| |
Treatment for lipoatrophy: facing the real costs; should be reimbursed
EDITORIAL COMMENT
|
| |
| |
AIDS:Volume 21(13)20 August 2007p 1819-1820
Margolis, David M
From the University of North Carolina at Chapel Hill, Chapel Hill, North Carolina, USA.
Patients unlucky enough to suffer chronic illnesses such as HIV infection, leprosy, tuberculosis, or mental illness bear an additional burden: stigma. Indeed, the fear of being identified as HIV infected or receiving antiretroviral therapy may lead a significant number of patients to avoid appropriate medical care. Nowhere is this a more obvious problem than in individuals suffering HIV-associated facial lipoatrophy.
The causes of facial lipoatrophy and of HIV-associated metabolic abnormalities in general, are yet to be fully defined [1]. These conditions appear to be multifactorial, owing in some part to metabolic changes induced by HIV infection, but in large part to exposure to antiretrovirals. Specific nucleoside reverse transcriptase inhibitors play a prominent role, and studies have shown modest improvements in lipoatrophy following the use of alternative antiretroviral regimens [2,3]. Given the improved recognition of these disorders, and the appreciation of antiretroviral regimens that are less likely to result in lipoatrophy, one would hope to soon see a decline in the prevalence of this troubling disorder.
Despite the efforts of many, medical approaches to treat lipoatrophy once it is apparent have met with only modest success [4]. In some studies, but not all, thiazolidinediones have been shown to result in modest recovery in fat volume [5]. The use of human growth hormone can improve visceral adiposity, but may worsen facial or peripheral lipoatrophy [6].
Given the lack of effective medical therapy, patients have turned to surgical alternatives. Facial fillers are currently the only therapy that can result in prompt improvement of lipoatrophy. A wide variety of biodegradable implants using autologous fat transfer, collagen or cadaveric dermis implants, poly-L-lactic acid, hyaluronic acid, or calcium hydroxylapatite, have been used. Permanent materials such as silicone, expanded polytetrafluoroethylene, polymethyl-methacrylate implants or polyacrylamide and polyalkylimide gels. Few well performed, fully powered studies have been done; one comparative study has recently been reported [7].
In this issue Loutfy and co-workers in Toronto compare the effects observed in a group of patients with facial lipoatrophy treated immediately with polyalkylimide gel, an injectable product, or followed for 12 weeks prior to treatment [8]. Polyalkylimide gel is licensed in Canada and Europe, and has been used there to treat HIV-associated facial lipoatrophy. Loutfy and colleagues treated 31 patients, almost all male. Most of the patients had mild to moderately severe lipoatrophy, with few graded subjectively as having the most severe disfigurement. Both patients and physicians found that the immediately treated group improved significantly, graded with a subjective scale. Obviously, all the patients and probably most clinicians who were grading the response knew which patients had received injections at week 12. The improvement persisted to 48 weeks, however, and by 48 weeks the delayed treatment group had achieved equal, sustained improvement. In this study group of modest size, they note the absence of complications, particularly site reactions and nodules noted with other products; however, unsurprisingly, others have recently reported postoperative complications after the use of polyalkylimide gel [9].
As in few other studies of facial fillers, Loufty and coworkers studied the effect of their intervention on mental health and quality-of-life scores. While the immediately treated group had improvements in these scores compared to the untreated group at week 12, when re-evaluated at week 48 after both groups had been treated the picture changed somewhat. Although mental health and quality-of-life scores had improved somewhat from baseline to week 48 for both groups, the extent of these changes was less uniform. Only improvements in depression and anxiety scores achieved statistical significance.
The authors estimate that a course of therapy for an average patient, taking into account the need for repeat injections in some, might be between US$ 1750-4375 for a 10-15 ml course (US$ 175 per ml), whereas in Europe the cost varies in the range EU 200-425 per ml depending upon nation and treatment centre. They conclude that polyalkylimide gel might be a preferred intervention due to its permanence, extractability in cases of adverse outcome, and the ability to administer high volumes of product, and sadly, the authors must conclude that treatment with polyalkylimide gel may be restricted due to its cost.
