| |
Heart Disease Prevention in Women (men too)
|
| |
| |
Cardiovascular Disease in Women
Are There Solutions?
Augustus O. Grant, MD, PhD; Alice K. Jacobs, MD; Carolyn Clancy, MD
From Duke University Medical Center (A.O.G.), Durham, NC; the Boston University Medical Center (A.K.J.), Boston, Mass; and the Agency for Healthcare Research and Quality, Department of Health and Human Services, Rockville, Md.
This issue of Circulation is devoted to an important problem facing us today. Despite American Heart Association (AHA) initiatives over more than a decade aimed at educating women about their risk of heart disease, the efforts of other organizations committed to women's health, and the recent "The Heart Truth" program of the National Heart, Lung and Blood Institute, in which the American Heart Association is an active partner, most women still do not internalize their risk from cardiovascular disease and thus do not act to reduce it. We report in this issue the third of a series of AHA surveys of women's awareness, performed every 3 years over the past 9 years. In fact, there has been an increase in the number of women who have heard that heart disease ranks as the No. 1 killer of women. However, the percentage that actually rank heart disease as their greatest personal health threat has only increased minimally from the 7% reported in the first survey, and remains far too low at 13%. Dr Wenger's Focused Perspective reminds us that cardiovascular disease affects not just older women but those in their 40s and 50s as well. Many cardiovascular problems, including atherosclerosis, begin in young adulthood, and prevention must begin at least between the ages of 20 and 30 to have its greatest impact. Furthermore, despite a recent focus on women's health in the research community, Dr Wenger points out that there are many as-yet unanswered questions that need to be addressed. Still, the critical issue of the moment is that we are not even using the information that is available, in part because women are unaware that they are at risk and in part because the information about women is not available in an easily accessible form for their physicians.
A recent article in The New England Journal of Medicine focuses on clinical research that is lost in translation.1 Findings from the National Healthcare Quality Report, recently published by the Department of Health and Human Services' Agency for Healthcare Research and Quality,2 also underscore the opportunities for clinical improvement with regard to cardiac disease. For example, only 69.6% of adult white women, 70.9% of black women, 59% of American Indian/Alaska Native women, and 60.9% of low-income women have had their cholesterol checked in the past 5 years. In addition, women with an acute myocardial infarction are less likely than men to receive aspirin within 24 hours of admission (82.6% versus 87.1%), have aspirin prescribed at discharge (84.2% versus 87.2%), and receive B-blockers at admission (67.34% versus 70.37%), though there are clearly opportunities for improvement for all.
To address this critical problem, the AHA has brought together experts from the relevant areas to develop Guidelines for the prevention of cardiovascular events in women. These Guidelines, presented in this issue, provide the best information available from the current medical literature for the care of healthy women, those at risk, and those who have already developed cardiovascular disease.
In addition, the AHA is launching our Go Red for Women campaign this month to help raise awareness among women that cardiovascular disease is their greatest health threat. The campaign has two important aspects. First, it is designed to create a rallying cry for increased awareness. You will see multiple national and community programs around the country over the next weeks, months, and years that will help this nation recognize the threat to its women. Second, Go Red for Women will help healthcare professionals provide the most up-to-date prevention and treatment for heart disease in women. Following the release of the AHA's new treatment and prevention Guidelines specific to women, the AHA will work to disseminate these Guidelines widely to healthcare providers and healthcare systems. Our ultimate goal is to reduce the risk of cardiovascular disease and stroke through improved quality of care as defined by these Guidelines. Ultimately, the goal of Go Red for Women is to encourage women and their healthcare providers to take control of women's heart health and to help them live longer, stronger lives. We invite your participation.
Heart Disease Prevention in Women
Cardiology Patient Page
(Circulation. 2004;109:e158-e160.)
2004 American Heart Association, Inc.
Lori Mosca, MD, PhD
From Columbia University College of Physicians and Surgeons, New York, NY.
A recent national study conducted by the American Heart Association showed that fewer than 50% of American women know that heart disease is their leading killer. The study included more than 1000 women from many different racial and ethnic backgrounds. More women in this study knew that heart disease was women's leading killer than in similar studies conducted in 1997 and 2000, but there's still a lot of room for improvement.
Cardiovascular disease- the No. 1 cause of death in the United States- claims the lives of almost 500 000 women each year. That's nearly one death every minute. Being aware of the risk of heart disease is important because it's the first step in taking action to lower risk.
