 |
 |
 |
| |
Influence of NRTI Choice and Efavirenz Versus Lopinavir Treatment Options on Lipoatrophy-Associated Adipose Tissue Toxicity: A Longitudinal Study
|
| |
| |
Reported by Jules Levin
15th CROI, Feb 2008, Boston
Emma Hammond, Bethy McKinnon, Craig Pace, Simon Mallal, David Nolan
Centre for Clinical Immunology and Biomedical Statistics, Murdoch University & Royal Perth Hospital, Perth, Western Australia
Clinical trials and cohort data have demonstrated associations between thymidine NRTI (particularly stavudine) use and lipoatrophy, while more recent data from the ACTG 5142 study suggest an additional effect of efavirenz versus lopinavir therapy [Haubrich R et al. 14th CROI, 2007, #38]. This study investigates the effects of HIV treatment choice in longitudinal adipose tissue specimens.
AUTHOR SUMMARY
MtDNA depletion and elevated cytokine expression in adipose tissue from individuals initiating first line therapy was associated with thymidine treatment. There was no evidence that use of efavirenz or lopinavir impacted these measures. Longer duration of thymidine treatment correlated with increased cytokine expression and macrophage count, but did not exacerbate mtDNA depletion. Moderate increases in mtDNA levels were observed in those switching from thymidines, but reductions in cytokine expression for these individuals were less marked.
Adipose tissue mtDNA depletion and pathological changes characteristic of clinical lipoatrophy are strongly and specifically associated with thymidine NRTI treatment. No independent effects of efavirenz or lopinavir treatment could be identified.
MATERIALS & METHODS
Longitudinal adipose biopsies were obtained from HIV+ patients. Samples were assessed for MtDNA depletion (realtime PCR) and tissue histology, with a subset further assessed for cytokine expression (IFN-gamma, TNF, IL-8, IL-12, IL-18) and macrophage density. Cytokines were scored between 0 and 3 (inclusive) according to both intensity and extent of immunoreactivity, with the average used for analyses. Macrophage count was performed per x 40 field of view. Statistical analysis utilized t-tests and mixed effects regression models for group comparisons.
Biopsies: N = 66 patients (n = 146 samples, mean = 2.2/person )
mtDNA: N = 65 (n = 140 samples)
cytokines: N = 31 (n = 69 samples)
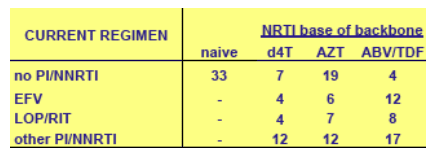
Initiating first line therapy
N = 40 (<24 months therapy)
Both pre-therapy and on-therapy samples: 5 d4T, 9 AZT, 10 ABV/TDF
Current thymidine (d4T/AZT) containing regimen:
Cumulative time on d4T/AZT: median (IQR) = 31 (9-70) months
Current non-thymidine only backbone:
No thymidine exposure - 15 ABV, 2 TDF, 1 ABV+TDF
Prior thymidine exposure - 21 ABV, 4 TDF, 2 ABV+TDF
- cumulative time on d4T/AZT: median (IQR) = 57 (28-89) months
- n=8 paired with pre-switch samples (5-23 mths since d4T/AZT)
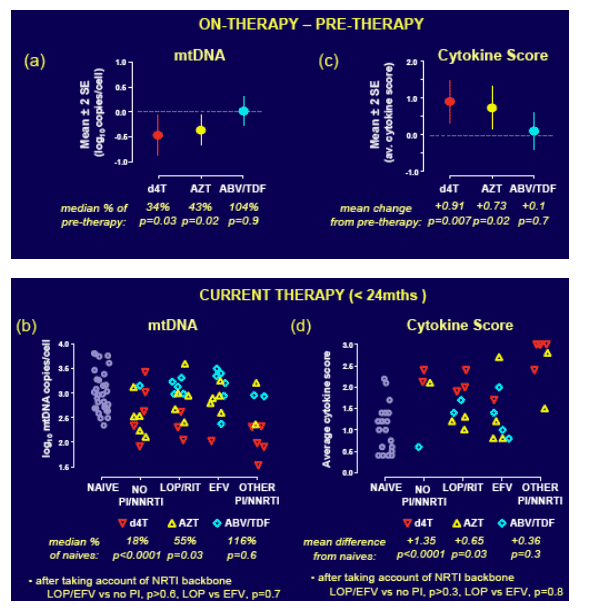
Figure 1. For patients initiating therapy, decreased mtDNA (a-b) and increased cytokine expression (c-d) were associated with thymidine treatment (d4T>AZT). No additive nor differential effects were observed with lopinavir/efavirenz choice.
RESULTS
Figure 2. Duration of thymidines had little impact on mtNA content (a) but correlated with increased cytokine expression (b-d). No independent effects of lopinavir or efavirenz were observed.
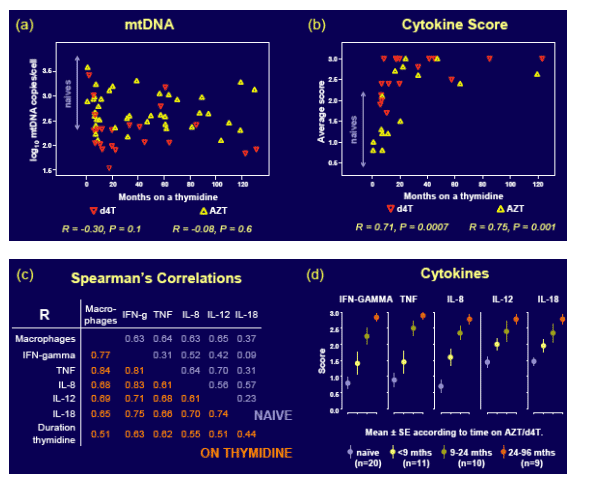
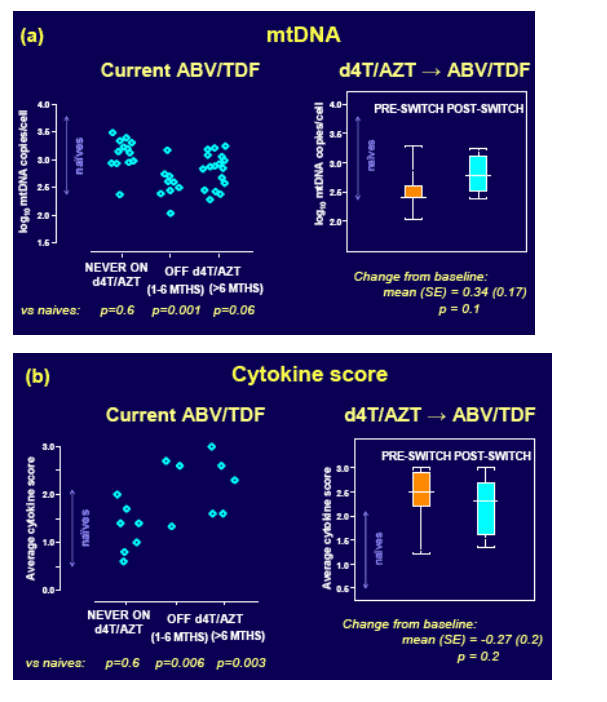
Figure 3. Those switching from long-term thymidine therapy showed partial normalisation of mtDNA levels (a) but limited reductions in cytokine expression (b).
|
| |
|
 |
 |
|
|