While this might be the case in the current healthcare environment, perhaps we should ask the questions that take the next logical step. While facial lipoatrophy is not fatal, it is devastating for the lives of many. Do we know what its attendant costs really are? Can facial fillers obviate some of the need for antidepressants or counseling? Are they more cost-effective? In the developed world, a treatment course of polyalkylimide gel appears to be a fraction of the annual cost of antiretroviral therapy. What is the real cost of untreated facial lipoatrophy? Should not healthcare systems provide treatment for a condition that appears to be, for the lack of a kinder word, iatrogenic (�eused to describe a symptom or illness brought on unintentionally by something that a doctor does or says�f)?
AIDS:Volume 21(9)31 May 2007p 1147-1155
"Immediate versus delayed polyalkylimide gel injections to correct facial lipoatrophy in HIV-positive patients"
Loutfy, Mona Ra,b; Raboud, Janet Mb,c; Antoniou, Tonya,d; Kovacs, Colina,b; Shen, Sandyc; Halpenny, Robertaa; Ellenor, Darlenea; Ezekiel, Daviaa; Zhao, Alicea; Beninger, Francise
From the aMaple Leaf Medical Clinic, Canada
bDepartment of Medicine, University of Toronto
cDivision of Infectious Diseases, University Health Network, Canada
dDepartment of Family and Community Medicine, St Michael's Hospital, Canada
eDivision of Plastic Surgery, University of Toronto, Toronto, Ontario, Canada.
Abstract
Objective: To evaluate the safety and efficacy of polyalkylimide gel (PAIG) in the treatment of HIV-associated facial lipoatrophy.
Design: A randomized, open-label, single-centre study.
Methods: HIV-positive individuals with facial lipoatrophy (based on physician assessment) were randomly assigned to immediate (weeks 0 and 6) or delayed (weeks 12 and 18) PAIG injections administered into the subcutaneous plane. Outcome measures included a change in facial lipoatrophy severity scores (five-point scale), adverse events, photographic assessment, and changes in quality of life (QoL), depression and anxiety using validated surveys.
Results: Thirty-one patients (median age 48 years, 97% male) were enrolled and completed 48 weeks of follow-up. Overall, the median volume of product injected bilaterally was 16.0 ml. Adverse events, including swelling, redness, bruising and pain, were mild, and resolved after a median of 3 days. There were no cases of necrosis, nodules or infection. Compared with patients randomly assigned to delayed treatment, patients in the immediate therapy group had significantly lower physician-rated facial lipoatrophy scores (0 versus 2; P < 0.0001), improved QoL (P = 0.01), and lower anxiety (P = 0.02) at week 12. At week 48, median physician and patient facial lipoatrophy scores were 0 and 1, respectively, for the entire cohort, and were not significantly different between the groups. Significant improvements in patient anxiety (P = 0.001) and depression (P = 0.01) were observed from baseline to week 48.
Conclusion: Treatment with PAIG was effective and safe and led to improvements in facial lipoatrophy grading, QoL, anxiety and depression scores in HIV-infected patients with facial lipoatrophy.
Introduction
Facial lipoatrophy has emerged as perhaps the most distressing and devastating manifestation of the antiretroviral therapy (ART)-associated lipodystrophy syndrome for patients infected with HIV. The profound depletion in both superficial and buccal facial fat is highly stigmatizing for patients, resulting in feelings of low self-esteem, social withdrawal and forced disclosure of HIV status [1-3]. In addition, the appearance of facial lipoatrophy may adversely affect adherence to ART, and act as a deterrent to initiating therapy in patients for whom ART would otherwise be indicated [1,4]. Although some progress has been made in elucidating the aetiology of and risk factors for facial lipoatrophy [5], currently available medical treatments appear insufficient for managing this adverse effect. In particular, intervening with either recombinant human growth hormone or thiazolidinediones has yielded negligible, if any, effect on facial lipoatrophy [6-8]. Furthermore, although switching from a thymidine analogue to either an abacavir, tenofovir or nucleoside-sparing-based regimen has improved peripheral fat loss in randomized controlled trials evaluating this approach, this option is not always virologically feasible, and the clinical significance of the observed fat recovery is questionable [9,10]. Given the lack of improvement associated with pharmacological approaches, interest has increased in the surgical correction of lipoatrophy with facial fillers.
