 |
 |
 |
| |
Report from the 7th International Workshop on Adverse Drug Reactions and Lipodystrophy in HIV
|
| |
| |
By
Carl Grunfeld, MD, PhD
Professor of Medicine, University of California, San Francisco
Chief, Metabolism and Endocrine Sections, Veterans Affairs Medical Center
Following selected summaries by Grunfeld are the full abstracts of studies presented at the Workshop. Jules Levin
A frequent topic of discussion at the meeting was a report from another meeting that was sponsored by The Forum for Collaborative HIV Research and preceded the workshop. (I did not attend the HIV Forum meeting.) That meeting focused on monitoring drug toxicities in resource poor settings. Many regimens in third world countries contain stavudine (d4T), whose toxicities have been well documented in the literature and at these Workshops. The sentiment of many was expressed best by Willi Rozenbaum who asked two questions. Why give so many millions of patients drugs such as stavudine with known toxicities when alternatives are available? Why spend money monitoring known toxicities? The response to the first question, given by Bill Powderly, was one of simple economics: stavudine regimens cost several hundred dollars less and that means many more people with HIV who will be treated in the third world. It is hard to argue with the latter, but one can hope that a way can be found to reduce the cost of less toxic regimens. With regard to why spend money to monitor the toxicities, some argued that the toxicities may be different in resource poor areas. Or they may be the same, but at higher rates. In that light, a poster by Gerard et al found that of 31 women of African origin treated with stavudine based regimens, 15 achieved viral suppression, but of those three developed severe (> 5mM) and three mild (2-5mM) lactatemia, while one developed peripheral neuropathy. While Gerard's study is too small to draw quantitative conclusions, it reinforced the worry that toxicities may be higher than expected. Nevertheless, many felt it unseemly that academics would jockey for grant money to study toxicities in the developing world because of drugs that we know are toxic.
Lipodystrophy
Gallagher discussed adipose tissue and its measurement. MRI is more informative than CT which in turn is more informative that DXA. Unfortunately, the cost is the opposite. In one study where 11.9 kg of weight was lost in obese subjects, 2.5 kg was lean and 9.4 kg was fat, of which 34.5 % was visceral adipose tissue (VAT). In thinner subjects, not as much VAT is lost with weight loss. The pattern of VAT may vary with disease. In some, VAT goes up to heart. In HIV it goes lower than controls. HIV+ children may have more VAT, but they also have more SAT. A large population-based study of children is needed. Elderly develop sarcopenia (age-related loss of muscle mass, strength & function; may be related to loss of neurons & function). Though there weight may be stable over time, they often lose lean and gain fat, especially intermuscular fat (beneath fascia and between muscle bundles). Increased intramuscular fat (within muscle fibers as measured by spectroscopy) is associated with insulin resistance in HIV and controls.
A reanalysis of the Mitox and Rosey studies (Wand et al, presented by Carr), looked at predictors of fat at baseline and after switch or treatment with rosiglitazone. They found a positive, not negative correlation between change in limb fat and VAT in men recovering form lipoatrophy. The factors associated with the two depots were, however, different. These data in prospective studies were described as consistent with the cross-sectional data from the FRAM study. (Note from Jules Levin: in other words, Carr says if limb fat loss & belly fat gain were a single process, then as limb fat gain occurs in Rosey & Mitox studies belly fat would decrease, but Carr found increases both in limb fat & in the belly correlated in this analysis he presented at Workshop. See Abstract 3 at the end of this report).
Continuing the increasing focus on lipoatrophy (risk factors) as the HIV-specific syndrome, Parker reported results from further analysis of ACTG 5005s, the substudy of 384. Lipoatrophy, defined as a decrease of 28% or more in limb fat, was found in 44% of those on d4T compared to 17% on AZT. There was also a small effect of PI (47% for PI 39% for NRTI in those on d4T). Greater baseline CD4 and BMI were also weak predictors of lipoatrophy. Triglycerides were increased in the ddI/d4T arm and were weakly associated with lipoatrophy. (Note from Jules Levin: Parker said in program abstract: The association between TG increase and lipoatrophy however appeared to be largely due to the effect of ddI+d4T assignment, where the median week 8 increase in TGs was 103 mg/dl in those with lipoatrophy (n=19) and 28mg/dl without (n=24); with ZDV+3TC, for those with lipoatrophy (n=6) TGs increased by median 24mg/dl, for those without (n=28) 26 mg/dl.). See Abstract 4 and 2 at end of report)
Sutinen presented further data on uridine supplementation with NucleomaxX in lipodystrophy. In a randomized, double-blind placebo controlled trial, they found an 800 gram fat gain in limb fat with uridine vs. only 200 gm in three months. While highly encouraging, the amount gained was small compared to the deficit. Larger and especially longer studies are needed to understand the potential of this interesting therapy. Of interest, VAT also increased (200 cm2 vs. -80), emphasizing once again that there is no inverse correlation between limb fat and VAT. The cost of 252 euros for one month at this dose is of concern. Banasch reported improvement in hepatic mitochondrial decarboxylation with NucleomaxX. However, McComsey had a poster showing no change in mitochondrial DNA in a small number of subjects given NucleomaxX. (Abstracts 7 & 82 below)
There continued to be switch studies presented in talks or posters, with the finding of recovery of limited amounts of limb fat. Benn reported a substudy of 47 lipoatrophic subjects from the RAVE study. They measured facial lipoatrophy by a laser scan costing 75 Euros as well as limb fat by DXA. Subjects were switched from a thymidine analogue to tenofovir or abacavir and studied 48 weeks later. Both groups had similar small increases in limb fat (0.36 kg), which were highly correlated with changes in face fat (r = 0.35-0.41 for correlation of limb fat to face fat). Most subjects did not report subjective improvement; those that did gained much more fat (ca. 3 kg). Zhong found an increase of only 0.42 kg limb fat at 48 weeks in 85 subjects switched from stavudine to tenofovir at the end of Gilead 9003A. Tsekes reported a 1 kg increase in leg fat in 10 subjects switched from stavudine to tenofovir. Hammond examined 68 biopsies from 32 males before and after switching from d4T or AZT. They found modest improvements in fat cell morphology and mitochondrial DNA (p = 0.008). IL-8 expression decreased and there was a trend for other cytokines to decrease. There was no significant gain in fat. Thus the consensus is that subjects switched off of thymidine analogues gain some fat, but most do not approach a normal amount.
