| |
Hysterectomy Among Women With HIV: Indications and Incidence
|
| |
| |
[Brief Report: Clinical Science]
JAIDS Journal of Acquired Immune Deficiency Syndromes:Volume 44(5)15 April 2007pp 566-568
Massad, L Stewart MD*; Evans, Charlesnika MPH; Weber, Kathleen BSN; Cejtin, Helen E MD; Golub, Elizabeth T PhD; DiGilio, Kathy RN; Alpern, Amy CNM#; Watts, D Heather MD
Data in this manuscript were collected by the WIHS Collaborative Study Group, with centers (Principal Investigators) at the New York City/Bronx Consortium (Kathryn Anastos); in Brooklyn, NY (Howard Minkoff); at the Washington, DC Metropolitan Consortium (Mary Young); at the Connie Wofsy Study Consortium of Northern California (Ruth Greenblatt); at the Los Angeles County/Southern California Consortium (Alexandra Levine); at the Chicago Consortium (Mardge Cohen); and at the Data Coordinating Center (Stephen Gange).
Abstract
Objective: To describe hysterectomy rates and indications among women with HIV and to compare them with at-risk HIV-seronegative women.
Methods: Reports of hysterectomy were collected from 3752 participants in a prospective cohort study of women with HIV and comparison uninfected women. Available operative notes were retrieved and abstracted. Comparisons were made using the Fisher exact, χ2, Wilcoxon 2-sample, and Student's t tests.
Results:
Incident hysterectomy was performed for 106 (4.5%) of 2361 HIV-seropositive women, most often for cervical neoplasia, and for 24 (2.9%) of 837 HIV-seronegative women (P = 0.04).
The incidence of hysterectomy was 7.7 per 1000 person-years for HIV-seropositive women and 5.3 per 1000 person-years for HIV-seronegative women (P = 0.09). HIV-seropositive and HIV-seronegative women undergoing incident hysterectomy were similar, except for a higher likelihood of an abnormal preoperative Papanicolaou test result in the former (P = 0.001). Surgical indications did not differ by serostatus.
Conclusion: Women with HIV are more likely than uninfected women to require a hysterectomy, most often for cervical neoplasia.
Hysterectomy is the second most common major surgical procedure among US women after cesarean section.1,2 More than 600,000 hysterectomies are performed each year, with an annual rate of 5.5 per 1000 women. An estimated 123,405 women in the United States were living with HIV in 2004,3 but the frequency of hysterectomy among these women is unclear. Paramsothy and colleagues4 reported in a study of participants in the HIV Epidemiology Research Study (HERS) that hysterectomy was substantially more common in HIV-infected women than in uninfected women, and they found that 73% of hysterectomies in women with HIV enrolled in the HERS were performed in the presence of cervical neoplasia. Data from the National Hospital Discharge Survey (NHDS) also showed that cervical neoplasia was a more common indication for hysterectomy among HIV-seropositive than HIV-seronegative women.5 We reviewed results of the Women's Interagency HIV Study (WIHS) to refine our understanding of the incidence of and indications for hysterectomy among women with HIV.
METHODS
This investigation was part of the WIHS, a multicenter prospective cohort study of the natural history of HIV infection and related health conditions among HIV-seropositive women and at-risk HIV-seronegative comparison women. The protocols, procedures, and baseline results of the WIHS have been previously described; WIHS participants are representative of US women with HIV.6 Briefly, the WIHS enrolled 2059 HIV-seropositive and 569 at-risk HIV-seronegative women in 1994 through 1995 at 6 study consortia incorporating 21 sites. Additional enrollment of 406 at-risk HIV-seronegative and 739 HIV-seropositive women without a prior AIDS diagnosis was conducted in 2001 through 2002. Written informed consent was obtained after approval by local human subjects committees. This analysis included all information obtained between October 1, 1994 and October 1, 2004 at 6 sites.
At each visit, women were asked about interval hysterectomy, and absence of a uterus was confirmed by examination. Medical records abstraction was attempted for each woman reporting incident hysterectomy, although retrieval of records regarding hysterectomy before enrollment was not attempted. When available, operative notes were reviewed, and indications and estimated blood loss were tabulated, but detailed chart review was not feasible. Quality of life was scored using an instrument previously validated in women with HIV.7 Fisher exact and χ2 tests were used to evaluate associations between categoric variables. Wilcoxon 2-sample and Student's t tests were used to assess associations between means and medians.
