 |
 |
 |
| |
Continuous Antiretroviral
Therapy Decreases Bone Mineral Density: Results from the SMART Study
|
| |
| |
Reported by Jules Levin
Presented at ICAAC and the Adverse Drug Reactions and Lipodystrophy Workshop
Birgit Grund1, Grace Peng1, Rachel Isaksson1, Kenneth Ellis2, Cynthia Gibert3, Judith Shlay4, Fraser Drummond5, Esteban Martinez6, Jennifer Hoy7, Daniel Pearce8, Peter Reiss9, Wafaa El-Sadr10, Avis Thomas1,
Fehmida Visnegarwala11, Andrew Carr12, for the INSIGHT SMART Study Group
1Univ. of Minnesota, Minneapolis, USA; 2Baylor College of Medicine, Houston, TX, USA, 3Veterans Affairs Medical Center, Washington, DC, USA; 4Denver Public Health, Denver, CO, USA; 5National Centre in HIV Epidemiology and Clinical Research,
Univ. of New South Wales, Sydney, Australia; 6Hospital Clinic, Institut d'Investigacions Biomediques August Pi i Sunyer, University of Barcelona, Spain; 7Alfred Hospital and Monash Univ., Melbourne, Australia; 8Western Univ. of Health Sciences, Pomona, CA, USA; 9Academic Medical Center,
Univ. of Amsterdam, Amsterdam, The Netherlands; 10Harlem Hospital and Columbia Univ., New York, USA; 11AbsoluteCare Medical Center and Morehouse School of Medicine, Atlanta, GA, USA, 12St. Vincent's Hospital and University of New South Wales, Sydney, Australia
AUTHOR DISCUSSION
The randomized comparison provides evidence that ART use contributes to the decline
in BMD.
BMD remained stable in the first year in the DC group, then declined at roughly similar rate as in the VS group. This pattern is consistent with the increased ART use after year 1 (Figure 2). There was no evidence that uncontrolled viral load (during the first year, most participants in the DC group) contributed to BMD loss.
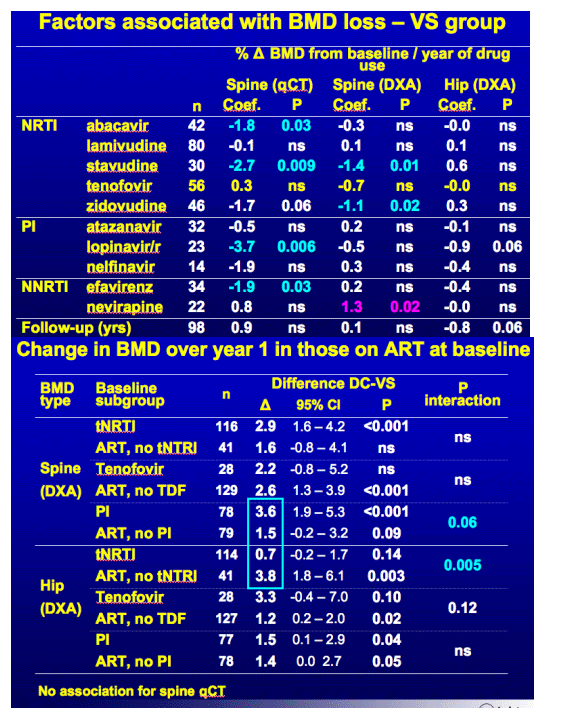
Stavudine, zidovudine and lopinavir/r were associated with decline in spine BMD by qCT and DXA. Consistent with other studies.
No evidence for association of tenofovir with BMD loss, contrary to other studies.
In HIV-negative adults, age-related BMD loss differs by location and x-ray technique.
Density of the trabecular bone of the spine (by qCT) declines faster than spine or hip BMD by DXA. [4].
Limitations
Study was not designed for identifying effects of individual drugs on BMD. Participants were taking multiple drugs, and ART regimens were not pre-specified.
Moderate sample size and follow-up time.
AUTHOR CONCLUSIONS
Continuous ART contributes to BMD loss and may increase the risk of fractures relative to intermittent, CD4-guided ART.
Intermittent ART is not recommended due to increased risk of AIDS, cardiovascular, renal and liver diseases, and death observed in the SMART study.
