 |
 |
 |
| |
Effects of Fuzeon on Body Composition and Lipids Through 48 weeks in the TORO Trials
|
| |
| |
Reported by Jules Levin
11th Annual Retrovirus Conference, Feb 8-11, 2004,San Francisco, poster 715
Authors: D A Cooper*1, P Reiss2, K Henry3, M Nelson4, M O'Hearn5, P Piliero6, J Reynes7, K Arasteh8, J Chung9, D Guimaraes9, T Kinchelow9, A Bertasso9, and the TORO 1 and TORO 2 study groups
1Natl. Ctr. in HIV Epidemiology and Clin. Res., Univ. of New South Wales, Sydney, Australia; 2Academic Med. Ctr., Amsterdam, The Netherlands; 3Hennepin County Med. Ctr., Minneapolis, MN, USA; 4Chelsea and Westminster Hosp., London, UK; 5Oregon Hlth. and Sci. Univ., Portland, USA; 6Albany Med. Coll., NY, USA; 7Hosp. Gui de Chauliac, Montpellier, France; 8EPIMED c/o Vivantes Auguste-Viktoria-Klinikum, Berlin, Germany; and 9Roche, Nutley, NJ, USA
Summary: This study examined about 1000 who received either Fuzeon based ART or a regimen without Fuzeon in the large phase III clinical trials for Fuzeon (TORO I & II), for the purpose of looking at the development of body changes and metabolic abnormalities; to see if Fuzeon was associated with body changes and abnormalities in cholesterol, triglycerides, and glucose. The TORO studies were to examine the benefit of Fuzeon in viral load & CD4 count for highly treatment experienced patients with few treatment options left. DEXA and CT scans were used. The authors of this study reported that the incidence of treatment-emergent fat distribution adverse events was marginally less for patients receiving Fuzeon (9.2 events per 100 patient-years) versus the optimized therapy group (11.7 events per 100 patient years): optimized therapy was a regimen patients received without Fuzeon, patients received the best regimen that could be designed but without Fuzeon. The authors commented that the body composition scan results should be interpreted with caution due to the relatively small number of patients in each group at 48 weeks (65-90 patients in Fuzeon group and 12-50 in the other group; see Table below), but you can see that in this study Fuzeon did not appear to cause increased incidences in body changes and many parameters of metabolic values. This is the first data on body changes and metabolics for entry inhibitors, which work outside the CD4 cell and it was suggested that because of that this new class of drugs might have different effects than other classes of ART drugs which appear associated with effects on body changes and metabolics. Still, in research related to lipodystrophy, HIV itself and other factors have been found to be associated with body changes and perhaps lipid abnormalities, so it may be premature to draw too many conclusions yet until we see further data. Nonetheless, the results from this study is encouraging.
The study authors concluded that based on body composition scans (DEXA and CT) and anthropometric measurements, the addition of enfuvirtide (Fuzeon) to an OB (optimized background) ARV regimen does not appear to have any adverse effect on fat distribution compared to patients on OB treatment alone.Enfuvirtide was not associated with any adverse lipid or glycemic laboratoryparameters.
Antiretrovirals (ARVs) have been implicated in the development of metabolic and morphologic adverse effects in HIV-infected patients, but the effect of enfuvirtide (ENF) (Fuzeon) on body composition and lipid parameters has not been determined. This study reports on the effect of Fuzeon (enfuvirtide) on body changes and metabolic effects seen in the large phase III study.
Metabolic changes have included elevations in both triglycerides and cholesterol. These changes have been mainly associated with a number of protease inhibitors (PIs), as well as with certain nucleoside and non-nucleoside reverse transcriptase inhibitors (NRTIs and NNRTIs). Impaired glucose metabolism has also been strongly associated with the use of PIs, particularly indinavir. Morphologic adverse events include loss of fat (lipoatrophy) from the face and extremities. Conversely, accumulations of fat (lipohypertrophy) in the abdomen, on the back of the neck between the shoulder blades (buffalo hump), in the submandibular region, and in the breasts (gynecomastia) can also be seen in patients receiving antiretroviral therapy. PI therapy and NRTI therapy have both been implicated in the development of body composition changes.
Enfuvirtide (Fuzeon, akaT-20) is the first in a new class of ARV agents, theHIV-1 fusion inhibitors, which targets HIV-1 gp41 and blocks the virus fromentering host cells. The safety and efficacy of chronically administered ENF hasbeen demonstrated in Phase III clinical studies. There is a question of whether entry inhibitors, which work outside the host cells (cd4 cells) as opposed to other ART drugs which work inside cells, will effect body changes and lipid abnormalities similarly to the other ART drugs. This study may not conclusively answer this question but offers some preliminary insights. Additional studies with Fuzeon and new entry inhibitors (attachment and CCR5 inhibitors) in earlier stages of development will provide more insight into this question.