Multiple posters on injections for treatment of lipoatrophy showed excellent looking restoration in the selected examples. One study by Fontivela injected silicone in buttocks and hips with improvement.
In a surprising secondary analysis, Mallon looked at body composition in a small (33 subject) study of the effects of pravastatin on cholesterol levels. Limb fat increased by 0.72 kg on pravastatin, but only 0.19 kg on placebo (p = 0.04). This unexpected finding needs conformation in a large study designed for such an endpoint. (see Abstract 23 below)
Examining metabolism in lipodystrophy, Grinspoon reported no decrease in glucose uptake into adipose tissue in subjects selected for lipoatrophy on a PI based regimen. Indeed, uptake in subcutaneous adipose tissue (SAT) was increased. If the primary driving force of lipoatrophy due to PI's was their ability to block insulin-stimulated glucose uptake into fat, one would expect there to have been a decrease. The interpretation of these results is that the proposed mechanism Of note BMI and VAT were lower in the subjects in this study than in his previous studies. Some of the defects described previously in lipodystrophy by this group may be due to the increase in VAT and not due to lipoatrophy, which we now know is the HIV-specific finding. (Grinspoon said in program abstract: This is the first study to directly demonstrate increased glucose uptake in subcutaneous fat of lipoatrophic patients, which may partially compensate for loss of subcutaneous adipose tissue. Furthermore, we demonstrate a clear relationship between VAT and glucose metabolism in multiple fat and muscle depots, suggesting the crucial importance of this depot in the regulation of glucose and highlighting the significant potential role of adiponectin in this process. (See abstract 14 below). (NOTE from Jules Levin: As well, Grinspoon reported that 46% prevalence of fatty liver was found in HIV+ individuals, abstract 47 can be read below). abdominal VAT was the strongest independent predictor of liver % fat. Fatty liver can result in elevated ALT, fibrosis, and reduced response to peginterferon therapy for hepatitis C. Nonetheless, fatty liver in HIV remains neglected as a potential health risk.
Shankar found no effect of four weeks of indinavir in healthy HIV-negative volunteers on adipogenic transcription factors, which are the proteins responsible for forming fat. This human study contrasts with studies of PI in cultured cells in vitro, where studies have shown decreases in such factors and investigators have extrapolated those cultured cell findings to suggest a mechanism for effects in patients on PI therapy. Shankar's results emphasize the always present need to direct study findings suggested from culture in humans under real-life conditions. If the proposed results are not found in humans, the mechanism may not be what is happening.
Balasubramanyam examined the role of leptin in the metabolic disturbances of HIV lipodystrophy. Leptin is a hormone that is made in fat cells. Severe loss of fat leads to low leptin levels and is associated with insulin resistance, high triglycerides and fatty liver in humans and mice; leptin therapy under those circumstances improves each metabolic parameter. Studies of the effects of ARV on cultured fat cells often find deceased leptin production. Leptin is being tested in HIV lipodystrophy. They compared subjects with HIV lipodystrophy and low leptin levels (using the common definition of < 4 ng/ml that is the entry for some HIV trials) to those with normal leptin levels. They found no association of leptin levels with metabolic abnormalities. They conclude either that low leptin levels play no role in the metabolic abnormalities of HIV lipodystrophy or that the definition of "low levels"
Kim found preservation of multiple mitochondrial enzyme activities despite mitochondrial depletion in patients with lipodystrophy. Levels of mRNA for Cox 2 were decreased, with those for Cox 4 increased. However, but Cox2 protein was unchanged. Cytochrome oxidase, another important mitochondrial enzyme was normal. Mitochondrial proliferation was seen. The effects on mitochondrial transcription factors were complex. A long list of complicated changes did not show a clear pattern suggesting a definitive mechanism for lipoatrophy. Review of many mitochondrial toxicity abstracts and papers reveals that there is no uniform hypothesis for how changes in mitochondria might cause changes in fat. More work is needed.
Yarasheski hypothesized that muscle mtDNA depletion may be associated with
HIV-metabolic syndromes. He quantified muscle mtDNA and mtRNA copy number per cell in vastus lateralis muscle samples (10mg) obtained after an overnight fast from 13 HIV-infected
subjects with impaired glucose tolerance (HIV+IGT), 10 HIV+ with normal glucose tolerance
(HIV+NGT), 12 HIV-seronegative controls (CTRL), and correlated these with parameters of glucose lipid, and amino acid metabolism measured during a hyperinsulinaemic-euglycaemic clamp, NRTI use and serum markers of inflammation. They reported finding mitochondrial DNA and morphology changes in muscle. They also found no change in key activities, such as in cytochrome oxidase and citrate synthase enzyme activity. BUT, there was no relation to abnormalities of glucose metabolism. Muscle is not severely affected by these drugs despite being highly dependent on mitochondria. These results again emphasize that the link between mitochondrial dysfunction and outcome is not clear.
Shikuma looked at HIV DNA and number of macrophages in adipose tissue in small numbers of subjects from a previous cross sectional study of lipoatrophy. They found more HIV DNA in PBMCs of lipoatrophic patients despite lower circulating HIV RNA levels. The types of circulating cells were not studied. There was a trend to more macrophages in adipose tissue by %CD68, but questions were raised about how to normalize in the face of lipoatrophy. Furthermore, those who were ARV naive and did not have lipoatrophy had as many macrophages. Nevertheless, this study provoked more interest in the issue of immune cells in adipose tissue.
Metabolism
Lee reported no effect of single dose of amprenavir on fasting glucose or insulin or insulin-stimulated glucose disposal in HIV-negative subjects. While amprenavir itself is no longer used, these data may explain why amprenavir was not associated with abnormalities of glucose metabolism in the past. The pharmacokinetics of amprenavir may play a role in these findings. Noor compared the effects on glucose and lipid metabolism of 10 days (time required to reach steady state levels) of boosted atazanavir to that of Kaletra in an open-labeled study compared to baseline. They found a non-significant 9-10% decrease in insulin mediated glucose disposal on ATVr vs. a significant 25% decrease on Kaletra. During oral glucose tolerance testing, both showed an increase in insulin levels. After 10 days triglycerides increased on both drugs, but the Kaletra effect was larger. These studies emphasize that PIs differ in their effects on metabolism. Some PI's have larger and some smaller effects on glucose or lipid metabolism, allowing one to tailor regimens when complications occur.