Poly-L-lactic acid (PLA; New-Fill, Biotech Industry SA, Luxembourg) is an aliphatic polyester that is the first filler to be approved by the United States Food and Drug Administration for the treatment of ART-associated facial lipoatrophy. Approval of PLA was based on data from four open-label studies documenting the safety and efficacy of this product in 278 patients with facial lipoatrophy [11-14]. Long-term follow-up of one cohort suggested that the benefits of PLA persist for up to 96 weeks [11]. Although it is the most extensively studied facial filler, PLA has several potential drawbacks. As a biodegradable product, the effect of PLA is temporary, and therefore re-treatment is eventually necessary. Multiple treatment sessions are required to administer PLA, necessitating repeat visits and injections for the patient. Furthermore, subcutaneous nodules have been reported after the injection of PLA [11-14]. Assessment of alternative options for patients with facial lipoatrophy is therefore important.
Polyalkylimide gel (PAIG; Bio-Alcamid, Polymekon, Biotech Industrie, Milan, Italy), a non-biodegradable, non-allergenic, non-toxic polymer composed of 96% non-pyrogenic water and 4% polyalkylimide, possesses several properties that make further study of this compound in HIV-positive patients worthwhile [15]. In particular, once implanted, PAIG is unique among injectable fillers in that a fine (0.02 mm) collagen capsule develops around the gel, isolating it from host tissue [16]. As a result of the encapsulation process, the implant can be readily identified and, should the need arise, easily removed by expressing the capsule and squeezing the material out. Also, the cosmetic effects of PAIG are permanent, obviating the need for further treatments [15]. The benefits and safety of PAIG have been reported in a multicentre study of 2000 otherwise healthy patients, who attained excellent cosmetic results, with no evidence of implant migration, dislocation, granuloma or allergic responses noted. Although 12 patients developed postoperative staphylococcal infections, these could be attributed to the implanted material in only three cases [15]. These findings have been replicated by several published case series of HIV-positive patients with facial lipoatrophy, in whom restorative treatment with PAIG was assessed as being safe and effective [16,17]. Randomized trials of PAIG incorporating measures of patient quality of life (QoL) have yet to be performed.
The objectives of this study were to evaluate the efficacy, safety and impact on QoL of PAIG given in a single session, with an additional follow-up session as needed if the level of correction was deemed less than optimal by the treating surgeon (i.e. a 'touch up' session).
Materials and methods
The study was an open-label, randomized, 24-week study of immediate versus delayed treatment with PAIG injections in HIV-infected patients with facial lipoatrophy. The study design was modelled after a previous trial of immediate versus delayed injections of PLA, with the intention of assessing the temporal association between treatment and improvements in both facial lipoatrophy score and patient QoL [12].
Study participants
HIV-positive individuals, 18 years of age or older who self-identified as having facial lipoatrophy with confirmation by their primary care physician were eligible for the study. The severity of facial lipoatrophy was determined using the validated Carruther's scale of facial lipoatrophy which goes from grade 1 (mild lipoatrophy) to grade 4 (most severe lipoatrophy) (Fig. 1) [18]. Exclusion criteria included pregnancy or intent for pregnancy, injectable therapy for facial lipoatrophy within the past 9 months, the presence of an inflammatory condition of the face and the use of anticoagulation or non-steroidal inflammatory agents in the 7 days before injection. The study protocol was approved by our Research Ethics Board and all patients provided written informed consent. Consent for the publication of photographs was also obtained.
Study injection technique
Patients received PAIG injections at their first treatment visit by a single trained plastic surgeon into the subcutaneous plane, avoiding the muscle or dermal planes (Fig. 2). At this initial visit, patients received deposits of PAIG in several injections because this product works on the principle of applying a minimum of 0.3 ml, or preferably, 0.5 ml per aliquot, which encourages the encapsulation process. Smaller aliquots do not encapsulate and are absorbed by the body. A 16 gauge, 11/2 inch needle was used for the baseline large aliquot injection. A 20 gauge, 11/2 inch needle was used when PAIG was transferred from a 5 ml syringe to a 1 ml syringe. Care was taken to ensure not to go medial to the midpupilar line as this might broaden the aspect of the nose and not to go above the midline of the zygomatic bone because this may deepen the orbital rim. When filling the cheeks, a minimum amount of PAIG was always applied over the zygomatic bone to blend in with the existing structures. To minimize pain, 1-2% lidocaine with or without epinephrine was injected locally before the procedure. Patients were given a 5-day course of antibiotic prophylaxis with oral cephalexin 500 mg four times per day, to be started one day before the treatment. Levofloxacin 500 mg a day was used in cases of penicillin allergy. The quantity of PAIG injected varied with the severity of skin depression. At the end of the initial injection, the cheeks were thoroughly and aggressively massaged to smoothen out all the aliquots of PAIG, including intra-oral massage techniques. A second session was organized 6 weeks after the initial injection if the surgeon judged the level of correction to be less than optimal and not fully corrected. In that case, the surgeon would provide a 'touch up', defined as the necessary volume of PAIG needed to optimize the aesthetic result. A 20 gauge, 11/2 inch needle was used for the small aliquot touch ups. Additional touch-up injections could be arranged as required to optimize treatment outcome at the discretion of the plastic surgeon. Treatment was discontinued if any severe or moderate reaction developed after injection.
