 |
 |
 |
| |
"Beyond Serum Creatinine: Identification of Renal Insufficiency Using GFR: Implications for Clinical Research and Care"
|
| |
| |
Reported by Jules Levin
HERE IS THE POSTER PRESENTED BY STEVE BECKER AT the 12th CROI.
12th Conference on Retroviruses and
Opportunistic Infections
Boston, MA, USA. February 22-25, 2005
Poster 819
Stephen L Becker1, Rukmini B Balu2, Jennifer S Fusco2, and Gregory P Fusco2
1Pacific Horizon Medical Group, San Francisco, CA; 2CHORUS Cohort, Research Triangle Park, NC.
2 websites where you & your doctor can calculate your kidney function. As well, you can perform a direct measure by using a 24-hour urine test (collecting urines for 24 hours in container & then test by blood.
Website to calculate Cockroft-Gault equation for patients:
http://www.clinicalculator.com/english/nephrology/cockroft/cca.htm
MDRD GFR Calculator
http://www.kidney.org/kls/public/gfr_calculator.cfm
ABSTRACT
Background: Recent reports of renal insufficiency associated with the NRTIs have included elevations in serum creatinine, proximal tubular dysfunction, nephrogenic diabetes insipidus, renal failure, Fanconi-like syndrome and death. Appropriate methods for identification of patients at risk for severe renal injury are needed for monitoring and clinical dosage modification.
Methods:Using an antiretroviral known to cause renal impairment (tenofovir disproxil fumarate TDF) as a model, we evaluated the rate of grade 1 and grade 4 renal insufficiency using serum creatinine(sCr) and a method to more precisely evaluate glomerular filtration, Modification of Diet in Renal Disease (MDRD) GFR. Literature suggests that even minor changes in sCr result in substantial decreases in GFR. Moreover, sCr is influenced by other factors including age, race, sex and body mass. According to the National Kidney Foundation (NKF) GFR is the "best overall indicator of the level of kidney function". This is especially true in patients with comorbid conditions. Multivariable logistic models were fit to consider age, race, study site, sex, route of HIV infection, AIDS, baseline VL and CD4, baseline renal function, concurrent use of other
nephrotoxic drugs, history of renal disease, hypertension and diabetes as predictors of renal insufficiency in patients treated with TDF.
Results: 1298 patients initiated first TDF on or after consent to CHORUS. Using a combined endpoint of sCr and clinical events, 22 patients (1.7%) experienced a grade 1 event, 1 patient (<0.1%) experienced a grade 4 event. Using a combined endpoint of GFR and clinical events, 128 patients (9.9%) experienced a
grade 3 event, 7 patients (<0.1%) experienced a grade 4 event. Multivariable analysis identified past history of renal disease [RR=4.9; 95% CI=2.7,8.8], abnormal baseline GFR [18.9; 9.2,39.1], hypertension [1.6; 1.1,2.3], and concurrent use of other nephrotoxic medications [2.7; 1.9,3.9] as important predictors of renal insufficiency.
Conclusion: The elevations in sCr observed in CHORUS are consistent with those seen in other populations, observational or otherwise. The proportion of patients with extreme grade 4+ GFR values is comparable to results seen for grade 4+ sCr in other studies. However, nearly 10% of our patients have
renal dysfunction using the grade 3+ GFR criterion. This level is defined by the NKF as chronic kidney disease. GFR should be considered for the evaluation of renal insufficiency in HIV.
BACKGROUND
HIV patients are at increased risk for renal dysfunction as a result of HIV disease- and therapy-related renal damage, diabetes mellitus, hypertension, and other comorbid conditions. Appropriate methods for identification of patients at risk for severe renal injury are needed for monitoring and clinical dosage
modification.
Traditionally, clinical studies have evaluated nephrotoxicity through elevations of serum creatinine. However, the National Kidney Foundation (NKF) has recently noted that the use of serum creatinine alone may not be suitable for detection of renal impairment.1 Serum creatinine levels are susceptible to changes in body mass, sex, age and race. Furthermore, minor changes in serum creatinine result
in substantial decreases in renal function.2,3 Therefore, the NKF recommends using a measure of glomerular filtration rate as the best indicator of renal function, as it takes into account serum creatinine as well as some of the additional factors that make measurement of serum creatinine alone, an
insufficient clinical marker, especially in patients with comorbidities.
