 |
 |
 |
| |
Treatment Response among HIV Patients Co-enrolled in the Etravirine (ETR) and Raltegravir (RAL) Expanded Access Programs (EAPs)
at Kaiser Permanente
|
| |
| |
Reported by Jules Levin
ICAAC/IDSA Oct 28 2008 Wash DC
Kerrigan H1, Towner W1, Klein D2, Follansbee S3
1Kaiser Permanente, Los Angeles, CA, USA; 2Kaiser Permanente, Hayward, CA, USA; 3Kaiser Permanente, San Francisco, CA, USA
BACKGROUND
In HIV treatment-experienced patients, DHHS guidelines recommend the inclusion of at least two, and preferably three, fully active antiretroviral agents when constructing drug regimens.1
Etravirine (ETR) is a next-generation non-nucleoside reverse transcriptase inhibitor (NNRTI) with demonstrated virologic activity against NNRTI resistant virus as well as a favorable safety profile.2-3
Raltegravir (RAL) is an oral integrase inhibitor with established safety, efficacy, and patient tolerability. As a member of a novel drug class, it is unexpected for treatment-experienced patients to have significant resistance to RAL.4-5
In the clinic setting, the concurrent ETR and RAL Expanded Access Programs (EAPs) provided an opportunity to examine the efficacy and safety of ETR + RAL + background therapy (BT) in treatment-experienced patients.
AUTHOR CONCLUSIONS
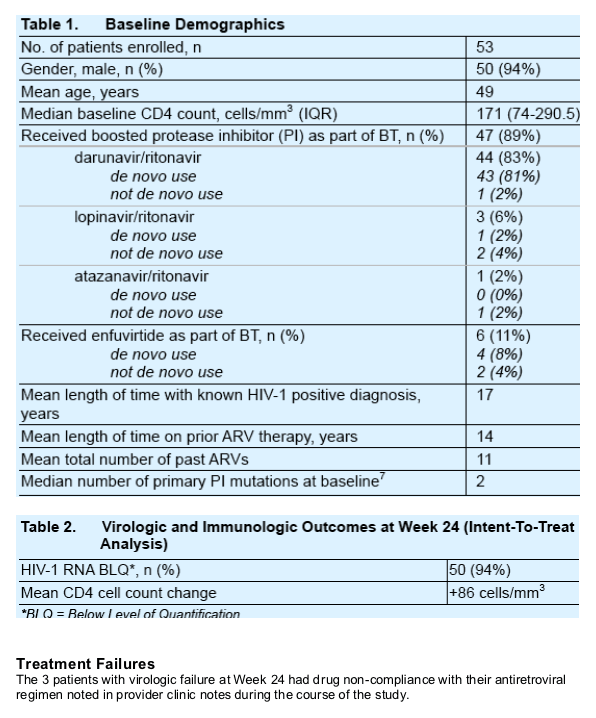
Among treatment-experienced patients receiving ETR + RAL + BT, over 90% of
patients achieved HIV-1 RNA below the level of quantification after 24 weeks of
therapy.
All patients were NNRTI experienced, however prior to initiating ETR + RAL + BT, more than half of patients had an ETR mutation score ≦ 2. The majority of these patients had mutations not associated with ETR resistance such as K103N, V108I, and P225H.
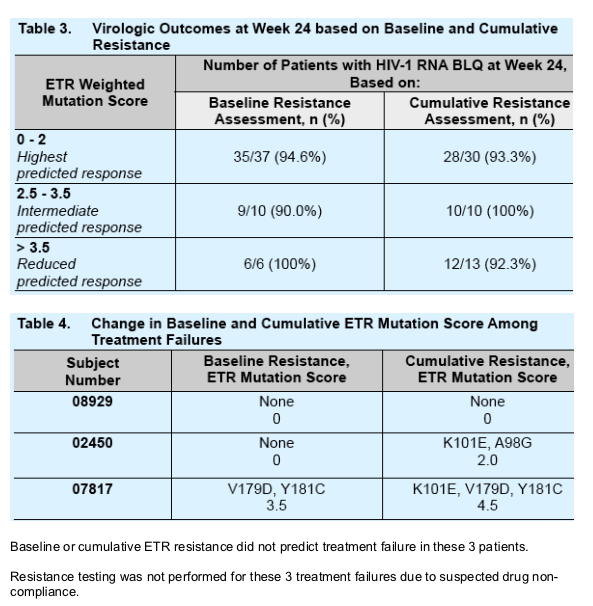
When comparing virologic outcomes by baseline versus cumulative resistance, the additional historical mutations obtained from the cumulative resistance did not appear to significantly change the observed response in this limited data set.
ETR resistance could not predict all treatment failures. Other factors such as
medication compliance and baseline PI resistance were likely to affect virologic
outcomes.
The high rate of virologic success in this study population can be contributed to the use of multiple active agents in the regimen, including ETR, RAL and/or a boosted PI.
The combination of ETR + RAL + BT was a safe and tolerable antiretroviral regimen, with minimal adverse events.
OBJECTIVES
Primary Objective
To assess the virologic effect of ETR + RAL + BT in HIV-1 infected treatment-experienced patients.