Study design and follow-up
Study participants were randomly assigned to immediate treatment with injections of PAIG to the buccal area, and in some cases, the temple region, on day 0 with a touch up at week 6, or to delayed treatment with the injections being done at week 12 with a touch up session at week 18. Randomization was performed by the sequential opening of sealed opaque envelopes containing treatment assignments as determined with a random number generator. At the baseline visit, patients were evaluated by clinical examination, fasting blood work (complete blood count, biochemistry, liver function, lipids, glucose, lactate, viral load and CD4 cell count), standardized facial photography and QoL, anxiety and depression questionnaires. Clinical examination, facial photography and the administration of all questionnaires were repeated at weeks 2, 6, 12 and 24 of follow-up. Additional visits are planned for weeks 48, 72 and 96. The clinical examination and scoring were performed by two HIV specialists and the injecting plastic surgeon at each facial lipoatrophy grading visit using the Facial Lipoatrophy Severity Scale (FLSS) (Fig. 1). Each patient was scored by the three reviewers, the average of which was used to derive the score for the analysis. Adverse events and safety reporting were performed at each of the visits.
Study endpoints
The primary endpoint of the study was the change from baseline to week 12 in the facial lipoatrophy severity score as assessed by the three physicians using the FLSS. The FLSS is a validated four-point grading of facial lipoatrophy from 1 (mild facial lipoatrophy) to 4 (severe facial lipoatrophy) developed by Dr Carruther (Fig. 1). Grade 0 was used to represent the condition of no facial lipoatrophy. The secondary endpoints include the change in facial lipoatrophy grading score as determined by the patient using the FLSS, the nature and incidence of adverse events, and the change in QoL and depression scores from baseline to weeks 12 and 48. QoL and depression were assessed using the Medical Outcomes Study HIV Health Survey (MOS-HIV), the Hospital Anxiety and Depression Scale (HADS) and the slightly modified Dermatology Quality of Life Survey (sDQLS). The MOS-HIV is the standard validated survey used to assess QoL in HIV-positive patients, and includes functional, mental health and QoL subscales [19]. The subscales are scored out of 600, 700 and 100, respectively, with a higher number indicating better health. The HADS is a validated survey assessing both depression and anxiety that has been used in the setting of facial lipoatrophy treatment [20]. Each subscale is measured out of 21, with higher numbers representing greater degrees of depression and anxiety. The sDQLS is a survey that has been validated using the word 'skin' and measures the impact of skin diseases on QoL [21]. For this study, the survey was slightly modified by changing the word 'skin' to 'facial lipoatrophy'. The sDQLS is scored out of 30, and the literature has identified that the higher the score, the more a given individual's impaired QoL is caused by appearance.
Statistical analysis
The primary analysis was a comparison of the difference in the change from baseline to week 12 in the FLSS score, as graded by the three physicians between the immediate and delayed groups using a Wilcoxon rank sum test. Wilcoxon rank sum tests were also used to compare the change in secondary outcomes from baseline to week 12 and primary and secondary outcomes between the treatment groups at week 48. The proportion of patients experiencing each adverse event was tabulated by treatment group. Pain was assessed by duration, peak severity on a scale of 0-10, and current severity out of 10. Medians and interquartile ranges (IQR) were used to summarize peak and current severity. Wilcoxon signed rank tests were used to compare the patient FLSS score and survey score between baseline and week 48 for the entire study group.