A rapid and accurate measure of glomerular filtration rate is especially important when beginning a therapy which could be nephrotoxic, or when a drug used could reach toxic levels due to impaired renal function. Direct measures of glomerular filtration, such as 24-hour inulin clearance, are considered the
gold standard.4,5 However, they are expensive, time-consuming, and taxing on the patient. Therefore, estimates of glomerular filtration have been sought through numerous studies. These estimates frequently have used serum creatinine adjusted for a variety of demographic characteristics. The Cockcroft-Gault and Modification of Diet in Renal Disease estimations have been widely studied both in clinical research and management.2,3,6,7
The aim of this analysis was to evaluate renal function, using serum creatinine and the Modification of Diet in Renal Disease estimated glomerular filtration rate (MDRD GFR) in a population of HIV-infected adults to evaluate the burden of chronic kidney disease and sensitivity of the measures for identifying clinically relevant renal events. Several case reports have shown an association between the use of the nucleotide analog tenofovir disoproxil fumarate (TDF) and varying degrees of renal dysfunction, ranging from elevations in serum creatinine, proximal tubular dysfunction, nephrogenic diabetes insipidus, renal failure, Fanconi like syndrome and death. Therefore we chose to evaluate markers of renal dysfunction in a subpopulation of patients treated with TDF.8-12
Methods
Study hypothesis
Patients prescribed tenofovir have a comparable burden of illness and sensitivity for identifying impaired renal function when measured by MDRD GFR compared to serum creatinine.
Study population
This analysis was restricted to a subset of patients who started their first TDF-containing regimen on or after consent into the CHORUS study. Eligible patients must have had at least 6 months of follow up in the study to be considered in this analysis. They were enrolled at one of the following 7 study sites: Comprehensive Care Center, Nashville, TN, Liberty Medical Group, New York, NY, Pacific Oaks Medical Group, Los Angeles, CA, Pacific Horizon Medical Group, San Francisco, CA, Orlando Immunology Center, Orlando, FL, Treasure Coast Infectious Disease, Vero Beach, FL, and ID Consultants, Charlotte, NC.
Analysis
Patients who were prescribed TDF were followed for diagnoses and laboratory values consistent with renal dysfunction - increase in serum creatinine, decrease in GFR and clinical events indicative of nephrotoxicity.
Glomerular filtration rate was calculated using the MDRD formula:
MDRD GFR = (186)*(Serum creatinine mg/dl-1.154)*(age-0.203)*(0.742 if female)*(1.212 if AfrAm)
Laboratory events were defined as moderate (ACTG grade 1+) elevations in serum creatinine defined as 1.5 times the upper limit of normal (ULN), severe (ACTG grade 3+) elevations in serum creatinine defined as 3X ULN, moderate (NKF stage 3+ chronic kidney disease) decreases in GFR defined as ≤ 59
mL/min/1.73m2 and severe (NKF stage 4+ chronic kidney disease) decreases in GFR defined as ≤ 29 mL/min/1.73m2. Clinical events were defined as diagnoses of renal or kidney failure, renal insufficiency, proximal tubular dysfunction, acute tubular necrosis, nephrogenic diabetes, FanconiÕs syndrome, hypophosphatemia, acute interstitial nephritis, nephrotic syndrome, renal tubular dysfunction, and death due to renal failure. All events were identified while on the regimen of interest or within seven days after discontinuation.
As a first step in data analysis, the analysis population was described at baseline and by outcome variables. Some of the baseline variables evaluated were age, race, sex, study site, route of HIV infection, CD4 and viral load at baseline, hepatitis B or C coinfection, concurrent use of nephrotoxic drugs, comorbidities including hypertension and diabetes, and past renal disease. Events were further
described by the time from baseline to an event by the ascertainment methods. Then, multivariable models were fit to take into consideration these baseline characteristics in the assessment of risk of renal dysfunction by measurement type (serum creatinine versus MDRD GFR).