TORO 1 and TORO 2 are randomized Phase III studies of Fuzeon plus an optimized background (OB) ARV regimen versus an OB regimen alone. A total of 997 triple class-experienced patients were randomized in a 2:1 ratio [Fuzeon + OB (n=663): OB alone (n=334)], treated and had at least one follow-up safety measurement.
As a result of differences in the extent of exposure to Fuzeon + OB versus OB,rates of adverse events (AEs) and laboratory abnormalities are reported here asnumber of patients with events per 100 patient-years of treatment exposure.A separate analysis was performed investigating the incidence of collapsedadverse event terms (single terms used to combine different AEs that might beconsidered clinically equivalent) in order to identify whether a small increase in incidence of several AEs might, when combined, lead to a relevant difference between treatment arms in the collapsed term.
Fat distribution adverse events
Anthropometric measurements of the waist and hips were determined in allpatients enrolled in TORO 1 and TORO 2 at baseline, week 24, and week 48.
To determine the effect of enfuvirtide on body composition, whole body dualenergy X-ray absorptiometry (DEXA) and single slice computed tomography (CT)scans at the level of the L4 vertebra were performed in a metabolic substudy of TORO patients (ENF + OB group, n = 102; OB group, n = 53) who volunteeredfor these assessments at sites capable of performing the scans. Scans weretaken at baseline, 24, and 48 weeks.
Preferred terms summarized using the collapsed term
Collapsed term: Preferred terms
distribution adverse events: gynecomastia, lipoatrophy,lipodystrophy acquired, fat redistribution
Diabetes mellitus and blood glucose increased: hyperglycemia diabetes mellitus aggravated, diabetes mellitus inadequate control, diabetes mellitus non-insulin dependent, diabetes mellitus nos, glycosuria present, hyperglycemia nos, insulin resistance
Coronary artery disease: angina pectoris, angina pectoris aggravated, angina unstable, coronary artery disease nos, coronary artery thrombosis, myocardial infarction, myocardial ischemia
Hypercholesterolemia: blood cholesterol increased,Hypertriglyceridemia: blood triglycerides increased,or hyperlipidemia: hypercholesterolemia, hyperchylomicronemia, hyperlipidemia nos, hypertriglyceridemia, hyperglyceridemia nos increased(nos, not otherwise specified)
Laboratory tests
Fasting chemistries for the following laboratory parameters were assessed atbaseline and weeks 8, 16, 24, 32, and 48 for all patients:
- Glucose
- Insulin
- Total cholesterol
- High-density lipoprotein (HDL)
- Triglycerides
- C-peptide
- Calculated low-density lipoprotein (LDL) and very low-density lipoprotein (VLDL)
Statistical analyses
This study was a planned descriptive analysis only and no significance tests are presented.
RESULTS
TORO trials
Over the 48-week study period, exposure to ENF + OB and OB was 557.04 and162.13 patient-years, respectively.
The composition of the OB regimen was similar between the treatment groups.
Of patients who received ENF + OB, 30.4% achieved < 400 copies/mL HIV-1RNA at 48 weeks as compared to 12.0% of patients in the OB group. Similarresults favouring ENF + OB were seen in patients that achieved < 50 copies/mLHIV-1 RNA or demonstrated at least a 1.0 log10 decrease from baseline.9
At 48 weeks an analysis of safety showed that ENF added to OB did notexacerbate most of the known toxicities associated with other ARVs. Inparticular, the incidence of diarrhea in the ENF + OB group was approximatelyhalf that of the OB group (37.7 versus 73.4 events per 100 patient-years).
The most common AE was injection site reactions (ISRs), seen in almost allpatients (98.3%). These were generally mild to moderate and were treatmentlimiting in only 4.4% of patients.
A higher rate of pneumonia was observed in subjects treated with ENFcompared to the control arm, but the rate was within expected ranges for thispatient population. Drug relationship was not established.
Systemic hypersensitivity to ENF was reported in a small number of patients (< 1%).
Fat distribution adverse events
Overall, the incidence of treatment-emergent fat distribution adverse events(collapsed term) was marginally less in the ENF + OB group (9.2 events per 100patient-years) versus the OB group (11.7 events per 100 patient years). Similar results were observed in patients who already had these conditions at study entry.