Secondary Objectives
To study the immunologic effect of ETR + RAL + BT in HIV-1 infected treatment-experienced patients.
To evaluate the effect of cumulative and baseline ETR resistance on virologic
outcomes. Cumulative resistance defined as baseline resistance + all available historic resistance data.
To summarize the safety profile of ETR + RAL + BT.
METHODS
Inclusion Criteria
Patients initiating ETR and RAL simultaneously via EAP enrollment at Kaiser Permanente Northern and Southern California.
Key EAP inclusion criteria included:
_Patient has limited or no treatment options due to virologic resistance or intolerance to multiple antiretroviral regimens.
-- Documented resistance to at least 1 drug in each of the 3 classes of oral ARVs (NRTI, NNRTI, and PI) by genotype or phenotype testing.
-- Intolerance is defined as having had a clinically significant adverse event which in the opinion of the investigator provides a contraindication to the use of any drug in that class.
Patient has experience to at least 3 antiretroviral classes (NRTI, NNRTI, and PI).
Patient is not achieving adequate virologic suppression on his/her current regimen and at risk of clinical or immunologic progression.
Patient is unable to use currently approved NNRTIs due to resistance (primary or
acquired) and/or intolerance.
Patient has not received RAL or any other integrase inhibitor prior to EAP
enrollment.
Study Design
A multicenter, retrospective study evaluating patients concurrently enrolled in ETR and RAL EAPs at 10 Kaiser Permanente HIV clinics in Northern and Southern California.
HIV-1 RNA, CD4 cell count, LFTs, serum creatinine, and lipid panel were collected at Screening, Baseline, Weeks 4, 12, and 24.
All available genotype tests prior to ETR + RAL + BT initiation were collected for study analysis.
ETR resistance was calculated utilizing the 2008 ETR weighted score method6. The 17 ETR mutations included were:
-- V90I, A98G, L100I, K101E, K101H, K101P, V106I, E138A, V179D, V179F, V179T, Y181C, Y181I, Y181V, G190A, G190S, M230L
Baseline ETR mutation score was calculated for each patient using their most recent genotype, prior to initiating ETR + RAL + BT regimen.
Cumulative ETR mutation score was calculated using the baseline genotype plus all available historic genotypes.
RESULTS
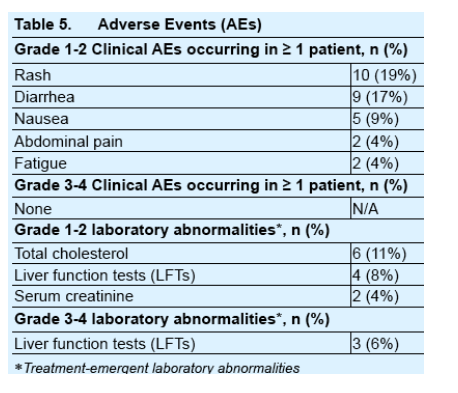
No patients discontinued therapy due to adverse events.
The 3 patients experiencing Grade 3-4 liver function tests had chronic hepatitis at baseline. These LFTs subsequently decreased in all patients.
REFERENCES
1. Panel on Antiretroviral Guidelines for Adult and Adolescents. Guidelines for the use of antiretroviral agents in HIV-1 infected adults and adolescents. Department of Health and Human Services. January 29, 2008; 1-128. Available at http:// www.aidsinfo.nih.gov/ContentFiles/AdultandAdolescentGL.pdf. Accessed June 5, 2008.
2. Madruga JV, Cahn P, Grinsztejn B, et al. Efficacy and safety of TMC125 (etravirine) in treatment-experienced HIV-1-infected patients in DUET-1: 24-week results from a randomized, double-blind, placebo-controlled trial. Lancet. 2007;Jul 7;370(9581):29-38.
3. Lazzarin A, Campbell T, Clotet B, et al. Efficacy and safety of TMC125 (etravirine) in treatment-experienced HIV-1-infected patients in DUET-2: 24-week results from a randomized, double-blind, placebo-controlled trial. Lancet. 2007;Jul 7;370(9581):39-48.
4. Steigbel R, Cooper D, Kumar P, et al. Raltegravir with optimized background therapy for resistant HIV-1 infection. N Engl J Med. 2008;359:399-54
5. Hazuda D, Felock P, Witmer M, et al. Inhibitors of strand transfer that prevent
integration and inhibit HIV-1 replication in cells. Science. 2000; Jan 28;287(5453):646-50
6. Vingerhoets J, Peeters M, Azijn H, et al. An update of the list of NNRTI mutations associated with decreased virologic response to etravirine (ETR): multivariate analyses on the pooled DUET-1 and DUET-2 clinical trial data. XVIIth International Drug Resistance Workshop; June 10-14, 2008; Sitges, Spain. Abstract 24.
7. Johnson V, Brun-Vezinet F, Clotet B, et al. Update of the Drug Resistance Mutations in HIV-1: Spring 2008. Topics in HIV Medicine. 2008;March/April;16(1):62-68
|
| |
|
 |
 |
|
|