Finally, all analyses were repeated for subsets of the analysis population known to make serum creatinine an unreliable indicator of renal impairment (age defined as < 50 versus ≥ 50 years, sex defined as male versus female, and race defined as African Americans versus all other races). Event frequencies and time to event were calculated for these subgroups as well.
RESULTS
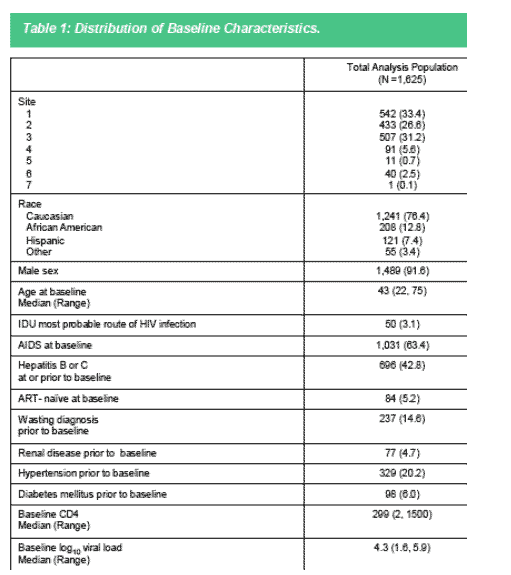
These analyses were updated since the abstract submission. As indicated in table 1, the analysis population (n=1,625) was predominantly Caucasian, male, and already diagnosed with AIDS. The median age was 43 years. Most patients had experienced ART (95%) prior to taking the regimen of interest.
| |
| |
| |
 |
|
| |
| |
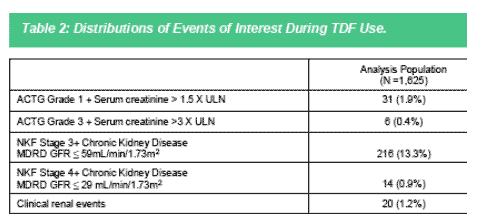
Table 2 lists frequencies of events of interest occurring during the regimen of interest. Very few patients in the study sample had severe renal impairment regardless of the method of ascertainment. Mild to moderate elevations in serum creatinine occurred rarely (2%). However, more than 10% of the patients
followed had grade 3 chronic kidney disease (NKF definition) as measured by GFR.
| |
| |
| |
 |
|
| |
| |
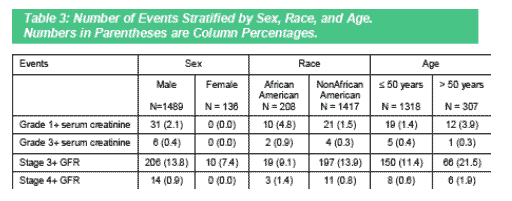
The events were further described by demographic characteristics known to effect interpretation of serum creatinine; sex, race and age (Table 3). As expected, moderately elevated serum creatinine was unable to identify any women with renal insufficiency. In contrast, 7.4% of women were identified with
chronic kidney disease (stage 3+ GFR). Serum creatinine identified more African Americans than non- African Americans with renal insufficiency but under reported both groups substantially. The most significant difference was observed for the rate of renal impairment in the patients over 50 years of age. Serum creatinine only identified a rate of 3.9% compared to the rate of 21.5% with GFR.
| |
| |
| |
 |
|
| |
| |
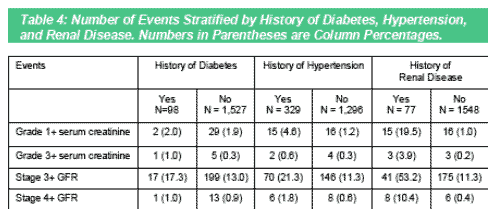
We hypothesized that we would see more renal events in patients with a history of diabetes, hypertension and past renal disease. Both serum creatinine and GFR identified more events in these at-risk populations. However, GFR identified 8 times more renal impairment in diabetics than serum creatinine and 5 times more in patients with hypertension. This trend continued in patients with a history
of renal disease. GFR identified more than twice as many patients with renal impairment as serum creatinine representing more than 50% of all patients at risk.
