| |
Prevalence of Drug-Resistant HIV-1 Variants in Untreated Individuals in Europe: Implications for Clinical Management, 3.5% 3-Class Resistant
|
| |
| |
.....in 1 of 10 antiretroviral-naive patients in Europe, viruses with resistance to at least 1 drug are found..... The possible impact of transmitted resistance on the susceptibility to the different antiretroviral drugs was calculated with 2 resistance interpretation algorithms. The predicted reduction in susceptibility was quite extensive for the class of nucleoside RT inhibitors (NRTIs; 18%-65% of all strains harboring drug-resistance mutations), was intermediate for NNRTIs (36% for all), and was less pronounced for the PIs (20%-25%).... Resistance to >1 class of drugs was observed in 19% (45/231) of patients carrying drug-resistant HIV variants, whereas resistance to all 3 classes was seen in only 3.5% (8/226)....
The Journal of Infectious Diseases
Sept 15, 2005;192:958-966
....We studied the rate of transmission of drug-resistant HIV-1 over time in Europe. The results of this international study showed that 10.4% of patients who had never been exposed to antiretroviral therapy carried HIV with >1 drug-resistance mutation...... We found a significant difference (P = .006) in the level of baseline resistance between recently infected patients (13.5%) and patients infected for >1 year (8.7%)..... The most commonly observed mutations in our study were those associated with resistance to the thymidine analogues zidovudine and stavudine.... The continuous transmission of drug-resistant viruses to newly infected patients demonstrates that a portion of HIV-infected individuals receiving antiretroviral medication is still engaging in risk-related behavior, despite awareness of their infection status..... preliminary data show that baseline resistance may compromise the response to antiretroviral therapy. In 3 studies, the time to viral suppression was significantly prolonged in individuals infected with drug-resistant HIV. Also, the time to virological failure was shorter if baseline resistance was present..... Recently updated guidelines recommend drug-susceptibility testing for patients presenting with recent infection (<1 year) and for all newly diagnosed cases when the regional prevalence in an area increases to >5% and >10%, respectively. Moreover, the results of modeling studies have suggested that offering genotypic resistance testing before the initiation of therapy was cost-effective in a US healthcare setting at a 4% prevalence of baseline resistance...... our data support genotypic resistance testing for all antiretroviral-naive individuals before combination therapy is selected.....
Authors: Annemarie M. J. Wensing,1,2 David A. van de Vijver,1 Gioacchino Angarano,4 Birgitta Åsjö,9 Claudia Balotta,5 Enzo Boeri,6 Ricardo Camacho,11 Maire-Laure Chaix,12 Dominique Costagliola,13 Andrea De Luca,7 Inge Derdelinckx,15 Zehava Grossman,16 Osamah Hamouda,18 Angelos Hatzakis,19 Robert Hemmer,20 Andy Hoepelman,2 Andrzej Horban,21 Klaus Korn,17 Claudia Kücherer,18 Thomas Leitner,22 Clive Loveday,23 Eilidh MacRae,23 Irina Maljkovic,24 Carmen de Mendoza,25 Laurence Meyer,14 Claus Nielsen,31 Eline L. Op de Coul,3 Vidar Ormaasen,10 Dimitris Paraskevis,19 Luc Perrin,26 Elisabeth Puchhammer-Stöckl,27 Lidia Ruiz,28 Mika Salminen,29 Jean-Claude Schmit,20 Francois Schneider,20 Rob Schuurman,1 Vincent Soriano,25 Grzegorz Stanczak,21 Maja Stanojevic,30 Anne-Mieke Vandamme,15 Kristel Van Laethem,15 Michela Violin,5 Karin Wilbe,24 Sabine Yerly,26 Maurizio Zazzi,8 and Charles A. Boucher,1 for the SPREAD Programmea
ABSTRACT
Background. Infection with drug-resistant human immunodeficiency virus type 1 (HIV-1) can impair the response to combination therapy. Widespread transmission of drug-resistant variants has the disturbing potential of limiting future therapy options and affecting the efficacy of postexposure prophylaxis.
Methods. We determined the baseline rate of drug resistance in 2208 therapy-naive patients recently and chronically infected with HIV-1 from 19 European countries during 1996-2002.
Results.
In Europe, 1 of 10 antiretroviral-naive patients carried viruses with >1 drug-resistance mutation.