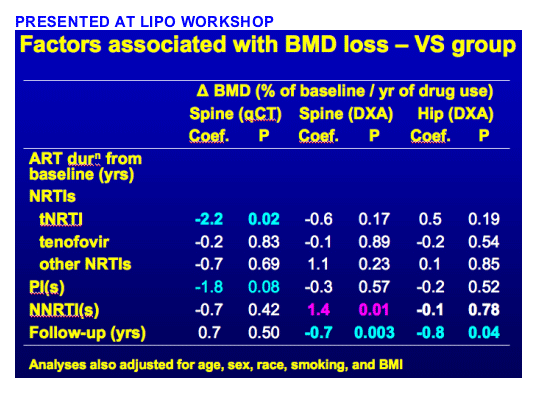
FROM LIPO WORKSHOP
Continuous ART causes greater loss of hip and spine BMD than intermittent, CD4-guided ART (the numbers of patients in the graphs below get small near the end of the followup)
BMD loss continued over 4 years and greater than expected for population of this age
No ART component was consistently associated with BMD decline
Intermittent ART in SMART was associated with significantly more OIs, deaths, major cardiovascular, renal and hepatic events, HIV transmission and with lower quality of life. The decreased loss of BMD with this strategy does not outweigh its substantial risks
INTRODUCTION
HIV-infected adults have lower bone mineral density (BMD) than the general population and may have more fractures. In cross-sectional studies, associations of tNRTI, tenofovir and protease inhibitor (PI) use with low BMD were found [1].
In the Strategies for Management of Anti-Retroviral Therapy (SMART) trial, 5472 participants were randomly allocated to continuous ART [VS group] versus CD4-guided intermittent ART [DC group]. Rates of AIDS, death, and non-AIDS clinical events were higher in the DC group; the DC strategy was stopped in January 2006. Design and results of the SMART study were published [2, 3].
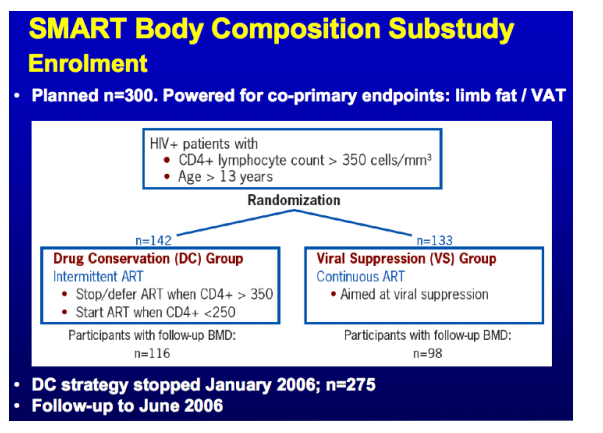
We evaluated the effect of ART on BMD prospectively in 214 participants co-enrolled in the Body Composition sub-study of SMART.

METHODS
Population
From May 2002 to January 2006, 275 participants were co-enrolled in the Body Composition substudy. The substudy closed June 2006. We analyzed BMD changes in the 214 participants who had follow-up measurements.
32 clinical sites (10 radiology sites) in the USA, Australia and Spain.
Bone Mineral Density Measurements
At baseline and annually, by quantitative computed tomography (qCT) and dual-energy
x-ray absorptiometry (DXA),
1. Lumbar spine BMD by qCT, measured volumetric density of the trabecular bone
2. Lumbar spine BMD by AP DXA
3. Total hip BMD by DXA
T-scores compare the BMD to the mean of a healthy, young (20 to 30-years) reference population, matched by sex and race, expressed as number of standard deviations above or below the reference mean.
Z-scores: references are also matched by age
Change in BMD was expressed in percent of baseline BMD.
Fractures
Passively collected from grade 4 adverse event reports in the main SMART study, January 2002 through July 2007. Identified by ICD-9 codes.
Research Questions and Analysis
1. What is the effect of continuous ART on BMD and fractures, compared with
intermittent ART? We compared treatment groups for change in BMD using longitudinal
models. In the full SMART study (n=5472), we compared the DC and VS groups for
incidence of fractures using Cox regression.
2. Are specific drugs or drug classes associated with decline in BMD? In the VS cohort,
we prospectively evaluated associations of cumulative drug use with changes in BMD.
Method: longitudinal regression with time-updated covariates for ART use.
