7 (1.7%) subjects.
Conclusion: Mortality in community NAFLD patients is significantly higher than the general population and predicted by older age, glucose intolerance/diabetes and cirrhosis. Overall mortality and liver related death in NAFLD patients from the community is considerably lower than previous reports from referral centers.
CAUSAL RELATIONSHIP BETWEEN HEPATITIS C VIRUS INFECTION AND THE DEVELOPMENT OF TYPE 2 DIABETES MELLITUS IN A HEPATITIS C VIRUS HYPERENDEMIC AREA
Takumi Kawaguchi, Yumiko Nagao, Takafumi Yoshida, Kazuo Tanaka, Tatsuya Ide, Masaru Harada, Ryukichi Kumashiro, Michio Sata, Kurume University School of Medicine, Kurume, Japan
Backgrounds: Hepatitis C virus (HCV) infection antedates insulin resistance. However, this association at the population level including asymptomatic HCV carriers remains unclear. Furthermore, the involvement of HCV core, showing many biological properties, in the development of type 2 diabetes mellitus (DM) has never been examined.
Aims: The aims of this study are to examine an association between HCV infection and insulin resistance, and a causal relationship between HCV infection and the development of type 2 DM in an HCV hyperendemic area.
Methods: In an HCV hyperendemic area (adult population is 7,389 and 23.6% residents are anti-HCV positive), randomly selected subjects with anti-HCV positive (n = 31) and subjects with anti-HCV negative (n = 44) were enrolled in this study. An association between HCV infection and insulin resistance was examined in 1995. Insulin resistance was evaluated by the homeostasis model assessment (HOMA-IR). After 7 years follow-up, we examined the relative risk of the development of type 2 DM by a case-cohort analysis.
Results: There was no significant difference in age, sex, BMI, alcohol intake, and γ-glutamyltranspeptidase between the subjects with anti-HCV positive and negative. Although alanine aminotransferase level showed significant increase in anti-HCV positive subjects, mean value was within normal range. Anti-HCV-positive subjects showed increased HOMA-IR values compared to anti-HCV negative subjects (6.8 ± 1.4 vs 3.8 ± 0.6; p = .04). Moreover, stratification of the anti-HCV-positive group according to serum HCV core titer revealed an association between HCV core and insulin resistance. HOMA-IR values (9.3 ± 2.7) was significantly increased in subjects with high titer (>= 300 fmol/L) of HCV core compared to those (4.5 ± 1.0; p = .03) in subjects with low titer (< 300 fmol/L) of HCV core and those (3.8 ± 0.6; p = .004) in subjects with anti-HCV negative. Among 71 subjects free of DM in 1995, 8 subjects developed type 2 DM over 7 years of follow-up evaluation. Overall, anti-HCV-positive subjects were 3-fold as likely as anti-HCV-negative subjects to develop type 2 DM, but this difference was not significant (p = .11; relative hazard, 3.62; 95% CI, 0.45 - 1.05). After stratification of the anti-HCV-positive group according to serum HCV core titer, a significant increase in the incidence of type 2 DM was seen in subjects with high titer of HCV core compared to anti-HCV-negative subjects (p = .04; relative hazard, 5.25; 95% CI, 0.49 - 0.95).
Conclusions: We report here for the first time community-based evidence for an association between HCV infection and insulin resistance, and a causal relationship between HCV infection and the development of type 2 DM. We also showed the involvement of HCV core in the development of type 2 DM.
BODY COMPOSITION AND NUTRIENT UTILISATION IN PATIENTS WITH NON-ALCOHOLIC STEATO-HEPATITIS (NASH)
Esmeralda Capristo, Alessandra Forgione, Vittoria Vero, Luca Miele, Michele Diana, Sara Farnetti, Giovanni Gasbarrini, Antonio Grieco, Catholic University, Rome, Italy
Background and Aim: Metabolic alterations are a common feature in patients affected by non-alcoholic steato-hepatitis (NASH). A dietary treatment, with consequent body weight reduction, represents a fundamental tool in the management of these patients.
Aim: The aim of the present study was to evaluate body composition, energy expenditure and substrate utilisation in male patients with NASH, comparing them with patients affected by chronic hepatitis related to HCV infection (HCV) and a group of healthy volunteers.
Methods: Twenty male outpatients with NASH (age: 41±11 yr; BMI: 26.2±2.1 kg/m2) and 14 HCV male patients (age 44.6±13 yr; BMI: 24.8±2.8 kg/m2) were enrolled in the study. A group of 20 healthy male subjects (age: 39±10 yr; BMI: 23.3±1.1 kg/m2) were studied as controls. Body composition was assessed by anthropometry and dual-energy X-ray absorptiometry; resting metabolic rate and nutrient oxidation by indirect calorimetry. A 7-day food diary was collected. The main biochemical parameters were measured using standardised laboratory techniques.
Results: Body weight was higher in NASH patients with respect to HCV patients and control subjects (respectively 75.2±8.9 vs 68.5±9.4 and vs 67.0±8.0 kg; P<0.01) and this was essentially due to fat mass (FM) increase (29.8±4.8 vs 26.8±5.0%; P< 0.05). A reduction in fat-free mass (FFM) was found in HCV patients with respect to both NASH and control subjects. Patients with NASH had a significantly higher waist circumference (104±6 cm; P<0.01) with respect to HCV (95±6 cm) and control subjects (92±5 cm). After adjustment for age and body composition, resting metabolic rate (RMR) was lower in NASH compared to HCV and control subjects, while HCV patients showed an increase in RMR and in lipid utilisation with respect to the other 2 groups (P<0.01 both). Energy intake was significantly higher in NASH patients (2210±840 kcal/die; P<0.01) compared to both HCV (1980±760 and control subjects (1880±570 kcal/die).