Recently infected patients harbored resistant variants more often than did chronically infected patients (13.5% vs. 8.7%; P = .006).
Non-B viruses (30%) less frequently carried resistance mutations than did subtype B viruses (4.8% vs. 12.9%; P < .01).
Baseline resistance increased over time in newly diagnosed cases of non-B infection: from 2.0% (1/49) in 1996-1998 to 8.2% (16/194) in 2000-2001.
Conclusions. Drug-resistant variants are frequently present in both recently and chronically infected therapy-naive patients. Drug-resistant variants are most commonly seen in patients infected with subtype B virus, probably because of longer exposure of these viruses to drugs. However, an increase in baseline resistance in non-B viruses is observed. These data argue for testing all drug-naive patients and are of relevance when guidelines for management of postexposure prophylaxis and first-line therapy are updated.
DISCUSSION
We studied the rate of transmission of drug-resistant HIV-1 over time in Europe. The results of this international study showed that 10.4% of patients who had never been exposed to antiretroviral therapy carried HIV with ⩾1 drug-resistance mutation. This rate differs from that in several earlier reports. The previous studies included relatively small numbers of participants, were often limited to single countries, and varied widely in the type of mutations considered or the method used to determine resistance. As a consequence, the rate of new infections by drug-resistant HIV has been difficult to estimate on a continentwide scale [3]. To our knowledge, our study is the first to have analyzed a large resistance data set with uniform definitions that has taken into account duration of infection and variations in subtype.
As in any study of the transmission of resistance, it cannot be ruled out that patients who are considered to be antiretroviral naive might not have been truthful about their lack of exposure to therapy, which would result in an overestimation of baseline resistance. However, the prescription procedures in Europe (which are mainly done by HIV-specialized centers), reimbursement for therapy by national healthcare programs, and the high level of insurance coverage do not give reasons for hiding previous exposure to therapy.
Theoretically, differences in sampling strategy and size of the data sets could have influenced the results. To minimize sampling biases, no isolated clinical samples were included. All samples in the study were collected either as part of surveillance, as part of a standard practice of baseline resistance testing, or, less frequently, as baseline samples for transmission studies. We consider the influence of sample sizes of the data sets to be small, given that a weighted analysis showed that differences in sample size among countries barely influenced the overall rate of transmission.
Differences in the duration of infections may be more relevant. We found a significant difference (P = .006) in the level of baseline resistance between recently infected patients (13.5%) and patients infected for >1 year (8.7%). The lower prevalence of resistance in chronic infection is most likely due to a lower exposure to drug-resistant virus in the past. In addition, the lower prevalence can be explained by reversion from resistant variants to sensitive wild-type viruses over time [21]. Interestingly, drug-resistance mutations could still be detected in the plasma of quite a few chronically infected patients, which indicates that complete reversion does not always occur. Indeed, recent studies have indicated that drug-resistant viruses can persist for a couple of years in the plasma of treatment-naive HIV-infected patients [22, 23].
Differences in data sets among countries may also have resulted from specific biological and cultural characteristics as they relate to national epidemics, such as transmission routes, the proportion of non-B viruses, and prescription guidelines. For instance, the proportion of non-B subtypes seems to have a substantial influence on the frequency of baseline resistance. Resistance was higher in antiretroviral-naive patients who were infected with subtype B (12.9%) than in those infected with non-B viruses (4.8%). Moreover, in recently infected patients, the risk of being infected with drug-resistant HIV was 4 times higher in patients with subtype B infections (16%) than in patients with non-B infections (4%).
Subtype B was originally the predominant subtype in Europe and in North America, whereas non-B subtypes have spread widely in Africa and Asia. Differences in the prevalence of baseline resistance may thus likely reflect the longer period during which subtype B viruses have been exposed to antiretroviral drugs. Interestingly, we noticed a consistent increase in baseline resistance in non-B viruses. This trend is consistent with the increasing number of patients identified with non-B viruses in Europe who are currently being exposed to therapy [14, 24].
The most commonly observed mutations in our study were those associated with resistance to the thymidine analogues zidovudine and stavudine. Zidovudine and, to a lesser degree, stavudine have been extensively used as monotherapy or as part of dual therapy in the past and are frequently present in current regimens. Also, viruses with TAM resistance profiles may have better transmissibility and/or preservation in a drug-free environment, compared with viruses that contain other resistance mutations that more extensively compromise viral fitness.