| |
| |
| |
 |
|
| |
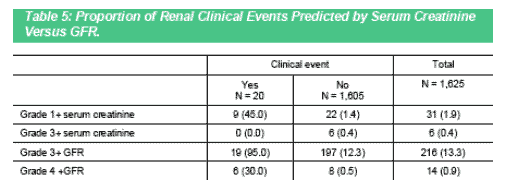
Finally, we sought to understand the number of clinical renal events predicted by serum creatinine versus GFR (Table 5). 95% of clinical renal events observed in this analysis population were predicted by a GFR ≤ 59mL/min/1.73m2. Mild to moderate elevations in serum creatinine only identified 45% of the clinical events. Most clinical events were identified and diagnosed before GFR or serum creatinine reached severe levels.
| |
| |
| |
 |
|
| |
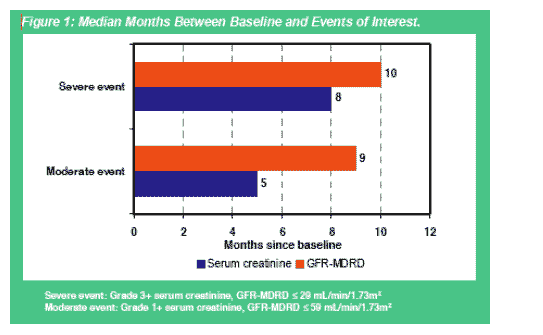
It was anticipated that the time to a renal event would be longer in the less sensitive measure. However, Figure 1 shows the median time to a grade 1+ serum creatinine elevation occur after 5 months on tenofovir (range: <1 to 55 months). In contrast, the large group of events identified by the GFR estimation occurred a median of 9 months after initiation of tenofovir (range: <1 to 42 months). Severe events by either measure occurred about 9 months from baseline as well.
| |
| |
| |
 |
|
| |
Through stepwise selection, we were able to determine the most important variables across all events. Age, abnormal renal function at baseline, history of hypertension, and concurrent use of other nephrotoxic drugs with the tenofovir-containing ART regimen were important predictors of renal events.
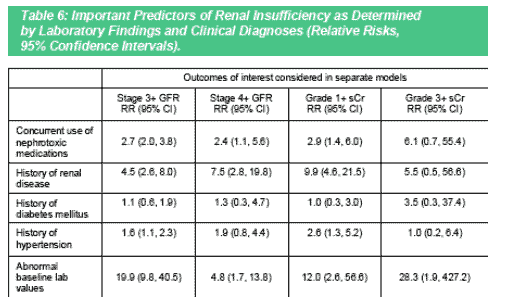
Table 6 lists the results of fitting multivariable models. Important predictors of moderate or severe renal event as measured by GFR were past history of renal disease [RR=4.5; 95% CI=2.6,8.0], abnormal baseline GFR [19.9; 9.8,40.5], hypertension [1.6; 1.1,2.3], and concurrent use of other nephrotoxic
medications [2.7; 2.0,3.8]. Diabetes failed to be important in predicting any of the renal events perhaps because of the known association and heightened index of suspicion by clinicians.
| |
| |
| |
 |
|
| |
Discussion
To our knowledge, this is the first large observational study to evaluate renal function in HIV-infected patients using glomerular filtration rate in addition to serum creatinine.
In general, the rates of severe renal dysfunction were very low in CHORUS - these numbers are comparable to those observed in other cohorts.
The proportion of patients with severe elevations in serum creatinine was comparable to the proportion of patients with severe decrease in glomerular filtration rate. However, the proportion of patients with moderate decrease in GFR consistent with stage 3 chronic kidney disease was much higher than the
proportion of patients with moderate increases in serum creatinine.
This analysis benefited from a large population of patients in whom a wide range of demographic, clinical and laboratory parameters were collected and available for statistical modeling, thus enabling the calculation of GFR with multiple variables and allowing multivariable modeling for least biased estimates of measures of association. However, because of the small number of events, many models yielded large confidence intervals even when risk ratios were statistically significant.