Diop reported that hemoglobin A1c may underestimate abnormalities in glucose metabolism in HIV infected subjects when there is hemolysis. An obvious conclusion is that one should follow glucose levels. However an interesting finding was that hemolysis was more common than expected. Low haptoglobin, a marker of hemolysis, was found in 22% of patients and correlated with lamivudine use. In contrast, zidovudine, stavudine and lamivudine were correlated with macrocytosis. Macrocytosis and anemia were not well correlated with haptoglobin.
Dube presented the ACTG Niaspan study. Of 34 subjects, there was a 38% decrease in triglycerides and a 15% increase in HDL. Most were on Kaletra. Of note, they did not exclude baseline defects in glucose metabolism. 42% had impaired fasting glucose or impaired glucose tolerance tests. While clinical laboratory values for glucose were not significantly different, central lab glucose rose slightly from 98.5 to 101 mg/dl. There were also increases in insulin and HOMA IR. This study is encouraging and similar to that in non-HIV-infected populations. On average there is likely to be little change in glucose, but some patients may be thrown out of control. The data do suggest that careful glucose monitoring is needed in HIV-infected patients put on nicotinic acid analogues.
Sakkas tested the effects in HIV of supplementation with creatine, a performance enhancing drug. They did not get an increase in phosphocreatine with creatine therapy at 20 gm/5d then 4.8 gm/d. They found a small increase in muscle mass, but absolutely no increase in muscle performance. There results were clear-cut and in contrast to studies in other disease states where creatine therapy has led to improvements.
Rose studied 25 HIV-infected subjects not on ARV (50% naive), 28 on PI-based HAART and 35 controls to look at the pathways that prevent or reverse atherosclerosis. HIV-infected subjects had more apo B, lower HDL-C, but similar apo A-I levels. A-1 was proportional to CD4. LCAT and CETP activities were higher. These proteins may be more atherogenic in the presence of hypertriglyceridenmia, as occurs in HIV. She postulated that HDL was less able to remove cholesterol from atherosclerotic plaque and deliver it to the liver for excretion. However, there was little difference between those on PI therapy and those not receiving PI therapy. These results predict more atherosclerosis in HIV infection regardless of antiretroviral therapy. (ED NOTE from Jules Levin. Rose said in program abstract: Reverse cholesterol transport (RCT) is a pathway that acts to remove excessive cholesterol from macrophages in the arterial wall to the plasma high density lipoprotein (HDL), thus protecting against development of atherosclerosis. RCT in HIV patients is diverted toward transferring cholesterol from anti-atherogenic HDL toward atherogenic apolipoprotein-B-containing lipoproteins. This would reduce the efficiency of RCT and consequently increase the risk of development of atherosclerosis. Our findings also suggest that CETP inhibitors may be effective for correcting the effect of HIV on RCT. Furthermore, our findings suggest that HIV infection itself, rather than treatment is likely to be the major contributor to the impairment of RCT in HIV patients. (see Abstract 21 below).
Cade found that HIV-infected subjects had higher palmitate oxidation at rest and with exercise than controls. Lipolysis was not different. HDL levels were lower. HIV-infected subjects also had lower diastolic velocity, a measurement of diastolic dysfunction and vascular disease. They had slightly higher ventricular mass. There were significant correlations of decreased function with the changes in HDL and oxidation. The authors found little effect of PI therapy. Cade said in program abstract: HIV infection, regardless of PI use, was associated with increased whole-body FFA oxidation rates during rest and exercise. Increased FFA oxidation and lower serum HDL levels were predictive of depressed
cardiac, specifically diastolic, function. (see abstract 22 below)
In the study of the effect of 40 mg pravastatin on cholesterol, Mallon found a small decrease in cholesterol AUC over the course of the study (-0.82 vs. -0.34 for placebo). However, pravastatin levels maybe decreased by PI therapy (in contrast to the increase seen with other statins) and the levels of pravastatin had not yet been analyzed.
Yki-Jarvenin presented the case in non-HIV infected subjects, fatty liver (steatosis) was the major change leading to increased hepatic glucose production, which in turn is the major determinant of fasting glucose. She feels that hepatic abnormalities are much more important than abnormalities in fat or muscle. She proposed that overeating increased fat cells, leading to macrophage recruitment causing hepatic insulin resistance via TNF. There was a strong correlation between VAT and steatosis. The data did not make a case that steatosis was more important than VAT. She did not address the role of intra- or inter-muscular fat.
Kidney
Klotman reported that in his New York hospital there are 30-40 inpatients with HIV at any time. Approximately one-third have some renal disease if which 12% have acute renal failure. Statewide, 6% of such patients have acute renal failure. 26.6% of those with acute renal failure die that admission vs. 4.5% of who do not. Among outpatients, Caucasians have mebranoproliferative glomerulopathy associated with hepatitis, Asians have IgA nephropathy with hepatitis, whereas African-Americans have HIVAN. HIVAN is the 3rd most common cause of ESRD in African-Americans > 20 yo. HIVAN kidneys are normal or large. Genetic background gives susceptibility, but most meet the criteria for AIDS. There is renal expression of HIV with gag protein in tubules. Although HAART has been reported to reverse ESRD in one patient they still see HIV DNA in kidney after HAART. Nef may be the gene responsible for proliferation via SRC and MAPK/Stat1 pathways. Dedifferentiation may be due to Rho A. In the Chelsea-Westminster cohort 28% had elevated creatinine. Treated patients had lower creatinine levels than not treated patients. More effective treatment gave less renal failure. There was no clear effect of tenofovir. He concluded that renal disease has emerged as a major complication of HIV and is often a direct effect of HIV in the kidney.
Cote did a retrospective analysis of kidney biopsies in patients who had received tenofovir within 6 mos of biopsy vs. 10 who were never on TDF. They found a decrease in mitochondrial DNA in the kidney that was more prominent in those on tenofovir plus ddI. Unfortunately they did not have biopsies in those on ddI without tenofovir and did not report on stavudine. In regression analysis, both HIV and tenofovir-ddI were associated with kidney mitochondrial changes. (see Abstract 17 below).