The total number of recently infected patients with drug resistance displayed a fluctuating pattern over time (figure 2). This pattern results from changes in resistance to RT inhibitors and can be explained by several mechanisms. The initial high level of NRTI resistance most likely reflects less-effective viral suppression and the easy selection of drug resistance at the time of prescription of suboptimal monotherapy and dual NRTI therapy. The second phase reflects a decline in NRTI resistance after the introduction of highly active antiretroviral therapy (HAART), which results in a more-effective suppression of HIV replication. Because a low viral load has been associated with a reduced risk of sexual transmission [25], the introduction of HAART may account for the observed decrease in transmitted NRTI drug resistance.
The third phase, which is characterized by a sharp increase in NNRTI resistance, may reflect the enhanced use of NNRTI-based regimens, compared with PI-based regimens. An additional explanation may be a higher level of NNRTI resistance in the general population, given that NNRTIs have a lower genetic barrier to resistance and that just one point mutation can be sufficient to confer high-level resistance to this class of drugs [26]. In addition, viruses with NNRTI resistance may be more fit and therefore more able to establish infection in the new host, compared with PI resistance-related variants.
Our results may have important consequences for clinical management. The continuous transmission of drug-resistant viruses to newly infected patients demonstrates that a portion of HIV-infected individuals receiving antiretroviral medication is still engaging in risk-related behavior, despite awareness of their infection status [27]. These patients are receiving medical attention and should therefore be accessible targets for prevention programs.
Likewise, major concerns exist about the clinical impact of transmitted drug resistance. In the present data set, the loss in predicted susceptibility was most extensive for NRTIs, whereas predicted high-level resistance was more pronounced for drugs with a low genetic barrier, such as lamivudine and NNRTIs. The precise impact of transmitted resistance might be difficult to assess, because the correlation between baseline resistance and therapeutic response is influenced by the knowledge of baseline resistance patterns at time of the initiation of therapy and by the availability of alternative treatment options. Nevertheless, preliminary data show that baseline resistance may compromise the response to antiretroviral therapy. In 3 studies, the time to viral suppression was significantly prolonged in individuals infected with drug-resistant HIV [4, 5, 28]. Also, the time to virological failure was shorter if baseline resistance was present [5]. Additionally, individuals from the ICONA cohort harboring revertants or atypical mutants at position 215 of RT had an increased risk for selecting drug-resistance mutations and experiencing virological failure [6].
Recently updated guidelines recommend drug-susceptibility testing for patients presenting with recent infection (<1 year) and for all newly diagnosed cases when the regional prevalence in an area increases to >5% and >10%, respectively [1, 7]. Moreover, the results of modeling studies have suggested that offering genotypic resistance testing before the initiation of therapy was cost-effective in a US healthcare setting at a 4% prevalence of baseline resistance [29]. At present, most clinical centers in Europe do not perform baseline resistance testing as standard procedure. However, we have shown that considerable baseline drug resistance can be found in antiretroviral-naive patients even after they have been infected for >1 year. Therefore, our data support genotypic resistance testing for all antiretroviral-naive individuals before combination therapy is selected.
Additionally, when making decisions about initial therapy, one should consider the possibility that more-complex patterns are transmitted but that certain mutations are not frequently identified in antiretroviral-naive patients because of reversion and the resistance test's inability to detect minority variants. In the case of an inadequate virological response to initial therapy, resistance testing should be repeated early, to identify the rapid selection of former minority variants.
Finally, the resistance patterns observed in the present study represent the viruses that are currently circulating in Europe. Because the failure of postexposure prophylaxis has been described after exposure to drug-resistant HIV-1, the reduced susceptibility of these viruses should be taken into account when selecting prophylaxis for those patients for whom no source-related information is available [8, 9, 30].
In conclusion, in 1 of 10 antiretroviral-naive patients in Europe, viruses with resistance to at least 1 drug are found. This high prevalence should be taken into account when decisions are made about initial regimens for therapy-naive individuals and about the selection of drugs for prophylaxis. Continuous surveillance of the spread of drug-resistant HIV-1, as well as the distribution of non-B viruses, is of utmost importance.