While serum creatinine remains an important parameter in the management of acute renal failure, we propose that a more sensitive measure of renal impairment should be used for HIV clinical research and management to assess the subtle, progressive renal injuries HIV patients endure resulting in
chronic kidney damage and disease.
Future analyses include evaluation of other NRTIs and ARTs, stratification by naive versus experienced patients, comparison of patients with baseline renal impairment versus those without, and contrasting Cockcroft-Gault estimation of GFR with the MDRD method.
Conclusions
More than 10% of patients in this analysis were found to have renal insufficiency consistent with the NKF's definition of stage 3 chronic kidney disease determined by decreased glomerular filtration rate. Only about 2% would have been identified if serum creatinine alone were used.
Patients with HIV infection are at risk for renal injury from HIV disease, comorbidities and therapy. The use of a more sensitive marker, like GFR, may be warranted for early detection of renal impairment.
References
1. Johnson CA, Levey AS, Coresh J, Levin A, Lau J, Eknoyan G. Clinical practice guidelines for chronic kidney disease in adults: Part II. Glomerular filtration rate, proteinuria and other markers. Am Fam Physician 2004; 70: 869-76.
2. Levey AS, Bosch JP, Lewis JF, Greene T, Rogers N, Roth D. A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation from Modification of Diet in Renal Disease study group. Ann Intern Med. 1993; 130-70.
3. Gault MH, Longerich LL, Harnett JD, Wesolowski C. Predicting glomerular function from adjusted serum creatinine. Nephron 1992; 62: 249-56.
4. Levey AS. Use of glomerular filtration rate measurements to assess the progression of renal disease. Semin Nephrol 1989; 9: 370-79.
5. Toto RD. Conventional measurement of renal function utilizing serum creatinine, creatinine clearance, inulin and para-amino hippuric acid clearance. Curr Opin Nephrol Hyperten 1995; 4: 505-09.
6. Pierrat A, Gravier E, Saunders C, Caira MV, Ait-Djafer Z, Legras B, Mallie JP. Predicting glomerular filtration rate in children and adults: a comparison of Cockcroft-Gault, Schwartz, and Modification in Diet on Renal Disease formulas. Kidney Intl 2003; 64:1425-36.
7. Kingdon EJ, Knight CJ, Dustan K, Irwin AG, Thomas M, Powis SH, Burns A, Hilson AJW, Black CM. Calculated glomerular filtration rate is a useful screening tool to identify scleroderma patients with renal impairment. Rheumatology 2003; 42:26-33.
8. Coca S, Perazella MA. Rapid communication: acute renal failure associated with tenofovir: evidence of drug-induced nephrotoxicity. Am J Med Sci 2002; 324 (6): 342-4.
9. Karras A, Lafaurie M, Furco A, Bourgarit A, Droz D, Sereni D, Legendre C, Martinez F, Molina JM. Tenofovir-related nephrotoxicity in human immunodeficiency virus-infected patients: three cases of renal failure, Fanconi syndrome, and nephrogenic diabetes insipidus. Clin Infect Dis 2003; 36 (8): 1070-3.
10. Verhelst D, Monge M, Meynard JL, Fouqueray B, Mougenot B, Girard PM, Ronco P, Rossert J. Fanconi syndrome and renal failure induced by tenofovir: a first case report. Am J Kidney Dis 2002; 40 (6): 1331-3.
11. Rosso R, Di Biagio A, Ferrazin A, Bassetti M, Ciravegna BW, Bassetti D. Fatal lactic acidosis and mimicking Guillain-Barre syndrome in an adolescent with human immunodeficiency virus infection. Pediatr Infect Dis J 2003; 22 (7): 668-70.
12. Rivas P, Polo J, de Gorgolas M, Fernandez-Guerrero ML. Drug points: Fatal lactic acidosis associated with tenofovir. BMJ 2003; 327 (7417): 711.
| |
| |
| |
|
 |
 |
|
|