ABSTRACTS
ABSTRACT 21
Antiviral Therapy 2005; 10:L14
HIV-1 infection diverts reverse cholesterol transport toward atherogenic pathway
H Rose 1, J Hoy2, I Woolley2, A Dart 1 and D Sviridov 1
1Baker Heart Research Institute, Melbourne, Victoria, Australia;
2Department of Infectious Diseases, Alfred Hospital, Melbourne,
Victoria, Australia
Background: HIV infection and its treatment with protease inhibitors (PI) is associated with an atherogenic lipid profile including hypoalphalipoproteinaemia, yet no study has investigated the impact of HIV on specifically reverse cholesterol transport (RCT). RCT is a pathway that acts to remove excessive cholesterol from macrophages in the arterial wall to the plasma high-density lipoprotein (HDL), thus protecting against development of atherosclerosis. HDL is then re-modelled through esterification of its cholesterol, by lecithin cholesterol acyl-transferase (LCAT), and by exchanging cholesteryl esters and phospholipids
with other lipoproteins through the action of cholesterol ester transfer protein (CETP) and phospholipids transfer protein (PLTP). The proportion of cholesterol delivered to the liver for excretion or to the atherogenic lipoproteins may determine the protective efficiency of RCT.
Methods: A 20 ml blood sample was taken from male volunteers; 33 HIV-negative controls, 25 HIV-positive untreated patients and 28 HIV-positive PI-treated patients. Lipids, lipoproteins and RCT transfer protein's mass and activities were measured. Viral load, CD4+ cell count and CD4 % were also measured for subjects in the HIV groups.
Results: Plasma triglyceride level, mass and activity of LCAT and CETP activity were all significantly higher in both HIV groups compared with the control (P<0.05). Plasma HDL-C and preb1-HDL levels were significantly lower in both HIV groups (P<0.05), whereas plasma
apolipoprotein A-I (apoA-I) levels were unchanged. There was a significant positive correlation between apoA-I and CD4+ cell levels in the combined HIV data (r=0.5,
P<0.01). There was no difference between treated and untreated HIV patients in all but one of the RCT parameters. The only parameter affected by treatment was a significantly lower activity of PLTP (P<0.05).
Conclusions: Reverse cholesterol transport in HIV patients is diverted toward transferring cholesterol from anti-atherogenic HDL toward atherogenic apolipoprotein-B-containing lipoproteins. This would reduce the efficiency of RCT and consequently increase the risk of
development of atherosclerosis. Our findings also suggest that CETP inhibitors may be effective for correcting the effect of HIV on RCT. Furthermore, our findings suggest
that HIV infection itself, rather than treatment is likely to be the major contributor to the impairment of RCT in HIV patients.
ABSTRACT 22
Antiviral Therapy 2005; 10:L15
Diastolic function is associated with whole-body palmitate oxidation and serum high density lipoprotein in HIV+ subjects taking ART
WT Cade 1, DN Reeds 1, V Davila-Roman1, A Waggoner 1, S Klein 1, WG Powderly 2 and
KE Yarasheski1
Washington University School of Medicine, St. Louis, MO, USA;
2University College Dublin, Dublin, Ireland.
Objectives: HIV and protease inhibitor (PI)-based antiretroviral treatment (ART) are associated with abnormal lipid metabolism and diastolic dysfunction. We used submaximal
exercise to stimulate whole-body lipolysis and free fatty acid (FFA) oxidation and examined relationships among FFA kinetics, resting cardiac function and PI use in HIV+ taking PI (ritonavir)-based ART (HIV+PI), HIV+ taking NRTI-based ART (HIVnoPI) and HIV-negative
controls (Ctrl). We hypothesized that HIV+PI would have higher lipolytic rates and lower FFA oxidation rates during rest and exercise than HIVnoPI and Ctrl and that FFA kinetics would be associated with abnormalities in cardiac function.
Methods: 1-13C palmitate was infused during rest and 70 min of submaximal exercise (50% peakVO2) to quantify basal and exercise-stimulated lipolytic rate (PalmRa) and palmitate oxidation rate (PalmOx) in three groups: HIV+PI (n=10), HIVnoPI (n=9) and Ctrl (n=5). Resting 2D and Doppler echocardiography was used to quantify cardiac contractile and anatomic parameters.
Results: In contrast to our hypothesis, PalmRa was similar among the three groups during rest and exercise. Resting PalmOx was higher in HIV+PI (1.0±0.5, P<0.05) than Ctrl (0.4±0.1), but was not different between Ctrl and HIVnoPI (0.8 ±0.4 mmol/kgFFM/min). When
HIV+ groups were combined, PalmOx during rest (0.9±0.4 vs 0.4±0.1) and during exercise (2.0±0.9 vs 0.8±0.4 mmol/kgFFM/min, P<0.03) were higher than Ctrl. HIV+ subjects exhibited lower early diastolic velocity (global em: 12.0±4.0 vs 16.4±3.8 m/s, P<0.02) and peak early (E) to peak late (A) diastolic flow velocity ratio (E/A ratio: 1.4±0.4 vs 2.1±0.5, P<0.001) while left ventricular mass index (LVMI) tended to be greater (97.1±14.4 vs 86.1±6.2g/m2, P<0.09) than Ctrl. PalmOx during exercise was related to LVMI (r=0.46, P<0.05). Serum high-density lipoprotein (HDL) levels were positively related to global em (r=0.58, P<0.003), ejection
fraction (r=0.37, P<0.08), flow propagation (r=0.56, P<0.006), E (r=0.44, P<0.03), E/A (r=0.55, P<0.006) and negatively related to mean arterial pressure (r=-0.49, P<0.02) and diastolic BP (r=-0.49, P<0.02).
Conclusions: HIV infection, regardless of PI use, was associated with increased whole-body FFA oxidation rates during rest and exercise. Increased FFA oxidation and lower serum HDL levels were predictive of depressed cardiac, specifically diastolic, function.
Acknowledgements: Supported by NIH.