Because heart disease can often be prevented, the survey findings are an urgent call to action. The American Heart Association and 11 other leading national health organizations came together to develop comprehensive guidelines for heart disease prevention in women. They include a rating scale to express the strength of recommendations and the quality of research to support specific preventive therapies.
Each recommendation was categorized to help doctors and women decide which preventive therapies should or should not be used. A Class I category indicates that the type of therapy should be provided routinely. Class IIa indicates that most scientific evidence favors providing the type of therapy, whereas Class IIb indicates the usefulness of therapy is less well-established. Class III indicates that the type of therapy isn't useful and may be harmful.
Being aware of personal risk and treatment options can empower a woman to live a long and healthy life. Physicians who follow these guidelines will be able to help female patients make lifestyle changes and better select the right medications to help them avoid or treat heart disease.
In developing these guidelines, a panel of renowned health professionals and scientists reviewed the highest-quality research from a search of nearly 7000 scientific articles that addressed important topics about preventing heart disease. The experts used the findings to develop clinical guidelines to help doctors provide the best possible preventive heart care for female patients. The guidelines were also designed to help women achieve a heart-healthy life and reduce their chances of having a heart attack or stroke. Awareness, knowledge, and action are by far the most important factors in saying "goodbye" (ALOHA) to the No. 1 killer of women.
ALOHA to Heart Disease
It's easy to remember what you need to know about the guidelines and setting priorities. Just think ALOHA:
A- Assess your risk and rank yourself as high, intermediate, or lower risk.
L- Lifestyle recommendations are priority No. 1 in heart disease prevention.
O- Other interventions are prioritized according to the expert panel rating scale.
H- Highest priority for therapy is for women at highest risk.
A- Avoid medical therapies called Class III.
A - Assess Your Risk
Heart disease risk isn't something you either have or don't have. It's a risk that people have to a greater or lesser degree. The first step in lowering your risk requires assessing- or measuring- your risk. You and your doctor can use a tool called the Framingham Risk Assessment Calculator to rank your personal heart disease risk as "high," "intermediate" or "lower."
Your risk score tells you your chances of having a heart attack or dying of heart disease over a 10-year period. You're given points on the basis of your age, total cholesterol level, HDL ("good") cholesterol level, blood pressure, and whether you smoke. The points are added up and converted into a 10-year risk. Your risk can be interpreted as the number of chances out of 100 that you'll develop or die from heart disease in the next 10 years, according to your current risk profile. Assessing, knowing, and acting are the best ways to change your risk profile.
If you already have heart disease, stroke, peripheral arterial disease, abdominal aortic aneurysm, diabetes mellitus, or chronic kidney disease, you're automatically considered to be at high risk. Also, some women with genetic cholesterol problems may also be at high risk.
You can use the Framingham Risk Assessment Calculator shown here to score your own risk. Share the results with your physician and discuss next steps.
L - Lifestyle Change: First Line of Defense Against Heart Disease
No matter what your risk score is, the most important thing you can do to lower your risk of heart disease is to make living a healthy lifestyle your top priority.
The following five lifestyle changes were rated as Class I. That means they're the strongest recommendations given by the expert panel.
1. Stop smoking cigarettes and avoid secondhand tobacco smoke.
2. Get at least 30 minutes of physical activity each day.
3. Start a cardiac rehabilitation program if you've recently been hospitalized or had a procedure for heart disease.
4. Eat a heart-healthy diet that includes fruits, vegetables, grains, low-fat or nonfat dairy products, fish, legumes, and sources of protein low in saturated fat (such as, poultry, lean meats, and plant sources). Limit intake of trans fatty acids such as those found in hydrogenated oils.
5. To maintain a healthy weight, balance the calories you eat with the amount you use up each day. To lose weight, you need to use up more calories than you take in. If you need to, enroll in a formal weight-loss program.
O - Other Interventions Prioritized by the Evidence Rating Scale
The expert panel rated other interventions as Class I. They should definitely be provided as a standard of medical care. These interventions include lowering high blood pressure in all women with hypertension, ensuring healthy cholesterol levels in high- and intermediate-risk women, and keeping diabetes under control. You'll need to work with your doctor to manage these risk factors.
1. Blood pressure is optimal at less than 120/80 mm Hg. If there's a slight rise in pressure, the first line of self-defense is to improve your lifestyle habits. If your blood pressure stays at 140/90 or higher (or greater than 130/80 if you have diabetes), drugs should be added to control it.