Conclusions: NASH patients showed an increase in body weight, fat mass and visceral fat accumulation with respect to HCV and control subjects. The reduction in RMR, coupled with increase energy intake may explain the body composition alterations found in these patients. An accurate nutritional and metabolic evaluation of these patients may allow to optimize their dietary treatment and to identify those patients at higher risk of metabolic or cardiovascolar complications.
ADIPOKINE LEVELS ARE PREDICTIVE OF HISTOLOGY IN PATIENTS WITH NON-ALCOHOLIC FATTY LIVER DISEASE
Samer Gawrieh, Barbara Rosado, Keith Lindor, Michael R Charlton, Mayo Clinic, Rochester, MN
Background: Adipocytes are the source of several important cytokines (adipokines) including leptin, resistin and adiponectin. Leptin has been shown to be a mediator of hepatic inflammation and fibrosis in non-alcoholic fatty liver disease (NAFLD). Resistin and adiponectin have been shown to be important modulators of insulin resistance, a central factor in the pathogenesis of NAFLD. Aim: We evaluated 1) whether adipokine levels are different among patients (pts) with NAFLD when compared to obese and lean controls, and 2) whether adipokine levels are predictive of steatohepatitis (SH) grade and stage.
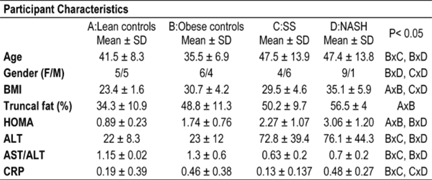
Methods: 20 controls (10 lean and 10 obese individuals without evidence of liver disease: normal liver tests and no fatty infiltration on ultrasound) and 20 pts with biopsy proven NAFLD (10 with simple steatosis (SS) and 10 with NASH) were prospectively studied. Demographic, anthropometric measurements, DEXA, liver tests, HOMA and CRP were measured in all participants. Leptin, resistin and adiponectin levels were determined by ELISA.
Results: Characteristics of participants are summarized in the table. Compared to controls, pts with NAFLD (SS and NASH) were older, and tended to have higher BMI, total and truncal fat, insulin resistance, transaminases, and leptin levels but lower AST/ALT, adiponectin and resistin levels. Compared to SS, subjects with NASH (SH grade >= 2) had higher BMI, total and truncal fat, evidence of insulin resistance, AST, ALT, AST/ALT and CRP levels. Leptin (23.7±18.7 vs 58.4±22, p 0.001) and resistin (0.85±0.31 vs1.34±0.39, p 0.006), but not adiponectin (12.2±3.4 vs 14.7±9.4, p 0.4) levels, were higher in subjects with NASH than with SS. The combination of leptin level >= 40 or resistin level >= 1.1 has sensitivity of 100%, specificity of 90%, and a negative predictive value of 100% in differentiating pts with NASH from those with SS.
Conclusions: NASH is associated with high levels of leptin and resistin when compared to simple steatosis. A combination of leptin level >= 40 and/or resistin level >= 1.1 is strongly predictive of SH grade and stage and may be useful clinically in differentiating pts with NASH from those with SS without liver biopsy.
|
|
| |
| |
 |
|
| |
| |
SERUM LEVELS OF NOVEL HEPATOPROTECTIVE PEPTIDE ADIPONECTIN IN NONALCOHOLIC FATTY LIVER DISEASE AND CHRONIC VIRAL HEPATITIS
Cem Aygun, Omer Senturk, Suleyman Uraz, Sadettin Hulagu, Altay Celebi, Tolga Konduk, Kocaeli University, Kocaeli, Turkey; Ahmet Danalioglu, SSK Vakif Gureba Hospital, Istanbul, Turkey; Birsen Mutlu, Zeynep Canturk, Kocaeli University, Kocaeli, Turkey
Aim: Adiponectin is an adipose tissue-specific protein which has anti-inflammatory, antidiabetic and antiobesity effects. Recently it has been suggested that adiponectin has a hepatoprotective role. Nonalcoholic steatohepatitis (NASH) is a common disorder which causes liver inflammation and injury. In this study, serum adiponectin levels were investigated in patients with NASH and chronic viral hepatitis to determine its possible role on hepatic inflammation and injury.
Methods: Twenty-nine patients (14F, 15M) with NASH diagnosed by biopsy, 20 nonalcoholic fatty liver (NAFL) patients (13F, 7M) with normal liver enzymes, 20 patients (9F, 11M) with biopsy proven chronic viral hepatitis (CVH) and 20 healty adults (10F, 10M) were enrolled in the study. From fasting blood samples, serum adiponectin levels were measured by ELISA. Body mass index (BMI), serum glucose, insulin, cholesterol and triglyceride levels were determined.
Results: Serum adiponectin levels were 4.99±2.1µ/ml, 9.49±3.91µ/ml, 11.61±5.57µ/ml and 7.74±4.41µ/ml in NASH, NAFL, CVH and healty adult control groups respectively. Mean serum adiponectin level in the NASH group was significantly lower than those of other groups tested (p<0.001). Mean serum adiponectin level of CVH group was significantly higher than the NASH and control groups (p<0.001) but the difference was not significant from NAFL group (p=0.07). BMI, insulin, cholesterol and triglyceride levels of NASH patients were significantly higher than CVH and control groups (p<0.05) but were not significantly different from NAFL group (p>0.05).
Conclusion: Serum adiponectin levels were significantly lower in patients with NASH but they were significantly increased by CVH. In NASH patients reduced hepatoprotective adiponectin concentrations may be involved in the pathogenesis of inflammation while in CVH elevated levels may be secondary to the inflammatory response of body to viral infection.
|
| |
|
 |
 |
|
|