ABSTRACT 17
Antiviral Therapy 2005; 10:L12
Mitochondrial nephrotoxicity, a potential mechanism of kidney dysfunction in HIV-infected patients on HAART
HCF Cote 1,3, AB Magil2,3, M Harris 1, BJ Scarth1,
I Gadawski1, NY Wang1, E Yu4, B Yip1,
N Zalunardo2, R Werb 2, RS Hogg1, PR Harrigan1
and JS Montaner1
1British Columbia Centre for Excellence in HIV/AIDS, Providence Health Care, Vancouver, B.C. Canada; 2St. Paul's Hospital, Providence Health Care, Vancouver, B.C. Canada; 3Department of Pathology & Laboratory Medicine, University of British Columbia,
Vancouver, B.C., Canada; 4Centre for Health Evaluation and Outcome Sciences, St. Paul's Hospital, Vancouver, B.C., Canada
Background: Tenofovir disoproxil fumarate (TDF) use has been associated with renal dysfunction. Mitochondrial nephrotoxicity was investigated as a potential mechanism. Given the known pharmacokinetic interaction between TDF and didanosine (ddI), the effect
of their concurrent use was also investigated.
Methods: Relative kidney mitochondrial DNA (mtDNA) to nuclear DNA ratios were measured retrospectively in diagnostic kidney biopsies divided into three groups: HIV-infected
individuals who received TDF within 6 months preceeding the biopsy (HIV+/TDF+, n=21, 13 with acute tubular necrosis [ATN]); HIV+ individuals who never received TDF (HIV+/TDF-, n=10, 3 ATN); HIV-uninfected controls (HIV-, n=22, 12 ATN). Twelve HIV+/TDF+ individuals received concurrent ddI, 10 of them at unadjusted dose. Tubular mitochondria morphology was also examined by electron microscopy. Statistical analyses were done on log-transformed mtDNA ratios, using non-parametric tests.
Results: Relative kidney mtDNA levels were different among the three groups (P=0.046). Median [IQR] mtDNA ratios were lower in HIV+/TDF+ subjects (7.5 [2.0-12.1]) than in HIV-uninfected ones (14.3 [6.0-16.5], P=0.014), but not lower than HIV+/TDF- controls (6.4
[2.8-11.9], P=0.82).
Among HIV+ subjects, there was a difference between TDF-, TDF+/ddI- and TDF+/ddI+
(P=0.005), as concurrent use of TDF/ddI was associated with lower mtDNA (2.1 [1.9-5.5]; n=12) than TDF use without ddI (13.8 [7.5-16.4]; n=9, P=0.003), with a similar prevalence of ATN in both groups. No TDF-/ddI+ biopsies were available.
In regression analyses adjusting for age, gender, HIV, ATN and the use of TDF±ddI, only
HIV infection (P=0.03), and TDF/ddI use (P=0.003) were associated with lower mtDNA. Ultrastructurally, abnormal tubular mitochondrial morphology was more prevalent
in HIV+/TDF+ biopsies than HIV+/TDF- and HIV- ones together (P<0.001) but not more so in TDF+/ddI+ biopsies than TDF+/ddI- ones (P=0.67). None of the co-variates tested were significantly associated with abnormal mitochondria.
Conclusions: Renal dysfunction in patients receiving TDF can be mediated through mitochondrial nephrotoxicity, influenced by both HIV infection and concurrent TDF/ddI
therapy, two drugs that are cleared renally. The current clinical relevance of these findings needs to be further evaluated given the recommendation for lower doses of ddI when used with TDF.
ABSTRACT 3
Antiviral Therapy 2005; 10:L5
Increase in limb fat after nucleoside analogue cessation is not associated with decreased visceral fat and has different risk factors
H Wand1, MG Law1, S Emery1, DA Cooper1,2 and
A Carr 2 for the MITOX and ROSEY Study Groups
1National Centre in HIV Epidemiology and Clinical Research,
University of New South Wales; 2St Vincent's Hospital, Sydney, Australia
Objectives: No patient characteristic is known to predict lipoatrophy improvement after stopping thymidine nucleoside analogues. It is also unknown whether lipoatrophy
and central fat accumulation represent a single process or are at least partially independent. If a single process, lipoatrophy improvements should inversely correlate with changes in visceral adipose tissue (VAT) and risk factors for lipoatrophy and VAT improvements should be similar. We evaluated long-term data from two randomized lipoatrophy trials: MITOX (a switch from d4T [n=85] or AZT [n=26] to abacavir for 24 weeks), and ROSEY (rosiglitazone
[RSG; n=53] or placebo [n=55]).
Methods: All participants (98% male) had moderate-severe lipoatrophy in 1 region (face, arms, legs, buttocks) and were followed for 72 weeks. Factors associated with
increasing limb fat (0.5kg) and decreasing VAT were assessed and included HIV duration, baseline age, CD4+ cell count, viral load, body composition and lipid and glycaemic parameters. Changes in limb fat mass (DEXA) were correlated with changes in VAT area (computed tomography).
Results: There was a significant, although relatively weak, positive correlation between the changes in limb fat mass and VAT (week 48: r=0.19, P=0.01; week 72: r=0.25, P=0.001). Limb fat increased by 0.5kg in only 23%, 33% and 41% of patients at 24, 48 and 72 weeks, respectively.
The only baseline parameter significantly correlated with a 0.5kg increase in limb fat was higher baseline body mass index (OR 1.6 [95%CI 1.3, 2.0]; P<0.0001); increase in
VAT at week 72 was independently associated with 0.5kg increase in limb fat (OR 1.02 [95%CI 1.01, 1.04]; P=0.001).
In contrast, independent risk factors at baseline for a decrease in VAT were higher limb fat mass (P<0.0001), lower HDL-C (P=0.002) and higher insulin (P=0.03), as well as a greater decrease in limb fat to week 72 (P<0.0001). Changes in subcutaneous abdominal fat
also correlated positively with change in limb fat mass (week 48: r=0.19, P=0.01; week 72: r=0.24, P=0.001).
Conclusions: An increase in limb fat in men recovering from lipoatrophy is not associated with a reduction in VAT, but rather an increase. Changes in limb fat and VAT also have
differing risk factors. Both findings suggest that lipoatrophy and visceral obesity are at least partially independent processes. Lipoatrophy improved in 50% of patients after 18 months and was less likely in those with lower BMI.