2. Cholesterol levels are important for women to know. Total cholesterol optimally should be less than 200 mg/dL; LDL (bad cholesterol), less than 100 mg/dL; HDL (good cholesterol), more than 50 mg/dL; and triglycerides (a type of fat in the blood), less than 150 mg/dL.
3. Diabetes (high blood sugar) is becoming more common in the United States. Unhealthy eating habits and gaining too much weight are leading causes of type II (acquired) diabetes. If you don't manage diabetes, it can lead to heart attack and stroke. Diet, exercise, and medication are the keys to normal blood glucose levels. Long-term control of glucose is measured with an HbA1C level; the panel recommends that it be maintained at less than 7%.
Other priorities for heart disease prevention are listed according to risk level in the Table.
Priorities for Prevention in Practice According to Risk Assessment
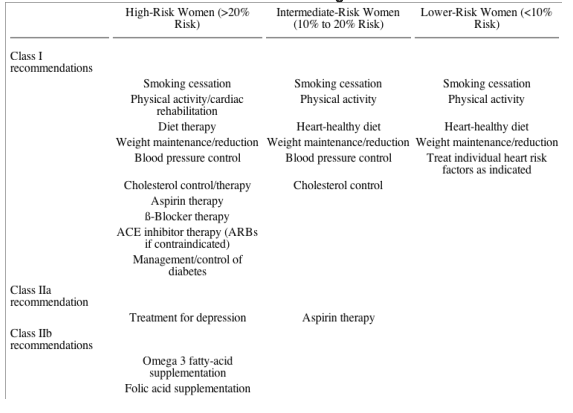
H - Highest Priority for Therapy Is for Women at Highest Risk
Women who are considered to be at highest risk are most likely to benefit from preventive therapy. Women at highest risk are those who already have cardiovascular disease, diabetes, or chronic kidney disease. Besides lifestyle changes and controlling major risk factors, several drugs have been shown to prevent heart attacks or increase survival in this group. The expert panel gave the medications listed below a Class I rating (desirable therapies) for women at high risk.
* ACE (angiotensin-converting enzyme) inhibitor therapy. If a woman on ACE therapy has side effects such as coughing, it's recommended that an ARB (angiotensin receptor blocker) be used instead, if she has a history of heart failure.
* Aspirin therapy (baby aspirin or a maximum dose of 162 mg). Women who have liver or kidney disease, stomach ulcers and other gastrointestinal problems, bleeding problems, or aspirin allergies should not take aspirin regularly.
* Beta-blocker therapy. Beta-blockers are recommended for women who have had a heart attack or have ongoing angina or chest pain.
* Statin therapy. Statins effectively reduce total cholesterol and LDL (bad cholesterol). Recent studies have shown statins are helpful even when the LDL is below 100, so the panel recommended that high-risk women take them if possible.
* Niacin or fibrate therapy. The panel recommended that high-risk women with a low HDL (good cholesterol) or high non-HDL (all the bad cholesterol and fats together) use niacin or fibrate therapy. Niacin therapy lowers total cholesterol and raises HDL (good cholesterol). Prescription niacin can be used alone or together with statin therapy. Dietary supplement niacin must not be used as a substitute for prescription niacin. Over-the-counter niacin should only be used if approved and monitored by a physician.
* Fibrates. Fibrates are effective in lowering triglycerides and, to some extent, can help improve HDL (good cholesterol levels). Fibrates are generally well tolerated by most women.
* Warfarin. Women with atrial fibrillation- a type of irregular heartbeat that can lead to stroke- should take the blood thinner warfarin unless they can't or are considered to be at low risk for a stroke. In that case, they should take 325 mg of aspirin daily.
A - Avoid Medical Interventions Called "Class III"
The panel said that three interventions should not be used to prevent heart disease because research has shown no benefit- and in some cases found harm. Ongoing research will provide more information about these therapies, but in the meantime, avoid their use to prevent heart disease.
* Combined postmenopausal hormone therapy (estrogen and progestin) has been recently shown (in the Women's Health Initiative) to have no benefit in preventing heart disease. In some women it may cause heart attacks, stroke, or blood clots. The benefits and risks of estrogen alone are still being studied. Talk to your doctor about the benefits and risks of hormone therapy to treat symptoms of menopause.