RESULTS
Of 3752 women in the WIHS, 254 had undergone a hysterectomy before their baseline visit: 211 (7.6%) of 2793 HIV-seropositive women and 43 (4.5%) of 959 HIV-seronegative women (P = 0.0007). An additional 300 women (221 HIV-seropositive and 79 HIV-seronegative) had no follow-up. This left 3198 women for analysis. Incident hysterectomy was performed in 106 (4.5%) of 2361 HIV-seropositive women and 24 (2.9%) of 837 HIV-seronegative women (P = 0.04). The cumulative risk of hysterectomy was 11.4% for HIV-seropositive women and 7.0% for HIV-seronegative women (P = 0.0001).
HIV-seropositive women were followed for 13,679 person-years (median = 5.4 years), and HIV-seronegative women were followed for 4504 person-years (median = 3.1 years). The incidence of hysterectomy was 7.7 per 1000 person-years for HIV-seropositive women and 5.3 per 1000 person-years for HIV-seronegative women (P = 0.09). There were also no differences in hysterectomy rates when women were compared by HIV serostatus using the Kaplan-Meier method.
We found no differences in ethnicity, parity, uterine size, menopausal status, amenorrhea, history of pelvic inflammatory disease, or presence of a pelvic mass among women undergoing hysterectomy by HIV serostatus. The Papanicolaou test result before hysterectomy was abnormal in 53 (50.0%) HIV-seropositive and 3 (12.5%) HIV-seronegative women (P = 0.001). HIV-seropositive women were younger than HIV-seronegative women at the time of hysterectomy (median age = 40.8 years among HIV-seropositive women vs. 42.9 years among HIV-seronegative women; P = 0.05). No difference in quality of life was found after hysterectomy in HIV-seropositive or HIV-seronegative women.
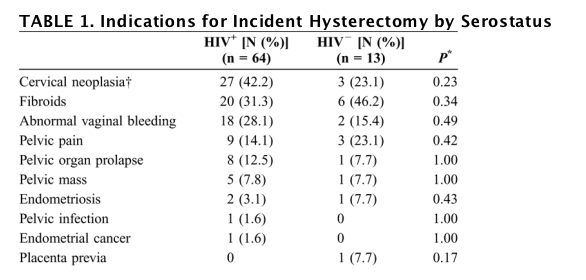
Table 1 presents the indications for hysterectomy among the 77 women for whom medical records could be abstracted. We did not find differences in hysterectomy rates by indication. HIV-seropositive women were less likely to have had a supracervical hysterectomy than HIV-seronegative women (4 [6%] cases in HIV-seropositive women vs. 4 [31%] cases in HIV-seronegative women; P = 0.04), but we did not find other differences in operative approach by serostatus. Notes defining estimated intraoperative blood loss could be retrieved for 54 (42%) women. HIV-seropositive women were less likely than HIV-seronegative women to have blood loss estimated at more than 250 mL (19 [44%] of 43 women vs. 9 [81%] of 11 women; P = 0.04).
DISCUSSION
Hysterectomy is the most common major surgical procedure among nonpregnant US women. Our results show that it is common among women with HIV, with an annual incidence of 7.7 per 1000 person-years. Although the higher annual incidence rates found in HIV-seropositive women were of borderline significance compared with the rates among HIV-seronegative women (P = 0.09), the difference did reach significance after including prevalent cases.
Cervical neoplasia is more common among women with HIV8 and was the leading indication for hysterectomy among women with HIV. The HERS found that 73% of women undergoing a hysterectomy have the procedure in the face of cervical disease,4 whereas (NHDS) data showed that cervical neoplasia was the indication for 44% of women with HIV, second only to menstrual dysfunction.5 All these findings are in contrast to our findings in HIV-seronegative women and to prior reports of hysterectomy indications in the general population, in whom fibroids, endometriosis, and prolapse predominate.1,2
Our study also was remarkable for its negative findings. Like Paramsothy and colleagues,4 we found that pelvic pain, pelvic inflammatory disease, and endometriosis were not more common indications for hysterectomy in HIV-seropositive compared with HIV-seronegative women. This suggests that immunodeficiency does not promote the development of severe forms of these disorders. Women with these conditions can be reassured that although they may require surgery, the presence of HIV infection does not seem to increase their need for hysterectomy dramatically.
Despite the large numbers of women enrolled in the WIHS, the number undergoing hysterectomy remains small enough that we may have lacked power to detect significantly increased rates of hysterectomy for abnormal bleeding and prolapse. In addition, we did not have access to full hospital charts and outpatient records for many women who received care outside WIHS home institutions, and we cannot determine whether women with HIV experience more serious perioperative complications after hysterectomy than HIV-seronegative women.
As the population of women with HIV ages, genital prolapse is likely to become more common, whereas hormone-dependent indications, such as uterine fibroids or endometriosis, and indications related to sexual activity, such as pelvic infection, are likely to decline. Continuing surveillance of hysterectomy trends is ongoing in the WIHS.
|
|
| |
| |
|
|
|