ABSTRACT 4
Antiviral Therapy 2005; 10:L5
Baseline and early on-treatment predictors of lipoatrophy at 64 weeks in a randomized trial of initial antiretroviral therapy: a secondary analysis of A5005s, a substudy of ACTG 384
RA Parker 1,2, L Komarow1,2, SK Grinspoon2, K Mulligan3, GK Robbins 2, P Tebas 4 and MP Dube 5
1Statistical and Data Analysis Center, Boston, MA, USA; 2Harvard
University, Boston, MA, USA; 3UCSF, San Francisco, CA, USA;
4University of Pennsylvania, Philadelphia, PA, USA; 5Indiana University, Indianapolis, IN, USA
Background: Observational studies have reported many non-drug risk factors for lipoatrophy. We sought to identify baseline characteristics and early on-treatment
metabolic changes predictive of lipoatrophy.
Methods: Antiretroviral-naive subjects were randomized to nelfinavir, efavirenz or both with ZDV+3TC or ddI+d4T. DEXA was available at entry and week 64 for 102 subjects; 95 subjects had baseline lipids and 77 also had week 8 lipids available. One-third had lipoatrophy, defined as >20% decrease in limb fat from baseline. Individual variables were screened using standard tests (Wilcoxon Rank Sum; Fisher's Exact test); logistic regression
was used for multivariate analyses.
Results: In univariate analyses, higher baseline (pre-ART) CD4, body mass index (BMI), triglycerides (TGs) and cholesterol and assignment to ddI+d4T were associated
with an increased risk of lipoatrophy at week 64 (each P=0.2).
At week 8, larger increases in TGs and cholesterol were associated with an increased risk of lipoatrophy, but changes in fasting C-peptide, HOMA-IR, and HDL-C were not. In multivariate models, the odds ratio for developing lipoatrophy was 3.27 (95% CI: 1.40-7.63) for a
100 mg/dl increase in TGs at week 8 and was 3.19 (0.99-10.22) for assignment to ddI+d4T; baseline BMI, CD4 and RNA were not significant predictors after adjustment for these factors. The association between TG increase and lipoatrophy however appeared to be
largely due to the effect of ddI+d4T assignment, where the median week 8 increase in TGs was 103 mg/dl in those with lipoatrophy (n=19) and 28mg/dl without (n=24); with ZDV+3TC, for those with lipoatrophy (n=6) TGs increased by median 24mg/dl, for those without (n=28) 26 mg/dl.
Conclusions: Nucleoside assignment, greater baseline CD4 and BMI, but not age, sex or white race were associated with lipoatrophy in univariate analyses. Baseline TGs and cholesterol (and their early changes), but not measures of glucose metabolism, were associated with lipoatrophy. In multivariate models, increases in TGs and ddI+d4T treatment were associated with lipoatrophy. We did not find evidence of an association between lower
nadir CD4+ cell counts and white race with lipoatrophy.
ABSTRACT 2
Antiviral Therapy 2005; 10:L4
Assessing the contribution of ART, HIV and host factors to adipose tissue changes occurring in HIV-infected individuals: risk profile for lipoatrophy
E Hammond1, D Nolan1, E McKinnon1, C Pace1, C Metcalf 2 and S Mallal1
1Royal Perth Hospital, Murdoch University and the Institute for Clinical Research; 2Royal Perth Hospital, Australia
Objectives: For HIV-infected individuals receiving antiretroviral therapy (ART), the development of lipoatrophy significantly impacts clinical management. To identify critical risk factors for lipoatrophy, we assessed in vivo adipose tissue changes occurring longitudinally
in HIV-infected patients.
Methods: Subcutaneous fat (n=68 biopsies; n=32 individuals) was paraffin processed and stained by immunohistochemistry for scoring of macrophage numbers and adipocyte-specific protein expression of cytokines (IL-18, IL-6, TNFa, IL-8, IL-12). Data was analysed cross-sectionally and for changes over time (median=7.0, IQR=5.9-10.1 months). Data included samples from individuals initiating [zidovudine (AZT) n=6; stavudine (d4T) n=7; abacavir (ABC)/non-thymidine n=6], switching (d4T onto AZT/ABC n=8; AZT onto ABC n=2) or continuing therapy (n=7). Mitochondrial DNA (mtDNA) content and relative transcriptional expression of caspase I, IL-18, IL-6, TNFa, adiponectin and PPAR-g were also measured
in frozen biopsies (AZT n=6; d4T n=10; naive n=14; ABC n=13). The influence of ART, disease and host-related factors on these endpoints was investigated.
Results: Cross-sectional analysis revealed protein expression of all cytokines correlated with current ART (all P<0.03), with each other (all P<0.001), %leg fat/BMI (all P<0.05), %leg fat (all P<0.01), and macrophage count (all P<0.001).
Neither cytokine expression nor macrophage count was independently associated with viral load, age, BMI, CD4 or HOMA score, although, TNFa expression correlated with BMI (P=0.04) in ART-naive individuals.
Initiating d4T or AZT was associated with increases in mtDNA depletion (P=0.003), macrophage count (P=0.006) and protein expression of cytokines (TNFa, IL-6, IL-8, IL-12 all P<0.03, IL-18 P=0.06). Initiating ABC (in the absence of thymidine therapy) was not associated with any outcomes (P>0.2). No significant effect of protease inhibitor therapy was detected.
Switching from d4T or AZT was associated with modest improvements in tissue morphology and improvements in mtDNA depletion (P=0.008), macrophage numbers and expression of all cytokines, but significance was restricted to IL-8 (P=0.008). Fat gain (positive changes in % leg fat/BMI) was undetectable. Gene expression data failed to show significant
correlations with protein expression (all P>0.05).
Conclusions: Profiling of adipose tissue morphology, cytokine protein expression and mtDNA depletion identified ART [d4T>AZT>ABC (without d4t/AZT)= naive], but not viral or host variables, as risk factors for lipoatrophy.