* Antioxidant supplements, such as vitamin E and beta carotene, should not be used to prevent heart disease. Several clinical trials have shown no benefit and some have shown an unexpected increase in hemorrhagic (bleeding) strokes. These supplements may also interfere with the beneficial effects of statin therapy.
* Aspirin for low-risk patients isn't recommended. The potential benefits may be outweighed by risks such as stomach bleeding or ulcers. Also, the benefit has not yet been proven in women who have a low risk of heart attack.
Conclusions
Overwhelming evidence suggests that heart disease can be prevented in both women and men. The new guidelines, if they are used, can help women lower their risk of developing heart disease. Every woman should know what her risk level is and talk to her doctor about her prevention goals and the best way to reach them. It's important to remember that the expert panel's recommendations are a guide. The best advice will come from your own healthcare provider(s). By following these guidelines, you and other women can help say "Aloha" (goodbye) to heart disease.
For more information, visit the American Heart Association web site: http://www.americanheart.org.
Editorials
Summary of the American Heart Association's Evidence-Based Guidelines for Cardiovascular Disease Prevention in Women
Lori Mosca for the Expert Panel/WritingGroup
From the Preventive Cardiology Program, New York-Presbyterian Hospital/Columbia University Medical Center and Weill Cornell Medical College, New York, NY.
Cardiovascular disease (CVD) is the largest killer of women in the United States. 1 More than 500 000 women die of CVD annually, more than the number of CVD-related deaths in men or related to the next 7 causes of death in women combined.1 Despite these statistics, a national survey in 2003 by the American Heart Association (AHA) showed that less than half of all women know that CVD is their leading cause of death.2 In an effort to raise awareness and educate health care providers and the public about methods to prevent incident and recurrent CVD events, an expert panel was convened to establish evidence-based guidelines for the prevention of CVD in women. The panel consisted of representatives from 11 AHA Scientific Councils and 11 federal and other professional organizations. There were an additional 22 endorsers. Details of the process and the complete guidelines have been published.3
Briefly, candidate recommendations for CVD risk-reducing interventions were discussed, prioritized, and then selected for a systematic literature search. Randomized, clinical trials and large, prospective, cohort studies evaluating cardiovascular risk-reducing interventions with a focus on major clinical endpoints (death, myocardial infarction [MI], stroke, revascularization procedure, congestive heart failure, or a composite CVD endpoint), whether or not there were female participants, were included. Nearly 7000 abstracts were identified in the initial search; 1279 were included for full-text screening and 399 studies were included in the summary evidence tables for each recommendation, with sex-specific information if available. The evidence tables are published online at http://atvb.ahajournals.org. The expert panel used an evidence rating system based on methods used in previous AHA/American College of Cardiology (ACC) guidelines and is outlined in Table 1.4 In addition, a generalizability index was used to rate the likelihood that results generated from studies conducted in men would be applicable to women.
TABLE 1. Recommendation Classifications and Levels of Evidence
Classification
Class I: Intervention is useful and effective
Class IIa: Weight of evidence/opinion is in favor of usefulness/efficacy
Class IIb: Usefulness/efficacy less well-established by evidence/opinion
Class III: Intervention is not useful/effective and may be harmful Level of
Evidence
A: Sufficient evidence from multiple randomized trials
B: Limited evidence from single, randomized trial or other nonrandomized studies
C: Based on expert opinion, case studies, or standard of care
Risk Assessment and Stratification
The Expert Panel recommended stratifying women into 3 risk groups (high, intermediate, and lower risk) based on the absolute 10-year probability of a coronary event (using the Framingham Risk Score for women) and based on clinical diagnoses. Women at high risk have a calculated 10-year CHD risk >20% and/or established CHD, other vascular disease, diabetes, or chronic kidney disease. Women at intermediate risk have a 10-year risk of 10% to 20% and may have subclinical CVD (ie, coronary calcification), metabolic syndrome, multiple risk factors, markedly elevated levels of 1 risk factor or a first-degree relative with early CVD. Women at lower risk have a 10-year risk <10% and may have metabolic syndrome or variable numbers of risk factors. Additionally, an optimal risk group was defined as women who have desirable levels of risk factors and who have a heart-healthy lifestyle.