RESULTS
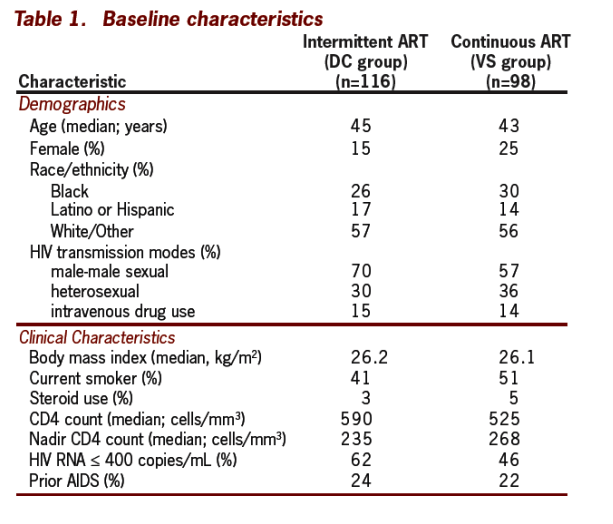
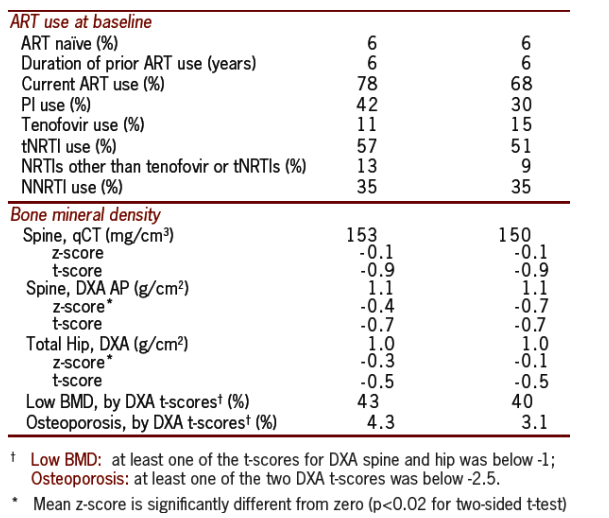
Analyses adjusted for sex, race and sex-race interaction
Change in BMD in the DC versus the VS groups
Overall, BMD declined less in the DC group (Figures 3A-C)
BMD declined by 0.9% per year (hip), 2.9% (spine qCT) and 0.4% (spine DXA) in the VS group
Estimated DC minus VS group differences in mean BMD change from baseline through follow-up were 1.4% (p=0.002) at the hip, 2.9% (p=0.01) for spine by qCT, and 1.2% (p=0.05) for spine by DXA.
Fractures
In the main SMART study (about 7500 person-years of follow-up per group)
⋅ 10 of 2753 participants in the VS group (rate 0.13 per 100 PY) and 2 of 2720 in the DC group (rate 0.03 per 100 PY) experienced grade 4 fractures
⋅ Hazard ratio (VS/DC) 4.9; 95% CI: 1.1 to 22.5; p=0.04
VS cohort: Association of cumulative ART use with BMD loss
Associations of specific drugs with BMD decline were not consistent across spine qCT, spine DXA, and hip DXA BMD (Table 2)
Traditional risk factors were not associated with BMD decline through follow-up (data not shown).
As ime goes by the number of evaluable patients gets smaller.
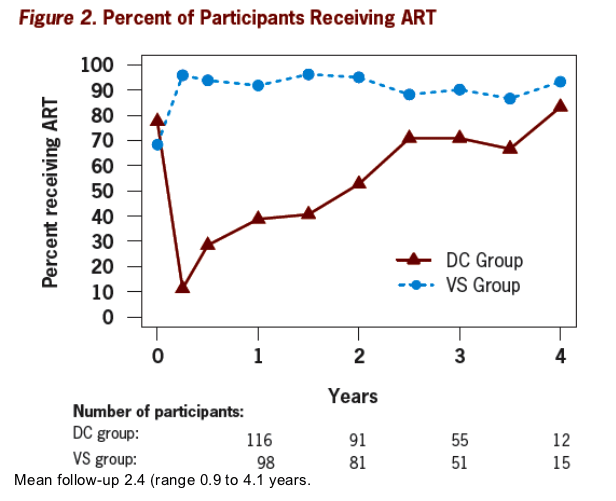
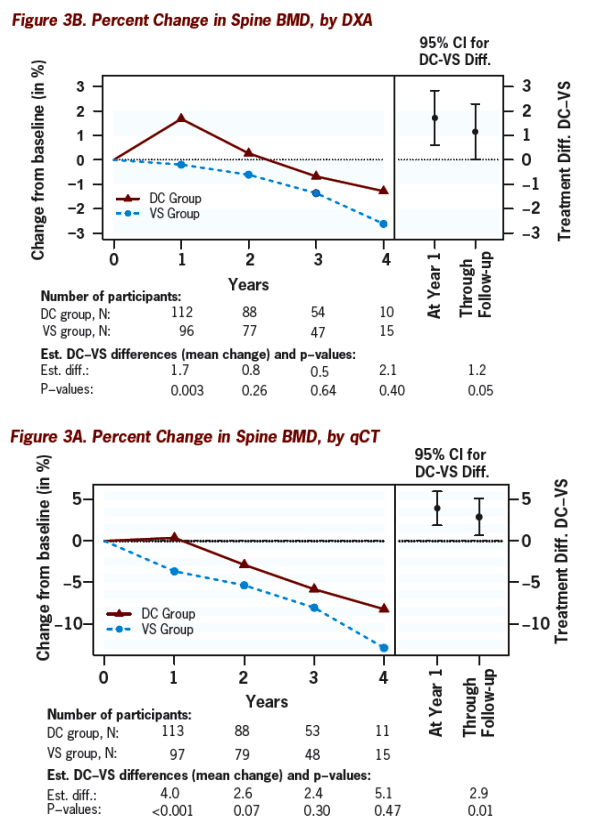
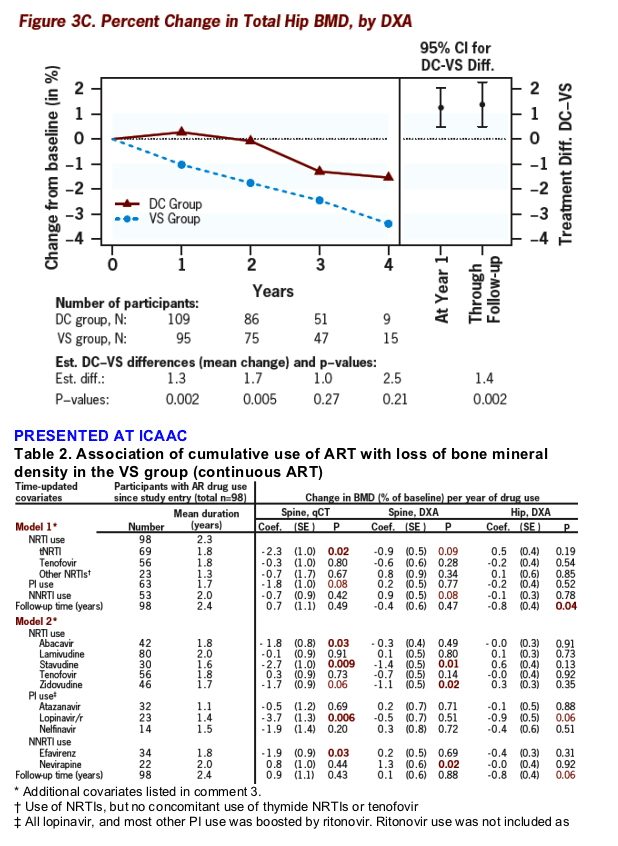
Table 2 Comments:
1. Coefficients estimate the change in BMD, as percent of baseline BMD, per year of using the drug or drug class after study entry. Estimates and p-values were obtained in longitudinal mixed models.