ABSTRACT 7
Antiviral Therapy 2005; 10:L7
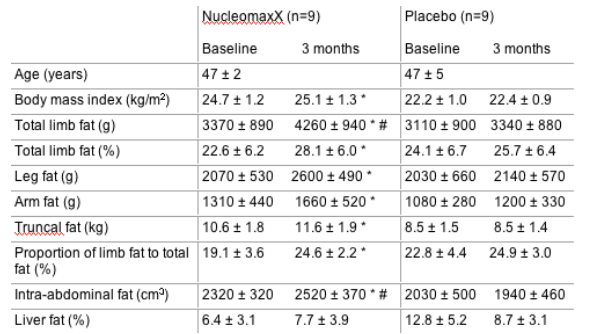
Uridine supplementation increases subcutaneous fat in patients with HAART-associated lipodystrophy: a randomized, placebo-controlled trial
J Sutinen1, UA Walker 2, K Sevastianova1,
AM Hakkinen1, M Ristola1 and H Yki-Jarvinen1
1Helsinki University Central Hospital, Helsinki, Finland; 2Freiburg
University Hospital, Freiburg, Germany
Objectives: In vitro, uridine abrogates NRTI-induced mitochondrial toxicity on adipocytes. The aim of the study was to investigate the effects of uridine on highly active antiretroviral therapy (HAART)-associated lipodystrophy (HAL).
Methods: Twenty patients with HAL were randomized to receive either NucleomaxX, a dietary supplement which increases uridine serum levels (36 g NucleomaxX three
times a day for 10 days/month) or placebo for 3 months. Body composition was measured using DEXA and MRI. Liver fat was quantified by proton spectroscopy.
Results: Eighteen patients completed the study. There were no significant differences between the groups at baseline.
Conclusions: NucleomaxX increased predominantly the amount of subcutaneous fat, but did not change liver fat content in lipoatrophic patients with unchanged HAART.
ABSTRACT 82
Antiviral Therapy 2005; 10:L49
Effect of NucleomaxX on fat and blood mitochondrial DNA in d4T-treated subjects with clinical lipoatrophy
GA McComsey1,2, M O'Riordan1, B Setzer 3,
D Lebrecht3, E Baron2 and UA Walker 3
1Rainbow Babies and Children's Hospital; 2Case Western Reserve
University, Cleveland, Ohio; 3Medizinische Universitätsklinik,
Freiburg, Germany
Background: Uridine abrogates mitochondrial toxicities of NRTIs in adipocyte cell culture. The effect on human adipocyte mtDNA levels is unclear.
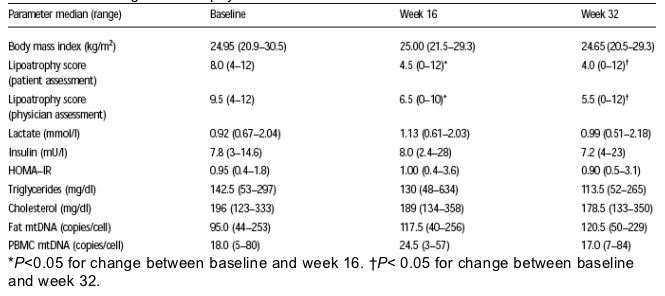
Methods: Sixteen patients with lipoatrophy on d4T containing HAART were enrolled, and received NucleomaxX, a dietary supplement which effectively increases serum uridine (36g TID every other day for 16 weeks). Patients were then followed off-uridine on the same HAART for another 16 weeks.
Results: Fourteen patients completed the study (median age 49 years, 10 males). Two subjects dropped out before week 4 due to loss of follow up. No subject modified
his HAART during the trial. No adverse events were noted throughout the study. HIV-1 RNA, CD4, ALT and haemoglobin levels didn't change significantly. At study entry, fat mtDNA correlated negatively with the lipoatrophy score generated by the patients (r=-0.82; P=0.0003) and by the physician (r=-0.47; P=0.09).
Conclusions: NucleomaxX is safe and well-tolerated in HIV-infected subjects with lipoatrophy. Despite an improvement in patient- and physician-generated clinical
lipoatrophy score, no significant changes in fat or PBMC mtDNA levels were seen after 16 weeks of NucleomaxX. Our results suggest that pyrimidine-depletion could be one of the factors contributing to fat atrophy.
ABSTRACT 23
Antiviral Therapy 2005; 10:L15
Changes in body composition and cardiovascular measures in hypercholesterolaemic HIV-infected men treated with pravastatin: a randomized, placebo-controlled study
PWG Mallon1,2, J Miller 2, J Kovacic 3, J Kent-Hughes 2, R Norris 2, K Samaras 4, M Feneley 3, DA Cooper 1,2 and A Carr 2
1National Centre in HIV Epidemiology and Clinical Research, University of New South Wales; 2HIV, Immunology and Infectious Diseases Clinical Services Unit, St Vincent's Hospital;
3Department of Cardiology, St Vincent's Hospital; 4Garvan Institute of Medical Research, Sydney, Australia
Objectives: Protease inhibitor (PI) use is associated with hypercholesterolaemia, peripheral lipoatrophy and central fat accumulation. We aimed to determine the effect of the
HMG-CoA reductase inhibitor pravastatin in HIV-infected, PI-treated men with hypercholesterolaemia.
Methods: A randomized, placebo-controlled, 16-week study of pravastatin 40mg daily in 33 HIV-infected men on stable PI therapy (HIV RNA <400 copies/ml) with high fasting cholesterol (>6.5 mmol/l). Subjects commenced a lipid-lowering diet at week 0 and were randomized to pravastatin or placebo at week 4. Primary endpoint was time-weighted change (AUC) in total cholesterol from week 0. Secondary endpoints included AUC cholesterol
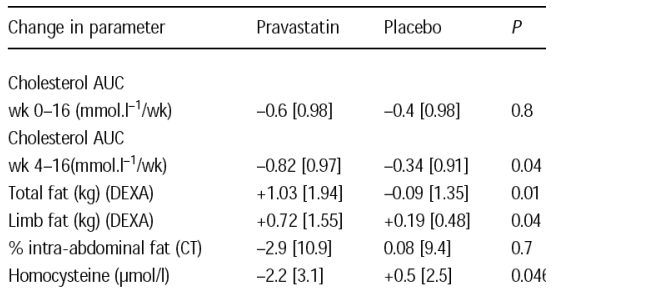
from week 4 (start of pravastatin), body composition (DEXA and abdominal CT), high density lipoprotein cholesterol, triglycerides, glucose, insulin, endothelial function (flow mediated vasodilatation [FMV]) and markers of cardiovascular risk (homocysteine, hs-CRP, fibrinogen and PAI-1). Non-parametric analyses were used and results presented as median [IQR].