Clinical Recommendations
Clinical recommendations are grouped by lifestyle interventions, major risk factor interventions, preventive drug interventions, atrial fibrillation/stroke prevention, and a class III category, which outlines interventions that are not recommended for CVD prevention in women. Clinical recommendations are prioritized based on strength of the recommendation and the level of evidence. A summary of priorities for CVD prevention in women based on risk classification is presented in Table 2. The complete list of recommendations is available online at http://atvb.ahajournals.org.
TABLE 2. Priorities for Prevention in Practice Based on Risk Classification
Women at High Risk (>20% Risk)
Class I Recommendations
Smoking cessation/environmental smoke avoidance
Physical activity/cardiac rehabilitation
Diet therapy
Weight maintenance/reduction
Blood pressure control
Lipid control with LDL-C-lowering agents, niacin, fibrates
Statin therapy in women with LDL-C <100 mg/dL
Aspirin therapy (75-162 mg)
Beta-blocker therapy unless contraindicated
ACE inhibitor therapy (ARBs if contraindicated)
Glycemic control in diabetics
Class IIa Recommendation:
Evaluation/referral for depression
Class IIb Recommendations:
Omega 3 fatty-acid supplementation
Folic acid supplementation
Women at Intermediate Risk (10%-20% Risk)
Class I Recommendations:
Smoking cessation/environmental smoke avoidance
Physical activity
Heart-healthy diet or lipid-lowering diet
Weight maintenance/reduction
Blood pressure control
Lipid control
Class IIa Recommendation:
Aspirin therapy (75-162 mg)
Women at Lower Risk (<10% Risk)
Class I Recommendations
Smoking cessation/environmental smoke avoidance
Physical activity
Heart-healthy diet or lipid-lowering diet
Weight maintenance/reduction
Treat individual CVD risk factors as indicated
Stroke Prevention Among Women With Atrial Fibrillation
Class I Recommendations:
High-intermediate risk of stroke
Warfarin therapy
Low risk of stroke (<1%/year) or contraindication to warfarin
Aspirin 325 mg therapy
Class III (Not Recommended for CVD Prevention):
Hormone therapy in postmenopausal women
Antioxidant supplements
Aspirin therapy in low risk women
Lifestyle Interventions
All women should be encouraged not to smoke and to avoid environmental smoke, and to get at least 30 minutes of moderate exercise (ie, brisk walking) on most and preferably all days or, in women with a recent coronary event, to participate in a rehabilitation program. A heart-healthy diet is recommended; for women without hyperlipidemia, that incorporates a variety of fruits, vegetables, grains, low-fat or non-fat dairy products, fish, legumes, and sources of protein that are low in saturated fat (limit saturated fat to <10% of calories and cholesterol to <300 mg/d). In addition, for women who also need lipid-lowering, saturated fat should be limited to <7% of calories, and cholesterol should be limited to <200 mg/d. Weight control should be encouraged to achieve a body mass index (BMI) between 18.5 and 24.9 kg/m2 and a waist circumference <35 inches.
These lifestyle interventions received class I recommendations (useful and effective), although supporting evidence was classified as B (limited to single randomized trial and/or several non-randomized studies). This reflects the strength of the observational data and ethical issues that prevent controlled trials of certain interventions (ie, smoking cessation). Furthermore, a "heart-healthy lifestyle" can prevent the development of major risk factors for CVD. Other lifestyle interventions that may be considered in women at high risk include the use of omega-3 fatty acids and folic acid (both class IIb, level B), as well as referral/treatment for depression (class IIa, level B). Regardless of risk group, lifestyle interventions are a top priority for CVD prevention in women.
Major Risk Factor Interventions
Major risk factor interventions target hypertension, dyslipidemia, and diabetes. Previously published guidelines, including the National Cholesterol Education Program- Adult Treatment Panel III,5 the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure,6 and the American Diabetes Association,7 can be referred to for specific management strategies. In addition, previous AHA prevention guidelines8-10 were used as a resource to develop and update sex-specific recommendations for women.
Clinical recommendations include maintenance of an optimal blood pressure <120/80 mm Hg through lifestyle approaches, including the dietary approaches to stop hypertension (DASH) eating plan (class I, level B).6 Pharmacotherapy is indicated at levels >=140/90 mm Hg or even lower in the setting of blood pressure-related target organ damage or diabetes. Thiazide diuretics are recommended as part of the antihypertensive regimen, unless contraindicated (class I, level A).