As well, there appeared to be no difference between the Fuzeon regimen and the OB regimen regarding the incidence of lipodystrophy acquired, lipoatrophy, gynecomastia, and fat redistribution. The rates of other related adverse events were also similar or favorable to Fuzeon: diabetes and hyperglycemia were about the same (4.8 per 100 patients yrs for Fuzeon vs 3.7 for OB), coronary heart disease (1.6 per 100 patients yrs vs 2.5), and hypercholesterolemia, hyperglyceridemia, and hyperlipiemia were perhaps favorable to Fuzeon or at least the same (7.9 vs 9.9 per 100 patient yrs).
The mean change from baseline in waist and hip circumference as surrogatemarkers of body fat did not indicate any effect of ENF on body fat distributionover 48 weeks of follow up. The mean change of waist:hip ratio for the ENF +OB group was 0.01 (n = 440) versus 0.00 (n = 70) for the OB group.
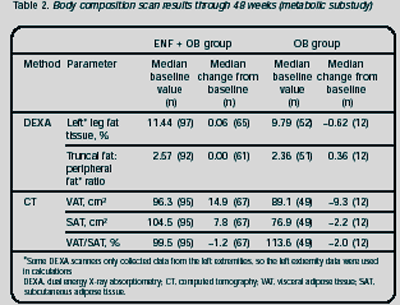
Table 2 shows the body composition scan results from the metabolic substudypopulation at 48 weeks. These results should be interpreted with caution due to the relatively small number of patients in each group at 48 weeks. DEXA of left leg fat tissue did not change in patients receiving Fuzeon but was reduced in patients receiving OB. Truncal fat remained the same for patients receiving Fuzeon but increased for patients receiving OB. Subcutaneous fat (SAT) increased for patients receiving Fuzeon but not for patients receiving OB.
Patients in the metabolic substudy receiving ENF + OB showed a greaterincrease in median body weight from baseline [1.70 kg (n = 81)] than thosereceiving OB alone [1.00 kg (n = 15)]. In all patients, the median change in body weight from baseline was similar for both treatment groups [ENF + OB group, 0.90 kg (n = 490) versus OB group, 1.00 kg (n = 77)].
The increase in fat observed in the ENF + OB arm could be expected, given thegeneral gain in total body weight in this group.
|
|
| |
| |
 |
|
| |
| |
Laboratory test results
Changes in laboratory parameters for fasting glucose, LDL, HDL, totalcholesterol, and triglycerides from baseline were observed at all or nearly alltimepoints (8, 16, 24, 32, and 48 weeks) and were of similar magnitude in theENF + OB and OB groups, suggesting that they were not related to enfuvirtidetreatment.
Differences were observed for insulin (mean change from baseline 0.44 µU/mLfor ENF + OB versus --0.81 µU/mL for OB) and VLDL (mean change frombaseline --0.15 mmol/L for ENF + OB versus 0.20 mmol/L for OB) at week 48,however the standard deviation for both was large (data not shown) possiblyindicating extensive interpatient variability.
Discussion By Authors
In the general population, hypercholesterolemia and hypertriglyceridemia are both independent risk factors for coronary heart disease (CHD) and associated acute coronary syndromes. HAART-related toxicities, several of which are risk factors for cardiovascular disease, have raised the concern that ARV therapy may increase risk for cardiovascular disease in HIV-infected, treated individuals.
A recent study has found that the covariate-adjusted relative risk for thedevelopment of CHD in HIV-infected individuals aged 18--33 years receiving ARVtherapy compared to those not receiving ARV therapy was 2.06 (p < 0.001).10 The D:A:D study found a slight but statistically significant independent association between exposure to combination ARV therapy and myocardial infarction (26% increase per year of treatment exposure during the first 4--6 years of use compared to HIV-infected patients not receiving treatment). There were insufficient data from this study to allow an analysis by type of ARV regimen.
In the present study patients receiving ENF + OB showed a mean increase in insulin of 0.44 µU/mL together with a mean decrease in VLDL of 0.15 mmol/L over the 48 weeks; however, these changes are unlikely to be clinically relevant.
While not clinically serious in and of themselves, changes in body shape resulting from ARV therapy can have serious psychological consequences and can adversely affect adherence to medication and quality of life. In 2003, the HIV Lipodystrophy Case Definition Study Group published a validated model to provide a specific case definition of lipodystrophy in HIV-infected adults. According to this definition, body composition factors to be evaluated are waist-to-hip ratio, intraabdominal (VAT) to extra-abdominal (SAT) fat ratio from abdominal CT scans, trunk to-peripheral fat ratio from DEXA scans, and percentage leg fat from DEXA scans. When these factors were examined, the ENF + OB group showed a similar or reduced adverse effect on fat distribution compared to the OB group.
|
|
| |
| |
|
| |
|
 |
 |
|
|