Results: Of 33 men enrolled (pravastatin n=16), 31 completed the study. Groups were matched for baseline cholesterol (7.6 [1.7] pravastatin vs 7.6 [1.4] mmol/l placebo) and body composition, but the pravastatin group was older (52 [12] vs 43 [9] years) with greater endothelial dysfunction (%FMV 3.2 [3] vs 4.7 [3.4]). Although there was no significant difference in AUC cholesterol from week 0 between groups, AUC cholesterol from week
4 decreased more in the pravastatin group (Table 1). Total fat, predominantly limb fat, increased significantly in the pravastatin group. Apart from homocysteine, which
decreased in the pravastatin group, there were no significant differences in other cardiovascular, lipid, glucose or dietary parameters.
Conclusions: Despite limited effects on cholesterol, use of pravastatin 40mg daily for 12 weeks in this population resulted in significant increases in limb fat.
ABSTRACT 14
Antiviral Therapy 2005; 10:L10
Depot specific regulation of glucose intake and insulin sensitivity in HIV lipodystrophy
D Kamin1, C Hadigan1, J Liebau1, S Mazza1, S Barrow2, M Torriani 3, R Rubin4, S Weiss 2,
A Fischman2 and S Grinspoon1
1Program in Nutritional Metabolism, Massachusetts General Hospital, Boston, MA, USA; 2Nuclear Medicine Division, Massachusetts General Hospital, Boston, MA, USA; 3Division of
Musculoskeletal Radiology, Massachusetts General Hospital, Boston, MA, USA; 4Infectious Diseases Division, Brigham and Women's Hospital, Boston, MA, USA
Background: Altered fat distribution is associated with insulin resistance in HIV, but little is known about regional glucose metabolism in fat and muscle depots in this patient population. The aim of the present study was to quantify regional fat, muscle and whole body glucose disposal in HIV-infected men with lipoatrophy.
Methods: Whole body glucose disposal was determined by hyperinsulinaemic clamp technique (80mU/m2/min) in six HIV-infected men and five age-weight-matched
healthy volunteers. Regional glucose uptake in muscle, subcutaneous and visceral adipose tissue (VAT) was quantified in fasting and insulin-stimulated states using 2[18F]fluoro-2-deoxy-D-glucose (FDG) positron emission tomography (PET).
Results: HIV-infected subjects with lipoatrophy had significantly increased glucose uptake into subcutaneous adipose tissue (3.8±0.4 vs 2.3±0.5 mmol/kg tissue/min, P<0.05) in
the fasted state. Glucose uptake into VAT did not differ between groups. VAT area was inversely related with whole body glucose disposal, insulin sensitivity, and muscle glucose
uptake during insulin stimulation. VAT area was highly predictive of whole body glucose disposal (r2=0.94, P<0.0001). This may be mediated by adiponectin, which was significantly
associated with VAT area (r=-0.75, P=0.008) and whole body glucose disposal (r=0.80, P=0.003).
Conclusions: This is the first study to directly demonstrate increased glucose uptake in subcutaneous fat of lipoatrophic patients, which may partially compensate for loss of subcutaneous adipose tissue. Furthermore, we demonstrate a clear relationship between VAT and glucose metabolism in multiple fat and muscle depots, suggesting the crucial importance of this depot in the regulation of glucose and highlighting the significant potential role of adiponectin in this process.
ABSTRACT 47
Antiviral Therapy 2005; 10:L30
Hepatic steatosis and insulin resistance in HIV infection
J Liebau1, R Andersen1, S Grinspoon1, N Holalkere 2, D Sahani 2 and C Hadigan1
1Program in Nutritional Metabolism, Massachusetts General Hospital, Boston, MA, USA; 2Department of Radiology, Massachusetts General Hospital, Boston, MA, USA
Objectives: HIV-infected patients have a number of potential risk factors that may predispose them to the development of hepatic steatosis, including increased visceral fat,
hyperlipidaemia, insulin resistance, HCV co-infection and drug toxicities. The aim of the study was to evaluate HIV-infected men and women for hepatic steatosis using noninvasive
MR spectroscopy (MRS) and to evaluate the relationship between liver fat content, insulin resistance and other associated risk factors.
Methods: We examined 28 consecutively recruited HIV-infected subjects (21 men and 7 women) without specific referral for liver disease from community-based organizations.
Subjects with alcohol abuse within 3 years were excluded. The primary clinical measures were homeostatic model for assessment of insulin resistance (HOMA-IR) calculated from fasting insulin and glucose, liver fat content measured by MRS and visceral abdominal fat area (VAT) measured by computed tomography.
Results: Steatosis (defined as liver % fat >5) was found in 13 (46%) subjects. Subjects with steatosis were older [48 (3) vs 42 (2) years, P=0.04], more likely to be male [male/female ratio 12/1 vs 9/6, P=0.04] and had higher mean HOMA-IR [2.9 (0.6) vs 1.5 (0.2), P=0.03], alanine aminotransferase [64 (7) vs 43 (3) U/L, P=0.005], and VAT [17 249 (2532) vs 9852 (1123) mm2, P=0.01] compared to subjects without steatosis.
We identified a strong positive correlation between liver % fat and VAT (r=0.71, P<0.0001) and liver % fat and HOMA-IR (r=0.58, P=0.0014). A positive history of HCV co-infection or past alcohol abuse was not associated with increased steatosis. There was no difference in CD4 T cell count between subjects with and without steatosis. In a multivariate regression
model, abdominal VAT was the strongest independent predictor of liver % fat (P<0.005).
Discussion: We identify a high prevalence of steatosis among HIV-infected subjects. Subjects with steatosis had significantly greater insulin resistance and increased visceral adipose tissue, and these variables were tightly correlated with the degree of hepatic steatosis. Further studies are needed to determine the prevalence and extent
of steatosis in the general population of HIV-infected patients. Our data suggest that hepatic steatosis is a common finding and we show strong correlations between steatosis and risk factors known to be associated with fatty liver in the general population.
|
|
| |
| |
|
 |
 |
|
|