2. Participants were taking ART for 93% of their follow-up time, and follow-up time is included as covariate. Therefore, p-values assess effects of individual drugs (or classes) on BMD changes beyond the average ART regimen.
3. Models also contained the following covariates: race, sex, race by sex interaction, age, smoking (ever and time-updated current smoking status), history of alcohol abuse, BMI (baseline and time-updated change), and baseline BMD. Among these traditional risk factors, only change in BMI was associated with change in hip BMD, coefficient 0.8 per 1 BMI unit, p<0.001. 4. Results are hypothesis-generating. Associations do not prove causation.

REFERENCES
1. Brown TT, Qaqish RB. Antiretroviral therapy and the prevalence of osteopenia and osteoporosis: a meta-analytic review. AIDS 2006,20:2165-2174.
2. The SMART Study Group. CD4+ guided antiretroviral treatment interruption: Primary results of the SMART study. New England Journal of Medicine 2006,355: 2283-2296.
3. The SMART Study Group. Risk for opportunistic disease and death after reinitiating continuous antiretroviral therapy in HIV patients previously receiving episodic therapy: a randomized trial. Annals of Internal Medicine 2008,149:289-299.
4. Blake GM, Fogelman I. The role of DXA bone density scans in the diagnosis and treatment of osteoporosis. Postgrad Med J 2007,83:509-517.
|
| |
|
 |
 |
|
|