Optimal levels of lipids and lipoproteins for women were defined as low-density lipoprotein cholesterol (LDL-C) <100 mg/dL, triglycerides <150 mg/dL, non-high-density lipoprotein cholesterol (HDL-C) <130 mg/dL, and HDL-C >50 mg/dL. For women at high risk, LDL-C-lowering therapy (statins preferred) was recommended to be initiated in conjunction with lifestyle therapy if LDL-C >=100 mg/dL (class I, level A). Statin therapy was also recommended in high-risk women with LDL-C <100 mg/dL unless contraindicated (class I, level B). Niacin or a fibrate was recommended for treatment of low HDL-C or elevated non-HDL-C (class I, level B) among high-risk women. For women at intermediate risk, LDL-C-lowering with statins was recommended if levels were >=130 mg/dL with lifestyle therapy (class I, level A). For women at lower risk, LDL-C-lowering was recommended if levels were >=190 mg/dL or >=160 mg/dL in the presence of multiple risk factors (class IIa, level B). Niacin or a fibrate was recommended for treatment of low HDL-C or elevated non-HDL-C once the LDL-C goal was reached for both intermediate-risk (class I, level B) and lower-risk (class IIa, level B) groups. Among diabetic women, diet and pharmacotherapy were recommended to achieve an HbA1C <7% (class I, level B).
Preventive Drug Interventions
Several pharmacologic interventions were recommended for women at high cardiovascular risk. ACE inhibitors are indicated in all high-risk women (class I, level A); if contraindicated, then angiotensin receptor blockers (ARBs) should be used in those with clinical evidence of heart failure or a left ventricular ejection faction <40% (class I, level B). Beta-blockers are recommended in all women after MI or with chronic ischemic syndromes (class I, level A). Aspirin (75 to 162 mg/d), or clopidogrel for intolerance, is a class I, level A recommendation for high-risk women unless contraindicated. Aspirin is a class IIa, level B recommendation in those at intermediate risk if blood pressure is controlled and the benefits outweigh the risks of adverse gastrointestinal effects. In women with atrial fibrillation, warfarin is recommended (class I, level A) unless the patient has a contraindication or the risk for stroke is low (<1%/year), in which cases aspirin (325 mg/d) is recommended (class I, level A).
Class III Recommendations
A unique aspect of these guidelines is the designation of class III interventions that should not be used for CVD prevention. Aspirin in lower-risk women, hormone therapy in postmenopausal women, and antioxidant vitamin supplements in all women were rated as class III, because of the unproven benefits and possible harm associated with their use, pending results of ongoing and future trials.
Conclusions
The expert panel concluded that high-quality observational and clinical trial evidence supports the use of risk-modifying interventions that may have a substantial impact on reducing CVD in women if more uniformly implemented. As part of the AHA "Go Red for Women" national campaign to raise awareness about CVD in women, these guidelines will be disseminated to health care providers as well as other partners and will be incorporated into continuing medical education programs. Because a recent national survey documented that less than half of all women recognize that CVD is their leading killer, these guidelines can be used as an educational tool to help women understand their risk and take appropriate action.2 The report highlighted the persistent gap in knowledge related to racial/ethnic minorities and elderly women. The panel also emphasized that the guidelines are never a substitute for good clinical practice.
Acknowledgments
Members of the writing group included: Lawrence J. Appel, MD; Emelia J. Benjamin, MD; Kathy Berra, MSN, ANP; Nisha Chandra-Strobos, MD; Rosalind P. Fabumni, PhD; Deborah Grady, MD, MPH; Constance K. Haan, MD; Sharonne N. Hayes, MD; Debra R. Judelson, MD; Nora L. Keenan, PhD, Patrick McBride, MD, MPH; Suzanne Oparil, MD; Pamela Ouyang, MD; Mehmet C. Oz, MD; Michael E. Mendelsohn, MD; Richard C. Pasternak, MD; Vivian W. Pinn, MD; Rose Marie Robertson, MD; Karin Schenck-Gustafsson, MD, PhD; Cathy A. Sila, MD; Sidney C. Smith, Jr, MD; George Sopko, MD, MPH; Anne L. Taylor, MD; Brian W. Walsh, MD; Nanette K. Wenger, MD; Christine L. Williams, MD, MPH
The Duke Center for Clinical Health Policy Research, Durham, NC conducted the literature searches with support from the Foundation for the Advancement of Cardiac Therapies (FACT) Foundation, Palm Beach, Fla.
|
|
| |
| |
|
|
|