RESULTS
Study population. We enrolled 2208 HIV-1-infected therapy-naive patients from whom a blood sample for HIV pol nucleotide sequence analysis was available during the period 1996-2002. Table 1 shows the characteristics of the patients, grouped according to duration of infection. All patients were naive for therapy at the time of testing; 1601 were newly diagnosed cases of HIV infection, and 607 were known to be chronically infected (>1 year). Of the newly diagnosed cases, 777 patients were identified to have a recent infection (>1 year) on the basis of negative or indeterminate HIV serological results. The remaining newly diagnosed cases (824) presented with an unknown duration of infection. Transmission routes were identified for 1571 patients. The most common transmission route was sexual contact, 678 (43%) through sex between men and 641 (41%) through heterosexual contact. Other transmission routes were intravenous drug use (239 [15%]) and exposure to HIV-infected blood (13 [1%]). At the time of resistance analysis, the median CD4+ cell count was higher in recently infected patients (500 cells/mm3) than in patients with chronic infection (313 cells/mm3) or patients with an unknown duration of infection (330 cells/mm3) (P < .001). The mean HIV RNA load was slightly higher in recently infected patients (5.03 log HIV RNA copies/mL) than in patients with chronic infection (4.65 log HIV RNA copies/mL) or an unknown duration of infection (4.71 log HIV RNA copies/mL) (P < .001). The proportion of recently infected patients varied between countries.
Resistance analysis. The percentage of antiretroviral-naive patients carrying HIV-1 with ⩾1 resistance-related mutation in Europe during 1996-2002 was 10.4% (95% confidence interval [CI], 9.1%-11.7%) (230/2208). The weighted analysis resulted in a comparable prevalence of 11.1% (95% CI, 9.6%-12.2%). The rate of transmission of drug resistance in each country varied from 0% (0/8) in the small data set from Finland to 23% (14/62) in Germany. Recently infected patients (105/777 [13.5%]) harbored resistant HIV variants more frequently than did patients with chronic infection or patients with infection of unknown duration (53/607 [8.7%] and 72/824 [8.7%], respectively) (odds ratio [OR], 1.6 [95% CI, 1.2-2.3]; P = .006). In the subset of patients for whom information on the route of transmission was available, we did not find statistically significant differences in the frequency of resistance (data not shown).
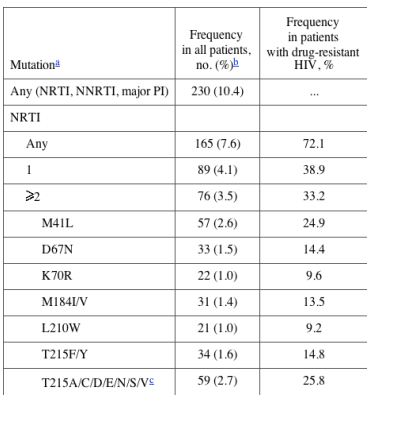
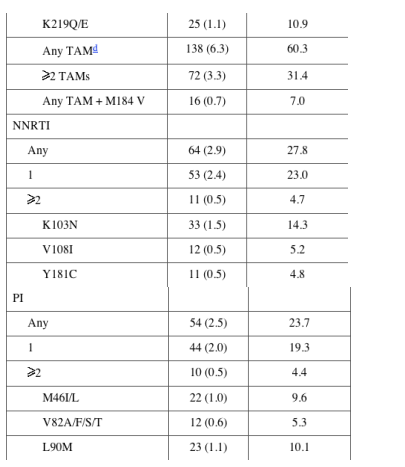
Genotypic profiles and predicted susceptibility. Table 2 shows the frequency of resistance-related mutations. Mutations associated with thymidine analogues (TAMs) (138/229 [60.3%]) were the most predominant. Among the TAMs, substitutions at RT codon 215, including those associated with partial reversion to drug-sensitive virus, were detected most frequently (93/229 [41%]). The most common nonnucleoside RT inhibitor (NNRTI)-related mutation was K103N, and the most common protease inhibitor (PI)-related mutation was L90M. Resistance to >1 class of drugs was observed in 19% (45/231) of patients carrying drug-resistant HIV variants, whereas resistance to all 3 classes was seen in only 3.5% (8/226).
The possible impact of transmitted resistance on the susceptibility to the different antiretroviral drugs was calculated with 2 resistance interpretation algorithms. The predicted reduction in susceptibility was quite extensive for the class of nucleoside RT inhibitors (NRTIs; 18%-65% of all strains harboring drug-resistance mutations), was intermediate for NNRTIs (36% for all), and was less pronounced for the PIs (20%-25%).