The interrater agreement was assessed using the AC1 statistic (K. Gwet, 2002, unpublished observation) instead of the more widely used kappa. Kappa is low when the outcome of many subjects falls into one category. In this study, many subjects had an FLSS score of zero at the last visit. As kappa measures the agreement over and above the 'agreement by chance', it indicates a low level of agreement when the agreement-by-chance is high. The AC1 statistic is similar in nature to kappa, but accounts for the large proportion of outcomes in one group; therefore it is a more robust chance-corrected statistic.
Results
Thirty-one patients were enrolled between April and July 2005. The baseline characteristics of the cohort are summarized in Table 1 by treatment group. Twenty-three patients (74%) had moderate to severe facial lipoatrophy at baseline with a median physician FLSS of 2 (IQR 1, 3). In addition to facial lipoatrophy, 27 patients (90%) complained of evidence of fat loss elsewhere in the body. All 31 patients received PAIG injections, with 16 randomly assigned to the immediate group and 15 to the delayed group. Week 12 data are available for 30 patients, as one participant in the immediate group missed the week 12 visit. Similarly, week 48 data are available for 30 patients as one patient was lost to follow-up subsequent to the week 12 visit. The two groups were similar with respect to baseline patient and physician-graded FLSS score as well as QoL indices. The median volume of PAIG injected in the immediate and delayed group was 16.6 ml (IQR 14.8, 22.3) and 13.5 ml (IQR 10.5, 18.0), respectively (P = 0.18). Overall, the median total volume of PAIG injected by week 48 was 16.0 ml (IQR 12, 20), with the median volume for each grade and arm presented in Table 2. The majority of patients (58%) required either one injection of PAIG (n = 5; two in the immediate group, three in the delayed group) or one injection with one touch-up session 6 weeks later (n = 13; five in the immediate group, eight in the delayed group). Eight patients (six in the immediate group, two in the delayed group) required three injections (baseline with two touch-up injections), four patients (two in the immediate group, two in the delayed group) received four injections, whereas the remaining patient (immediate group) received five injections. The number of patients requiring touch-up injections of PAIG was not significantly different between the two groups (P = 0.15).
The median change in the physician FLSS score from baseline to week 12 was -2 (IQR -3, -2) for the immediate group and 0 (IQR 0, 0) for the delayed group (P < 0.0001; Table 3). The interreviewer agreement for the three physicians was 0.79 [95% confidence interval (CI) 0.64-0.94] at baseline and 0.75 (95% CI 0.61-0.89) at 12 weeks' follow-up. The median change in the patient FLSS score from baseline to week 12 was -2 (IQR -2, -1) for the immediate group and 0 (IQR 0, 0) for the delayed group (P = 0.002; Table 3). The interperson agreement between patient's self grade and the median physician score was 0.44 (95% CI 0.20-0.68) at baseline and 0.47 (95% CI 0.24-0.70) at 12 weeks' of follow-up. High resolution digital photographs were taken at baseline and at each follow-up visit, and a representative selection are presented in Fig. 3. The median change in MOS-HIV, HADS and sDQLS scores by week 12 is presented in Table 3 by treatment group. All three subscales of the MOS-HIV were improved for the immediate group compared with the delayed group, although the QoL (P = 0.01) and psychological subscales (P = 0.02) were more significantly affected than the physical subscale. Statistically significant improvements in the anxiety portion of the HADS and the sDQLS were seen in the immediate groups compared with the delayed group at week 12 (P = 0.02 and P = 0.001, respectively).
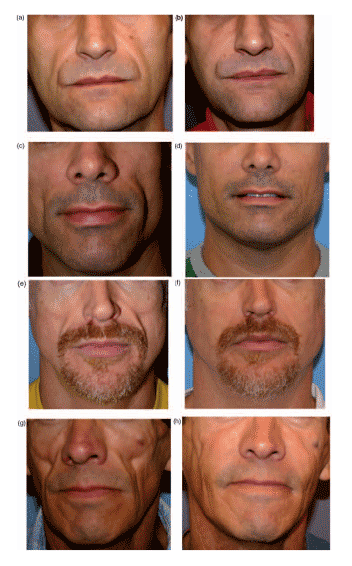
Fig. 3. Pictures before and after injection of polyalkylimide gel. (a) before and (b) after grade 1 FLA; (c) before and (d) after grade 2 FLA; (e) before and (f) after grade 3 FLA; (g) before and (h) after grade 4 FLA. FLA, facial lipoatrophy.