Time trends. For patients with a recent infection, the presence of >1 resistance mutation to any antiretroviral drug varied among time periods (figure 2). The initial relatively high proportion of resistance to NRTIs decreased significantly over time, from 13.4% (29/217) in 1996-1998, to 9.8% (44/448) in 1999-2000, and to 6.3% (6/95) in 2001-2002 (P = .048). In contrast, NNRTI-related resistance was initially low and displayed a significant increase through time, from 2.3% (5/217) in 1996-1998, to 3.1% (14/454) in 1999-2000, and to 9.2% (8/87) in 2001-2002 (P = .02). PI-related resistance remained relatively stable over time (2.8%, 4.4%, and 3.2%, respectively; P = .65).
Phylogenetic analysis. Phylogenetic analysis revealed that 70% of the patients were infected with subtype B virus (1535/2208). Thirty-six strains (36/2208 [2%]) could not be determined, because they did not cluster with any known subtype and were therefore scored as unclassified non-B subtypes.
Among non-B subtype, subtype C was the most prevalent (221/2208 [10%]), followed by subtype G (96/2208 [4%]) and CRF02_AG (94/2208 [4%]). The proportion of infections with non-B subtypes varied among countries, from 0% in Poland and Germany to >70% in Israel (82/104) and Portugal (69/91). Patients with an infection of known duration more frequently carried subtype B viruses (915/1431 [64%]) than did patients with an infection of unknown duration (473/824 [57%]) (P = .002).
Interestingly, subtype B viruses displayed a higher frequency of baseline drug resistance (198/1535 [12.9%]) than did non-B viruses (32/673 [4.8%]) (OR, 3.0 [95% CI, 2.0-4.4]) (P < .001). When the analysis was restricted to the subgroup of recently infected patients, the risk of being infected with a drug-resistant virus was 4 times higher in subtype B infections (99/620 [16%]) than in non-B infections (6/157 [3.8%]) (OR, 4.2 [95% CI, 1.9-9.4]; P < .001).
A multivariate analysis in the subset of patients with an infection of known duration showed that the difference in resistance between B and non-B subtypes was not confounded by time and duration of infection. The ORs of the univariate and multivariate analysis were 3.8 (95% CI, 2.1-6.7) (P < .001) and 3.7 (95% CI, 2.0-6.6) (P < .001), respectively. Nevertheless, a time-dependent increase in the rate of resistance was observed in all newly diagnosed cases of non-B infection: from 2.0% (1/49) in 1996-1998, to 3.0% (8/265) in 1999-2000, and to 8.2% (16/194) in 2000-2001.
INTRODUCTION
In countries with wide access to antiretroviral therapy, various drugs are currently available to suppress HIV-1 infection. Unfortunately, the frequent development of drug resistance during combination therapy limits the sustained response to antiretroviral drugs in many HIV-1-infected patients. Because cross-resistance is common, failure of therapy can also result in resistance to drugs that were not a part of the failing regimen. Drug-resistance testing of HIV-1 is therefore an important tool for the selection of subsequent regimens, and it has become a standard of care in the clinical management of therapeutic failure [1].
Suggestions have been made that viruses that contain mutations conferring drug resistance may be less transmissible than drug-sensitive virus [2]. However, over the past few years, transmission of all kinds of drug-resistant HIV-1 variants from therapy-experienced patients to newly infected individuals has been observed [3]. Recent publications have shown that the acquisition of an infection with drug-resistant HIV-1 may result in a less-favorable response to therapy [4-6].
Resistance testing before the initiation of therapy may help guide the optimal selection of antiretroviral drugs. Different categories of patients can be identified, depending on the duration of infection. For recently infected patients, current guidelines recommend drug-resistance testing before the initiation of therapy [1, 7]. For chronically infected patients, the guidelines are less concordant, because it is assumed that, in the absence of drug-selection pressure, reversion to or overtake by drug-sensitive virus can occur over time and preclude the detection of drug-resistant variants.
Widespread dissemination of drug-resistant HIV-1 variants has the serious potential to limit therapeutic options in new patients. In addition, the efficacy of postexposure prophylaxis may be affected by the circulation of drug-resistant HIV-1 [8, 9]. To gain insight into the prevalence of transmitted drug resistance in Europe in both categories of therapy-naive patients, a large study of 2208 therapy-naive HIV-1-infected patients from 19 European countries was conducted.
|
|
| |
| |
|
|
|