Adverse events were mostly mild and transient, resolving after a median of 3 days (IQR 2, 5). Swelling, pain, bruising and erythema were the most common adverse effects, occurring in 24 (77%), 21 (68%), 18 (58%) and 13 (42%) patients, respectively. The median duration of swelling, pain, bruising and erythema was 4 days (IQR 3, 7), one day (IQR 1, 3), 3 days (IQR 3, 5) and 3 days (IQR 2, 3), respectively. The median peak degree of pain was 2 (IQR 1, 4) on a scale of 0-10. There were no serious adverse events and no cases of cellulitis or necrosis. No nodules or micronodules were found up to week 48.
Although the groups were different with regard to the endpoints at week 12, no significant difference between groups was evident in any endpoint by week 48 (Table 4). Subsequently, the week 48 analysis was carried out for the entire group as a single cohort. Relative to baseline, physician and patient FLSS scores both changed by a median of -2 (IQR -3, -1; P < 0.0001) and -2(IQR -2, -1; P < 0.0001), respectively, such that the median physician and patient FLSS scores at week 48 were 0 (IQR 0, 1) and 1 (IQR 0, 1), respectively. Whereas improvements in all domains of the MOS-HIV were observed from baseline to week 48, statistical significance was attained only for the mental health summary score (P = 0.01). In terms of the sDQLS from baseline to week 48, there was a statistically significant change observed with a median change of -3 (IQR -7, -1; P < 0.0001). Furthermore, statistically significant improvements were noted in both the depression (-3, IQR -5, 1; P = 0.01) and anxiety (-3, IQR -4, -1; P = 0.001) portions of the HADS scale from baseline to week 48.
Discussion
The results of our study indicate that injections of PAIG are associated with improvements in FLSS scores, as assessed by both physicians and patients. Benefits persisted through to week 48 of the study, with the delayed treatment group attaining similar benefits at the end of the study. In addition, treatment was associated with improved QoL and physical scores using the MOS-HIV, attributable predominantly to the mental health portion of the instrument. Similarly, anxiety scores on the HADS questionnaire and the sDQOL score were significantly reduced among patients receiving immediate therapy with PAIG compared with patients receiving deferred therapy, whereas the HADS depression score was less affected. Improvements in the mental health portion of the MOS-HIV, the sDQOL and the depression and anxiety portions of the HADS were maintained to 48 weeks when the cohort was analysed as a whole. Furthermore, treatment with PAIG was safe, with local side effects of a mild and transient nature being reported most often. Importantly, no infections were noted, and palpable nodules or micronodules were absent through the first 48 weeks of follow-up. As facial lipoatrophy is not directly harmful to health, the improvements noted in patient levels of anxiety and depression and QoL are probably the most relevant clinical indices of efficacy associated with the use of PAIG in our study.
Our study has several limitations, including the lack of assessment of dermal thickness by objective methods and short-term follow-up. Patients will continue to be followed in the study from an efficacy and toxicity perspective for a total of 96 weeks, thereby providing longer-term follow-up. Furthermore, the lack of blinding at the time the FLSS score was derived may have introduced bias into the study, particularly in the week 48 evaluation of the persistence of treatment effect. Blinding of the observers at the time of FLSS scoring to patient treatment status or time on-study, or the use of a control group would have remedied this limitation of our study. Finally, our cohort was composed almost exclusively of men, the majority of whom had either grade 1 or 2 lipoatrophy. We are therefore unable to draw conclusions about the safety, efficacy and impact on QoL of this product in women with facial lipoatrophy and patients with more severe facial lipoatrophy.
A practical limitation of therapy with all facial fillers for patients with facial lipoatrophy is the cost associated with these products. At the time of writing, the cost of PAIG in Canada was US$175.00 per millilitre, such that patients requiring 10-25 ml of the product would have to pay US$1750.00-4375.00 for a course of treatment. European prices vary by nation and treatment centre, ranging from 200 to 425 Euros per millilitre. Controlled trials with extended follow-up are required to determine whether improvements in patient anxiety and depression associated with corrective treatment of facial lipoatrophy offers a financial advantage compared with the costs associated with the psychological morbidity of this condition.
In summary, PAIG is a safe and effective corrective option for the correction of HIV-associated facial lipoatrophy, resulting in clinically important improvements in patient appearance, QoL, anxiety and depression. Extended follow-up of patients is necessary to confirm that the benefits of this product persist beyond the 48-week period of our study.
|
|
| |
| |
|
|
|